Search
- Page Path
- HOME > Search
- Correlation between HER2 gene copy number and immunohistochemistry categories in HER2-negative breast cancer: diagnostic utility for differentiating HER2-null, ultralow, and low tumors
- Min Chong Kim, Young Kyung Bae
- Received September 1, 2025 Accepted November 7, 2025 Published online February 25, 2026
- DOI: https://doi.org/10.4132/jptm.2025.11.07 [Epub ahead of print]
- 283 View
- 34 Download
-
 Abstract
Abstract
 PDF
PDF - Background
The recent recognition of human epidermal growth factor receptor 2 (HER2)–low and HER2-ultralow breast cancers (BCs) has expanded the therapeutic relevance of HER2 testing in the antibody-drug conjugate era. However, the biological continuum of HER2 expression measured by immunohistochemistry (IHC) and its relationship with the HER2 gene copy number remain unclear. Methods: We retrospectively analyzed 135 HER2-negative invasive BCs and reclassified them as HER2-null (IHC 0), HER2-ultralow (0+), or HER2-low (1+ or 2+ without amplification). HER2 gene copy number was determined using silver-enhanced in situ hybridization. Statistical analyses were performed to compare HER2 copy number among IHC categories and evaluate the discriminatory value of HER2 copy number for distinguishing IHC subgroups. Results: The mean HER2 copy number increased stepwise across IHC categories: 1.95 ± 0.54 (null), 2.03 ± 0.43 (ultralow), 2.25 ± 0.65 (low, 1+), and 3.29 ± 1.05 (low, 2+). Significant differences were observed between the ultralow and low groups (p = .003) and between the null and low groups (p < .001), but not between the null and ultralow groups or between the ultralow and 1+ groups. Conclusions: HER2 gene copy number was positively correlated with protein expression as reflected by IHC categories. Although HER2 gene copy number was statistically higher in HER2-low than in HER2-null tumors, the substantial overlap in copy number ranges likely limits its utility in distinguishing HER2-low from HER2- null BCs.
- Revisiting human sparganosis: a pathologic review from a single institution
- Jeemin Yim, Young A Kim, Jeong Hwan Park, Hye Eun Park, Hyun Beom Song, Ji Eun Kim
- J Pathol Transl Med. 2026;60(1):83-91. Published online January 9, 2026
- DOI: https://doi.org/10.4132/jptm.2025.10.14
- 1,580 View
- 92 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Sparganosis is a rare parasitic infection caused by Spirometra species. Although it was relatively common in the past, it is now often overlooked. In this study, we review cases diagnosed through histopathological examination at a single institution in recent years to raise awareness of this neglected parasitic disease. Methods: We retrospectively analyzed cases of human sparganosis identified in the pathology archives of a single institution in South Korea between 2004 and 2025. A comprehensive review was conducted, including demographic data, clinical features, lesion locations, imaging findings, exposure history (such as dietary habits), and histopathologic findings. Results: A total of 15 patients were identified, including 10 females and 5 males, with a mean age of 65.1 years. Lesions were most commonly located in the lower extremities and breast. Imaging findings were largely nonspecific, with ultrasonography being the most frequently used modality. In most cases, clinical suspicion of sparganosis was absent, and excision was performed under the impression of a benign or malignant tumor. Histologically, variably degenerated parasitic structures were identified within granulomatous inflammation. However, preserved features such as calcospherules and tegumental structures facilitated definitive diagnosis. Conclusions: This study underscores the importance of recognizing the characteristic histopathological features of sparganosis, which can allow for accurate diagnosis even in the absence of clinical suspicion. Although rare, sparganosis remains a relevant diagnostic consideration in endemic regions, particularly in East Asia.
- Spectrum of thyroiditis types: clinical, cytomorphological, and radiological findings
- Anam Singh, Indrajeet Kundu
- J Pathol Transl Med. 2025;59(6):421-433. Published online November 6, 2025
- DOI: https://doi.org/10.4132/jptm.2025.08.13
- 3,480 View
- 180 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Thyroiditis encompasses a range of inflammatory conditions affecting the thyroid gland. Lymphocytic thyroiditis (LT) is a common form of thyroiditis, with acute suppuration of the thyroid, while tuberculous thyroiditis is relatively rare. Fine-needle aspiration cytology (FNAC) remains a safe and cost-effective tool for diagnosing thyroid-related diseases, especially when paired with ultrasound (US) and clinical examination. Methods: This is a cross-sectional study including 21 cases. The cases were reported as thyroiditis on US and FNAC, and the findings were correlated with patient clinical history, symptoms during presentation, and serological profiles. Results: The cases of thyroiditis encompassed the more common forms, LT and subacute granulomatous thyroiditis (SAT), as well as relatively rare forms like tuberculous thyroiditis and thyroid abscess. Cases of follicular neoplasms (FN) arising in the context of LT also are included in this study. The case of tuberculous thyroiditis presented as a bulky thyroid gland that appeared heterogeneous on US with extensive necrosis on FNAC. The cases of thyroid abscess and SAT presented with painful neck swellings, with granulomas in the latter cases. US features of LT showed an array of appearances ranging from pseudonodular to an atrophic thyroid gland. All cases of FN showed a lymphocytic background. Conclusions: Thyroiditis is a commonly encountered condition that needs to be sub-categorized accurately into acute, subacute, and chronic types for appropriate clinical management, as they can sometimes show overlapping features. Though rare, acute suppurative and tuberculous thyroiditis are often encountered and warrant immediate care and treatment.
- BRCA-mutated gastric adenocarcinomas are associated with chromosomal instability and responsiveness to platinum-based chemotherapy
- Ji Hyun Oh, Chang Ohk Sung, Hyung-Don Kim, Sung-Min Chun, Jihun Kim
- J Pathol Transl Med. 2023;57(6):323-331. Published online November 14, 2023
- DOI: https://doi.org/10.4132/jptm.2023.10.22
- 6,831 View
- 268 Download
- 7 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Homologous recombination defect is an important biomarker of chemotherapy in certain tumor types, and the presence of pathogenic or likely pathogenic mutations involving BRCA1 or BRCA2 (p-BRCA) mutations is the most well-established marker for the homologous recombination defect. Gastric cancer, one of the most prevalent tumor types in Asia, also harbors p-BRCA mutations.
Methods
To investigate the clinical significance of p-BRCA mutations, we analyzed 366 gastric cancer cases through next-generation sequencing. We determined the zygosity of p-BRCA mutations based on the calculated tumor purity through variant allelic fraction patterns and investigated whether the presence of p-BRCA mutations is associated with platinum-based chemotherapy and a certain molecular subtype.
Results
Biallelic p-BRCA mutation was associated with better response to platinum-based chemotherapy than heterozygous p-BRCA mutation or wild type BRCA genes. The biallelic p-BRCA mutations was observed only in the chromosomal instability subtype, while all p-BRCA mutations were heterozygous in microsatellite instability subtype.
Conclusions
In conclusion, patients with gastric cancer harboring biallelic p-BRCA mutations were associated with a good initial response to platinum-based chemotherapy and those tumors were exclusively chromosomal instability subtype. Further investigation for potential association with homologous recombination defect is warranted. -
Citations
Citations to this article as recorded by- Risk prediction criteria for the primary hepatic perivascular epithelioid cell tumour family, including angiomyolipoma: analysis of 132 cases with a literature review
Youngeun Yoo, Jihun Kim, In Hye Song
Histopathology.2025; 86(6): 979. CrossRef - Presence of RB1 or Absence of LRP1B Mutation Predicts Poor Overall Survival in Patients with Gastric Neuroendocrine Carcinoma and Mixed Adenoneuroendocrine Carcinoma
In Hye Song, Bokyung Ahn, Young Soo Park, Deok Hoon Kim, Seung-Mo Hong
Cancer Research and Treatment.2025; 57(2): 492. CrossRef - Predictive value of homologous recombination-related gene mutations in survival outcomes of first-line nivolumab plus chemotherapy for gastric cancer
Yuna Lee, Hyung-Don Kim, Sun Young Lee, Hyungeun Lee, Jaewon Hyung, Meesun Moon, Jinho Shin, Young Soo Park, Tae Won Kim, Min-Hee Ryu
Gastric Cancer.2025; 28(6): 1158. CrossRef - Association of RAD51 expression with response to neoadjuvant treatment and prognosis in locally advanced gastric cancer
Serhat Sekmek, Serhat Ozan, Fahriye Tugba Kos, Hayriye Tatli Dogan, Mehmet Akif Parlar, Didem Sener Dede
Expert Review of Anticancer Therapy.2025; 25(12): 1433. CrossRef - Artificial intelligence algorithm for neoplastic cell percentage estimation and its application to copy number variation in urinary tract cancer
Jinahn Jeong, Deokhoon Kim, Yeon-Mi Ryu, Ja-Min Park, Sun Young Yoon, Bokyung Ahn, Gi Hwan Kim, Se Un Jeong, Hyun-Jung Sung, Yong Il Lee, Sang-Yeob Kim, Yong Mee Cho
Journal of Pathology and Translational Medicine.2024; 58(5): 229. CrossRef
- Risk prediction criteria for the primary hepatic perivascular epithelioid cell tumour family, including angiomyolipoma: analysis of 132 cases with a literature review
- Infections and immunity: associations with obesity and related metabolic disorders
- Amitabha Ray, Melissa J. L. Bonorden, Rajashree Pandit, Katai J. Nkhata, Anupam Bishayee
- J Pathol Transl Med. 2023;57(1):28-42. Published online January 15, 2023
- DOI: https://doi.org/10.4132/jptm.2022.11.14
- 15,350 View
- 295 Download
- 18 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF - About one-fourth of the global population is either overweight or obese, both of which increase the risk of insulin resistance, cardiovascular diseases, and infections. In obesity, both immune cells and adipocytes produce an excess of pro-inflammatory cytokines that may play a significant role in disease progression. In the recent coronavirus disease 2019 (COVID-19) pandemic, important pathological characteristics such as involvement of the renin-angiotensin-aldosterone system, endothelial injury, and pro-inflammatory cytokine release have been shown to be connected with obesity and associated sequelae such as insulin resistance/type 2 diabetes and hypertension. This pathological connection may explain the severity of COVID-19 in patients with metabolic disorders. Many studies have also reported an association between type 2 diabetes and persistent viral infections. Similarly, diabetes favors the growth of various microorganisms including protozoal pathogens as well as opportunistic bacteria and fungi. Furthermore, diabetes is a risk factor for a number of prion-like diseases. There is also an interesting relationship between helminths and type 2 diabetes; helminthiasis may reduce the pro-inflammatory state, but is also associated with type 2 diabetes or even neoplastic processes. Several studies have also documented altered circulating levels of neutrophils, lymphocytes, and monocytes in obesity, which likely modifies vaccine effectiveness. Timely monitoring of inflammatory markers (e.g., C-reactive protein) and energy homeostasis markers (e.g., leptin) could be helpful in preventing many obesity-related diseases.
-
Citations
Citations to this article as recorded by- Nonlinear association between pre-pregnancy body mass index and preterm birth in singleton pregnancies conceived with assisted reproductive technology
Tingting Zhuang, Jingli Sun, Yu Zhang
Frontiers in Nutrition.2026;[Epub] CrossRef - β-Lactam Antibiotics in Obese Adults: A Review of Population Pharmacokinetic Analyses
Guiva Annane, Benoît Crevier, Anis Ouyahia, Amélie Marsot
Clinical Pharmacokinetics.2026;[Epub] CrossRef - The Human Energy Balance: Uncovering the Hidden Variables of Obesity
Nikolaos Theodorakis, Maria Nikolaou
Diseases.2025; 13(2): 55. CrossRef - Candida infections in COVID-19 patients: A review of prevalence, risk factors, and mortality
Eduardo Franco Tulio, Fabíola Lucini, Allan Carminatti de Lima, Natalia Daiane Garoni Martins do Carmo, Marcelo dos Santos Barbosa, Gleyce Hellen de Almeida de Souza, Luana Rossato
Indian Journal of Medical Microbiology.2025; 55: 100831. CrossRef - Cell therapies for immune-mediated disorders
Natalia Wiewiórska-Krata, Bartosz Foroncewicz, Krzysztof Mucha, Radosław Zagożdżon
Frontiers in Medicine.2025;[Epub] CrossRef - Adipose Tissue in Chagas Disease: A Neglected Component of Pathogenesis
Vitória França dos Santos Pessoa, Mariana Hecht, Nadjar Nitz, Luciana Hagström
Pathogens.2025; 14(4): 339. CrossRef - The Impact of Obesity on Readmission and Healthcare Costs in Patients with Skin and Subcutaneous Tissue Infections
David Suh, Seung-Mi Lee
Risk Management and Healthcare Policy.2025; Volume 18: 1579. CrossRef - SARS-CoV-2 mRNA vaccines confer protection in diet-induced obese mice despite altered immune cell profiles in the lung
Katherine S. Lee, Dylan T. Boehm, Olivia A. Miller-Stump, Nathaniel A. Rader, Melissa Cooper, Holly A. Cyphert, Emel Sen-Kilic, Mariette Barbier, F. Heath Damron
Scientific Reports.2025;[Epub] CrossRef - Obesity promotes urinary tract infection by disrupting bladder focal adhesion kinase signaling
Laura Schwartz, Kristin Salamon, Aaron Simoni, Israel Cotzomi-Ortega, Yuriko Sanchez-Zamora, Sarah Linn-Peirano, Preeti John, Juan de Dios Ruiz-Rosado, Ashley R. Jackson, Xin Wang, John David Spencer
iScience.2025; 28(11): 113862. CrossRef - Theory of the Leaky Intestine: Gender Differences in Intestinal Parasitic Infections, Cytoskeletal Wall Dysfunctions, and Hypertension
Philip Njemanze, Anthonia Chioma Amadi, Joy E. Onuchukwu, Chinwendu C. Darlington, Nneoma E. Ukeje, Clinton O. Mezu, Clara C. Ofoegbu, Chidera Okuh, Chidimma O. Ukaegbu, Linda O. Uzoma, Marvis Amuchie, Faustina N. Ojilere, Lilian C. Mbara, Esther C. Nneke
Qeios.2024;[Epub] CrossRef - The potential of DNA methylation markers in the study of obesity
A. F. Nikolaeva, K. O. Petrova, O. V. Vasyukova, R. M. Guseinova, I. R. Minniakhmetov, R. I. Khusainova, N. G. Mokrysheva, V. O. Sigin
Obesity and metabolism.2024; 20(4): 301. CrossRef - Dysbiosis of the gut microbiota and its effect on α-synuclein and prion protein misfolding: consequences for neurodegeneration
Nasir Uddin Mahbub, Md Minarul Islam, Seong-Tshool Hong, Hea-Jong Chung
Frontiers in Cellular and Infection Microbiology.2024;[Epub] CrossRef - Sarcoma Size and Limb Dimensions Predict Complications, Recurrence, and Death in Patients with Soft Tissue Sarcoma in the Thigh: A Multidimensional Analysis
Rami Elmorsi, Luis Camacho, David D. Krijgh, Gordon S. Tilney, Heather Lyu, Raymond S. Traweek, Russell G. Witt, Margaret S. Roubaud, Christina L. Roland, Alexander F. Mericli
Annals of Surgical Oncology.2024; 31(8): 5421. CrossRef - Theory of the Leaky Intestine: Sex Differences in Intestinal Parasitic Infections, Cytoskeletal Wall Dysfunctions, and Hypertension
Philip Njemanze, Anthonia Chioma Amadi, Joy E. Onuchukwu, Chinwendu C. Darlington, Nneoma E. Ukeje, Clinton O. Mezu, Clara C. Ofoegbu, Chidera Okuh, Chidimma O. Ukaegbu, Linda O. Uzoma, Marvis Amuchie, Faustina N. Ojilere, Lilian C. Mbara, Esther C. Nneke
Qeios.2024;[Epub] CrossRef - Cellular immune response to a single dose of live attenuated hepatitis a virus vaccine in obese children and adolescents
Tanatchabhorn Soponkanabhorn, Narissara Suratannon, Supranee Buranapraditkun, Chomchanat Tubjareon, Sittichoke Prachuapthunyachart, Sutha Eiamkulbutr, Voranush Chongsrisawat
Heliyon.2024; 10(16): e36610. CrossRef - Increased Fruit and Vegetable Consumption Prevents Dysregulated Immune and Inflammatory Responses in High-Fat Diet-Induced Obese Mice
Weimin Guo, Dayong Wu, Lijun Li, Erin D Lewis, Simin Nikbin Meydani
The Journal of Nutrition.2024; 154(10): 3144. CrossRef - Sex differences in the inflammation-depression link: A systematic review and meta-analysis
Dana A. Jarkas, Ally H. Villeneuve, Ayeila Z.B. Daneshmend, Paul J. Villeneuve, Robyn J. McQuaid
Brain, Behavior, and Immunity.2024; 121: 257. CrossRef - The Strong Effect of Propolis in Suppressing NF-κB, CysC, and ACE2 on a High-fat Diet
Muhammad Reza Primaguna, Haerani Rasyid, Makbul Aman, Syakib Bakri, Hasyim Kasim, Harun Iskandar, Ressy Dwiyanti, Ade Rifka Junita, Ridwan Ridwan, Rizki Amelia Noviyanthi, Nur Indah Purnamasar, Mochammad Hatta
Biomedical and Pharmacology Journal.2024; 17(3): 1539. CrossRef - How market integration impacts human disease ecology
Lev Kolinski, Tyler M Barrett, Randall A Kramer, Charles L Nunn
Evolution, Medicine, and Public Health.2024; 12(1): 229. CrossRef - Molecular Pathways Linking High-Fat Diet and PM2.5 Exposure to Metabolically Abnormal Obesity: A Systematic Review and Meta-Analysis
Sagrario Lobato, Víctor Manuel Salomón-Soto, Claudia Magaly Espinosa-Méndez, María Nancy Herrera-Moreno, Beatriz García-Solano, Ernestina Pérez-González, Facundo Comba-Marcó-del-Pont, Mireya Montesano-Villamil, Marco Antonio Mora-Ramírez, Claudia Mancilla
Biomolecules.2024; 14(12): 1607. CrossRef - Anti-Obesity Effects of Marine Macroalgae Extract Caulerpa lentillifera in a Caenorhabditis elegans Model
Kawita Chumphoochai, Preeyanuch Manohong, Nakorn Niamnont, Montakan Tamtin, Prasert Sobhon, Krai Meemon
Marine Drugs.2023; 21(11): 577. CrossRef - Obesity and consequent changes in the body
Bojana Kisić, Dragana Puhalo-Sladoje, Dijana Mirić, Dragiša Rašić, Tatjana Novaković
Praxis medica.2022; 51(3): 35. CrossRef
- Nonlinear association between pre-pregnancy body mass index and preterm birth in singleton pregnancies conceived with assisted reproductive technology
- Lymphoproliferative disorder involving body fluid: diagnostic approaches and roles of ancillary studies
- Jiwon Koh, Sun Ah Shin, Ji Ae Lee, Yoon Kyung Jeon
- J Pathol Transl Med. 2022;56(4):173-186. Published online July 4, 2022
- DOI: https://doi.org/10.4132/jptm.2022.05.16
- 11,529 View
- 324 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Lymphocyte-rich effusions represent benign reactive process or neoplastic condition. Involvement of lymphoproliferative disease in body cavity is not uncommon, and it often causes diagnostic challenge. In this review, we suggest a practical diagnostic approach toward lymphocyte-rich effusions, share representative cases, and discuss the utility of ancillary tests. Cytomorphologic features favoring neoplastic condition include high cellularity, cellular atypia/pleomorphism, monomorphic cell population, and frequent apoptosis, whereas lack of atypia, polymorphic cell population, and predominance of small T cells usually represent benign reactive process. Involvement of non-hematolymphoid malignant cells in body fluid should be ruled out first, followed by categorization of the samples into either small/medium-sized cell dominant or large-sized cell dominant fluid. Small/medium-sized cell dominant effusions require ancillary tests when either cellular atypia or history/clinical suspicion of lymphoproliferative disease is present. Large-sized cell dominant effusions usually suggest neoplastic condition, however, in the settings of initial presentation or low overall cellularity, ancillary studies are helpful for more clarification. Ancillary tests including immunocytochemistry, in situ hybridization, clonality test, and next-generation sequencing can be performed using cytologic preparations. Throughout the diagnostic process, proper review of clinical history, cytomorphologic examination, and application of adequate ancillary tests are key elements for successful diagnosis.
-
Citations
Citations to this article as recorded by- Fluid Overload-Associated Large B-Cell Lymphoma Presenting as Isolated Pleural Effusion
Kevin Leeper, Lauren Borecky, Mojtaba Akhtari, Jun Wang
Hematology Reports.2026; 18(1): 13. CrossRef - The case of the sneaky lymphoma: solved by flow cytometry
Renu Singh, Md Ali Osama, Rachana Meena, Shailaja Shukla, Jagdish Chandra
Indian Journal of Thoracic and Cardiovascular Surgery.2025; 41(9): 1258. CrossRef - The urgency of Burkitt lymphoma diagnosis in fluid cytology—A tertiary care experience
Soundarya Ravi, Anu K. Devi, Prabhu Manivannan, Debasis Gochhait, Rakhee Kar, Neelaiah Siddaraju
Cytopathology.2024; 35(2): 275. CrossRef - Immunocytochemistry on frozen-embedded cell block for the diagnosis of hematolymphoid cytology specimen: a straightforward alternative to the conventional cell block
Youjeong Seo, Sanzida Alam Prome, Lucia Kim, Jee Young Han, Joon Mee Kim, Suk Jin Choi
Journal of Hematopathology.2024; 17(1): 1. CrossRef - Lymphoma presenting as the first finding in pleural fluid cytology: A rare cytologic presentation
Kafil Akhtar, Gowthami Nagendhran, Anjum Ara, Masheera Akhtar
IP Archives of Cytology and Histopathology Research.2024; 8(4): 250. CrossRef
- Fluid Overload-Associated Large B-Cell Lymphoma Presenting as Isolated Pleural Effusion
- Pathologic interpretation of endoscopic ultrasound–guided fine needle aspiration cytology/biopsy for pancreatic lesions
- Haeryoung Kim, Kee-Taek Jang
- J Pathol Transl Med. 2020;54(5):367-377. Published online August 31, 2020
- DOI: https://doi.org/10.4132/jptm.2020.07.21
- 9,440 View
- 224 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Pathologic interpretation of endoscopic ultrasound–guided fine needle aspiration (EUS-FNA) cytology/biopsy specimens is one of the most challenging tasks in cytology and surgical pathology practice, as the procedure often yields minimal amounts of diagnostic material and contains contaminants, such as blood cells and normal intestinal mucosa. EUS-FNA cytology/biopsy will nevertheless become a more popular procedure for evaluation of various pancreatic lesions because they are difficult to approach with conventional endoscopic procedures. Pathologists should understand the structural differences and limitations of EUS-FNA that make pathologic diagnosis difficult. Ancillary tests are available for differential diagnosis of EUS-FNA for various pancreatic lesions. Immunostains are the most commonly used ancillary tests, and pathologists should able to choose the necessary panel for differential diagnosis. Pathologists should review clinical history and radiologic and/or EUS findings before selecting an immunostain panel and making a pathologic diagnosis. In addition, one’s threshold of malignancy should be adjusted according to the appropriate clinical setting to avoid under-evaluation of pathologic diagnoses. Clinico-pathologic correlation is essential in pathologic evaluation of EUS-FNA for pancreatic lesions. Pathologists can reduce errors by correlating clinical and radiologic findings when evaluating EUS-FNA. Some molecular tests can be applied in differential diagnosis of pancreatic neoplastic and cystic lesions. Molecular data should be used as supportive evidence of a specific disease entity, rather than direct evidence, and should be correlated with clinico-pathologic findings to avoid errors in pathologic diagnosis.
-
Citations
Citations to this article as recorded by- Diagnostic Performance of EUS‐FNA for Pancreatic Lesions at Tertiary Centers in Iran Without Rapid On‐Site Evaluation
Maryam Bazmandegan, Gholam Reza Sivandzadeh, Kamran Bagheri Lankarani, Zahra Beyzaei, Bita Geramizadeh
Cytopathology.2025;[Epub] CrossRef - Endoscopic Ultrasound-Guided Pancreatic Tissue Sampling: Lesion Assessment, Needles, and Techniques
Jahnvi Dhar, Jayanta Samanta, Zaheer Nabi, Manik Aggarwal, Maria Cristina Conti Bellocchi, Antonio Facciorusso, Luca Frulloni, Stefano Francesco Crinò
Medicina.2024; 60(12): 2021. CrossRef - A prospective randomized noninferiority trial comparing conventional smears and SurePathTM liquid-based cytology in endoscopic ultrasound-guided sampling of esophageal, gastric, and duodenal lesions
Jae Chang Jun, Sang Hyub Lee, Han Myung Lee, Sang Gyun Kim, Hyunsoo Chung, Joo Seong Kim, Namyoung Park, Jin Ho Choi, Yoonjin Kwak, Soo-Jeong Cho
Medicine.2023; 102(29): e34321. CrossRef - Double Ki-67 and synaptophysin labeling in pancreatic neuroendocrine tumor biopsies
Bokyung Ahn, Jin Kying Jung, HaeSung Jung, Yeon-Mi Ryu, Yeon Wook Kim, Tae Jun Song, Do Hyun Park, Dae wook Hwang, HyungJun Cho, Sang-Yeob Kim, Seung-Mo Hong
Pancreatology.2022; 22(3): 427. CrossRef - Comparison of Endoscopic Ultrasound-Guided Fine Needle Aspiration with 19-Gauge and 22-Gauge Needles for Solid Pancreatic Lesions
Changjuan Li, Jianwei Mi, Fulai Gao, Xinying Zhu, Miao Su, Xiaoli Xie, Dongqiang Zhao
International Journal of General Medicine.2021; Volume 14: 10439. CrossRef
- Diagnostic Performance of EUS‐FNA for Pancreatic Lesions at Tertiary Centers in Iran Without Rapid On‐Site Evaluation
- Clinical Utility of a Fully Automated Microsatellite Instability Test with Minimal Hands-on Time
- Miseon Lee, Sung-Min Chun, Chang Ohk Sung, Sun Y. Kim, Tae W. Kim, Se Jin Jang, Jihun Kim
- J Pathol Transl Med. 2019;53(6):386-392. Published online October 11, 2019
- DOI: https://doi.org/10.4132/jptm.2019.09.25
- 10,035 View
- 234 Download
- 20 Web of Science
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Microsatellite instability (MSI) analysis is becoming increasingly important in many types of tumor including colorectal cancer (CRC). The commonly used MSI tests are either time-consuming or labor-intensive. A fully automated MSI test, the Idylla MSI assay, has recently been introduced. However, its diagnostic performance has not been extensively validated in clinical CRC samples.
Methods
We evaluated 133 samples whose MSI status had been rigorously validated by standard polymerase chain reaction (PCR), clinical nextgeneration sequencing (NGS) cancer panel test, or both. We evaluated the diagnostic performance of the Idylla MSI assay in terms of sensitivity, specificity, and positive and negative predictive values, as well as various sample requirements, such as minimum tumor purity and the quality of paraffin blocks.
Results
Compared with the gold standard results confirmed through both PCR MSI test and NGS, the Idylla MSI assay showed 99.05% accuracy (104/105), 100% sensitivity (11/11), 98.94% specificity (93/94), 91.67% positive predictive value (11/12), and 100% negative predictive value (93/93). In addition, the Idylla MSI assay did not require macro-dissection in most samples and reliably detected MSI-high in samples with approximately 10% tumor purity. The total turnaround time was about 150 minutes and the hands-on time was less than 2 minutes.
Conclusions
The Idylla MSI assay shows good diagnostic performance that is sufficient for its implementation in the clinic to determine the MSI status of at least the CRC samples. In addition, the fully automated procedure requires only a few slices of formalin-fixed paraffin-embedded tissue and might greatly save time and labor. -
Citations
Citations to this article as recorded by- Leveraging Radiomics and Hybrid Quantum–Classical Convolutional Networks for Non-Invasive Detection of Microsatellite Instability in Colorectal Cancer
T. Buvaneswari, M. Ramkumar, Prabhu Venkatesan, R. Sarath Kumar
Molecular Imaging and Biology.2025; 27(2): 227. CrossRef - Molecular Profiling of H-MSI/dMMR/for Endometrial Cancer Patients: “New Challenges in Diagnostic Routine Practice”
Riccardo Adorisio, Giancarlo Troncone, Massimo Barberis, Francesco Pepe
Journal of Molecular Pathology.2024; 5(2): 187. CrossRef - Enhanced Commendable Sensitivity and Specificity for MSI in Colorectal Cancer by a New PCR‐HRM Based 8‐Loci MSI Assay
Xueping Xiang, Xiaojing Ma, Linlin Ying, Hong Zou
Journal of Clinical Laboratory Analysis.2024;[Epub] CrossRef - Endometriumkarzinom: molekulare Klassifikation in der Routinepathologie
Udo Siebolts, Birgid Schömig-Markiefka, Janna Siemanowski-Hrach, Sabine Merkelbach-Bruse
Die Pathologie.2024; 45(5): 347. CrossRef - Integration of rapid PCR testing as an adjunct to NGS in diagnostic pathology services within the UK: evidence from a case series of non-squamous, non-small cell lung cancer (NSCLC) patients with follow-up
Alison Finall, Gareth Davies, Trevor Jones, Gwion Emlyn, Pearl Huey, Anna Mullard
Journal of Clinical Pathology.2023; 76(6): 391. CrossRef - Analytical Validation and Clinical Utilization of the Oncomine Comprehensive Assay Plus Panel for Comprehensive Genomic Profiling in Solid Tumors
Catherine I. Dumur, Ramakrishnan Krishnan, Jorge A. Almenara, Kathleen E. Brown, Kailyn R. Dugan, Christiana Farni, Fatima Z. Ibrahim, Naomi A. Sanchez, Sumra Rathore, Dinesh Pradhan, Jonathan H. Hughes
Journal of Molecular Pathology.2023; 4(2): 109. CrossRef - Performance of Immunohistochemical and Molecular Methods in Detecting Microsatellite Instability in Gastric Cancer: A Multicenter Study
Diogo Sousa Marques, Irene Gullo, Luís Mascarenhas-Lemos, João Ricardo Silva, Catarina Neto do Nascimento, Patrícia Pontes, Lídia Pinho, Luis Cirnes, Xiaogang Wen, Marília Cravo, Fátima Carneiro
Pathobiology.2023; 90(6): 389. CrossRef - Diagnostic mutationnel rapide Idylla™ : applications théranostiques actuelles et futures
Amélie Bourhis, Annabelle Remoué, Laura Samaison, Arnaud Uguen
Annales de Pathologie.2022; 42(4): 329. CrossRef - Comparison of the Idylla™ MSI assay with the Promega™ MSI Analysis System and immunohistochemistry on formalin-fixed paraffin-embedded tissue of endometrial carcinoma: results from an international, multicenter study
Sonia Gatius, Ana Velasco, Mar Varela, Miriam Cuatrecasas, Pedro Jares, Lisa Setaffy, Benjamin Bonhomme, Almudena Santon, Kristina Lindemann, Sabrina Croce, Ben Davidson, Sigurd Lax, Jose Palacios, Xavier Matias-Guiu
Virchows Archiv.2022; 480(5): 1031. CrossRef - Idylla MSI test combined with immunohistochemistry is a valuable and cost effective strategy to search for microsatellite instable tumors of noncolorectal origin
Laura Samaison, Arnaud Uguen
Pathology International.2022; 72(4): 234. CrossRef - Detection of microsatellite instability in a panel of solid tumours with the Idylla MSI Test using extracted DNA
Adrien Pécriaux, Loetitia Favre, Julien Calderaro, Cécile Charpy, Jonathan Derman, Anaïs Pujals
Journal of Clinical Pathology.2021; 74(1): 36. CrossRef - Idylla microsatellite instability assay versus mismatch repair immunohistochemistry: a retrospective comparison in gastric adenocarcinoma
Luke Farmkiss, Ilona Hopkins, Mary Jones
Journal of Clinical Pathology.2021; 74(9): 604. CrossRef - Multi-center real-world comparison of the fully automated Idylla™ microsatellite instability assay with routine molecular methods and immunohistochemistry on formalin-fixed paraffin-embedded tissue of colorectal cancer
Ana Velasco, Fatma Tokat, Jesper Bonde, Nicola Trim, Elisabeth Bauer, Adam Meeney, Wendy de Leng, George Chong, Véronique Dalstein, Lorand L. Kis, Jon A. Lorentzen, Snjezana Tomić, Keeley Thwaites, Martina Putzová, Astrid Birnbaum, Romena Qazi, Vanessa Pr
Virchows Archiv.2021; 478(5): 851. CrossRef - Detection of microsatellite instability with Idylla MSI assay in colorectal and endometrial cancer
Iiris Ukkola, Pirjo Nummela, Annukka Pasanen, Mia Kero, Anna Lepistö, Soili Kytölä, Ralf Bützow, Ari Ristimäki
Virchows Archiv.2021; 479(3): 471. CrossRef - Managing Difficulties of Microsatellite Instability Testing in Endometrial Cancer-Limitations and Advantages of Four Different PCR-Based Approaches
Janna Siemanowski, Birgid Schömig-Markiefka, Theresa Buhl, Anja Haak, Udo Siebolts, Wolfgang Dietmaier, Norbert Arens, Nina Pauly, Beyhan Ataseven, Reinhard Büttner, Sabine Merkelbach-Bruse
Cancers.2021; 13(6): 1268. CrossRef - Evaluation of Micro Satellite Instability and Mismatch Repair Status in Different Solid Tumors: A Multicenter Analysis in a Real World Setting
Umberto Malapelle, Paola Parente, Francesco Pepe, Caterina De Luca, Pasquale Pisapia, Roberta Sgariglia, Mariantonia Nacchio, Gianluca Gragnano, Gianluca Russo, Floriana Conticelli, Claudio Bellevicine, Elena Vigliar, Antonino Iaccarino, Claudia Covelli,
Cells.2021; 10(8): 1878. CrossRef - Novel Biocartis Idylla™ cartridge-based assay for detection of microsatellite instability in colorectal cancer tissues
Andres E. Mindiola-RomeroMD, Donald C. GreenBS, M. Rabie Al-TurkmaniPhD, Kelley N. GodwinBS, Anna C. MackayBS, Laura J. TafeMD, Bing RenMD, Gregory J. TsongalisPhD
Experimental and Molecular Pathology.2020; 116: 104519. CrossRef - Evaluation of 3 molecular-based assays for microsatellite instability detection in formalin-fixed tissues of patients with endometrial and colorectal cancers
Pauline Gilson, Julien Levy, Marie Rouyer, Jessica Demange, Marie Husson, Céline Bonnet, Julia Salleron, Agnès Leroux, Jean-Louis Merlin, Alexandre Harlé
Scientific Reports.2020;[Epub] CrossRef
- Leveraging Radiomics and Hybrid Quantum–Classical Convolutional Networks for Non-Invasive Detection of Microsatellite Instability in Colorectal Cancer
- An Experimental Infarct Targeting the Internal Capsule: Histopathological and Ultrastructural Changes
- Chang-Woo Han, Kyung-Hwa Lee, Myung Giun Noh, Jin-Myung Kim, Hyung-Seok Kim, Hyung-Sun Kim, Ra Gyung Kim, Jongwook Cho, Hyoung-Ihl Kim, Min-Cheol Lee
- J Pathol Transl Med. 2017;51(3):292-305. Published online May 10, 2017
- DOI: https://doi.org/10.4132/jptm.2017.02.17
- 10,648 View
- 117 Download
- 7 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Stroke involving the cerebral white matter (WM) has increased in prevalence, but most experimental studies have focused on ischemic injury of the gray matter. This study was performed to investigate the WM in a unique rat model of photothrombotic infarct targeting the posterior limb of internal capsule (PLIC), focusing on the identification of the most vulnerable structure in WM by ischemic injury, subsequent glial reaction to the injury, and the fundamental histopathologic feature causing different neurologic outcomes.
Methods
Light microscopy with immunohistochemical stains and electron microscopic examinations of the lesion were performed between 3 hours and 21 days post-ischemic injury.
Results
Initial pathological change develops in myelinated axon, concomitantly with reactive change of astrocytes. The first pathology to present is nodular loosening to separate the myelin sheath with axonal wrinkling. Subsequent pathologies include rupture of the myelin sheath with extrusion of axonal organelles, progressive necrosis, oligodendrocyte degeneration and death, and reactive gliosis. Increase of glial fibrillary acidic protein (GFAP) immunoreactivity is an early event in the ischemic lesion. WM pathologies result in motor dysfunction. Motor function recovery after the infarct was correlated to the extent of PLIC injury proper rather than the infarct volume.
Conclusions
Pathologic changes indicate that the cerebral WM, independent of cortical neurons, is highly vulnerable to the effects of focal ischemia, among which myelin sheath is first damaged. Early increase of GFAP immunoreactivity indicates that astrocyte response initially begins with myelinated axonal injury, and supports the biologic role related to WM injury or plasticity. The reaction of astrocytes in the experimental model might be important for the study of pathogenesis and treatment of the WM stroke. -
Citations
Citations to this article as recorded by- Neuroglia and immune cells play different roles in neuroinflammation and neuroimmune response in post-stroke neural injury and repair
Hui Guo, Wen-cao Liu, Yan-yun Sun, Xin-chun Jin, Pan-pan Geng
Acta Pharmacologica Sinica.2026; 47(2): 273. CrossRef - Animal models of focal ischemic stroke: brain size matters
Blazej Nowak, Piotr Rogujski, Raphael Guzman, Piotr Walczak, Anna Andrzejewska, Miroslaw Janowski
Frontiers in Stroke.2023;[Epub] CrossRef - Motor Cortex Plasticity During Functional Recovery Following Brain Damage
Noriyuki Higo
Journal of Robotics and Mechatronics.2022; 34(4): 700. CrossRef - Neurodegeneration, Myelin Loss and Glial Response in the Three-Vessel Global Ischemia Model in Rat
Tatiana Anan’ina, Alena Kisel, Marina Kudabaeva, Galina Chernysheva, Vera Smolyakova, Konstantin Usov, Elena Krutenkova, Mark Plotnikov, Marina Khodanovich
International Journal of Molecular Sciences.2020; 21(17): 6246. CrossRef - Quantitative assessment of demyelination in ischemic stroke in vivo using macromolecular proton fraction mapping
Marina Y Khodanovich, Alena A Kisel, Andrey E Akulov, Dmitriy N Atochin, Marina S Kudabaeva, Valentina Y Glazacheva, Michael V Svetlik, Yana A Medvednikova, Lilia R Mustafina, Vasily L Yarnykh
Journal of Cerebral Blood Flow & Metabolism.2018; 38(5): 919. CrossRef - Immunosignals of Oligodendrocyte Markers and Myelin-Associated Proteins Are Critically Affected after Experimental Stroke in Wild-Type and Alzheimer Modeling Mice of Different Ages
Dominik Michalski, Anna L. Keck, Jens Grosche, Henrik Martens, Wolfgang Härtig
Frontiers in Cellular Neuroscience.2018;[Epub] CrossRef - Administration of Downstream ApoE Attenuates the Adverse Effect of Brain ABCA1 Deficiency on Stroke
Xiaohui Wang, Rongwen Li, Alex Zacharek, Julie Landschoot-Ward, Fengjie Wang, Kuan-Han Hank Wu, Michael Chopp, Jieli Chen, Xu Cui
International Journal of Molecular Sciences.2018; 19(11): 3368. CrossRef
- Neuroglia and immune cells play different roles in neuroinflammation and neuroimmune response in post-stroke neural injury and repair
- Higher Expression of Toll-like Receptors 3, 7, 8, and 9 in Pityriasis Rosea
- Mostafa Abou El-Ela, Mohamed El-Komy, Rania Abdel Hay, Rehab Hegazy, Amin Sharobim, Laila Rashed, Khalda Amr
- J Pathol Transl Med. 2017;51(2):148-151. Published online February 13, 2017
- DOI: https://doi.org/10.4132/jptm.2016.09.09
- 9,219 View
- 101 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Pityriasis rosea (PR) is a common papulosquamous skin disease in which an infective agent may be implicated. Toll-like receptors (TLRs) play an important role in immune responses and in the pathophysiology of inflammatory skin diseases. Our aim was to determine the possible roles of TLRs 3, 7, 8, and 9 in the pathogenesis of PR. Methods: Twenty-four PR patients and 24 healthy individuals (as controls) were included in this case control study. All recruits were subjected to routine laboratory investigations. Biopsies were obtained from one active PR lesion and from healthy skin of controls for the detection of TLR 3, 7, 8, and 9 gene expression using real-time polymerase chain reaction. Results: This study included 24 patients (8 females and 16 males) with active PR lesions, with a mean age of 28.62 years. Twenty four healthy age- and sex-matched individuals were included as controls (8 females and 16 males, with a mean age of 30.83 years). The results of the routine laboratory tests revealed no significant differences between both groups. Significantly elevated expression of all studied TLRs were detected in PR patients relative to healthy controls (p < .001). Conclusions: TLRs 3, 7, 8, and 9 might be involved in the pathogenesis of PR. -
Citations
Citations to this article as recorded by- Toll-like Receptor-Mediated Immunomodulation of Th1-Type Response Stimulated by Recombinant Antigen of Type 2 Porcine Reproductive and Respiratory Syndrome Virus (PRRSV-2)
Rika Wahyuningtyas, Mei-Li Wu, Wen-Bin Chung, Hso-Chi Chaung, Ko-Tung Chang
Viruses.2023; 15(3): 775. CrossRef - Pityriasis Rosea: An Updated Review
Alexander K.C. Leung, Joseph M. Lam, Kin Fon Leong, Kam Lun Hon
Current Pediatric Reviews.2021; 17(3): 201. CrossRef - Double-blind randomized placebo-controlled trial to evaluate the efficacy and safety of short-course low-dose oral prednisolone in pityriasis rosea
Sidharth Sonthalia, Akshy Kumar, Vijay Zawar, Adity Priya, Pravesh Yadav, Sakshi Srivastava, Atula Gupta
Journal of Dermatological Treatment.2018; 29(6): 617. CrossRef
- Toll-like Receptor-Mediated Immunomodulation of Th1-Type Response Stimulated by Recombinant Antigen of Type 2 Porcine Reproductive and Respiratory Syndrome Virus (PRRSV-2)
- KRAS Mutation Test in Korean Patients with Colorectal Carcinomas: A Methodological Comparison between Sanger Sequencing and a Real-Time PCR-Based Assay
- Sung Hak Lee, Arthur Minwoo Chung, Ahwon Lee, Woo Jin Oh, Yeong Jin Choi, Youn-Soo Lee, Eun Sun Jung
- J Pathol Transl Med. 2017;51(1):24-31. Published online December 25, 2016
- DOI: https://doi.org/10.4132/jptm.2016.10.03
- 12,781 View
- 170 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Mutations in the KRAS gene have been identified in approximately 50% of colorectal cancers (CRCs). KRAS mutations are well established biomarkers in anti–epidermal growth factor receptor therapy. Therefore, assessment of KRAS mutations is needed in CRC patients to ensure appropriate treatment.
Methods
We compared the analytical performance of the cobas test to Sanger sequencing in 264 CRC cases. In addition, discordant specimens were evaluated by 454 pyrosequencing.
Results
KRAS mutations for codons 12/13 were detected in 43.2% of cases (114/264) by Sanger sequencing. Of 257 evaluable specimens for comparison, KRAS mutations were detected in 112 cases (43.6%) by Sanger sequencing and 118 cases (45.9%) by the cobas test. Concordance between the cobas test and Sanger sequencing for each lot was 93.8% positive percent agreement (PPA) and 91.0% negative percent agreement (NPA) for codons 12/13. Results from the cobas test and Sanger sequencing were discordant for 20 cases (7.8%). Twenty discrepant cases were subsequently subjected to 454 pyrosequencing. After comprehensive analysis of the results from combined Sanger sequencing–454 pyrosequencing and the cobas test, PPA was 97.5% and NPA was 100%.
Conclusions
The cobas test is an accurate and sensitive test for detecting KRAS-activating mutations and has analytical power equivalent to Sanger sequencing. Prescreening using the cobas test with subsequent application of Sanger sequencing is the best strategy for routine detection of KRAS mutations in CRC. -
Citations
Citations to this article as recorded by- Single-center study on clinicopathological and typical molecular pathologic features of metastatic brain tumor
Su Hwa Kim, Young Suk Lee, Sung Hak Lee, Yeoun Eun Sung, Ahwon Lee, Jun Kang, Jae-Sung Park, Sin Soo Jeun, Youn Soo Lee
Journal of Pathology and Translational Medicine.2023; 57(4): 217. CrossRef - Assessment of KRAS and NRAS status in metastatic colorectal cancer: Experience of the National Institute of Oncology in Rabat Morocco
Chaimaa Mounjid, Hajar El Agouri, Youssef Mahdi, Abdelilah Laraqui, En-nacer Chtati, Soumaya Ech-charif, Mouna Khmou, Youssef Bakri, Amine Souadka, Basma El Khannoussi
Annals of Cancer Research and Therapy.2022; 30(2): 80. CrossRef - The current understanding on the impact of KRAS on colorectal cancer
Mingjing Meng, Keying Zhong, Ting Jiang, Zhongqiu Liu, Hiu Yee Kwan, Tao Su
Biomedicine & Pharmacotherapy.2021; 140: 111717. CrossRef - Droplet digital PCR revealed high concordance between primary tumors and lymph node metastases in multiplex screening of KRAS mutations in colorectal cancer
Barbora Vanova, Michal Kalman, Karin Jasek, Ivana Kasubova, Tatiana Burjanivova, Anna Farkasova, Peter Kruzliak, Dietrich Busselberg, Lukas Plank, Zora Lasabova
Clinical and Experimental Medicine.2019; 19(2): 219. CrossRef - CRISPR Technology for Breast Cancer: Diagnostics, Modeling, and Therapy
Rachel L. Mintz, Madeleine A. Gao, Kahmun Lo, Yeh‐Hsing Lao, Mingqiang Li, Kam W. Leong
Advanced Biosystems.2018;[Epub] CrossRef
- Single-center study on clinicopathological and typical molecular pathologic features of metastatic brain tumor
- CD9 Expression in Colorectal Carcinomas and Its Prognostic Significance
- Kyung-Ju Kim, Hee Jung Kwon, Min Chong Kim, Young Kyung Bae
- J Pathol Transl Med. 2016;50(6):459-468. Published online October 25, 2016
- DOI: https://doi.org/10.4132/jptm.2016.10.02
- 10,775 View
- 156 Download
- 19 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
CD9, a member of the tetraspanin superfamily, is a tumor suppressor in many malignancies. The aim of this study was to evaluate the immunohistochemical expression of CD9 in colorectal carcinomas (CRCs) and determine clinicopathological and prognostic significance of its expression.
Methods
The CD9 expression status of 305 CRCs was evaluated using a semi-quantitative scoring system in tumor cells (T-CD9) and immune cells (I-CD9) by classifying the results as high and low expression.
Results
High T-CD9 (T-CD9 [+]) expression was detected in 175 samples (57.6%) and high I-CD9 (I-CD9 [+]) expression was detected in 265 samples (86.9%). Using Kaplan- Meier survival analysis, the T-CD9 (+) group showed a tendency for better disease-free survival (DFS) (p = .057). In left-sided tumors, DFS was significantly longer in the T-CD9 (+) group (p = .021) but no statistical significance was observed with right-sided tumors (p = .453). I-CD9 (+) CRCs significantly correlated with well/moderately differentiation (p = .014). In Kaplan-Meier analysis, the I-CD9 (+) group had a tendency towards worse DFS compared to the I-CD9 (–) group (p = .156). In combined survival analysis of T-CD9 and I-CD9, we found that the longest DFS was among patients in the T-CD9 (+)/I-CD9 (–) group, whereas the T-CD9 (–)/I-CD9 (+) group showed the shortest DFS (p = .054).
Conclusions
High expression of T-CD9 was associated with a favorable DFS, especially in left-sided CRCs. Combined evaluation of T-CD9 and I-CD9 is required to determine the comprehensive prognostic effect of CD9 in CRCs. -
Citations
Citations to this article as recorded by- Prognostic Significance of Nuclear Factor Kappa B and CD9/Motility-related Protein-1 in Stage II-III Rectal Cancer Patients Treated with Postoperative Chemoradiotherapy
Serkan KAPLAN, Oğuz Galip YILDIZ, Işın SOYUER, Serdar SOYUER
Journal of Eurasian Medical Science.2026; : 42. CrossRef - Predicting patient outcomes with gene-expression biomarkers from colorectal cancer organoids and cell lines
Alexandra Razumovskaya, Mariia Silkina, Andrey Poloznikov, Timur Kulagin, Maria Raigorodskaya, Nina Gorban, Anna Kudryavtseva, Maria Fedorova, Boris Alekseev, Alexander Tonevitsky, Sergey Nikulin
Frontiers in Molecular Biosciences.2025;[Epub] CrossRef - Intestinal estrogen receptor beta modulates the murine colon tumor immune microenvironment
Madeleine Birgersson, Matilda Holm, Carlos J. Gallardo-Dodd, Baizhen Chen, Lina Stepanauskaitė, Linnea Hases, Claudia Kutter, Amena Archer, Cecilia Williams
Cancer Letters.2025; 622: 217661. CrossRef - Establishment of Coala: a novel 3D and 2D cancer cell line derived from colorectal cancer liver metastasis
Sandra Mersakova, Juraj Marcinek, Dusan Brany, Olga Chodelkova, Martin Vorcak, Martin Cermak, Martina Poturnajova, Zuzana Kozovska, Henrieta Skovierova, Slavomira Novakova, Barbora Mitruskova, Dusan Loderer, Marian Grendar, Veronika Holubekova, Andrea Hor
Human Cell.2025;[Epub] CrossRef - CD9, a tetraspanin in cancer: biology and therapeutic promise in acute leukemia
Océane Guého, Elie Cousin, Jérémie Rouger-Gaudichon, Anne-Gaëlle Rio, Sébastien Corre, Virginie Gandemer, Frédéric Mazurier
Oncogenesis.2025;[Epub] CrossRef - Proteomic analysis of plasma exosomes in patients with metastatic colorectal cancer
Zhaoyue Zhong, Jiayin Ji, Hongxia Li, Ling Kang, Haipeng Zhu
Clinical Proteomics.2024;[Epub] CrossRef - Prognostic value and multifaceted roles of tetraspanin CD9 in cancer
Róbert Ondruššek, Barbora Kvokačková, Karolína Kryštofová, Světlana Brychtová, Karel Souček, Jan Bouchal
Frontiers in Oncology.2023;[Epub] CrossRef - Proteomic Signature of Extracellular Vesicles Associated with Colorectal Cancer
Natalia Soloveva, Svetlana Novikova, Tatiana Farafonova, Olga Tikhonova, Victor Zgoda
Molecules.2023; 28(10): 4227. CrossRef - Anti-Human CD9 Fab Fragment Antibody Blocks the Extracellular Vesicle-Mediated Increase in Malignancy of Colon Cancer Cells
Mark F. Santos, Germana Rappa, Simona Fontana, Jana Karbanová, Feryal Aalam, Derek Tai, Zhiyin Li, Marzia Pucci, Riccardo Alessandro, Chikao Morimoto, Denis Corbeil, Aurelio Lorico
Cells.2022; 11(16): 2474. CrossRef - The Study of the Extracellular Matrix in Chronic Inflammation: A Way to Prevent Cancer Initiation?
Asia Marangio, Andrea Biccari, Edoardo D’Angelo, Francesca Sensi, Gaya Spolverato, Salvatore Pucciarelli, Marco Agostini
Cancers.2022; 14(23): 5903. CrossRef - In vivo expansion of a CD9+ decidual-like NK cell subset following autologous hematopoietic stem cell transplantation
Ane Orrantia, Enrique Vázquez-De Luis, Gabirel Astarloa-Pando, Iñigo Terrén, Ainhoa Amarilla-Irusta, Diego Polanco-Alonso, Carmen González, Alasne Uranga, Tomás Carrascosa, Juan J. Mateos-Mazón, Juan C. García-Ruiz, Sergio Callejas, Ana Quintas, Ana Dopaz
iScience.2022; 25(10): 105235. CrossRef - Inhibition of cancer-cell migration by tetraspanin CD9-binding peptide
Thanawat Suwatthanarak, Masayoshi Tanaka, Yoshitaka Miyamoto, Kenji Miyado, Mina Okochi
Chemical Communications.2021; 57(40): 4906. CrossRef - High expression of tumor susceptibility gene 101 (TSG101) is associated with more aggressive behavior in colorectal carcinoma
Elmira Gheytanchi, Leili Saeednejad Zanjani, Roya Ghods, Maryam Abolhasani, Marzieh Shahin, Somayeh Vafaei, Marzieh Naseri, Fahimeh Fattahi, Zahra Madjd
Journal of Cancer Research and Clinical Oncology.2021; 147(6): 1631. CrossRef - Increased CD9 expression predicts favorable prognosis in human cancers: a systematic review and meta-analysis
Hyun Min Koh, Bo Gun Jang, Dong Hui Lee, Chang Lim Hyun
Cancer Cell International.2021;[Epub] CrossRef - Prognostic Value of CD9 in Solid Tumor: A Systematic Review and Meta-Analysis
Ping Zeng, Meng Si, Rui-xia Sun, Xu Cheng, Xiao-yang Li, Min-bin Chen
Frontiers in Oncology.2021;[Epub] CrossRef - Matrix Effect in the Isolation of Breast Cancer-Derived Nanovesicles by Immunomagnetic Separation and Electrochemical Immunosensing—A Comparative Study
Silio Lima Moura, Mercè Martì, María Isabel Pividori
Sensors.2020; 20(4): 965. CrossRef - CD9 expression indicates a poor outcome in acute lymphoblastic leukemia
Peiqi Liang, Miao Miao, Zhuogang Liu, Hongtao Wang, Wei Jiang, Shiyu Ma, Chuan Li, Rong Hu
Cancer Biomarkers.2018; 21(4): 781. CrossRef
- Prognostic Significance of Nuclear Factor Kappa B and CD9/Motility-related Protein-1 in Stage II-III Rectal Cancer Patients Treated with Postoperative Chemoradiotherapy
- Does Polymerase Chain Reaction of Tissue Specimens Aid in the Diagnosis of Tuberculosis?
- Yoo Jin Lee, Seojin Kim, Youngjin Kang, Jiyoon Jung, Eunjung Lee, Joo-Young Kim, Jeong Hyeon Lee, Youngseok Lee, Yang-seok Chae, Chul Hwan Kim
- J Pathol Transl Med. 2016;50(6):451-458. Published online October 10, 2016
- DOI: https://doi.org/10.4132/jptm.2016.08.04
- 14,306 View
- 258 Download
- 7 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Mycobacterial culture is the gold standard test for diagnosing tuberculosis (TB), but it is time-consuming. Polymerase chain reaction (PCR) is a highly sensitive and specific method that can reduce the time required for diagnosis. The diagnostic efficacy of PCR differs, so this study determined the actual sensitivity of TB-PCR in tissue specimens.
Methods
We retrospectively reviewed 574 cases. The results of the nested PCR of the IS6110 gene, mycobacterial culture, TB-specific antigen-induced interferon-γ release assay (IGRA), acid-fast bacilli (AFB) staining, and histological findings were evaluated.
Results
The positivity rates were 17.6% for PCR, 3.3% for the AFB stain, 22.2% for mycobacterial culture, and 55.4% for IGRA. PCR had a low sensitivity (51.1%) and a high specificity (86.3%) based on the culture results of other studies. The sensitivity was higher (65.5%) in cases with necrotizing granuloma but showed the highest sensitivity (66.7%) in those with necrosis only. The concordance rate between the methods indicated that PCR was the best method compared to mycobacterial culture, and the concordance rate increased for the methods using positive result for PCR or histologic features.
Conclusions
PCR of tissue specimens is a good alternative to detect tuberculosis, but it may not be as sensitive as previously suggested. Its reliability may also be influenced by some histological features. Our data showed a higher sensitivity when specimens contained necrosis, which indicated that only specimens with necrosis should be used for PCR to detect tuberculosis. -
Citations
Citations to this article as recorded by-
The Need for Persistence in the Diagnosis of Mycobacterium Tuberculosis Mono-arthritis: A Unique Case Presentation
T. Bekoulis, P. Christodoulou, K. Dogramatzis, E. Markopoulou, Emmanouel Antonogiannakis, E. Kokkinakis, Alexandros P. Apostolopoulos, A. Manimanaki
Journal of Long-Term Effects of Medical Implants.2024; 34(1): 35. CrossRef - A Case Report on Scrofuloderma: A Cutaneous Manifestation of Tuberculosis
Soham R Meghe, Adarshlata Singh, Drishti M Bhatt, Shreya N Gupta, Varun Hanumanthaiah, Shree Ramya Talasila
Cureus.2024;[Epub] CrossRef - An overview of infectious disease laboratory methods: an update for the histopathologist
Daniel R. Stevenson
Diagnostic Histopathology.2024; 30(10): 534. CrossRef - Diagnostic Utility of Biplex/Multiplex Polymerase Chain Reaction in Infectious Granulomatous Dermatitis in North Indian Population
Mayur Parkhi, Mukin Kumar S, Dipankar De, Rakesh Yadav, Sunil Sethi, Bishan Dass Radotra, Uma Nahar Saikia
The American Journal of Dermatopathology.2021; 43(8): 567. CrossRef - Reduction of turnaround time for non-tuberculous mycobacteria detection in heater–cooler units by propidium monoazide–real-time polymerase chain reaction
S. Ditommaso, M. Giacomuzzi, G. Memoli, R. Cavallo, A. Curtoni, M. Avolio, C. Silvestre, C.M. Zotti
Journal of Hospital Infection.2020; 104(3): 365. CrossRef - Ergonomic Diagnostic Tool based on Chip Mini RT-PCR for Diagnosis of Pulmonary and Extra Pulmonary Tuberculosis
V Mangayarkarasi, Sneka P, Sujith R, Jayaprakash Jayaprakash
Journal of Pure and Applied Microbiology.2019; 13(2): 1185. CrossRef - Cutaneous Tuberculosis: Clinicopathologic Arrays and Diagnostic Challenges
Priyatam Khadka, Soniya Koirala, Januka Thapaliya
Dermatology Research and Practice.2018; 2018: 1. CrossRef - Utility of Real-Time Quantitative Polymerase Chain Reaction in DetectingMycobacterium tuberculosis
Zhongquan Lv, Mingxin Zhang, Hui Zhang, Xinxin Lu
BioMed Research International.2017; 2017: 1. CrossRef - Primary Appendicular Tuberculosis
Vipul D Yagnik
Gastroenterology & Hepatology: Open Access.2017;[Epub] CrossRef
-
The Need for Persistence in the Diagnosis of Mycobacterium Tuberculosis Mono-arthritis: A Unique Case Presentation
- Detection of Human Papillomavirus in Korean Breast Cancer Patients by Real-Time Polymerase Chain Reaction and Meta-Analysis of Human Papillomavirus and Breast Cancer
- Jinhyuk Choi, Chungyeul Kim, Hye Seung Lee, Yoo Jin Choi, Ha Yeon Kim, Jinhwan Lee, Hyeyoon Chang, Aeree Kim
- J Pathol Transl Med. 2016;50(6):442-450. Published online October 10, 2016
- DOI: https://doi.org/10.4132/jptm.2016.07.08
- 14,431 View
- 225 Download
- 16 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) is a well-established oncogenic virus of cervical, anogenital, and oropharyngeal cancer. Various subtypes of HPV have been detected in 0% to 60% of breast cancers. The roles of HPV in the carcinogenesis of breast cancer remain controversial. This study was performed to determine the prevalence of HPV-positive breast cancer in Korean patients and to evaluate the possibility of carcinogenic effect of HPV on breast.
Methods
Meta-analysis was performed in 22 case-control studies for HPV infection in breast cancer. A total of 123 breast cancers, nine intraductal papillomas and 13 nipple tissues of patients with proven cervical HPV infection were tested by real-time polymerase chain reaction to detect 28 subtypes of HPV. Breast cancers were composed of 106 formalin-fixed and paraffin embedded (FFPE) breast cancer samples and 17 touch imprint cytology samples of breast cancers.
Results
The overall odds ratio between breast cancer and HPV infection was 5.43 (95% confidence interval, 3.24 to 9.12) with I2 = 34.5% in meta-analysis of published studies with case-control setting and it was statistically significant. HPV was detected in 22 cases of breast cancers (17.9%) and two cases of intaductal papillomas (22.2%). However, these cases had weak positivity.
Conclusions
These results failed to serve as significant evidence to support the relationship between HPV and breast cancer. Further study with larger epidemiologic population is merited to determine the relationship between HPV and breast cancer. -
Citations
Citations to this article as recorded by- HPV, APOBEC3B, and the origins of breast cancer: a narrative review and perspectives on novel mechanisms
Zhi-yong Liu, Ran Chen
Frontiers in Oncology.2026;[Epub] CrossRef - Advances in human papillomavirus detection for cervical cancer screening and diagnosis: challenges of conventional methods and opportunities for emergent tools
O. Fashedemi, Okoroike C. Ozoemena, Siwaphiwe Peteni, Aderemi B. Haruna, Leshweni J. Shai, Aicheng Chen, Frankie Rawson, Maggie E. Cruickshank, David Grant, Oluwafunmilola Ola, Kenneth I. Ozoemena
Analytical Methods.2025; 17(7): 1428. CrossRef - Bacterial-Viral Interactions in Human Orodigestive and Female Genital Tract Cancers: A Summary of Epidemiologic and Laboratory Evidence
Ikuko Kato, Jilei Zhang, Jun Sun
Cancers.2022; 14(2): 425. CrossRef - Breast cancer association with oncogenic papillomaviruses: papillomaviral DNA detection in breast cancer cells
G. M. Volgareva
Advances in Molecular Oncology.2022; 9(2): 10. CrossRef - Presence of Human Papillomavirus DNA in Malignant Neoplasia and Non-Malignant Breast Disease
Erika Maldonado-Rodríguez, Marisa Hernández-Barrales, Adrián Reyes-López, Susana Godina-González, Perla I. Gallegos-Flores, Edgar L. Esparza-Ibarra, Irma E. González-Curiel, Jesús Aguayo-Rojas, Adrián López-Saucedo, Gretel Mendoza-Almanza, Jorge L. Ayala-
Current Issues in Molecular Biology.2022; 44(8): 3648. CrossRef - Risk Role of Breast Cancer in Association with Human Papilloma Virus among Female Population in Taiwan: A Nationwide Population-Based Cohort Study
Chia-Hsin Liu, Chi-You Liao, Ming-Hsin Yeh, James Cheng-Chung Wei
Healthcare.2022; 10(11): 2235. CrossRef - HPV-Associated Breast Cancer: Myth or Fact?
Erik Kudela, Eva Kudelova, Erik Kozubík, Tomas Rokos, Terezia Pribulova, Veronika Holubekova, Kamil Biringer
Pathogens.2022; 11(12): 1510. CrossRef - Assessment of Human Papillomavirus Infection and Risk Factors in Egyptian Women With Breast Cancer
Nabila El-Sheikh, Nahla O Mousa, Amany M Tawfeik, Alaa M Saleh, Iman Elshikh, Mohamed Deyab, Faten Ragheb, Manar M Moneer, Ahmed Kawashti, Ahmed Osman, Mohamed Elrefaei
Breast Cancer: Basic and Clinical Research.2021;[Epub] CrossRef - Human Papillomavirus (HPV) Detection by Chromogenic In Situ Hybridization (CISH) and p16 Immunohistochemistry (IHC) in Breast Intraductal Papilloma and Breast Carcinoma
Hua Guo, Juan P. Idrovo, Jin Cao, Sudarshana Roychoudhury, Pooja Navale, Louis J. Auguste, Tawfiqul Bhuiya, Silvat Sheikh-Fayyaz
Clinical Breast Cancer.2021; 21(6): e638. CrossRef - Human Papillomavirus in Breast Carcinogenesis: A Passenger, a Cofactor, or a Causal Agent?
Rancés Blanco, Diego Carrillo-Beltrán, Juan P. Muñoz, Alejandro H. Corvalán, Gloria M. Calaf, Francisco Aguayo
Biology.2021; 10(8): 804. CrossRef - Systematic review and meta-analysis of the papillomavirus prevalence in breast cancer fresh tissues
Geilson Gomes de Oliveira, Ana Katherine Gonçalves, José Eleutério, Luiz Gonzaga Porto Pinheiro
Breast Disease.2021; 41(1): 123. CrossRef - Is human papillomavirus associated with breast cancer or papilloma presenting with pathologic nipple discharge?
Fatih Levent Balci, Cihan Uras, Sheldon Marc Feldman
Cancer Treatment and Research Communications.2019; 19: 100122. CrossRef - Is the HPV virus responsible for the development of breast cancer?
Erik Kudela, Marcela Nachajova, Jan Danko
The Breast Journal.2019; 25(5): 1053. CrossRef - Absence of Human Papillomavirus in Benign and Malignant Breast Tissue
Maryam Kazemi Aghdam, Seyed Alireza Nadji, Azadeh Alvandimanesh, Maliheh Khoddami, Yassaman Khademi
Iranian Journal of Pathology.2019; 14(4): 279. CrossRef - Oncogenic Viruses and Breast Cancer: Mouse Mammary Tumor Virus (MMTV), Bovine Leukemia Virus (BLV), Human Papilloma Virus (HPV), and Epstein–Barr Virus (EBV)
James S. Lawson, Brian Salmons, Wendy K. Glenn
Frontiers in Oncology.2018;[Epub] CrossRef - Viral infections and breast cancer – A current perspective
O.M. Gannon, A. Antonsson, I.C. Bennett, N.A. Saunders
Cancer Letters.2018; 420: 182. CrossRef - Prevalence of EBV, HPV and MMTV in Pakistani breast cancer patients: A possible etiological role of viruses in breast cancer
Wasifa Naushad, Orooj Surriya, Hajra Sadia
Infection, Genetics and Evolution.2017; 54: 230. CrossRef
- HPV, APOBEC3B, and the origins of breast cancer: a narrative review and perspectives on novel mechanisms
- Non-small Cell Lung Cancer with Concomitant EGFR, KRAS, and ALK Mutation: Clinicopathologic Features of 12 Cases
- Taebum Lee, Boram Lee, Yoon-La Choi, Joungho Han, Myung-Ju Ahn, Sang-Won Um
- J Pathol Transl Med. 2016;50(3):197-203. Published online April 18, 2016
- DOI: https://doi.org/10.4132/jptm.2016.03.09
- 22,394 View
- 319 Download
- 72 Web of Science
- 65 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Although epidermal growth factor receptor (EGFR), v-Ki-ras2 Kirsten rat sarcoma viral oncogene (KRAS), and anaplastic lymphoma kinase (ALK) mutations in non-small cell lung cancer (NSCLC) were thought to be mutually exclusive, some tumors harbor concomitant mutations. Discovering a driver mutation on the basis of morphologic features and therapeutic responses with mutation analysis can be used to understand pathogenesis and predict resistance in targeted therapy.
Methods
In 6,637 patients with NSCLC, 12 patients who had concomitant mutations were selected and clinicopathologic features were reviewed. Clinical characteristics included sex, age, smoking history, previous treatment, and targeted therapy with response and disease-free survival. Histologic features included dominant patterns, nuclear and cytoplasmic features.
Results
All patients were diagnosed with adenocarcinoma and had an EGFR mutation. Six patients had concomitant KRAS mutations and the other six had ALK mutations. Five of six EGFR-KRAS mutation patients showed papillary and acinar histologic patterns with hobnail cells. Three of six received EGFR tyrosine kinase inhibitor (TKI) and showed partial response for 7–29 months. All six EGFR-ALK mutation patients showed solid or cribriform patterns and three had signet ring cells. Five of six EGFR-ALK mutation patients received EGFR TKI and/or ALK inhibitor and four showed partial response or stable disease, except for one patient who had acquired an EGFR mutation.
Conclusions
EGFR and ALK mutations play an important role as driver mutations in double mutated NSCLC, and morphologic analysis can be used to predict treatment response. -
Citations
Citations to this article as recorded by- Integrative multi-omics machine learning reveals novel driver genes associations in lung adenocarcinoma
Fei Yuan, FeiMing Huang, Xiaoyu Cao, Yu-Hang Zhang, KaiYan Feng, YuSheng Bao, Tao Huang, Yu-Dong Cai
Biochimica et Biophysica Acta (BBA) - Proteins and Proteomics.2026; 1874(1): 141113. CrossRef - Ensartinib for EML4-ALK-positive lung adenocarcinoma with comorbid mutations in TP53, EGFR, and ERBB2: a case report
Xiaoqing Huang, Lingxian Zhou, Jianyong Xia, Haifeng Jian, Jinji Liu, Yunying Huang, Qingsheng Chen
Frontiers in Oncology.2025;[Epub] CrossRef - Dual EGFR L858R and KRAS G12A Mutations in Lung Adenocarcinoma: A Rare Case Report and Literature Review
Gang Wei, Jun Tang, Huaiwen Wang, Dongdong Zhang
Pharmacogenomics and Personalized Medicine.2025; Volume 18: 189. CrossRef -
Artificial Intelligence in Lung Cancer Imaging: From Data to Therapy
Michaela Cellina, Giuseppe De Padova, Nazarena Caldarelli, Dario Libri, Maurizio Cè, Carlo Martinenghi, Marco Alì, Sergio Papa, Gianpaolo Carrafiello
Critical Reviews™ in Oncogenesis.2024; 29(2): 1. CrossRef - Artificial Intelligence for Cardiothoracic Imaging: Overview of Current and Emerging Applications
Bruno Hochhegger, Romulo Pasini, Alysson Roncally Carvalho, Rosana Rodrigues, Stephan Altmayer, Leonardo Kayat Bittencourt, Edson Marchiori, Reza Forghani
Seminars in Roentgenology.2023; 58(2): 184. CrossRef - Genomic Landscape of Primary Resistance to Osimertinib Among Hispanic Patients with EGFR-Mutant Non-Small Cell Lung Cancer (NSCLC): Results of an Observational Longitudinal Cohort Study
Diego F. Chamorro, Andrés F. Cardona, July Rodríguez, Alejandro Ruiz-Patiño, Oscar Arrieta, Darwin A. Moreno-Pérez, Leonardo Rojas, Zyanya Lucia Zatarain-Barrón, Dora V. Ardila, Lucia Viola, Gonzalo Recondo, Juan B. Blaquier, Claudio Martín, Luis Raez, Su
Targeted Oncology.2023; 18(3): 425. CrossRef - Histone deacetylase inhibitor belinostat regulates metabolic reprogramming in killing KRAS‐mutant human lung cancer cells
Rebecca M. Peter, Md. Shahid Sarwar, Sarah Z. Mostafa, Yujue Wang, Xiaoyang Su, Ah‐Ng Kong
Molecular Carcinogenesis.2023; 62(8): 1136. CrossRef - Differential Distribution of Brain Metastases from Non-Small Cell Lung Cancer Based on Mutation Status
Bihong T. Chen, Taihao Jin, Ningrong Ye, Sean W. Chen, Russell C. Rockne, Stephanie Yoon, Isa Mambetsariev, Ebenezer Daniel, Ravi Salgia
Brain Sciences.2023; 13(7): 1057. CrossRef - Clinicopathological features and prognostic significance of pulmonary adenocarcinoma with signet ring cell components: meta-analysis and SEER analysis
Yang Tan, Ying-he Huang, Jia-wen Xue, Rui Zhang, Run Liu, Yan Wang, Zhen-Bo Feng
Clinical and Experimental Medicine.2023; 23(8): 4341. CrossRef - Ganoderma microsporum immunomodulatory protein as an extracellular epidermal growth factor receptor (EGFR) degrader for suppressing EGFR-positive lung cancer cells
Wei-Jyun Hua, Hsin Yeh, Zhi-Hu Lin, Ai-Jung Tseng, Li-Chen Huang, Wei-Lun Qiu, Tsung-Hsi Tu, Ding-Han Wang, Wei-Hung Hsu, Wei-Lun Hwang, Tung-Yi Lin
Cancer Letters.2023; 578: 216458. CrossRef - Next generation sequencing for detection of EGFR alterations in NSCLC: is more better?
Ullas Batra, Shrinidhi Nathany, Mansi Sharma, Parveen Jain, Anurag Mehta
Journal of Clinical Pathology.2022; 75(3): 164. CrossRef - Enkurin domain containing 1 (ENKD1) regulates the proliferation, migration and invasion of non‐small cell lung cancer cells
Ting Song, Peng Zhou, Chunjiao Sun, Na He, Haixia Li, Jie Ran, Jun Zhou, Yue Wu, Min Liu
Asia-Pacific Journal of Clinical Oncology.2022;[Epub] CrossRef - Targeting Mutant Kirsten Rat Sarcoma Viral Oncogene Homolog in Non-Small Cell Lung Cancer: Current Difficulties, Integrative Treatments and Future Perspectives
Jia-Xin Li, Run-Ze Li, Lin-Rui Ma, Peng Wang, Dong-Han Xu, Jie Huang, Li-Qi Li, Ling Tang, Ying Xie, Elaine Lai-Han Leung, Pei-Yu Yan
Frontiers in Pharmacology.2022;[Epub] CrossRef - Histone H3K9 methyltransferase SETDB1 augments invadopodia formation to promote tumor metastasis
Shuhei Ueshima, Jia Fang
Oncogene.2022; 41(24): 3370. CrossRef - ESMO expert consensus statements on the management of EGFR mutant non-small-cell lung cancer
A. Passaro, N. Leighl, F. Blackhall, S. Popat, K. Kerr, M.J. Ahn, M.E. Arcila, O. Arrieta, D. Planchard, F. de Marinis, A.M. Dingemans, R. Dziadziuszko, C. Faivre-Finn, J. Feldman, E. Felip, G. Curigliano, R. Herbst, P.A. Jänne, T. John, T. Mitsudomi, T.
Annals of Oncology.2022; 33(5): 466. CrossRef - Molecular Targets in Lung Cancer: Study of the Evolution of Biomarkers Associated with Treatment with Tyrosine Kinase Inhibitors—Has NF1 Tumor Suppressor a Key Role in Acquired Resistance?
Begoña O. Alen, Lara S. Estévez-Pérez, María Teresa Hermida-Romero, Ana Reguera-Arias, Rosario García-Campelo, Mercedes de la Torre-Bravos, Ángel Concha
Cancers.2022; 14(14): 3323. CrossRef - Analytical and clinical validation of a custom 15-gene next-generation sequencing panel for the evaluation of circulating tumor DNA mutations in patients with advanced non-small-cell lung cancer
Yock Ping Chow, Norziha Zainul Abidin, Ken Siong Kow, Lye Mun Tho, Chieh Lee Wong, Rama Krishna Kancha
PLOS ONE.2022; 17(10): e0276161. CrossRef - Potential Therapeutic Strategy for EGFR-Mutant Lung Cancer With Concomitant EML4-ALK Rearrangement—Combination of EGFR Tyrosine Kinase Inhibitors and ALK Inhibitors
Ming-Hung Huang, Jih-Hsiang Lee, Pei-Shan Hung, James Chih-Hsin Yang
JTO Clinical and Research Reports.2022; 3(11): 100405. CrossRef - Artificial Intelligence in Lung Cancer Imaging: Unfolding the Future
Michaela Cellina, Maurizio Cè, Giovanni Irmici, Velio Ascenti, Natallia Khenkina, Marco Toto-Brocchi, Carlo Martinenghi, Sergio Papa, Gianpaolo Carrafiello
Diagnostics.2022; 12(11): 2644. CrossRef - A single center analysis of first-line treatment in advanced KRAS mutant non-small cell lung cancer: real-world practice
Yanxia Liu, Yuan Gao, Ying Wang, Cong Zhao, Zhiyun Zhang, Baolan Li, Tongmei Zhang
BMC Cancer.2022;[Epub] CrossRef - High frequency of KRAS and EGFR mutation profiles in BRAF-negative thyroid carcinomas in Indonesia
Didik Setyo Heriyanto, Vincent Laiman, Nikko Vanda Limantara, Widyan Putra Anantawikrama, Fara Silvia Yuliani, Rita Cempaka, Sumadi Lukman Anwar
BMC Research Notes.2022;[Epub] CrossRef - Kirsten Rat Sarcoma Mutation in South Indians with Non-Small Lung Cancer
Gautam Balaram, Renjan Thomas, Suhas N. Ghorpade, Prarthana V. Kowsik, Baby Dharman, Yogesh Shivakumar, Shekar Patil, Satheesh Chiradoni Thungappa, HP Shashidhara, Somorat Bhattacharjee, Sridhar Papaiah Susheela, Radheshyam Naik, Srinivas Belagutty Jayapp
Journal of Precision Oncology.2022; 2(1): 3. CrossRef - Targeted next-generation sequencing for cancer-associated gene mutation and copy number detection in 206 patients with non–small-cell lung cancer
Songbai Zheng, Xiaodan Wang, Ying Fu, Beibei Li, Jianhua Xu, Haifang Wang, Zhen Huang, Hui Xu, Yurong Qiu, Yaozhou Shi, Kui Li
Bioengineered.2021; 12(1): 791. CrossRef - How mathematical modeling could contribute to the quantification of metastatic tumor burden under therapy: insights in immunotherapeutic treatment of non-small cell lung cancer
Pirmin Schlicke, Christina Kuttler, Christian Schumann
Theoretical Biology and Medical Modelling.2021;[Epub] CrossRef - A case of concomitant EGFR/ALK alteration against a mutated EGFR background in early-stage lung adenocarcinoma
Ki-Chang Lee, Jiwon Koh, Doo Hyun Chung, Yoon Kyung Jeon
Journal of Pathology and Translational Medicine.2021; 55(2): 139. CrossRef - Malfeasance of KRAS mutations in carcinogenesis
Rupal Tripathi, Shrinidhi Nathany, Anurag Mehta, Ullas Batra, Sakshi Mattoo, Mansi Sharma
Clinical and Experimental Medicine.2021; 21(3): 439. CrossRef - Detection of Low-Frequency KRAS Mutations in cfDNA From EGFR-Mutated NSCLC Patients After First-Line EGFR Tyrosine Kinase Inhibitors
Giorgia Nardo, Jessica Carlet, Ludovica Marra, Laura Bonanno, Alice Boscolo, Alessandro Dal Maso, Andrea Boscolo Bragadin, Stefano Indraccolo, Elisabetta Zulato
Frontiers in Oncology.2021;[Epub] CrossRef - Non-Small Cell Lung Cancer Harboring Concurrent EGFR Genomic Alterations: A Systematic Review and Critical Appraisal of the Double Dilemma
Valerio Gristina, Maria La Mantia, Antonio Galvano, Sofia Cutaia, Nadia Barraco, Marta Castiglia, Alessandro Perez, Marco Bono, Federica Iacono, Martina Greco, Katia Calcara, Valentina Calò, Sergio Rizzo, Lorena Incorvaia, Maria Chiara Lisanti, Giulia San
Journal of Molecular Pathology.2021; 2(2): 173. CrossRef - Testing for EGFR Mutations and ALK Rearrangements in Advanced Non-Small-Cell Lung Cancer: Considerations for Countries in Emerging Markets
Mercedes L Dalurzo, Alejandro Avilés-Salas, Fernando Augusto Soares, Yingyong Hou, Yuan Li, Anna Stroganova, Büge Öz, Arif Abdillah, Hui Wan, Yoon-La Choi
OncoTargets and Therapy.2021; Volume 14: 4671. CrossRef - Untangling the KRAS mutated lung cancer subsets and its therapeutic implications
Kulshrestha Ritu, Pawan Kumar, Amit Singh, K. Nupur, Sonam Spalgias, Parul Mrigpuri, Rajkumar
Molecular Biomedicine.2021;[Epub] CrossRef - Lorlatinib Induces Durable Disease Stabilization in a Pancreatic Cancer Patient with a ROS1 p.L1950F Mutation: Case Report
Janna-Lisa Velthaus, Peter Iglauer, Ronald Simon, Carsten Bokemeyer, Peter Bannas, Niklas Beumer, Charles D. Imbusch, Eray Goekkurt, Sonja Loges
Oncology Research and Treatment.2021; 44(9): 495. CrossRef - Proteasome-dependent degradation of Smad7 is critical for lung cancer metastasis
Lu Tong, Shihui Shen, Quan Huang, Junjiang Fu, Tianzhen Wang, Linian Pan, Pei Zhang, Geng Chen, Tingmei Huang, Ke Li, Qingwu Liu, Shaofang Xie, Xiao Yang, Robb E. Moses, Xiaotao Li, Lei Li
Cell Death & Differentiation.2020; 27(6): 1795. CrossRef - Circulating Cell-Free Dna As A Diagnostic and Prognostic Biomarker for Non-Small-Cell Lung Cancer: A Systematic Review and Meta-Analysis
Zhoumiao Chen, Huiwen Miao, Qingxin Zeng, Shaohua Xu, Zhao Chen, Kai Liu
Biomarkers in Medicine.2020; 14(7): 587. CrossRef - Influence of EGFR-activating mutations on sensitivity to tyrosine kinase inhibitors in a KRAS mutant non-small cell lung cancer cell line
Yoshinori Tsukumo, Mikihiko Naito, Takayoshi Suzuki, Srikumar Chellappan
PLOS ONE.2020; 15(3): e0229712. CrossRef - KRAS oncogene may be another target conquered in non‐small cell lung cancer (NSCLC)
Hanxiao Chen, Jun Zhao
Thoracic Cancer.2020; 11(12): 3425. CrossRef - Epidemiologic Features of NSCLC Gene Alterations in Hispanic Patients from Puerto Rico
Ruifang Zheng, Zhiwei Yin, Albert Alhatem, Derek Lyle, Bei You, Andrew S. Jiang, Dongfang Liu, Zsolt Jobbagy, Qing Wang, Seena Aisner, Jie-Gen Jiang
Cancers.2020; 12(12): 3492. CrossRef - Comprehensive pancancer genomic analysis reveals (RTK)-RAS-RAF-MEK as a key dysregulated pathway in cancer: Its clinical implications
Robin Imperial, Omer M Toor, Arif Hussain, Janakiraman Subramanian, Ashiq Masood
Seminars in Cancer Biology.2019; 54: 14. CrossRef - Epidermal growth factor receptor (EGFR), KRAS, and BRAF mutations in lung adenocarcinomas: A study from India
Varsha Singh, Prerna Guleria, Prabhat Singh Malik, Anant Mohan, Sanjay Thulkar, R M Pandey, Kalpana Luthra, Sudheer Arava, Ruma Ray, Deepali Jain
Current Problems in Cancer.2019; 43(5): 391. CrossRef - Clinical Validation of Coexisting Activating Mutations Within EGFR, Mitogen-Activated Protein Kinase, and Phosphatidylinositol 3-Kinase Pathways in Lung Cancers
Federico De Marchi, Lisa Haley, Henderson Fryer, Junaid Ibrahim, Katie Beierl, Gang Zheng, Christopher D. Gocke, James R. Eshleman, Deborah Belchis, Peter Illei, Ming-Tseh Lin
Archives of Pathology & Laboratory Medicine.2019; 143(2): 174. CrossRef - A sequential Monte Carlo algorithm for inference of subclonal structure in cancer
Oyetunji E. Ogundijo, Kaiyi Zhu, Xiaodong Wang, Dimitris Anastassiou, Xiang Li
PLOS ONE.2019; 14(1): e0211213. CrossRef - The Presence of Concomitant Mutations Affects the Activity of EGFR Tyrosine Kinase Inhibitors in EGFR-Mutant Non-Small Cell Lung Cancer (NSCLC) Patients
Anna Rachiglio, Francesca Fenizia, Maria Piccirillo, Domenico Galetta, Lucio Crinò, Bruno Vincenzi, Emiddio Barletta, Carmine Pinto, Francesco Ferraù, Matilde Lambiase, Agnese Montanino, Cristin Roma, Vienna Ludovini, Elisabetta Montagna, Antonella De Luc
Cancers.2019; 11(3): 341. CrossRef - Concurrent Driver Gene Mutations as Negative Predictive Factors in Epidermal Growth Factor Receptor-Positive Non-Small Cell Lung Cancer
Minjiang Chen, Yan Xu, Jing Zhao, Wei Zhong, Li Zhang, Yalan Bi, Mengzhao Wang
EBioMedicine.2019; 42: 304. CrossRef - Anaplastic Lymphoma Kinase (ALK)-positive Tumors
Rohan Gupta, Idoroenyi Amanam, Syed Rahmanuddin, Isa Mambetsariev, Yingyu Wang, Charity Huang, Karen Reckamp, Lalit Vora, Ravi Salgia
American Journal of Clinical Oncology.2019; 42(4): 337. CrossRef - Clinical features and therapeutic options in non‐small cell lung cancer patients with concomitant mutations of EGFR, ALK, ROS1, KRAS or BRAF
Xibin Zhuang, Chao Zhao, Jiayu Li, Chunxia Su, Xiaoxia Chen, Shengxiang Ren, Xuefei Li, Caicun Zhou
Cancer Medicine.2019; 8(6): 2858. CrossRef - Intrinsic Resistance to EGFR-Tyrosine Kinase Inhibitors in EGFR-Mutant Non-Small Cell Lung Cancer: Differences and Similarities with Acquired Resistance
Eric Santoni-Rugiu, Linea C. Melchior, Edyta M. Urbanska, Jan N. Jakobsen, Karin de Stricker, Morten Grauslund, Jens B. Sørensen
Cancers.2019; 11(7): 923. CrossRef - Clinical outcome of treatment of metastatic non-small cell lung cancer in patients harboring uncommon EGFR mutation
J. Chantharasamee, N. Poungvarin, P. Danchaivijitr, S. Techawatanawanna
BMC Cancer.2019;[Epub] CrossRef - Deregulated lncRNA expression profile in the mouse lung adenocarcinomas with KRAS‐G12D mutation and P53 knockout
Meiqin Zhang, Nan Jiang, Renjie Cui, Sichen Du, Huayuan Ou, Tinglan Chen, Runsheng Ge, Duan Ma, Jin Zhang
Journal of Cellular and Molecular Medicine.2019; 23(10): 6978. CrossRef - Open-Sourced CIViC Annotation Pipeline to Identify and Annotate Clinically Relevant Variants Using Single-Molecule Molecular Inversion Probes
Erica K. Barnell, Adam Waalkes, Matt C. Mosior, Kelsi Penewit, Kelsy C. Cotto, Arpad M. Danos, Lana M. Sheta, Katie M. Campbell, Kilannin Krysiak, Damian Rieke, Nicholas C. Spies, Zachary L. Skidmore, Colin C. Pritchard, Todd A. Fehniger, Ravindra Uppalur
JCO Clinical Cancer Informatics.2019; (3): 1. CrossRef - EGFR, KRAS, BRAF, ALK, and cMET genetic alterations in 1440 Sardinian patients with lung adenocarcinoma
Maria Colombino, Panagiotis Paliogiannis, Antonio Cossu, Davide Adriano Santeufemia, Maria Cristina Sini, Milena Casula, Grazia Palomba, Antonella Manca, Marina Pisano, Valentina Doneddu, Giuseppe Palmieri
BMC Pulmonary Medicine.2019;[Epub] CrossRef - Concomitant Presence of EGFR and ALK Fusion Gene Mutation in Adenocarcinoma of Lung: A Case Report and Review of the Literature
Nishitha Thumallapally, Hana Yu, Mohammad Farhan, Uroosa Ibrahim, Maricel Odiami
Journal of Pharmacy Practice.2018; 31(2): 244. CrossRef - Double Trouble: A Case Series on Concomitant Genetic Aberrations in NSCLC
Nele Van Der Steen, Yves Mentens, Marc Ramael, Leticia G. Leon, Paul Germonpré, Jose Ferri, David R. Gandara, Elisa Giovannetti, Godefridus J. Peters, Patrick Pauwels, Christian Rolfo
Clinical Lung Cancer.2018; 19(1): 35. CrossRef - KRAS oncogene in non-small cell lung cancer: clinical perspectives on the treatment of an old target
Marta Román, Iosune Baraibar, Inés López, Ernest Nadal, Christian Rolfo, Silvestre Vicent, Ignacio Gil-Bazo
Molecular Cancer.2018;[Epub] CrossRef - Pulmonary Adenocarcinoma, Harboring Both an EGFR Mutation and ALK Rearrangement, Presenting a Stable Disease to Erlotinib and a Partial Response to Alectinib
Akira Yokoyama, Atsuhisa Tamura, Kazuko Miyakawa, Kei Kusaka, Masahiro Shimada, Takashi Hirose, Hirotoshi Matsui, Masashi Kitani, Akira Hebisawa, Ken Ohta
Internal Medicine.2018; 57(16): 2377. CrossRef - Long-term survival with erlotinib in advanced lung adenocarcinoma harboring synchronous EGFR G719S and KRAS G12C mutations
Biagio Ricciuti, Sara Baglivo, Vienna Ludovini, Angelo Sidoni, Giulio Metro, Marta Brambilla, Annamaria Siggillino, Maria Sole Reda, Alberto Rebonato, Daniele Maiettini, Rita Chiari
Lung Cancer.2018; 120: 70. CrossRef - Concomitant driver mutations in advanced EGFR-mutated non-small-cell lung cancer and their impact on erlotinib treatment
Jan Nyrop Jakobsen, Eric Santoni-Rugiu, Morten Grauslund, Linea Melchior, Jens Benn Sørensen
Oncotarget.2018; 9(40): 26195. CrossRef - Implications of KRAS mutations in acquired resistance to treatment in NSCLC
Marzia Del Re, Eleonora Rofi, Giuliana Restante, Stefania Crucitta, Elena Arrigoni, Stefano Fogli, Massimo Di Maio, Iacopo Petrini, Romano Danesi
Oncotarget.2018; 9(5): 6630. CrossRef - Alk Immunohistochemistry is Highly Sensitive and Specific for the Detection of Alk Translocated Lung Adenocarcinomas: Lessons from An Audit of Lung Cancer Molecular Testing
YC Kheng, K Walsh, L Williams, WA Wallace, DJ Harrison, A Oniscu
Journal of the Royal College of Physicians of Edinburgh.2018; 48(1): 20. CrossRef - Targeting KRAS mutated non-small cell lung cancer: A history of failures and a future of hope for a diverse entity
Alexios Matikas, Dimitrios Mistriotis, Vasilios Georgoulias, Athanasios Kotsakis
Critical Reviews in Oncology/Hematology.2017; 110: 1. CrossRef - Clinical Outcome of ALK -Positive Non–Small Cell Lung Cancer (NSCLC) Patients with De Novo EGFR or KRAS Co-Mutations Receiving Tyrosine Kinase Inhibitors (TKIs)
Sabine Schmid, Oliver Gautschi, Sacha Rothschild, Michael Mark, Patrizia Froesch, Dirk Klingbiel, Hermann Reichegger, Wolfram Jochum, Joachim Diebold, Martin Früh
Journal of Thoracic Oncology.2017; 12(4): 681. CrossRef - EGFR and KRAS molecular genotyping for pulmonary carcinomas: Feasibility of a simple and rapid technique implementable in any department of pathology
Vincent Thomas De Montpréville, Maria-Rosa Ghigna, Ludovic Lacroix, Antoinette Lemoine, Benjamin Besse, Olaf Mercier, Élie Fadel, Peter Dorfmuller, Thierry Le Chevalier
Pathology - Research and Practice.2017; 213(7): 793. CrossRef - MET Exon 14 Skipping Mutations in Lung Adenocarcinoma: Clinicopathologic Implications and Prognostic Values
Geun Dong Lee, Seung Eun Lee, Doo-Yi Oh, Dan-bi Yu, Hae Min Jeong, Jooseok Kim, Sungyoul Hong, Hun Soon Jung, Ensel Oh, Ji-Young Song, Mi-Sook Lee, Mingi Kim, Kyungsoo Jung, Jhingook Kim, Young Kee Shin, Yoon-La Choi, Hyeong Ryul Kim
Journal of Thoracic Oncology.2017; 12(8): 1233. CrossRef - Non-Small-Cell Lung Cancer (NSCLC) Harboring ALK Translocations: Clinical Characteristics and Management in a Real-Life Setting: a French Retrospective Analysis (GFPC 02–14 Study)
Jean-Bernard Auliac, Isabelle Monnet, Catherine Dubos-Arvis, Anne Marie Chiappa, Nathalie Baize, Suzana Bota, Alain Vergnenegre, Helene Doubre, Chrystele Locher, Acya Bizieux, Gilles Robinet, Christos Chouaid
Targeted Oncology.2017; 12(6): 833. CrossRef - Concomitant EML4-ALK rearrangement and EGFR mutation in non-small cell lung cancer patients: a literature review of 100 cases
Giuseppe Lo Russo, Martina Imbimbo, Giulia Corrao, Claudia Proto, Diego Signorelli, Milena Vitali, Monica Ganzinelli, Laura Botta, Nicoletta Zilembo, Filippo de Braud, Marina Chiara Garassino
Oncotarget.2017; 8(35): 59889. CrossRef - Management of non-small cell lung cancer in the era of personalized medicine
Gaetano Rocco, Alessandro Morabito, Alessandra Leone, Paolo Muto, Francesco Fiore, Alfredo Budillon
The International Journal of Biochemistry & Cell Biology.2016; 78: 173. CrossRef - A long-term survivor of non-small-cell lung cancer harboring concomitant EGFR mutation and ALK translocation
Fumio Imamura, Takako Inoue, Madoka Kimura, Kazumi Nishino, Toru Kumagai
Respiratory Medicine Case Reports.2016; 19: 137. CrossRef
- Integrative multi-omics machine learning reveals novel driver genes associations in lung adenocarcinoma
- Effectiveness and Limitations of Core Needle Biopsy in the Diagnosis of Thyroid Nodules: Review of Current Literature
- Jung Hyun Yoon, Eun-Kyung Kim, Jin Young Kwak, Hee Jung Moon
- J Pathol Transl Med. 2015;49(3):230-235. Published online May 15, 2015
- DOI: https://doi.org/10.4132/jptm.2015.03.21
- 14,189 View
- 114 Download
- 54 Web of Science
- 52 Crossref
-
 Abstract
Abstract
 PDF
PDF - Fine needle aspiration (FNA) is currently accepted as an easy, safe, and reliable tool for the diagnosis of thyroid nodules. Nonetheless, a proportion of FNA samples are categorized into non-diagnostic or indeterminate cytology, which frustrates both the clinician and patient. To overcome this limitation of FNA, core needle biopsy (CNB) of the thyroid has been proposed as an additional diagnostic method for more accurate and decisive diagnosis for thyroid nodules of concern. In this review, we focus on the effectiveness and limitations of CNB, and what factors should be considered when CNB is utilized in the diagnosis of thyroid nodules.
-
Citations
Citations to this article as recorded by- Reevaluation of malignancy risk in nondiagnostic thyroid nodules with long‐term follow‐up via surgical resection or core needle biopsy: A retrospective study
Ji‐Seon Jeong, Young Jun Choi, Jeong Hyun Lee, Jung Hwan Baek, Yu‐Mi Lee, Tae‐Yon Sung, Dong Eun Song
Cancer Cytopathology.2026;[Epub] CrossRef - Biopsy Needle Integrated with Rotational Oblique Spectral Ultrasound (ROSUS) Imaging
Benjamin C. Kreager, Wei-Yi Chang, Jian Tian, Huaiyu Wu, Xiaoning Jiang
Sensors.2026; 26(4): 1098. CrossRef - Core needle biopsy as a first-line diagnostic tool for selected thyroid nodules: a real-world evaluation of diagnostic performance and safety
Xing Li, Yi Pan, Yanmei Ou, Xin Gao, Yue Gao, Luwei Liu, Yinze Li, Yong Xu, Wengui Xu
Frontiers in Oncology.2026;[Epub] CrossRef - Diagnostic yield of fine needle aspiration with simultaneous core needle biopsy for thyroid nodules
Mohammad Ali Hasannia, Ramin Pourghorban, Hoda Asefi, Amir Aria, Elham Nazar, Hojat Ebrahiminik, Alireza Mohamadian
Journal of Pathology and Translational Medicine.2025; 59(3): 180. CrossRef - A comparative analysis of core needle biopsy and repeat fine needle aspiration in patients with inconclusive initial cytology of thyroid nodules
Xuejiao Su, Can Yue, Wanting Yang, Buyun Ma
Frontiers in Endocrinology.2024;[Epub] CrossRef - High-Performance PMN-PT Single-Crystal-Based 1-3 Composite Transducer Integrated with a Biopsy Needle
Benjamin C. Kreager, Huaiyu Wu, Wei-Yi Chang, Sunho Moon, Josh Mitchell, Chang Peng, Chih-Chung Huang, Marie Muller, Jian Tian, Xiaoning Jiang
Biosensors.2024; 14(2): 74. CrossRef - TSE-GAN: strain elastography using generative adversarial network for thyroid disease diagnosis
Anping Song, Tianyi Li, Xuehai Ding, Mingye Wu, Ren Wang
Frontiers in Bioengineering and Biotechnology.2024;[Epub] CrossRef - Ultrasound Elastography: Methods, Clinical Applications, and Limitations: A Review Article
Ammar A. Oglat, Tala Abukhalil
Applied Sciences.2024; 14(10): 4308. CrossRef - Fine-Needle Aspiration versus the CytoCore® Motorized Rotating Needle Device for Thyroid Nodule Biopsies: A Retrospective Cohort Study
Adarsh Verma, Rhonda McDowell, Anthony Porreca
Acta Cytologica.2024; 68(5): 405. CrossRef - Ultrasound Elastography: Basic Principles and Examples of Clinical Applications with Artificial Intelligence—A Review
Maurizio Cè, Natascha Claudia D'Amico, Giulia Maria Danesini, Chiara Foschini, Giancarlo Oliva, Carlo Martinenghi, Michaela Cellina
BioMedInformatics.2023; 3(1): 17. CrossRef - Histology-based and cytology-based needle sampling for targeted next-generation sequencing in the indeterminate thyroid tumors
Chun-Nan Chen, Tsung-Lin Yang
European Archives of Oto-Rhino-Laryngology.2023; 280(8): 3773. CrossRef - Core needle biopsy and ultrasonography are superior to fine needle aspiration in the management of follicular variant papillary thyroid carcinomas
Ji-Ye Kim, Sunhee Chang, Ah-Young Kwon, Eun Young Park, Tae Hyuk Kim, Sangjoon Choi, Minju Lee, Young Lyun Oh
Endocrine.2022; 75(2): 437. CrossRef - Fine Needle Aspiration Cytology vs. Core Needle Biopsy for Thyroid Nodules: A Prospective, Experimental Study Using Surgical Specimen
Hyuk Kwon, Jandee Lee, Soon Won Hong, Hyeong Ju Kwon, Jin Young Kwak, Jung Hyun Yoon
Journal of the Korean Society of Radiology.2022; 83(3): 645. CrossRef - Clinicopathological and Molecular Features of Secondary Cancer (Metastasis) to the Thyroid and Advances in Management
Marie Nguyen, George He, Alfred King-Yin Lam
International Journal of Molecular Sciences.2022; 23(6): 3242. CrossRef - Ultrasound Features of Thyroid Metastatic Tumors from the Digestive System: A Report of 2 Case
Zhang,BS Chao, Li,MD Yingying, Zhang,MD Mingbo
ADVANCED ULTRASOUND IN DIAGNOSIS AND THERAPY.2022; 6(4): 217. CrossRef - Unsupervised Convolutional Neural Network for Motion Estimation in Ultrasound Elastography
Xingyue Wei, Yuanyuan Wang, Lin Ge, Bo Peng, Qiong He, Rui Wang, Lijie Huang, Yan Xu, Jianwen Luo
IEEE Transactions on Ultrasonics, Ferroelectrics, and Frequency Control.2022; 69(7): 2236. CrossRef - The Value of Ultrasonography Using Thyroid Imaging Reporting and Data Systems (TIRADS) in the Diagnosis of Thyroid Cancer Among the Population of Ha'il, Saudi Arabia
Ashraf Elaggan, Amr Mostafa, Raghad Albdair, Rema Almarshedi, Anas Aljohani, Zaid Alshammari
Cureus.2022;[Epub] CrossRef - NKD2 is correlated with the occurrence, progression and prognosis of thyroid carcinoma
Yu Gao, Yiwei Wang, Rende Guo
European Journal of Medical Research.2022;[Epub] CrossRef - Update on the Evaluation of Thyroid Nodules
Victor J. Bernet, Ana-Maria Chindris
Journal of Nuclear Medicine.2021; 62(Supplement): 13S. CrossRef - Core-Needle Biopsy Does Not Show Superior Diagnostic Performance to Fine-Needle Aspiration for Diagnosing Thyroid Nodules
Ilah Shin, Eun-Kyung Kim, Hee Jung Moon, Jung Hyun Yoon, Vivian Youngjean Park, Si Eun Lee, Hye Sun Lee, Jin Young Kwak
Yonsei Medical Journal.2020; 61(2): 161. CrossRef - Comparison Between Fine Needle Aspiration and Core Needle Biopsy for the Diagnosis of Thyroid Nodules: Effective Indications According to US Findings
Soo Yeon Hahn, Jung Hee Shin, Young Lyun Oh, Ko Woon Park, Yaeji Lim
Scientific Reports.2020;[Epub] CrossRef - Plasma-Derived miRNA-222 as a Candidate Marker for Papillary Thyroid Cancer
Aistė Kondrotienė, Albertas Daukša, Daina Pamedytytė, Mintautė Kazokaitė, Aurelija Žvirblienė, Dalia Daukšienė, Vaida Simanavičienė, Raimonda Klimaitė, Ieva Golubickaitė, Rytis Stakaitis, Valdas Šarauskas, Rasa Verkauskienė, Birutė Žilaitienė
International Journal of Molecular Sciences.2020; 21(17): 6445. CrossRef - Ultrasound‐guided needle biopsy of large thyroid nodules: Core needle biopsy yields more reliable results than fine needle aspiration
Hyeon Jin Lee, Young Joong Kim, Hye Yeon Han, Jae Young Seo, Cheol Mog Hwang, KeumWon Kim
Journal of Clinical Ultrasound.2019; 47(5): 255. CrossRef - Degenerating Thyroid Nodules: Ultrasound Diagnosis, Clinical Significance, and Management
Jie Ren, Jung Hwan Baek, Sae Rom Chung, Young Jun Choi, Chan Kwon Jung, Jeong Hyun Lee
Korean Journal of Radiology.2019; 20(6): 947. CrossRef - Thyroid core needle biopsy: patients’ pain and satisfaction compared to fine needle aspiration
Hyo Jin Kim, Yeo Koon Kim, Jae Hoon Moon, June Young Choi, Sang Il Choi
Endocrine.2019; 65(2): 365. CrossRef - Ultrasonography-Guided Core Needle Biopsy Did Not Reduce Diagnostic Lobectomy for Thyroid Nodules Diagnosed as Atypia of Undetermined Significance/Follicular Lesion of Undetermined Significance
Jung Hyun Yoon, Jin Young Kwak, Hee Jung Moon, Eun-Kyung Kim
Ultrasound Quarterly.2019; 35(3): 253. CrossRef - Diagnostic value of fine-needle aspiration combined with ultrasound for thyroid cancer
Juan Li, Qian Wang, Liangliang Wang, Jing Wang, Dongxiao Wang, Zhaoqin Xin, Yilin Liu, Qinghua Zhao
Oncology Letters.2019;[Epub] CrossRef - Utility of a formatted pathologic reporting system in thyroid core needle biopsy: A validation study of 1998 consecutive cases
Ji‐Young Choe, Yoonjin Kwak, Mimi Kim, Yul Ri Chung, Hyun Jeong Kim, Yeo Koon Kim, So Yeon Park
Clinical Endocrinology.2018; 88(1): 96. CrossRef - Nuclear features of papillary thyroid carcinoma: Comparison of Core needle biopsy and thyroidectomy specimens
Jae Yeon Seok, Jungsuk An, Hyun Yee Cho, Younghye Kim, Seung Yeon Ha
Annals of Diagnostic Pathology.2018; 32: 35. CrossRef - Statement and Recommendations on Interventional Ultrasound as a Thyroid Diagnostic and Treatment Procedure
Christoph F. Dietrich, Thomas Müller, Jörg Bojunga, Yi Dong, Giovanni Mauri, Maija Radzina, Manjiri Dighe, Xin-Wu Cui, Frank Grünwald, Andreas Schuler, Andre Ignee, Huedayi Korkusuz
Ultrasound in Medicine & Biology.2018; 44(1): 14. CrossRef - Core needle biopsy of thyroid nodules: outcomes and safety from a large single-center single-operator study
Jooae Choe, Jung Hwan Baek, Hye Sun Park, Young Jun Choi, Jeong Hyun Lee
Acta Radiologica.2018; 59(8): 924. CrossRef - A spectral X-ray CT simulation study for quantitative determination of iron
Ting Su, Valérie Kaftandjian, Philippe Duvauchelle, Yuemin Zhu
Nuclear Instruments and Methods in Physics Research Section A: Accelerators, Spectrometers, Detectors and Associated Equipment.2018; 894: 39. CrossRef - Comparison of the Diagnostic Efficacy of Ultrasound‐Guided Core Needle Biopsy With 18‐ Versus 20‐Gauge Needles for Thyroid Nodules
Hye Shin Ahn, Mirinae Seo, Su Min Ha, Hee Sung Kim
Journal of Ultrasound in Medicine.2018; 37(11): 2565. CrossRef - Evaluation of Modified Core-Needle Biopsy in the Diagnosis of Thyroid Nodules
Soomin Ahn, Sejin Jung, Ji-Ye Kim, Jung Hee Shin, Soo Yeon Hahn, Young Lyun Oh
Korean Journal of Radiology.2018; 19(4): 656. CrossRef - Model-based quantitative optical biopsy in multilayer in vitro soft tissue models for whole field assessment of nonmelanoma skin cancer
Bala Nivetha Kanakaraj
Journal of Medical Imaging.2018; 5(01): 1. CrossRef - Decreased apolipoprotein A4 and increased complement component 3 as potential markers for papillary thyroid carcinoma: A proteomic study
Reyhaneh Farrokhi Yekta, Afsaneh Arefi Oskouie, Mostafa Rezaei Tavirani, Mohammad R. Mohajeri-Tehrani, Ahmad R. Soroush
The International Journal of Biological Markers.2018; 33(4): 455. CrossRef - Usefulness of core needle biopsy for the diagnosis of thyroid Burkitt’s lymphoma: a case report and review of the literature
Stella Bernardi, Andrea Michelli, Deborah Bonazza, Veronica Calabrò, Fabrizio Zanconati, Gabriele Pozzato, Bruno Fabris
BMC Endocrine Disorders.2018;[Epub] CrossRef - Risk of malignancy according to sub‐classification of the atypia of undetermined significance or follicular lesion of undetermined significance (AUS/FLUS) category in the Bethesda system for reporting thyroid cytopathology
S. J. Kim, J. Roh, J. H. Baek, S. J. Hong, Y. K. Shong, W. B. Kim, D. E. Song
Cytopathology.2017; 28(1): 65. CrossRef - Fine-needle aspiration versus core needle biopsy for diagnosis of thyroid malignancy and neoplasm: a matched cohort study
Soo-Yeon Kim, Hye Sun Lee, Jieun Moon, Eun-Kyung Kim, Hee Jung Moon, Jung Hyun Yoon, Jin Young Kwak
European Radiology.2017; 27(2): 801. CrossRef - Core‐needle biopsy versus repeat fine‐needle aspiration for thyroid nodules initially read as atypia/follicular lesion of undetermined significance
Young Jun Choi, Jung Hwan Baek, Chong Hyun Suh, Woo Hyun Shim, Boseul Jeong, Jae Kyun Kim, Dong Eun Song, Tae Yong Kim, Ki‐Wook Chung, Jeong Hyun Lee
Head & Neck.2017; 39(2): 361. CrossRef - Core Needle Biopsy of the Thyroid: 2016 Consensus Statement and Recommendations from Korean Society of Thyroid Radiology
Dong Gyu Na, Jung Hwan Baek, So Lyung Jung, Ji-hoon Kim, Jin Yong Sung, Kyu Sun Kim, Jeong Hyun Lee, Jung Hee Shin, Yoon Jung Choi, Eun Ju Ha, Hyun Kyung Lim, Soo Jin Kim, Soo Yeon Hahn, Kwang Hwi Lee, Young Jun Choi, Inyoung Youn, Young Joong Kim, Hye Sh
Korean Journal of Radiology.2017; 18(1): 217. CrossRef - Ultrasound-Pathology Discordant Nodules on Core-Needle Biopsy: Malignancy Risk and Management Strategy
Sae Rom Chung, Jung Hwan Baek, Hye Sun Park, Young Jun Choi, Tae-Yon Sung, Dong Eun Song, Tae Yong Kim, Jeong Hyun Lee
Thyroid.2017; 27(5): 707. CrossRef - Ultrasound-guided fine needle aspiration versus core needle biopsy: comparison of post-biopsy hematoma rates and risk factors
In Hye Chae, Eun-Kyung Kim, Hee Jung Moon, Jung Hyun Yoon, Vivian Y. Park, Jin Young Kwak
Endocrine.2017; 57(1): 108. CrossRef - Serum and urine 1H NMR-based metabolomics in the diagnosis of selected thyroid diseases
Wojciech Wojtowicz, Adam Zabek, Stanislaw Deja, Tomasz Dawiskiba, Dorota Pawelka, Mateusz Glod, Waldemar Balcerzak, Piotr Mlynarz
Scientific Reports.2017;[Epub] CrossRef - Comparison of Core-Needle Biopsy and Fine-Needle Aspiration for Evaluating Thyroid Incidentalomas Detected by 18F-Fluorodeoxyglucose Positron Emission Tomography/Computed Tomography: A Propensity Score Analysis
Chong Hyun Suh, Young Jun Choi, Jong Jin Lee, Woo Hyun Shim, Jung Hwan Baek, Han Cheol Chung, Young Kee Shong, Dong Eun Song, Tae Yon Sung, Jeong Hyun Lee
Thyroid.2017; 27(10): 1258. CrossRef - Identification of novel diagnostic biomarkers for thyroid carcinoma
Xiliang Wang, Qing Zhang, Zhiming Cai, Yifan Dai, Lisha Mou
Oncotarget.2017; 8(67): 111551. CrossRef - Core-needle biopsy for the preoperative diagnosis of follicular neoplasm in thyroid nodule screening: A validation study
Sung Hak Lee, Gyeong Sin Park, So Lyung Jung, Min-Hee Kim, Ja Seong Bae, Dong Jun Lim, Chan Kwon Jung
Pathology - Research and Practice.2016; 212(1): 44. CrossRef - Non-Coding RNAs in Thyroid Cancer
Ranran Zhang, Heather Hardin, Jidong Chen, Zhenying Guo, Ricardo V. Lloyd
Endocrine Pathology.2016; 27(1): 12. CrossRef - Fine‐needle aspiration and core needle biopsy: An update on 2 common minimally invasive tissue sampling modalities
Paul A. VanderLaan
Cancer Cytopathology.2016; 124(12): 862. CrossRef - Core Needle Biopsy Is a More Conclusive Follow-up Method Than Repeat Fine Needle Aspiration for Thyroid Nodules with Initially Inconclusive Results: A Systematic Review and Meta-Analysis
Jung-Soo Pyo, Jin Hee Sohn, Guhyun Kang
Journal of Pathology and Translational Medicine.2016; 50(3): 217. CrossRef - The role of core-needle biopsy in the diagnosis of thyroid malignancy in 4580 patients with 4746 thyroid nodules: a systematic review and meta-analysis
Chong Hyun Suh, Jung Hwan Baek, Jeong Hyun Lee, Young Jun Choi, Kyung Won Kim, Jayoun Lee, Ki-Wook Chung, Young Kee Shong
Endocrine.2016; 54(2): 315. CrossRef - Fine‐needle aspiration versus core needle biopsy: Reconsidering the evidence of superiority
Annemieke van Zante, Britt‐Marie Ljung
Cancer Cytopathology.2016; 124(12): 853. CrossRef
- Reevaluation of malignancy risk in nondiagnostic thyroid nodules with long‐term follow‐up via surgical resection or core needle biopsy: A retrospective study
- Diagnostic Accuracy of Endoscopic Ultrasound-Guided Fine Needle Aspiration Cytology of Pancreatic Lesions
- Hae Woon Baek, Min Jee Park, Ye-Young Rhee, Kyoung Bun Lee, Min A Kim, In Ae Park
- J Pathol Transl Med. 2015;49(1):52-60. Published online January 15, 2015
- DOI: https://doi.org/10.4132/jptm.2014.10.26
- 13,129 View
- 96 Download
- 34 Web of Science
- 33 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Endoscopic ultrasound–guided fine needle aspiration cytology (EUS-FNAC) is currently the most commonly used procedure for obtaining cytologic specimens of the pancreas. It is accurate, minimally invasive, safe and cost-effective. However, there is discrepancy between cytological and surgical diagnoses. This study was aimed at evaluating the diagnostic accuracy of EUS-FNAC of the pancreas. Methods: We performed a retrospective review of 191 cases of pancreatic lesions initially diagnosed by EUS-FNAC with subsequent histological diagnosis between 2010 and 2012 in the Department of Pathology, Seoul National University Hospital. Cytologic and surgical diagnoses were categorized into five groups: negative, benign, atypical, malignant, and insufficient for diagnosis. Subsequently, 167 cases with satisfactory yield in both surgical and cytology specimens were statistically analyzed to determine correlations with diagnosis. Results: In comparison to surgical diagnoses, cytologic diagnoses were true-positive in 103 cases (61.7%), true-negative in 28 cases (16.8%), false-positive in 9 cases (5.4%), and false-negative in 27 cases (16.1%). The diagnostic accuracy was 78.4%, sensitivity was 79.2%, and specificity was 75.7%. The positive predictive value was 92.0%, and negative predictive value was 50.9%. Conclusions: EUS-FNAC has high accuracy, sensitivity, specificity and positive predictive value. Overcoming the limitations of EUS-FNAC will make it a useful and reliable diagnostic tool for accurate evaluation of pancreatic lesions. -
Citations
Citations to this article as recorded by- miR-6855-5p Enhances Radioresistance and Promotes Migration of Pancreatic Cancer by Inducing Epithelial-Mesenchymal Transition via Suppressing FOXA1: Potential of Plasma Exosomal miR-6855-5p as an Indicator of Radiosensitivity in Patients with Pancreatic
Hiroki Ueda, Hidenori Takahashi, Shogo Kobayashi, Masahiko Kubo, Kazuki Sasaki, Yoshifumi Iwagami, Daisaku Yamada, Yoshito Tomimaru, Tadafumi Asaoka, Takehiro Noda, Junzo Shimizu, Yuichiro Doki, Hidetoshi Eguchi
Annals of Surgical Oncology.2025; 32(2): 720. CrossRef - Combating false negatives in pancreatic cancer: A deep learning approach for aiding fine needle aspiration via accurate subregion identification
Ms Jasmine Chhikara, Nidhi Goel, Neeru Rathee
Engineering Applications of Artificial Intelligence.2025; 157: 111347. CrossRef - Grading pancreatic adenocarcinomas on fine needle aspiration cytology. The outstanding issues
Mrinmay Kumar Mallik, Laila Rafiq Qadan, Asit Kumar Mohanty, Ali Alali, Kusum Kapila
Cytopathology.2024; 35(2): 256. CrossRef - Reporting Pancreatic FNAC using the Papanicolaou System: Still a Diagnostic Challenge
Parul Verma, Saloni Goyal, Ruchita Tyagi, Mehar Ghuman, Ramit Mahajan, Arshneet Kaur Selhi, Harpreet Kaur, Pavneet Kaur Selhi
Journal of Cytology.2024; 41(2): 123. CrossRef - Preoperative treatment response prediction for pancreatic cancer by multiple microRNAs in plasma exosomes: Optimization using machine learning and network analysis
Hiroki Ueda, Hidenori Takahashi, Ryoto Sakaniwa, Tetsuhisa Kitamura, Shogo Kobayashi, Yoshito Tomimaru, Masahiko Kubo, Kazuki Sasaki, Yoshifumi Iwagami, Daisaku Yamada, Tadafumi Asaoka, Takehiro Noda, Junzo Shimizu, Yuichiro Doki, Hidetoshi Eguchi
Pancreatology.2024; 24(7): 1097. CrossRef - Comparison of Endoscopic Ultrasound-Guided Fine-Needle Aspiration with Fine-Needle Biopsy for Solid Gastrointestinal Lesions: A Randomized Crossover Single-Center study
Shivaraj Afzalpurkar, Vijay Kumar Rai, Nikhil Sonthalia, Gajanan Rodge, Awanesh Tewary, Mahesh Goenka
Journal of Digestive Endoscopy.2023; 14(01): 014. CrossRef - Diagnosing and monitoring pancreatic cancer through cell-free DNA methylation: progress and prospects
María Victoria García-Ortiz, Pablo Cano-Ramírez, Marta Toledano-Fonseca, Enrique Aranda, Antonio Rodríguez-Ariza
Biomarker Research.2023;[Epub] CrossRef - The impact of preoperative EUS-FNA for distal resectable pancreatic cancer: Is it really effective enough to take risks?
Jin-Seok Park, Jae Hoon Lee, Tae Jun Song, Joune Seup Lee, Seok Jung Jo, Dong Wook Oh, Ki Byung Song, Dae Wook Hwang, Do Hyun Park, Sang Soo Lee, Song Cheol Kim, Dong Wan Seo, Sung Koo Lee, Myung-Hwan Kim
Surgical Endoscopy.2022; 36(5): 3192. CrossRef - Magnetic Resonance Imaging Radiomics‐Based Nomogram From Primary Tumor for Pretreatment Prediction of Peripancreatic Lymph Node Metastasis in Pancreatic Ductal Adenocarcinoma: A Multicenter Study
Zhenshan Shi, Chengle Ma, Xinming Huang, Dairong Cao
Journal of Magnetic Resonance Imaging.2022; 55(3): 823. CrossRef - Role of Pathologist in the Era of Image-Guided and EUS-Guided Aspirations: A 10-Year Study at a Single Tertiary Care Oncology Institute in North India
Gurudutt Gupta, Anila Sharma, Meenakshi Kamboj, Anurag Sharma, Sunil Pasricha, Garima Durga, Anurag Mehta, Avinash Rao
Acta Cytologica.2022; 66(3): 187. CrossRef - Predicting Factors for Pancreatic Malignancy with Computed Tomography and Endoscopic Ultrasonography in Chronic Pancreatitis
Jian-Han Lai, Keng-Han Lee, Chen-Wang Chang, Ming-Jen Chen, Ching-Chung Lin
Diagnostics.2022; 12(4): 1004. CrossRef - Phenotypic profiling of pancreatic ductal adenocarcinoma plasma-derived small extracellular vesicles for cancer diagnosis and cancer stage prediction: a proof-of-concept study
Wei Zhang, Ling Wang, Dan Li, Douglas H. Campbell, Bradley J. Walsh, Nicolle H. Packer, Qing Dong, Erkang Wang, Yuling Wang
Analytical Methods.2022; 14(23): 2255. CrossRef - Cancer-derived small extracellular vesicles: emerging biomarkers and therapies for pancreatic ductal adenocarcinoma diagnosis/prognosis and treatment
Wei Zhang, Douglas H. Campbell, Bradley J. Walsh, Nicolle H. Packer, Dingbin Liu, Yuling Wang
Journal of Nanobiotechnology.2022;[Epub] CrossRef - Single Cell RNA Sequencing: A New Frontier in Pancreatic Ductal Adenocarcinoma
Maroun Bou Zerdan, Malek Shatila, Dhruv Sarwal, Youssef Bouferraa, Morgan Bou Zerdan, Sabine Allam, Merima Ramovic, Stephen Graziano
Cancers.2022; 14(19): 4589. CrossRef - Molecular Subtyping and Precision Medicine for Pancreatic Cancer
Fieke Froeling, Raffaella Casolino, Antonio Pea, Andrew Biankin, David Chang
Journal of Clinical Medicine.2021; 10(1): 149. CrossRef - Reshaping preoperative treatment of pancreatic cancer in the era of precision medicine
R. Casolino, C. Braconi, G. Malleo, S. Paiella, C. Bassi, M. Milella, S.B. Dreyer, F.E.M. Froeling, D.K. Chang, A.V. Biankin, T. Golan
Annals of Oncology.2021; 32(2): 183. CrossRef - Endoscopic Ultrasound-Guided Fine Needle Aspiration Cytology of Pancreatic Adenocarcinomas Revisited. A Detailed Cytological Analysis
Mrinmay Kumar Mallik, Kusum Kapila, Asit Kumar Mohanty, Shafi Ahmed Inamdar, Ali AlAli, Abdullah Al Naseer
Journal of Cytology.2021; 38(1): 31. CrossRef - Diagnostic value of various liquid biopsy methods for pancreatic cancer
Yuzhou Zhu, Hao Zhang, Nan Chen, Jianqi Hao, Hongyu Jin, Xuelei Ma
Medicine.2020; 99(3): e18581. CrossRef - Factors affecting cytological results of endoscopic ultrasound guided-fine needle aspiration during learning
Jian-Han Lai, Hsiang-Hung Lin, Ching-Chung Lin
Diagnostic Pathology.2020;[Epub] CrossRef - Comparison between Conventional Smear and Liquid-Based Preparation in Endoscopic Ultrasonography-Fine Needle Aspiration Cytology of Pancreatic Lesions
Soo Hee Ko, Jung-Soo Pyo, Byoung Kwan Son, Hyo Young Lee, Il Whan Oh, Kwang Hyun Chung
Diagnostics.2020; 10(5): 293. CrossRef - Evaluation of Pancreatic Lesions With Endoscopic Ultrasound and Fine Needle Aspiration
Yan Luk, Wong Hoi She, Felix Che Lok Chow, Ka Wing Ma, Simon Hing Yin Tsang, Wing Chiu Dai, Tan To Cheung, Chung Mau Lo
Surgical Innovation.2020; 27(5): 431. CrossRef - The applicability of Papanicolaou Society of Cytopathology system on reporting endoscopic ultrasound‐guided fine needle aspiration cytology specimens of pancreatic lesions in situations with limited availability of ancillary tests. Experience at a single
Mrinmay Kumar Mallik, Laila Rafiq Qadan, Abdullah Al Naseer, Ali AlAli, Taiba Al Ansari, Shafi Ahmed Inamdar Naquib, Dilip Kumar Das, Kusum Kapila
Cytopathology.2020; 31(6): 564. CrossRef - Circulating Cell-Free DNA-Based Liquid Biopsy Markers for the Non-Invasive Prognosis and Monitoring of Metastatic Pancreatic Cancer
Marta Toledano-Fonseca, M. Teresa Cano, Elizabeth Inga, Rosa Rodríguez-Alonso, M. Auxiliadora Gómez-España, Silvia Guil-Luna, Rafael Mena-Osuna, Juan R. de la Haba-Rodríguez, Antonio Rodríguez-Ariza, Enrique Aranda
Cancers.2020; 12(7): 1754. CrossRef - Risk of malignancy in the categories of the Papanicolaou Society of Cytopathology system for reporting pancreaticobiliary cytology
Raza S. Hoda, Elizabeth B. Finer, Ronald N. Arpin, Matthew Rosenbaum, Martha B. Pitman
Journal of the American Society of Cytopathology.2019; 8(3): 120. CrossRef - Endoscopic ultrasound guided fine‐needle aspiration vs core needle biopsy for solid pancreatic lesions: Comparison of diagnostic accuracy and procedural efficiency
Aslam Syed, Olivia Babich, Bharat Rao, Shailendra Singh, Neil Carleton, Abhishek Gulati, Archana Kulkarni, Mrinal Garg, Katie Farah, Gursimran Kochhar, Suzanne Morrissey, Marcia Mitre, Abhijit Kulkarni, Manish Dhawan, Jan F. Silverman, Majed Pharaon, Shya
Diagnostic Cytopathology.2019; 47(11): 1138. CrossRef - Liquid Biopsy as Surrogate for Tissue for Molecular Profiling in Pancreatic Cancer: A Meta-Analysis Towards Precision Medicine
Claudio Luchini, Nicola Veronese, Alessia Nottegar, Vera Cappelletti, Maria G. Daidone, Lee Smith, Christopher Parris, Lodewijk A. A. Brosens, Maria G. Caruso, Liang Cheng, Christopher L. Wolfgang, Laura D. Wood, Michele Milella, Roberto Salvia, Aldo Scar
Cancers.2019; 11(8): 1152. CrossRef - It is necessary to exam bottom and top slide smears of EUS-FNA for pancreatic cancer
Jong-chan Lee, Haeryoung Kim, Hyoung Woo Kim, Jongchan Lee, Kyu-hyun Paik, Jingu Kang, Jin-Hyeok Hwang, Jaihwan Kim
Hepatobiliary & Pancreatic Diseases International.2018; 17(6): 553. CrossRef - Preoperative EUS-guided FNA: effects on peritoneal recurrence and survival in patients with pancreatic cancer
Sun Hwa Kim, Young Sik Woo, Kwang Hyuck Lee, Jong Kyun Lee, Kyu Taek Lee, Joo Kyung Park, Soo Hoon Kang, Ji Won Kim, Jae Keun Park, Sung-Wook Park
Gastrointestinal Endoscopy.2018; 88(6): 926. CrossRef - Cytological characteristics of atypical cells in endoscopic ultrasound-guided fine-needle aspiration specimens obtained from the pancreas
Shikine ESAKA, Yoko MATSUDA, Yuri HAMASHIMA, Masayuki IMAIZUMI, Hiroya KOJIMA, Yuri KISO, Hiroto SHIRAHATA, Mayumi KINOSHITA, Akemi SUZUKI, Tomio ARAI
The Journal of the Japanese Society of Clinical Cytology.2018; 57(4): 199. CrossRef - Performance measures for endoscopic retrograde cholangiopancreatography and endoscopic ultrasound: A European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative
Dirk Domagk, Kofi W Oppong, Lars Aabakken, Laszlo Czakó, Tibor Gyökeres, Gianpiero Manes, Peter Meier, Jan-Werner Poley, Thierry Ponchon, Andrea Tringali, Cristina Bellisario, Silvia Minozzi, Carlo Senore, Cathy Bennett, Michael Bretthauer, Cesare Hassan,
United European Gastroenterology Journal.2018; 6(10): 1448. CrossRef - Performance measures for ERCP and endoscopic ultrasound: a European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative
Dirk Domagk, Kofi W. Oppong, Lars Aabakken, Laszlo Czakó, Tibor Gyökeres, Gianpiero Manes, Peter Meier, Jan-Werner Poley, Thierry Ponchon, Andrea Tringali, Cristina Bellisario, Silvia Minozzi, Carlo Senore, Cathy Bennett, Michael Bretthauer, Cesare Hassan
Endoscopy.2018; 50(11): 1116. CrossRef - Imaging modalities for characterising focal pancreatic lesions
Lawrence MJ Best, Vishal Rawji, Stephen P Pereira, Brian R Davidson, Kurinchi Selvan Gurusamy
Cochrane Database of Systematic Reviews.2017;[Epub] CrossRef - Percutaneous ultrasound‐guided core needle biopsy of solid pancreatic masses: Results in 250 patients
Guven Kahriman, Nevzat Ozcan, Serap Dogan, Soner Ozmen, Kemal Deniz
Journal of Clinical Ultrasound.2016; 44(8): 470. CrossRef
- miR-6855-5p Enhances Radioresistance and Promotes Migration of Pancreatic Cancer by Inducing Epithelial-Mesenchymal Transition via Suppressing FOXA1: Potential of Plasma Exosomal miR-6855-5p as an Indicator of Radiosensitivity in Patients with Pancreatic
- Indolent CD56-Positive Clonal T-Cell Lymphoproliferative Disease of the Stomach Mimicking Lymphomatoid Gastropathy
- Mineui Hong, Won Seog Kim, Young Hyeh Ko
- Korean J Pathol. 2014;48(6):430-433. Published online December 31, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.6.430
- 10,842 View
- 70 Download
- 3 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Indolent T- and Natural Killer-Cell Lymphomas and Lymphoproliferative Diseases—Entities in Evolution
Chi Sing Ng
Lymphatics.2025; 3(4): 41. CrossRef - Case Report: Primary Indolent Epstein-Barr Virus-Positive T-Cell Lymphoproliferative Disease Involving the Central Nervous System
Kun Wang, Jinjian Li, Xuehui Zhou, Junhui Lv, Yirong Wang, Xinwei Li
Frontiers in Surgery.2022;[Epub] CrossRef - Indolent NK cell proliferative lesion mimicking NK/T cell lymphoma in the gallbladder
Su Hyun Hwang, Joon Seong Park, Seong Hyun Jeong, Hyunee Yim, Jae Ho Han
Human Pathology: Case Reports.2016; 5: 39. CrossRef
- Indolent T- and Natural Killer-Cell Lymphomas and Lymphoproliferative Diseases—Entities in Evolution
- Comparison of Three
BRAF Mutation Tests in Formalin-Fixed Paraffin Embedded Clinical Samples - Soomin Ahn, Jeeyun Lee, Ji-Youn Sung, So Young Kang, Sang Yun Ha, Kee-Taek Jang, Yoon-La Choi, Jung-Sun Kim, Young Lyun Oh, Kyoung-Mee Kim
- Korean J Pathol. 2013;47(4):348-354. Published online August 26, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.4.348
- 10,099 View
- 60 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Recently,
BRAF inhibitors showed dramatic treatment outcomes inBRAF V600 mutant melanoma. Therefore, the accuracy ofBRAF mutation test is critical.Methods BRAF mutations were tested by dual-priming oligonucleotide-polymerase chain reaction (DPO-PCR), direct sequencing and subsequently retested with a real-time PCR assay, cobas 4800 V600 mutation test. In total, 64 tumors including 34 malignant melanomas and 16 papillary thyroid carcinomas were analyzed. DNA was extracted from formalin-fixed paraffin embedded tissue samples and the results of cobas test were directly compared with those of DPO-PCR and direct sequencing.Results BRAF mutations were found in 23 of 64 (35.9%) tumors. There was 9.4% discordance among 3 methods. Out of 6 discordant cases, 4 cases were melanomas; 3 cases wereBRAF V600E detected only by cobas test, but were not detected by DPO-PCR and direct sequencing. One melanoma patient withBRAF mutation detected only by cobas test has been on vemurafenib treatment for 6 months and showed a dramatic response to vemurafenib. DPO-PCR failed to detect V600K mutation in one case identified by both direct sequencing and cobas test.Conclusions In direct comparison of the currently available DPO-PCR, direct sequencing and real-time cobas test for
BRAF mutation, real-time PCR assay is the most sensitive method.-
Citations
Citations to this article as recorded by- Preoperative BRAFV600E mutation detection in thyroid carcinoma by immunocytochemistry
Kristine Zøylner Swan, Stine Horskær Madsen, Steen Joop Bonnema, Viveque Egsgaard Nielsen, Marie Louise Jespersen
APMIS.2022; 130(11): 627. CrossRef - Strategy to reduce unnecessary surgeries in thyroid nodules with cytology of Bethesda category III (AUS/FLUS): a retrospective analysis of 667 patients diagnosed by surgery
Yong Joon Suh, Yeon Ju Choi
Endocrine.2020; 69(3): 578. CrossRef - A new primer construction technique that effectively increases amplification of rare mutant templates in samples
Jr-Kai Huang, Ling Fan, Tao-Yeuan Wang, Pao-Shu Wu
BMC Biotechnology.2019;[Epub] CrossRef - BRAF and NRAS mutations and antitumor immunity in Korean malignant melanomas and their prognostic relevance: Gene set enrichment analysis and CIBERSORT analysis
Kyueng-Whan Min, Ji-Young Choe, Mi Jung Kwon, Hye Kyung Lee, Ho Suk Kang, Eun Sook Nam, Seong Jin Cho, Hye-Rim Park, Soo Kee Min, Jinwon Seo, Yun Joong Kim, Nan Young Kim, Ho Young Kim
Pathology - Research and Practice.2019; 215(12): 152671. CrossRef - The association between dermoscopic features and BRAF mutational status in cutaneous melanoma: Significance of the blue-white veil
Miquel Armengot-Carbó, Eduardo Nagore, Zaida García-Casado, Rafael Botella-Estrada
Journal of the American Academy of Dermatology.2018; 78(5): 920. CrossRef - Comparison of Five Different Assays for the Detection of BRAF Mutations in Formalin-Fixed Paraffin Embedded Tissues of Patients with Metastatic Melanoma
Claire Franczak, Julia Salleron, Cindy Dubois, Pierre Filhine-Trésarrieu, Agnès Leroux, Jean-Louis Merlin, Alexandre Harlé
Molecular Diagnosis & Therapy.2017; 21(2): 209. CrossRef - Validation of an NGS mutation detection panel for melanoma
Anne Reiman, Hugh Kikuchi, Daniela Scocchia, Peter Smith, Yee Wah Tsang, David Snead, Ian A Cree
BMC Cancer.2017;[Epub] CrossRef - Transformation to Small Cell Lung Cancer of Pulmonary Adenocarcinoma: Clinicopathologic Analysis of Six Cases
Soomin Ahn, Soo Hyun Hwang, Joungho Han, Yoon-La Choi, Se-Hoon Lee, Jin Seok Ahn, Keunchil Park, Myung-Ju Ahn, Woong-Yang Park
Journal of Pathology and Translational Medicine.2016; 50(4): 258. CrossRef - Immunohistochemistry with the anti-BRAF V600E (VE1) antibody: impact of pre-analytical conditions and concordance with DNA sequencing in colorectal and papillary thyroid carcinoma
Katerina Dvorak, Birte Aggeler, John Palting, Penny McKelvie, Andrew Ruszkiewicz, Paul Waring
Pathology.2014; 46(6): 509. CrossRef
- Preoperative BRAFV600E mutation detection in thyroid carcinoma by immunocytochemistry
- No Detection of Simian Virus 40 in Malignant Mesothelioma in Korea
- Minseob Eom, Jamshid Abdul-Ghafar, Sun-Mi Park, Joung Ho Han, Soon Won Hong, Kun Young Kwon, Eun Suk Ko, Lucia Kim, Wan Seop Kim, Seung Yeon Ha, Kyo Young Lee, Chang Hun Lee, Hye Kyoung Yoon, Yoo Duk Choi, Myoung Ja Chung, Soon-Hee Jung
- Korean J Pathol. 2013;47(2):124-129. Published online April 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.2.124
- 10,657 View
- 56 Download
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Simian virus 40 (SV40), a polyomavirus, was discovered as a contaminant of a human polio vaccine in the 1960s. It is known that malignant mesothelioma (MM) is associated with SV40, and that the virus works as a cofactor to the carcinogenetic effects of asbestos. However, the reports about the correlation between SV40 and MM have not been consistent. The purpose of this study is to identify SV40 in MM tissue in Korea through detection of SV40 protein and DNA.
Methods We analyzed 62 cases of available paraffin-blocks enrolled through the Korean Malignant Mesothelioma Surveillance System and performed immunohistochemistry for SV40 protein and real-time polymerase chain reaction (PCR) for SV40 DNA.
Results Of 62 total cases, 40 had disease involving the pleura (64.5%), and 29 (46.8%) were found to be of the epithelioid subtype. Immunostaining demonstrated that all examined tissues were negative for SV40 protein. Sufficient DNA was extracted for real-time PCR analysis from 36 cases. Quantitative PCR of these samples showed no increase in SV40 transcript compared to the negative controls.
Conclusions SV40 is not associated with the development of MM in Korea.
-
Citations
Citations to this article as recorded by- Association Study of Pleural Mesothelioma and Oncogenic Simian Virus 40 in the Crocidolite-Contaminated Area of Dayao County, Yunnan Province, Southwest China
Ru-ai Liu, Bo-yong Wang, Xin Chen, Yuan-qian Pu, Jia-ji Zi, Wen Mei, Ye-pin Zhang, Lu Qiu, Wei Xiong
Genetic Testing and Molecular Biomarkers.2024; 28(5): 189. CrossRef - Binding of SV40’s Viral Capsid Protein VP1 to Its Glycosphingolipid Receptor GM1 Induces Negative Membrane Curvature: A Molecular Dynamics Study
Raisa Kociurzynski, Sophie D. Beck, Jean-Baptiste Bouhon, Winfried Römer, Volker Knecht
Langmuir.2019; 35(9): 3534. CrossRef - Estimated future incidence of malignant mesothelioma in South Korea: Projection from 2014 to 2033
Kyeong Min Kwak, Domyung Paek, Seung-sik Hwang, Young-Su Ju, Mark Allen Pershouse
PLOS ONE.2017; 12(8): e0183404. CrossRef - The function, mechanisms, and role of the genes PTEN and TP53 and the effects of asbestos in the development of malignant mesothelioma: a review focused on the genes' molecular mechanisms
Leonardo Vinícius Monteiro de Assis, Mauro César Isoldi
Tumor Biology.2014; 35(2): 889. CrossRef - The role of key genes and pathways involved in the tumorigenesis of Malignant Mesothelioma
Leonardo Vinícius Monteiro de Assis, Jamille Locatelli, Mauro César Isoldi
Biochimica et Biophysica Acta (BBA) - Reviews on Cancer.2014; 1845(2): 232. CrossRef - Pleural Mesothelioma: An Institutional Experience of 66 Cases
Soomin Ahn, In Ho Choi, Joungho Han, Jhingook Kim, Myung-Ju Ahn
Korean Journal of Pathology.2014; 48(2): 91. CrossRef
- Association Study of Pleural Mesothelioma and Oncogenic Simian Virus 40 in the Crocidolite-Contaminated Area of Dayao County, Yunnan Province, Southwest China
- Prognostic Relevance of the Expression of CA IX, GLUT-1, and VEGF in Ovarian Epithelial Cancers
- Kyungbin Kim, Won Young Park, Jee Yeon Kim, Mee Young Sol, Dong Hun Shin, Do Youn Park, Chang Hun Lee, Jeong Hee Lee, Kyung Un Choi
- Korean J Pathol. 2012;46(6):532-540. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.532
- 10,636 View
- 42 Download
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Tumor hypoxia is associated with malignant progression and treatment resistance. Hypoxia-related factors, such as carbonic anhydrase IX (CA IX), glucose transporter-1 (GLUT-1), and vascular endothelial growth factor (VEGF) permit tumor cell adaptation to hypoxia. We attempted to elucidate the correlation of these markers with variable clinicopathological factors and overall prognosis.
Methods Immunohistochemistry for CA IX, GLUT-1, and VEGF was performed on formalin-fixed, paraffin-embedded tissues from 125 cases of ovarian epithelial cancer (OEC).
Results CA IX expression was significantly associated with an endometrioid and mucinous histology, nuclear grade, tumor necrosis, and mitosis. GLUT-1 expression was associated with tumor necrosis and mitosis. VEGF expression was correlated only with disease recurrence. Expression of each marker was not significant in terms of overall survival in OECs; however, there was a significant correlation between poor overall survival rate and high coexpression of these markers.
Conclusions The present study suggests that it is questionable whether CA IX, GLUT-1, or VEGF can be used alone as independent prognostic factors in OECs. Using at least two markers helps to predict patient outcomes in total OECs. Moreover, the inhibition of two target gene combinations might prove to be a novel anticancer therapy.
-
Citations
Citations to this article as recorded by- Glucose-transporter 1 (GLUT1) as a prognostic biomarker: evidence from 14,966 human tumors across 134 cancer types
Seyma Büyücek, Katharina Möller, Florian Viehweger, Ria Schlichter, Anne Menz, Andreas M Luebke, Viktor Reiswich, Martina Kluth, Claudia Hube-Magg, Andrea Hinsch, Florian Lutz, Sören Weidemann, Frank Jacobsen, Maximilian Lennartz, David Dum, Christian Ber
BMC Cancer.2026;[Epub] CrossRef - Role of Carbonic Anhydrase IX Expression in Triple-negative Breast Cancer
Hemali B Kotadiya, Nupur A Patel, Vora Hemangini H
Gujarat Cancer Society Research Journal.2026; 27(2): 31. CrossRef - Evaluation of the effect of Endogenous and Exogenous Antioxidants on Hypoxia Induced Breast Adenocarcinoma Cell Invasion and Migration:
In vitro
Subarnarekha Maitra, Poulami Sen, Dibya Sinha, Tathagata Roy
Research Journal of Pharmacy and Technology.2025; : 3153. CrossRef - Effect of Ultrasound Therapy at the ST11 on Sympathetic Nervous System Change: A Prospective Randomized Controlled Study
Shinwoo Kang, Dongho Keum
Journal of Korean Medicine Rehabilitation.2023; 33(4): 167. CrossRef - A systematic review verified by bioinformatic analysis based on TCGA reveals week prognosis power of CAIX in renal cancer
Zikuan Zhang, Bo Wu, Yuan Shao, Yongquan Chen, Dongwen Wang, Lucia Magnelli
PLOS ONE.2022; 17(12): e0278556. CrossRef - Effect of Acupuncture at the Field of the Auricular Branch of the Vagus Nerve on Autonomic Nervous System Change
Sunjoo An, Dongho Keum
Journal of Korean Medicine Rehabilitation.2021; 31(2): 81. CrossRef - Responses of Autonomic Nervous System and Gastrointestinal Function to Acupuncture at Abdominal Anterior Cutaneous Nerve : A Pilot Study
Seohyun Park, Hojun Kim, Dongho Keum
Journal of Korean Medicine.2019; 40(1): 99. CrossRef - Omega-3 polyunsaturated fatty acid docosahexaenoic acid and its role in exhaustive-exercise-induced changes in female rat ovulatory cycle
Abeer F. Mostafa, Shereen M. Samir, R.M. Nagib
Canadian Journal of Physiology and Pharmacology.2018; 96(4): 395. CrossRef - Clear cell carcinomas of the ovary and kidney: clarity through genomics
Jennifer X Ji, Yi Kan Wang, Dawn R Cochrane, David G Huntsman
The Journal of Pathology.2018; 244(5): 550. CrossRef - Prognostic Significance of Carbonic Anhydrase IX Expression in Cancer Patients: A Meta-Analysis
Simon J. A. van Kuijk, Ala Yaromina, Ruud Houben, Raymon Niemans, Philippe Lambin, Ludwig J. Dubois
Frontiers in Oncology.2016;[Epub] CrossRef - Review of Research Topics on Abdominal Examination
Jihye Kim, Jeong Hwan Park, Keun Ho Kim
Journal of Korean Medicine.2016; 37(3): 1. CrossRef - Expression of hypoxic markers and their prognostic significance in soft tissue sarcoma
JEUNG IL KIM, KYUNG UN CHOI, IN SOOK LEE, YOUNG JIN CHOI, WON TACK KIM, DONG HOON SHIN, KYUNGBIN KIM, JEONG HEE LEE, JEE YEON KIM, MEE YOUNG SOL
Oncology Letters.2015; 9(4): 1699. CrossRef - Evaluation of a Hypoxia Regulated Gene Panel in Ovarian Cancer
Amanda F. Baker, Scott W. Malm, Ritu Pandey, Cindy Laughren, Haiyan Cui, Denise Roe, Setsuko K. Chambers
Cancer Microenvironment.2015; 8(1): 45. CrossRef - Sulforaphane reduces molecular response to hypoxia in ovarian tumor cells independently of their resistance to chemotherapy
MICHAL PASTOREK, VERONIKA SIMKO, MARTINA TAKACOVA, MONIKA BARATHOVA, MARIA BARTOSOVA, LUBA HUNAKOVA, OLGA SEDLAKOVA, SONA HUDECOVA, OLGA KRIZANOVA, FRANCK DEQUIEDT, SILVIA PASTOREKOVA, JAN SEDLAK
International Journal of Oncology.2015; 47(1): 51. CrossRef - Overexpression of Glucose Transporter-1 (GLUT-1) Predicts Poor Prognosis in Epithelial Ovarian Cancer
Hanbyoul Cho, You Sun Lee, Julie Kim, Joon-Yong Chung, Jae-Hoon Kim
Cancer Investigation.2013; 31(9): 607. CrossRef - Towards Lipidomics of Low-Abundant Species for Exploring Tumor Heterogeneity Guided by High-Resolution Mass Spectrometry Imaging
Jonathan Cimino, David Calligaris, Johann Far, Delphine Debois, Silvia Blacher, Nor Sounni, Agnès Noel, Edwin De Pauw
International Journal of Molecular Sciences.2013; 14(12): 24560. CrossRef
- Glucose-transporter 1 (GLUT1) as a prognostic biomarker: evidence from 14,966 human tumors across 134 cancer types
- Extraskeletal Mesenchymal Chondrosarcoma in the Axillary Region: Reports of Two Cases
- Chang-Young Seo, Sung-Taek Jung, Jae-Wook Byun
- Korean J Pathol. 2012;46(5):483-488. Published online October 25, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.5.483
- 9,877 View
- 44 Download
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Extraskeletal mesenchymal chondrosarcomas (EMCs) are relatively uncommon, and a location in the upper extremity, especially in the shoulder or axillary region, is rare. Furthermore, the radiographic findings of EMCs do not show any features that distinguish them from other neoplasms, and therefore, definitive diagnoses are made based on histological features. EMC is an aggressive tumor with a poor prognosis, and requires wide surgical excision. However, its treatment may involve peculiarities such as a difficulty in obtaining a proper surgical margin in the axillary region or shoulder. In this report, the authors present two rare cases of EMCs in the axillary region.
-
Citations
Citations to this article as recorded by- Extraskeletal Mesenchymal Chondrosarcoma of the Arm: A Rare Case Report with a Review of Literature
Anubhuti Chaturvedi, Nimisha Dhankar, Swapnil Suman, Nita Khurana, Chandra Bhushan Singh, Sapna Singh
Journal of Bone and Joint Diseases.2025; 40(3): 170. CrossRef - Complete surgical excision of a high‐grade extraskeletal mesenchymal chondrosarcoma, resulting in a longer survival than previously reported
Hannah Reeves, Tesh Smalle
Veterinary Record Case Reports.2022;[Epub] CrossRef - Locally recurrent extraskeletal myxoid chondrosarcoma of the shoulder: a case of complete neoadjuvant radiotherapy response
Luca Improta, Sergio Valeri, Rossana Alloni, Chiara Pagnoni, Francesco Mallozzi Santa Maria, Beniamino Brunetti, Carlo Greco, Irene Aprile, Mirella Maselli, Bruno Vincenzi, Alessandro Gronchi
Clinical Sarcoma Research.2020;[Epub] CrossRef - Primary extraskeletal chondrosarcoma in the axillary region of a dog with review of the literature
Catrina Pennington, Josep Monne Rodriguez, Marlene Finck, Ben Walton
Veterinary Record Case Reports.2018;[Epub] CrossRef - Mesenchymal Chondrosarcoma of Bone and Soft Tissue: A Systematic Review of 107 Patients in the Past 20 Years
Jie Xu, Dasen Li, Lu Xie, Shun Tang, Wei Guo, David M Loeb
PLOS ONE.2015; 10(4): e0122216. CrossRef - Management of renal extraskeletal mesenchymal chondrosarcoma
Vitalie Gherman, Ciprian Tomuleasa, Catalina Bungardean, Nicolae Crisan, Victor-Dan Ona, Bogdan Feciche, Alexandru Irimie, Ioan Coman
BMC Surgery.2014;[Epub] CrossRef
- Extraskeletal Mesenchymal Chondrosarcoma of the Arm: A Rare Case Report with a Review of Literature
- Endoscopic Ultrasound-Guided Fine Needle Aspiration Cytology Diagnosis of Solid Pseudopapillary Neoplasm: Three Case Reports with Review of Literature
- Joon Seon Song, Chong Woo Yoo, Youngmee Kwon, Eun Kyung Hong
- Korean J Pathol. 2012;46(4):399-406. Published online August 23, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.4.399
- 10,398 View
- 62 Download
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF Solid pseudopapillary neoplasm of the pancreas (SPN) is relatively rare and it occurs almost exclusively in women. We recently experienced three cases of SPN diagnosed by endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA). These three cases were two male and one female patient whose age was 29, 37, and 44 years old. Radiological diagnosis was pancreatic endocrine tumor (PEN) showing solid with a heterogenous echogenicity. EUS-FNA cytology specimens consisted of single cells and aggregates of uniform cells, forming microadenoid structures, branching, papillary clusters with delicate fibrovascular cores. In conclusion, a single diagnosis of SPN based on clinical and radiological findings would be risky because there is a possibility of it being misdiagnosed as PEN or other malignancies. An EUS-FNA is therefore essential for establishing the diagnosis. In addition, the pathologists should recognize the characteristic cytologic findings with immunoprofiles of SPN to prevent misdiagnosis of SPN.
-
Citations
Citations to this article as recorded by- Spleen Preservation in Solid Pseudopapillary Neoplasms of the Distal Pancreas: A Single-Center Experience
Tiffany M. Yue, Beatrice J. Sun, Daniel J. Delitto, Monica M. Dua, Jeffrey A. Norton, George A. Poultsides, Brendan C. Visser, Byrne Lee
Journal of Surgical Research.2025; 310: 17. CrossRef - Laparoscopic parenchyma-sparing resections for solid pseudopapillary tumors located in the head of pancreas
Zhengdong Zou, Lu Feng, Bing Peng, Jianhua Liu, Yunqiang Cai
BMC Surgery.2023;[Epub] CrossRef - Solid pancreatic masses in children: A review of current evidence and clinical challenges
Kelli N. Patterson, Andrew T. Trout, Archana Shenoy, Maisam Abu-El-Haija, Jaimie D. Nathan
Frontiers in Pediatrics.2022;[Epub] CrossRef - Pancreatic solid pseudopapillary neoplasm in male patients: systematic review with three new cases
Anna Caterina Milanetto, Anna-Lea Gais Zürcher, Lorenzo Macchi, Alina David, Claudio Pasquali
Updates in Surgery.2021; 73(4): 1285. CrossRef - Silencing c-Myc Enhances the Antitumor Activity of Bufalin by Suppressing the HIF-1α/SDF-1/CXCR4 Pathway in Pancreatic Cancer Cells
Xia Liu, Yayun Zhou, Jiamin Peng, Bei Xie, Qiyang Shou, Jianchao Wang
Frontiers in Pharmacology.2020;[Epub] CrossRef - Simultaneous colorectal and parenchymal-sparing liver resection for advanced colorectal carcinoma with synchronous liver metastases: Between conventional and mini-invasive approaches
Emilio De Raffele, Mariateresa Mirarchi, Dajana Cuicchi, Ferdinando Lecce, Riccardo Casadei, Claudio Ricci, Saverio Selva, Francesco Minni
World Journal of Gastroenterology.2020; 26(42): 6529. CrossRef - Solid pseudopapillary neoplasm of the pancreas showing marked distal atrophy
Masanori Tsujie, Tomoko Wakasa, Shigeto Mizuno, Hajime Ishikawa, Hironobu Manabe, Taichi Koyama, Kotaro Kitani, Shumpei Satoi, Keisuke Inoue, Shuichi Fukuda, Toshihiko Kawasaki, Masao Yukawa, Yoshio Ohta, Masatoshi Inoue
International Journal of Surgery Case Reports.2019; 55(C): 136. CrossRef - Solid pseudopapillary neoplasm of the pancreas in pediatric patients: A case report and institutional case series
Justin B. Mahida, Rajan K. Thakkar, Jon Walker, Rulong Shen, Brian D. Kenney, Vinay Prasad, Jennifer H. Aldrink
Journal of Pediatric Surgery Case Reports.2015; 3(4): 149. CrossRef - Onsite cytopathology evaluation and ancillary studies beneficial in EUS‐FNA of pancreatic, mediastinal, intra‐abdominal, and submucosal lesions
Shafqat Mehmood, Amna Jahan, Asif Loya, Muhammed Aasim Yusuf
Diagnostic Cytopathology.2015; 43(4): 278. CrossRef - Multicentric solid pseudopapillary neoplasms of the pancreas diagnosed by endoscopic ultrasound-guided fine needle aspiration: a case report
Megumi Yamaguchi, Toshikatsu Fukuda, Masahiro Nakahara, Mio Amano, Daisuke Takei, Masumi Kawashima, Yusuke Sumi, Hironobu Amano, Shuji Yonehara, Keiji Hanada, Toshio Noriyuki
Surgical Case Reports.2015;[Epub] CrossRef - A solid pseudopapillary neoplasm without cysts that occurred in a patient diagnosed by endoscopic ultrasound-guided fine-needle aspiration: a case report
Masakuni Fujii, Masao Yoshioka, Takefumi Niguma, Hiroaki Saito, Toru Kojima, Soichiro Nose, Junji Shiode
Journal of Medical Case Reports.2014;[Epub] CrossRef - Surgical Management and Long-Term Follow-Up of Solid Pseudopapillary Tumor of Pancreas: A Large Series from a Single Institution
Yunqiang Cai, Xun Ran, Siming Xie, Xin Wang, Bing Peng, Gang Mai, Xubao Liu
Journal of Gastrointestinal Surgery.2014; 18(5): 935. CrossRef - A case of solid-pseudopapillary neoplasm in a middle-aged male preoperatively diagnosed by endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA)
Shin KATO, Takuya HONBU, Moriya ZAKIMI, Kenji CHINEN, Tomiaki KUBOTA, Masayuki ARASHIRO, Kaoru KIKUCHI, Takahiro MURAKAMI, Fumihito KUNISHIMA
Suizo.2014; 29(2): 263. CrossRef - Endoscopic ultrasound-guided fine needle aspiration improves the pre-operative diagnostic yield of solid-pseudopapillary neoplasm of the pancreas: an international multicenter case series (with video)
Joanna K. Law, Alina Stoita, Wallia Weaver, Ferga C. Gleeson, Andrew M. Dries, Amanda Blackford, Vandhana Kiswani, Eun Ji Shin, Mouen A. Khashab, Marcia Irene Canto, Vikesh K. Singh, Anne Marie Lennon
Surgical Endoscopy.2014; 28(9): 2592. CrossRef - Multiple Diagnostic Imaging of a Patient with Solid Pseudopapillary Tumour of the Pancreas: EUS, CT and FDG PET/CT
Ari Chong, Jung-Min Ha, Seong Young Kwon
Nuclear Medicine and Molecular Imaging.2014; 48(1): 82. CrossRef
- Spleen Preservation in Solid Pseudopapillary Neoplasms of the Distal Pancreas: A Single-Center Experience
- Primary Monophasic Synovial Sarcoma Arising in the Mesentery: Case Report of an Extremely Rare Mesenteric Sarcoma Confirmed by Molecular Detection of a
SYT-SSX2 Fusion Transcript - Han Suk Ryu, Ilyeong Heo, Jae Soo Koh, Sung-Ho Jin, Hye Jin Kang, Soo Youn Cho
- Korean J Pathol. 2012;46(2):187-191. Published online April 25, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.2.187
- 7,943 View
- 42 Download
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Synovial sarcoma arises in the para-articular tissues, and it can also occur in various unexpected sites. We report a rare case of primary monophasic synovial sarcoma (MSS) arising in the mesentery. A 59-year-old man presented with a palpable abdominal mass. On microscopic examination, the entire tumor comprised a dense proliferation of the spindle cells without epithelial components. The tumor cells were positive for transducin-like enhancer of split 1, bcl-2, epithelial membrane antigen and CD99 but negative for CD34, CD117, alpha-smooth muscle actin, cytokeratin, and calretinin on immunohistochemistry. The reverse transcriptase-polymerase chain reaction revealed a single 151-bp fragment representing the
SYT-SSX2 fusion transcript. Because mesenteric MSS is extremely rare and many cases display histologic findings that overlap with those of more frequently involved tumors such as hemangiopericytoma and gastrointestinal stromal tumor, there is a chance of making an incorrect diagnosis that can result in an inappropriate treatment.-
Citations
Citations to this article as recorded by- A case of primary mesenteric synovial sarcoma: a challenging presentation
Nihed Abdessayed, Malek Barka, Samiha Mabrouk, Zeineb Nfikha, Zeineb Maatoug, Yosra Fejji, Mohamed Salah Jarrar, Sabri Youssef, Moncef Mokni
Surgical Case Reports.2023;[Epub] CrossRef - Giant solitary fibrous tumor of the pelvis
Gerardo Palmieri, Carmine Grassi, Luigi Conti, Filippo Banchini, Maria Diletta Daccò, Gaetano M. Cattaneo, Patrizio Capelli
International Journal of Surgery Case Reports.2020; 77(D): S52. CrossRef - Tumeur neuroectodermique gastro-intestinale (GNET) : à propos d’un cas de tumeur du grêle avec métastases hépatiques
Thibault Kervarrec, Claire Lecointre, Rémy Kerdraon, Guido Bens, Arnaud Piquard, Patrick Michenet
Annales de Pathologie.2015; 35(6): 506. CrossRef
- A case of primary mesenteric synovial sarcoma: a challenging presentation
- Expression of DNA Topoisomerase II-alpha as a Proliferating Marker in Urothelial Carcinoma of Urinary Bladder based on World Health Organization/International Society of Urological Pathology Consensus Classification: A Correlation with Expression of Ki-67 and Apoptosis
- Tae Jin Lee, Dong Ki Lee, Eon Sub Park, Jae Hyung Yoo
- Korean J Pathol. 2002;36(5):305-313.
- 2,041 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
DNA topoisomerase II-alpha is linked with active cell proliferation in mammalian cells. The aim of this study was to examine the relationship between the expression of DNA topoisomerase II-alpha as a proliferating marker, and the expression of Ki-67 and apoptosis in urothelial carcinoma of urinary bladder based on World Health Organization/International Society of Urological Pathology (WHO/ISUP) consensus classification.
METHODS
73 urothelial carcinomas of the urinary bladder after transurethral resection and 25 carcinomas after radical cystectomy were investigated for histologic grading based on WHO and WHO/ISUP consensus classification. Formalin fixed, paraffin embedded tissue of 98 specimens from 73 patients were immunohistochemically stained for DNA topoisomerase II-alpha and Ki-67, and in situ TdT-mediated dUTP-biotin nick end labeling method for evaluation of apoptotic cells was performed. For each case, a DNA topoisomerase II-alpha, Ki-67, and apoptotic indices were determined.
RESULTS
The histologic grades of 73 cases based on the WHO grading system were 21.9% (16 cases) in grade 1, 65.8% (48 cases) in grade 2, and 12.3% (9 cases). 5.5% (4 cases) of papillary neoplasm of low malignant potential, 47.9% (35 cases) of urothelial carcinoma of low grade, and 46.6% (34 cases) in urothelial carcinoma of high grade were reclassified using the WHO/ISUP consensus classification. Histologic grades based on two grading systems were correlated to invasion and stage (p<0.05). DNA topoisomerase II-alpha, Ki-67, and apoptotic indices were correlated to histologic grades based on two grading system and invasion. Also, the correlation of DNA topoisomerase II-alpha and Ki-67 indices, and DNA topoisomerase II-alpha and apoptotic indices were significant, respectively.
CONCLUSIONS
DNA topoisomerase II-alpha appears to be an useful marker for assessing the proliferation potential of urothelial carcinoma of in the urinary bladder.
- Dedifferentiated Extraskeletal Myxoid Chondrosarcoma of the Masticator Space: A Case Report.
- Geunyoung Jung, Kyung Ja Cho, Seung Ho Choi, Mi Jung Kim
- Korean J Pathol. 2011;45:S101-S105.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.S1.S101
- 4,801 View
- 36 Download
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - We describe a 69-year-old woman who presented with a dedifferentiated extraskeletal myxoid chondrosarcoma arising in the left masticator space. Computed tomography and magnetic resonance imaging revealed a 5 cm sized mass in the left masticator space. Histologically, the tumor consisted of two distinct areas. The less cellular area was a low-grade extraskeletal myxoid chondrosarcoma, composed of strands or cords of uniform spindle cells and abundant myxoid stroma. The more cellular, dedifferentiated area corresponded to a high grade myxofibrosarcoma, consisting of anaplastic tumor cells in myxoid stroma and geographic necrosis. The tumor cells of the former area were positive for S-100 protein, microtubule-associated protein-2 (MAP-2) and class III beta-tubulin, but negative for cytokeratin, smooth muscle actin, and desmin. The tumor cells in the latter, pleomorphic area showed MAP-2 and beta-tubulin immunoreactivity with a high Ki-67 labeling index. Based on its histologic and immunohistochemical features, the tumor was considered a dedifferentiated extraskeletal myxoid chondrosarcoma.
-
Citations
Citations to this article as recorded by- Extraskeletal myxoid chondrosarcoma of the parotid gland
NyimiBushabu Fidele, Wu Tianfu, Bing Liu, Yanfang Sun, Zhao Yifang
Annals of Maxillofacial Surgery.2019; 9(2): 439. CrossRef - Myxoid chondrosarcoma of maxilla: A rare case report
Hiralal Ash, Ajoy Kumar Shahi, Kabita Chatterjee, Dipankar Samaddar
Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology.2016; 28(3): 273. CrossRef - Maxillo-facial Extraskeletal Myxoid Chondrosarcoma: A Case Report and Discussion
Ratnadeep Ganguly, Abhishek Mukherjee
The Korean Journal of Pathology.2011; 45(6): 639. CrossRef
- Extraskeletal myxoid chondrosarcoma of the parotid gland
- Maxillo-facial Extraskeletal Myxoid Chondrosarcoma: A Case Report and Discussion.
- Ratnadeep Ganguly, Abhishek Mukherjee
- Korean J Pathol. 2011;45(6):639-643.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.6.639
- 4,383 View
- 25 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - In this report, we share our experience of a case of maxillo-facial extraskeletal myxoid chondrosarcoma, a very rare location for this neoplasm. In addition, a literature review is provided. The patient, a 61-year-old male, had a maxillary mass encroaching on the nasal cavity. After debulking, the tumor recurred, attaining its pre-surgical proportion in two months. The patient improved clinically with radiation and remained stable for about one year. However, he ultimately developed metastases in his lung which were treated with palliative chemotherapy with a good outcome lasting three months. We could find only eight reported cases of this tumor in the head region of which two are in the maxilla; hence, ruling out other primary sites is mandatory for a patient presenting with a primary head and neck mass. Surgical removal may be complicated because of the location. A combination of surgery and radiation is the management of choice, with palliative chemotherapy in metastasis.
-
Citations
Citations to this article as recorded by- Extraskeletal Myxoid Chondrosarcoma of Floor of Mouth—A Rare Case Report and Review of Literature
Surendra K Dabas, Nandini N Menon, Reetesh Ranjan, Bikas Gurung, Sukirti Tiwari, Bharat Bhushan Bassan, Himanshu Shukla, Sunil Pasricha, Ajit Sinha, Rahul Kapoor, Vinay Kumar Verma, Devesh Verma, Saurabh Arora, Ashwani Sharma, Sourabh Mukharjee, Rishu Sin
Indian Journal of Otolaryngology and Head & Neck Surgery.2024; 76(1): 1290. CrossRef - Intracranial Metastasis of Extracranial Chondrosarcoma: Systematic Review With Illustrative Case
Charles E. Mackel, Harry Rosenberg, Hemant Varma, Erik J. Uhlmann, Rafael A. Vega, Ron L. Alterman
Brain Tumor Research and Treatment.2023; 11(2): 103. CrossRef
- Extraskeletal Myxoid Chondrosarcoma of Floor of Mouth—A Rare Case Report and Review of Literature
- Expression of Hepatocyte Growth Factor/c-met by RT-PCR in Meningiomas.
- Na Rae Kim, Yang Seok Chae, Weon Jeong Lim, Seong Jin Cho
- Korean J Pathol. 2011;45(5):463-468.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.5.463
- 3,999 View
- 33 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Hepatocyte growth factor (HGF) is a potent mitogenic cytokine. C-met protein, which is known to be the HGF receptor has transmembrane tyrosine kinase activity and is encoded by the c-met oncogene. The HGF/c-met signaling pathway may play various roles in the carcinogenesis of various organs.
METHODS
We examined HGF and c-met mRNA expression by utilizing reverse transcription polymerase chain reaction on 40 surgically resected intracranial meningiomas (25 benign, 10 atypical, and 5 anaplastic cases).
RESULTS
An HGF overexpression was detected in 28%, 50%, and 80% of the benign, atypical and anaplastic meningiomas, respectively; a high expression of HGF or the coexpression of HGF/c-met was detected in the high grade meningiomas (the atypical and anaplastic cases, p=0.046, p=0.014). An HGF expression was statistically significant in the recurrent meningiomas (p=0.003), and HGF expression was significantly lower than c-met mRNA expression in benign meningiomas (p=0.034).
CONCLUSIONS
There was no correlation between histologic subtypes and HGF/c-met expression. Determination of HGF expression can be used as a molecular predictor for recurrence of meningioimas. These results suggest that HGF and c-met expression in meningiomas may be associated with anaplastic progression.
- The Histone Acetyltransferase hMOF is Overexpressed in Non-small Cell Lung Carcinoma.
- Joon Seon Song, Sung Min Chun, Ji Young Lee, Dong Kwan Kim, Yong Hee Kim, Se Jin Jang
- Korean J Pathol. 2011;45(4):386-396.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.4.386
- 6,085 View
- 69 Download
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
One of the histone acetyltransferases (HATs) family of proteins, human MOF (hMOF, MYST1), is involved in histone H4 acetylation, particularly at lysine 16 (H4K16Ac), an epigenetic mark of active genes. Dysregulation of the epigenetic mark influences cellular biology and possibly leads to oncogenesis. We examined the involvement of hMOF and H4K16Ac in primary non-small cell lung cancer (NSCLC).
METHODS
Reverse transcription polymerase chain reaction using fresh-frozen lung cancer tissues and lung cancer cell lines and immunohistochemistry for hMOF and H4K16Ac via tissue microarray of 551 formalin-fixed paraffin-embedded NSCLC tissue blocks were conducted.
RESULTS
hMOF mRNA was frequently overexpressed in lung cancer tissues, compared with normal lung tissues (10/20, 50%). NSCLC tissues were positive for hMOF in 37.6% (184/489) and H4K16Ac in 24.7% (122/493) of cases. hMOF protein expression was tightly correlated with the H4K16Ac level in tumors (p<0.001). Knockdown of hMOF mRNA with siRNA led to a significant inhibition of growth in the Calu-6 cell line.
CONCLUSIONS
hMOF was frequently expressed in NSCLC and was correlated with H4K16Ac. To our knowledge, this is the first study that has focused on the expression status of HATs and hMOF in NSCLC. Our results clearly suggest a potential oncogenic role of the gene and support its utility as a potential therapeutic target. -
Citations
Citations to this article as recorded by- Stabilization of MOF (KAT8) by USP10 promotes esophageal squamous cell carcinoma proliferation and metastasis through epigenetic activation of ANXA2/Wnt signaling
Peichao Li, Lingxiao Yang, Sun Young Park, Fanrong Liu, Alex H. Li, Yilin Zhu, Huacong Sui, Fengyuan Gao, Lingbing Li, Lan Ye, Yongxin Zou, Zhongxian Tian, Yunpeng Zhao, Max Costa, Hong Sun, Xiaogang Zhao
Oncogene.2024; 43(12): 899. CrossRef - The Biological Significance of Targeting Acetylation-Mediated Gene Regulation for Designing New Mechanistic Tools and Potential Therapeutics
Chenise O’Garro, Loveth Igbineweka, Zonaira Ali, Mihaly Mezei, Shiraz Mujtaba
Biomolecules.2021; 11(3): 455. CrossRef - Histone Acetyltransferase MOF Orchestrates Outcomes at the Crossroad of Oncogenesis, DNA Damage Response, Proliferation, and Stem Cell Development
Mayank Singh, Albino Bacolla, Shilpi Chaudhary, Clayton R. Hunt, Shruti Pandita, Ravi Chauhan, Ashna Gupta, John A. Tainer, Tej K. Pandita
Molecular and Cellular Biology.2020;[Epub] CrossRef - The Functional Analysis of Histone Acetyltransferase MOF in Tumorigenesis
Jiaming Su, Fei Wang, Yong Cai, Jingji Jin
International Journal of Molecular Sciences.2016; 17(1): 99. CrossRef - Expression of hMOF, but not HDAC4, is responsible for the global histone H4K16 acetylation in gastric carcinoma
LIN ZHU, JIAXING YANG, LINHONG ZHAO, XUE YU, LINGYAO WANG, FEI WANG, YONG CAI, JINGJI JIN
International Journal of Oncology.2015; 46(6): 2535. CrossRef - Arsenic Trioxide Reduces Global Histone H4 Acetylation at Lysine 16 through Direct Binding to Histone Acetyltransferase hMOF in Human Cells
Da Liu, Donglu Wu, Linhong Zhao, Yang Yang, Jian Ding, Liguo Dong, Lianghai Hu, Fei Wang, Xiaoming Zhao, Yong Cai, Jingji Jin, Tim Thomas
PLOS ONE.2015; 10(10): e0141014. CrossRef - The histone acetyltransferase hMOF suppresses hepatocellular carcinoma growth
Jin Zhang, Hui Liu, Hao Pan, Yuan Yang, Gang Huang, Yun Yang, Wei-Ping Zhou, Ze-Ya Pan
Biochemical and Biophysical Research Communications.2014; 452(3): 575. CrossRef - Regulation and function of histone acetyltransferase MOF
Yang Yang, Xiaofei Han, Jingyun Guan, Xiangzhi Li
Frontiers of Medicine.2014; 8(1): 79. CrossRef - The histone acetylranseferase hMOF acetylates Nrf2 and regulates anti‐drug responses in human non‐small cell lung cancer
Zhiwei Chen, Xiangyun Ye, Naiwang Tang, Shengping Shen, Ziming Li, Xiaomin Niu, Shun Lu, Ling Xu
British Journal of Pharmacology.2014; 171(13): 3196. CrossRef - Correlation of low expression of hMOF with clinicopathological features of colorectal carcinoma, gastric cancer and renal cell carcinoma
LINGLING CAO, LIN ZHU, JIAXING YANG, JIAMING SU, JINSONG NI, YUJUN DU, DA LIU, YANFANG WANG, FEI WANG, JINGJI JIN, YONG CAI
International Journal of Oncology.2014; 44(4): 1207. CrossRef - Coactivator MYST1 Regulates Nuclear Factor-κB and Androgen Receptor Functions During Proliferation of Prostate Cancer Cells
Anbalagan Jaganathan, Pratima Chaurasia, Guang-Qian Xiao, Marc Philizaire, Xiang Lv, Shen Yao, Kerry L. Burnstein, De-Pei Liu, Alice C. Levine, Shiraz Mujtaba
Molecular Endocrinology.2014; 28(6): 872. CrossRef - A potential diagnostic marker for ovarian cancer: Involvement of the histone acetyltransferase, human males absent on the first
NING LIU, RUI ZHANG, XIAOMING ZHAO, JIAMING SU, XIAOLEI BIAN, JINSONG NI, YING YUE, YONG CAI, JINGJI JIN
Oncology Letters.2013; 6(2): 393. CrossRef - Epigenetic change in kidney tumor: downregulation of histone acetyltransferase MYST1 in human renal cell carcinoma
Yong Wang, Rui Zhang, Donglu Wu, Zhihua Lu, Wentao Sun, Yong Cai, Chunxi Wang, Jingji Jin
Journal of Experimental & Clinical Cancer Research.2013;[Epub] CrossRef
- Stabilization of MOF (KAT8) by USP10 promotes esophageal squamous cell carcinoma proliferation and metastasis through epigenetic activation of ANXA2/Wnt signaling
- Telomerase Activity in Urethane-Induced Mouse Lung Tumorigenesis.
- Ji Sun Song, Soon Hee Jung, Sang Yeop Yi, Hwa Eun Oh, Mee Yon Cho, Kwang Hwa Park
- Korean J Pathol. 2011;45(3):261-270.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.3.261
- 4,281 View
- 25 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Telomerase activity in precancerous conditions of lung adenocarcinomas has not been well studied. This study is designed to investigate the role of telomerase in premalignant lesions of urethane-induced mouse lung adenocarcinoma.
METHODS
We harvested A/J mouse lung tissues at 3, 6, 9, 12, 28, 41, and 48 weeks after intraperitoneal urethane treatment, and classified each lesion in terms of histologic findings. We examined telomerase activity using a modified version of the telomeric repeat amplification protocol assay using both gel-based and enzyme linked immunosorbent assay methods. An immunohistochemical analysis of proliferating cell nuclear antigen (PCNA) was performed.
RESULTS
In urethane-induced mouse lung tissues, it was sequentially developed from hyperplasia, adenoma, and eventually to adenocarcinoma. Telomerase activity began to show a positive level in tissues with no histologically visible nodule after urethane administration. It revealed a statistically significant increase in hyperplasia compared to the "control" lung tissue (p<0.05), which was proportionally elevated relative to adenoma and adenocarcinoma. There was a direct correlation between telomerase activity and the PCNA labeling index (p<0.05).
CONCLUSIONS
The elevation of telomerase activity in normal-appearing lung lesions is thought to be a possible marker of early detection of pulmonary adenocarcinoma. -
Citations
Citations to this article as recorded by- Non-invasive quantification of cell-free DNA mutations in plasma during lung tumor progression in mice
Soo-Jin Kim, Eunhee Kim, Kyung-Taek Rim
Cancer Biomarkers.2017; 20(4): 477. CrossRef
- Non-invasive quantification of cell-free DNA mutations in plasma during lung tumor progression in mice
- Rapid and Sensitive Detection of KRAS Mutation by Peptide Nucleic Acid-based Real-time PCR Clamping: A Comparison with Direct Sequencing between Fresh Tissue and Formalin-fixed and Paraffin Embedded Tissue of Colorectal Cancer.
- Dongjun Jeong, Yujun Jeong, Jonghyun Lee, Moo Jun Baek, Yongbae Kim, Ji Hye Lee, Hyun Deuk Cho, Mee Hye Oh, Chang Jin Kim
- Korean J Pathol. 2011;45(2):151-159.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.2.151
- 6,188 View
- 84 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Rapid and sensitive detection of KRAS mutation is needed to maximize the benefits for patients who are being treated with monoclonal antibodies to target the epidermal growth factor receptor in colorectal cancer. The aim of this study is to evaluate the efficacy of the peptide nucleic acid clamp real-time PCR (PCqPCR) as compared to that of direct sequencing (DS) between using fresh colorectal cancer tissue and the matched formalin-fixed and paraffin-embedded (FFPE) colorectal cancer tissue.
METHODS
The efficacy of PCqPCR was evaluated and compared with that of DS using fresh tissue and matched FFPE tissue from 30 cases of colorectal cancer.
RESULTS
PCqPCR is more sensitive than DS for detecting KRAS mutation. PCqPCR detected 1% of mutants in 1 ng DNA. PCqPCR detected mutation in 1% of mutant cells, while DS barely detected, by manual reading, that in 20-50% of mutant cells. In the clinical samples, PCqPCR detected KRAS mutation in 60.0% while DS detected KRAS mutation in 53.3% of the colorectal cancers. The two methods showed a 100% concordance rate for detecting KRAS mutation between the fresh tissue and FFPE tissue.
CONCLUSIONS
The PCqPCR method is efficiently applicable for the detection of KRAS mutation in a clinical setting. -
Citations
Citations to this article as recorded by- Advances and Challenges in KRAS Mutation Detection and Clinical Implications
Maryam Sadat Mirlohi, Tooba Yousefi, Javad Razaviyan, Samira Nomiri, Esmail Pishbin, Meer-Taher Shabani-Rad, Mohammad Reza Ahmadian, Siamak Salami
Cancers.2025; 18(1): 31. CrossRef - NTRK oncogenic fusions are exclusively associated with the serrated neoplasia pathway in the colorectum and begin to occur in sessile serrated lesions
Jung Ho Kim, Jeong Hoon Hong, Yoon‐La Choi, Ji Ae Lee, Mi‐kyoung Seo, Mi‐Sook Lee, Sung Bin An, Min Jung Sung, Nam‐Yun Cho, Sung‐Su Kim, Young Kee Shin, Sangwoo Kim, Gyeong Hoon Kang
The Journal of Pathology.2021; 255(4): 399. CrossRef - Discrimination of the V600E Mutation in BRAF by Rolling Circle Amplification and Förster Resonance Energy Transfer
Mariia Dekaliuk, Xue Qiu, Frédéric Troalen, Pierre Busson, Niko Hildebrandt
ACS Sensors.2019; 4(10): 2786. CrossRef - Sensitive Genotyping of Somatic Mutations in the EGFR, KRAS, PIK3CA, BRAF Genes from NSCLC Patients Using Hydrogel Biochips
Marina Emelyanova, Ksenia Arkhipova, Natalia Mazurenko, Alexander Chudinov, Irina Demidova, Irina Zborovskaya, Lyudmila Lyubchenko, Alexander Zasedatelev, Tatiana Nasedkina
Applied Immunohistochemistry & Molecular Morphology.2015; 23(4): 255. CrossRef - Low Frequency of KRAS Mutation in Pancreatic Ductal Adenocarcinomas in Korean Patients and Its Prognostic Value
Mi Jung Kwon, Jang Yong Jeon, Hye-Rim Park, Eun Sook Nam, Seong Jin Cho, Hyung Sik Shin, Ji Hyun Kwon, Joo Seop Kim, Boram Han, Dong Hoon Kim, Yoon-La Choi
Pancreas.2015; 44(3): 484. CrossRef - Comparison of PNA clamping and direct sequencing for detecting KRAS mutations in matched tumour tissue, cell block, pleural effusion and serum from patients with malignant pleural effusion
Ji Young Kang, Chan Kwon Park, Chang Dong Yeo, Hea Yeon Lee, Chin Kook Rhee, Seung Joon Kim, Seok Chan Kim, Young Kyoon Kim, Mi Sun Park, Hyeon Woo Yim
Respirology.2015; 20(1): 138. CrossRef - BRAF V600E Mutation Analysis in Papillary Thyroid Carcinomas by Peptide Nucleic Acid Clamp Real-time PCR
Dongjun Jeong, Yujun Jeong, Ji Hye Park, Sun Wook Han, Sung Yong Kim, Yeo Joo Kim, Sang Jin Kim, Young Hwangbo, Soyoung Park, Hyun Deuk Cho, Mee Hye Oh, Seung Ha Yang, Chang Jin Kim
Annals of Surgical Oncology.2013; 20(3): 759. CrossRef - Detection and comparison of EGFR mutations in matched tumor tissues, cell blocks, pleural effusions, and sera from patients with NSCLC with malignant pleural effusion, by PNA clamping and direct sequencing
Chang Dong Yeo, Jin Woo Kim, Kwan Hyoung Kim, Jick Hwan Ha, Chin Kook Rhee, Seung Joon Kim, Young Kyoon Kim, Chan Kwon Park, Sang Haak Lee, Mi Sun Park, Hyeon Woo Yim
Lung Cancer.2013; 81(2): 207. CrossRef - Detection ofBRAFV600EMutations in Papillary Thyroid Carcinomas by Peptide Nucleic Acid Clamp Real-Time PCR: A Comparison with Direct Sequencing
Dongjun Jeong, Yujun Jeong, Sungche Lee, Hyeran Lee, Wanju Lee, Hyungjoo Kim, Doosan Park, Soyoung Park, Wenxia Mu, Hyun-Deuk Cho, Mee-Hye Oh, Sung Soo Lee, Seung-Ha Yang, Chang-Jin Kim
Korean Journal of Pathology.2012; 46(1): 61. CrossRef
- Advances and Challenges in KRAS Mutation Detection and Clinical Implications
- A Consideration of MGMT Gene Promotor Methylation Analysis for Glioblastoma Using Methylation-Specific Polymerase Chain Reaction and Pyrosequencing.
- Sang Hwa Lee, Tae Sook Hwang, Young Cho Koh, Wook Youn Kim, Hye Seung Han, Wan Seop Kim, Young Sin Ko, So Dug Lim
- Korean J Pathol. 2011;45(1):21-29.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.1.21
- 5,222 View
- 52 Download
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
O6-methylguanine-DNA methyltransferase (MGMT) gene promoter methylation is currently the most promising predictive marker for the outcome and benefit from temozolomide treatment in patients with glioblastoma, but there is no consensus on the analysis method for assessing the methylation status in the molecular diagnostic field. The objective of this study was to evaluate methylation-specific polymerase chain reaction (MSP) and pyrosequencing methods for assessing MGMT gene promotor methylation of glioblastoma as well as assessing the MGMT protein expression by immunohistochemistry.
METHODS
Twenty-seven cases of glioblastoma from the archives at the Department of Pathology Konkuk University Hospital were selected. MGMT promoter methylation was evaluated by MSP and the pyrosequencing methods. The MGMT expression was also measured at the protein level by immunohistochemistry.
RESULTS
Overall, MGMT hypermethylation was observed in 44.4% (12/27 cases) of the case of glioblastoma using either MSP or pyrosequencing. The concordant rate was 70.3% (19/27 cases) between MSP and pyrosequencing for MGMT methylation. There was no correlation between MGMT methylation and the protein expression. No significant differences in progression free survival and overall survival were seen between the methylated group and the unmethylated group by using either MSP or pyrosequencing. The status of the MGMT protein expression was correlated with progression free survival (p=0.026).
CONCLUSIONS
In this study the concordance rate between MSP and the pyrosequencing methods for assessing MGMT gene promotor methylation was relatively low for the cases of glioblastoma. This suggests that more reliable techniques for routine MGMT methylation study of glioblastoma remain to be developed because of quality control and assurance issues. -
Citations
Citations to this article as recorded by- Prognostic Role of Methylation Status of theMGMTPromoter Determined Quantitatively by Pyrosequencing in Glioblastoma Patients
Dae Cheol Kim, Ki Uk Kim, Young Zoon Kim
Journal of Korean Neurosurgical Society.2016; 59(1): 26. CrossRef - Distinct genetic alterations in pediatric glioblastomas
Sun-ju Byeon, Jae Kyung Myung, Se Hoon Kim, Seung-Ki Kim, Ji Hoon Phi, Sung-Hye Park
Child's Nervous System.2012; 28(7): 1025. CrossRef - MGMTGene Promoter Methylation Analysis by Pyrosequencing of Brain Tumour
Young Zoon Kim, Young Jin Song, Ki Uk Kim, Dae Cheol Kim
The Korean Journal of Pathology.2011; 45(5): 455. CrossRef
- Prognostic Role of Methylation Status of theMGMTPromoter Determined Quantitatively by Pyrosequencing in Glioblastoma Patients
- Utility of Promoter Hypermethylation for Differentiating Malignant and Benign Effusions in Liquid-Based Cytology Specimens.
- Ga Eon Kim, Jo Heon Kim, Yeong Hui Kim, Chan Choi, Ji Shin Lee
- Korean J Pathol. 2010;44(3):315-321.
- DOI: https://doi.org/10.4132/KoreanJPathol.2010.44.3.315
- 3,854 View
- 25 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Making the cytologic differentiation between benign and malignant effusions can be difficult. Because promoter hypermethylation of tumor suppressor genes is a frequent epigenetic event in many human cancers, it could serve as a marker for the diagnosis of cancer. The aim of this study was to investigate the feasibility of detecting promoter hypermethylation as a diagnostic tool with using liquid-based cytology samples for differentiating between malignant and benign effusions.
METHODS
A multiplex, nested, methylation-specific polymerase chain reaction analysis was used to examine promoter methylation of 4 genes (retinoic acid receptor-beta, [RAR-beta], adenomatous polyposis coli [APC], Twist and high in normal-1 [HIN-1]) in malignant (n = 85) and benign (n = 31) liquid-based cytology samples.
RESULTS
The frequencies of hypermethylation of RAR-beta, APC, Twist and HIN-1 were significantly higher in the malignant effusions than in the benign effusions (p < 0.001 for each). On the receiver-operating characteristic analysis, the area under the curve (AUC) for APC was the greatest. The AUC for the best two-gene combination (APC/HIN-1) was not statistically different from the AUC for the best individual tumor suppressor gene (APC).
CONCLUSIONS
This study suggests that promoter methylation analysis on residual liquid-based effusion samples may be a feasible approach to detect malignant effusions, and that APC is the best marker for differentiating between malignant and benign effusions. -
Citations
Citations to this article as recorded by- A comparative analysis of conventional cytopreparatory and liquid based cytological techniques (Sure Path) in evaluation of serous effusion fluids
Hrishikesh Dadhich, Pampa Ch Toi, Neelaiah Siddaraju, Kalidas Sevvanthi
Diagnostic Cytopathology.2016; 44(11): 874. CrossRef
- A comparative analysis of conventional cytopreparatory and liquid based cytological techniques (Sure Path) in evaluation of serous effusion fluids
- Comparison of Various Detection Methods of Mycobacterium Species in Formalin-Fixed Paraffin-Embedded Tissue with Chronic Granulomatous Inflammation.
- Hyun Seung Lee, Hyoungnam Lee, Soyoung Im, Yun Su Lee, Kyo Young Lee, Yeong Jin Choi
- Korean J Pathol. 2010;44(3):259-266.
- DOI: https://doi.org/10.4132/KoreanJPathol.2010.44.3.259
- 4,830 View
- 52 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
To determine the most effective method for detecting mycobacteria in formalin- fixed paraffin-embedded (FFPE) tissue, we compared the results of Ziehl-Neelsen stain (ZNS) and mycobacterial culture with those of polymerase chain reaction (PCR) and real-time quantitative PCR (RQ-PCR).
METHODS
We analyzed 54 cases diagnosed as chronic granulomatous inflammation. In all cases, ZNS and nested PCR using three different primers, IS6110, Mpb64 and IS6110/Rpobeta were done. RQ-PCR with the IS6110/Rpobeta primer was done in 51 cases.
RESULTS
Mycobacteria were identified by ZNS in 15/54 (27.8%) cases. RQ-PCR had the highest sensitivity (80.0%) compared to PCR with IS6110 (73.3%), Mpb64 (60.0%) and IS6110/Rpobeta (73.3%). Specificity was higher in all PCR experiments (79.5-82.1%) than in RQ-PCR (69.4%) experiments. The false negative rate was lowest for RQ-PCR (20.0%) than for PCR with IS6110 (26.7%), Mpb64 (40.0%) and IS6110/Rpobeta (26.7%). The false positive rate was highest for RQ-PCR (30.6%) compared to PCR with IS6110 (20.5%), Mpb64 (17.9%) and IS6110/Rpobeta (20.5%).
CONCLUSIONS
RQ-PCR had the highest sensitivity, and the lowest false negative rate, but it also had a higher false positive rate than PCR for detection of mycobacteria in FFPE tissues. -
Citations
Citations to this article as recorded by- Clinical Usefulness of PCR for Differential Diagnosis of Tuberculosis and Nontuberculous Mycobacterial Infection in Paraffin-Embedded Lung Tissues
Yo Na Kim, Kyoung Min Kim, Ha Na Choi, Ju Hyung Lee, Ho Sung Park, Kyu Yun Jang, Woo Sung Moon, Myoung Jae Kang, Dong Geun Lee, Myoung Ja Chung
The Journal of Molecular Diagnostics.2015; 17(5): 597. CrossRef - Usefulness of PCR to Mycobacterium Tuberculous and Nontuberculous Mycobacteria from Paraffin-embedded Tissues
Yeon-Il Choi, Hye-Young Kim
Korean Journal of Clinical Laboratory Science.2014; 46(2): 47. CrossRef
- Clinical Usefulness of PCR for Differential Diagnosis of Tuberculosis and Nontuberculous Mycobacterial Infection in Paraffin-Embedded Lung Tissues
- Aberrant Promoter Methylation of the Vimentin Gene in Colorectal Cancer Associated with the Adenoma-Carcinoma Sequence.
- Mi Hee Cho, Yu Mi Lee, Jin Sook Kim, Hyun Soo Kim, Kyung Hwa Lee, Sang Woo Juhng, Jae Hyuk Lee
- Korean J Pathol. 2010;44(2):179-186.
- DOI: https://doi.org/10.4132/KoreanJPathol.2010.44.2.179
- 4,762 View
- 37 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
DNA hypermethylation is a common epigenetic finding in human cancers and is closely associated with transcriptional silencing. In the present study, we investigated the proportion of colorectal neoplasms that showed the adenoma-carcinoma progression and vimentin gene methylation.
METHODS
Methylation status of the vimentin gene was examined in nontumoral mucosa, adenomas, and adenocarcinomas from 45 colorectal cancer patients who had adenoma and adenocarcinoma together. Methylation status was determined by bisulfite modification and the methylation-specific polymerase chain reaction. The expression of the vimentin gene product was also examined by immunohistochemistry.
RESULTS
Promoter methylation of vimentin was detected in 80% (36 out of 45 cases) of adenocarcinomas, 82.2% (37 of 45) of adenomas, and 28.9% (13 of 45) of normal epithelia, and the difference between neoplastic and normal specimens was statistically significant (p < 0.001). However, no significant correlations were observed between methylation frequency and clinicopathologic variables. Immunohistochemically, vimentin expression was not observed in either normal epithelial cells or tumor cells. Protein expression and vimentin promoter methylation were not associated.
CONCLUSIONS
The frequency of aberrant methylation of the vimentin gene was high in colonic adenomas and adenocarcinomas. This result suggests that the methylation status of vimentin may be clinically beneficial in screening for colorectal cancer patients and may be helpful in clarifying colorectal cancer biology. -
Citations
Citations to this article as recorded by- Epigenetic Modifications as Biomarkers of Tumor Development, Therapy Response, and Recurrence across the Cancer Care Continuum
Margaret Thomas, Paola Marcato
Cancers.2018; 10(4): 101. CrossRef - Aberrant promoter methylation of beta‐1,4 galactosyltransferase 1 as potential cancer‐specific biomarker of colorectal tumors
Maria Luana Poeta, Emanuela Massi, Paola Parrella, Pasquale Pellegrini, Mariangela De Robertis, Massimiliano Copetti, Carla Rabitti, Giuseppe Perrone, Andrea Onetti Muda, Francesca Molinari, Elena Zanellato, Stefano Crippa, Damiano Caputo, Marco Caricato,
Genes, Chromosomes and Cancer.2012; 51(12): 1133. CrossRef
- Epigenetic Modifications as Biomarkers of Tumor Development, Therapy Response, and Recurrence across the Cancer Care Continuum
- Predictive Significance of KRAS and Tau for Chemoresponse in Advanced Non-Small-Cell Lung Cancer.
- Jinyoung Yoo, Byoung Yong Shim, Chang Young Yoo, Seok Jin Kang, Kyo Young Lee
- Korean J Pathol. 2009;43(5):435-440.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.5.435
- 4,472 View
- 40 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Taxane-platinum combinations are often used as first-line treatments for patients with advanced non-small cell lung cancer (NSCLC). Response to chemotherapy for these patients is still poor. The aim of our study was to investigate, for this disease, whether KRAS and Tau proteins affect responses to taxane-platinum combinations.
METHODS
Expression of KRAS and Tau was examined immunohistochemically in 71 tumor samples obtained from patients with stage IIIB or IV NSCLC prior to combination therapy. Expression was correlated with tumor responses.
RESULTS
The response rate was 55% (39 of 71). KRAS and Tau were expressed in seven (10%) and 31 (44%) patients, respectively. All seven KRAS-positive patients were non-responders (p=0.014). Among Tau-positive patients, 35% (11 of 31) responded to therapy, whereas a partial response was observed in 70% (28 of 40) of Tau-negatives (p=0.045). Two were positive for both, and they were non-responders. In patients negative for both, the response rate was 71% (25 of 35) (p=0.012).
CONCLUSIONS
Expression of KRAS and Tau are significantly correlated with poor responses to this combination therapy in advanced NSCLC patients, and may be a useful marker for chemoresistance. -
Citations
Citations to this article as recorded by- Emerging Evidences for an Implication of the Neurodegeneration-Associated Protein TAU in Cancer
Stéphanie Papin, Paolo Paganetti
Brain Sciences.2020; 10(11): 862. CrossRef
- Emerging Evidences for an Implication of the Neurodegeneration-Associated Protein TAU in Cancer
- Soft Tissue Perineurioma : A Case Report .
- Jun Mo Kim, Joon Hyuk Choi
- Korean J Pathol. 2009;43(3):266-270.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.3.266
- 4,525 View
- 38 Download
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Soft tissue perineurioma is a very rare tumor composed of entirely of neoplastic perineurial cells. A 54-year-old woman presented with a palpable mass in the right lower leg. The mass was excised. Grossly, the tumor measured 2.0x2.0x1.5 cm. The cut surface was well circumscribed, pale pinkish gray, and rubbery soft. Histological examination showed that the tumor was composed of spindle cells within collagenous and myxoid stroma. The tumor cells had elongated, tapering nuclei with long and thin cytoplasmic processes, and were arranged in fascicular, whorled, and storiform pattern. The tumor cells were positive for epithelial membrane antigen and collagen type IV and negative for S-100 protein. Ultrastructurally, tumor cells showed long and thin cytoplasmic processes, pinocytic vesicles, and incomplete external lamina. The diagnosis of soft tissue perineurioma was confirmed by immunohistochemical stain and ultrastructural study.
-
Citations
Citations to this article as recorded by- Cutaneous Perineurioma of the Medial Superciliary Arch: An Uncommon Location for a Rare, Benign Spindle Cell Neoplasm
Sri Naidnur, Valeria González-Molina, Kara Asbury, Emily DeSantis, Rick Lin
Cureus.2026;[Epub] CrossRef - Trauma-induced Soft Tissue Perineurioma on the Thumb of a Filipino Female
Angeli Carina Lahoz, Zharlah Gulmatico Flores, Elisa Rae L. Coo
Journal of the Philippine Dermatological Society.2025; 34(2): 83. CrossRef - Extraneural Soft Tissue Perineurioma: A Report of a Rare Case of Peripheral Nerve Sheath Tumor
Ramki Arunachalam Ganesh, Karthikeyan Selvaraj, Srinivasan Chandran, Jesu Pencilin Yesuvadiyan
Cureus.2024;[Epub] CrossRef - Périneuriome extraneural des tissus mous localisé au nez
A. Zaouak, R. Benmously, M. Belhadj Salah, W. Koubaa, A. Debbiche, I. Mokhtar
Annales de Dermatologie et de Vénéréologie.2013; 140(8-9): 540. CrossRef - A Soft Tissue Perineurioma and a Hybrid Tumor of Perineurioma and Schwannoma
Ji Young Park, Nam Jo Park, Sang Pyo Kim, Kun Young Kwon, Sang Sook Lee
Korean Journal of Pathology.2012; 46(1): 75. CrossRef
- Cutaneous Perineurioma of the Medial Superciliary Arch: An Uncommon Location for a Rare, Benign Spindle Cell Neoplasm
- Endoscopic Ultrasound-Guided Fine Needle Aspiration Cytology in the Diagnosis of a Gastrointestinal Stromal Tumor of the Stomach: A Case Report.
- Lucia Kim, Hyung Gil Kim, Young Chae Chu, In Suh Park, Suk Jin Choi, Jee Young Han, Sun Hee Kim, Don Haeng Lee, Joon Mee Kim
- J Pathol Transl Med. 2008;19(2):178-182.
- DOI: https://doi.org/10.3338/kjc.2008.19.2.178
- 2,740 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - We report here a case of a gastrointestinal stromal tumor (GIST) in the stomach that was diagnosed by endoscopic ultrasound-guided fine needle aspiration cytology (EUS-FNA). A 67 year old male patient underwent regular check-ups for five years due to the presence of a submucosal tumor that was found in the fundus of the stomach incidentally. EUS-FNA was performed to evaluate the tumor, which had increased in size from 1cm to 2.8cm. A cytologic smear revealed cohesive sheets or clusters of spindle cells with elongated nuclei. Immunohistochemical staining revealed a strong positive reaction for c-kit and CD34, without any reaction for smooth muscle actin and Ki-67. Therefore, a diagnosis of GIST was made.
- Methylation Abnormality in Body Fluid Cytology: A Supplemental Molecular Marker for the Diagnosis of Malignant Mesothelioma.
- Joon Seon Song, Jin Kyung Jung, Ji Hye Kang, Ilseon Hwang, Se Jin Jang
- J Pathol Transl Med. 2008;19(2):126-135.
- DOI: https://doi.org/10.3338/kjc.2008.19.2.126
- 3,189 View
- 12 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Malignant mesothelioma (MM) is a highly lethal neoplasm arising in pleura and the peritoneum and a rapid and accurate diagnosis is crucial for treatment of the disease. However, the sensitivity of cytological analysis using pleural or ascitic fluid is relatively low, yielding an accurate diagnosis in only 32~79% of cases. We tested the diagnostic value of epigenetic alterations in body fluid cytology as a supplement to conventional methods. Paraffin-embedded tissue blocks from 21 MM patients and associated body fluid cytology slides considered no evidence of malignancy were used to test for epigenetic alteration. Using methylation-specific PCR, we detected methylation of RASSF1A and p16 in 47.6% (10/21) of both surgically resected tumor samples, respectively. Body fluid samples of MM also showed abnormal methylation of RASSF1A and p16INK4a genes in 38.1% (8/21) and 33.3% (7/21) of cases. The concordance in the rates of RASSF1A and p16INK4a gene-methylation abnormalities determined from cytology samples and tissue samples were 61.9% (13/21) and 66.7% (14/21), respectively. Combining both genes increases the sensitivity of the test to 57.1% (12 of 21) of cases. Our results suggest that testing for methylation abnormalities in selected individual genes or gene combinations has diagnostic value as an alternative or adjunct method to conventional cytological diagnosis.
-
Citations
Citations to this article as recorded by- Utility of Promoter Hypermethylation for Differentiating Malignant and Benign Effusions in Liquid-Based Cytology Specimens
Ga-Eon Kim, Jo-Heon Kim, Yeong-Hui Kim, Chan Choi, Ji Shin Lee
The Korean Journal of Pathology.2010; 44(3): 315. CrossRef
- Utility of Promoter Hypermethylation for Differentiating Malignant and Benign Effusions in Liquid-Based Cytology Specimens
- Central Core Disease: A Case Report.
- Ji Hoon Kim, Young S Park, Sung Hye Park, Je G Chi
- Korean J Pathol. 2004;38(1):68-71.
- 2,239 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - Central core disease is a rare autosomal dominantly inherited non-progressive congenital myopathy, which is pathologically characterized by the formation of a "core". We report a 28-year-old female with non-progressive muscle weakness, who had a hypotonic posture at birth. The developmental milestones were delayed with her first walking at 18 months of age. She could not run or walk a long distance and weight-bearing tasks were almost impossible. None of her family members showed motor symptoms. An investigation of the electromyography and nerve conduction velocity showed non-specific results. A gastrocnemius muscle biopsy revealed central cores in approximately 70% of myofibers with a type 1 myofiber predominance and deranged sarcolemmal structures. To the best of our knowledge, this is the fifth report of central core disease in the Korean literature.
- Ultrastructural and Immunohistochemical Investigations of Exocrine and Endocrine Cells in Fetal Human Pancreas.
- Jung Ran Kim, Je G Chi, Jung Hee Cho
- Korean J Pathol. 1995;29(3):286-295.
- 2,032 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - The pancreas consists of two types of tissue arising from same primitive cells, but with entirely different functions. Although the adult human pancreas and fetal islet tissue have been the subject of numerous electron microscopic studies, little is known of the ultrastructure of the developing human exocrine pancreas. The purpose of the current study is to investigate development of endo and exocrine of pancreas, especially during the middle trimester of human fetal life, which is the period of acinar cell maturation. Fresh autopsy specimens of pancreas, taken from 15 human fetuses at the 12th (n=2), 13-16th (n=5), 17-20th (n=4), 21-24th (n=2) and 25-28th (n=2) weeks of gestation, were studied electron microscopically, and immunohistochemically. Antisera against insulin, somatostatin, glucagon, pancreatic polypeptide and gastrin, were used for immunohistochemistry. By the 12th week, primitive exocrine acini were identified and these were matured rapidly in the next 6 weeks. At the 17th week stage, ultrastructural examination revealed atypical zymogen granules in the acinar cells. These became progressively less numerous in the 21-28 week period when classical zymogen granules increased upto the level of adult stage. All the endocrine cells were found at the 12th week, forming primitive or mature islets. The relative ratio of endocrine cells at the 12th week was about 35.4%, 24.9%, 39.8%, 0.5% for A, B, D & PP cell, respectively. But at the 25th to 28th week of development, the relative numbers of A and D cells decreased somewhat, whereas those of the B cells increased. The PP cells were constant. The G cells were found at the 12th week of fetal period, which appeared through out the on period.
- Telomerase mRNA Expression by In Situ Hybridization in Premalignant Lesions and Carcinomas of the Breast.
- Young Kyung Bae, Dong Sug Kim, Soo Jung Lee, Koing Bo Kwun
- Korean J Pathol. 2001;35(1):53-59.
- 1,981 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Telomerase is a ribonucleoprotein, DNA polymerase that synthesizes telomere repeats onto chromosomal ends and maintains telomere length. Telomerase activity has been detected in a broad range of human malignant neoplasms, but not in normal somatic cells. So, activation of telomerase may represent an essential step in the malignant transformation of cells. However, the expression of telomerase in premalignant lesions remains relatively unexplored. This study was conducted to investigate the reactivation of telomerase in the carcinogenesis of human breast tissue.
METHODS
In situ hybridization for the telomerase RNA component (human telomerase mRNA; hTR) was used in a normal breast tissue (n=41), florid ductal hyperplasia (FDH) (n=10), atypical ductal hyperplasia (ADH) (n=3), ductal carcinoma in situ (DCIS) (n=44) and invasive carcinoma (n=33). hTR expression in relation to p53 status and the pathologic parameters in breast cancer was also studied.
RESULTS
Expression of hTR was demonstrated in 13 samples (31.7%) of normal breast tissues, 4 (40%) of FDH, 3 (100%) of ADH, 42 (95.5%) of DCIS, and 33 (100%) of invasive carcinoma. The rate of hTR expression of ADH was significantly different from that of FDH (p<0.05), and there were no differences in hTR expression rates among ADH, DCIS and invasive carcinomas. There was no correlation between hTR expression and nuclear grade, tumor size, and p53 status in invasive carcinomas.
CONCLUSION
These results suggest that telomerase activation may be an early event and an essential step in the carcinogenesis of human breast tissue, and that telomerase has no correlations with p53 status and prognostic parameters.
- Improved Technique of Digoxigenin Labeled RNA in situ Hybridization.
- Suk Keun Lee, Yeon Sook Kim, In Sun Song, Sang Shin Lee, Young Jun Lee, Woo Ho Kim, Je Geun Chi
- Korean J Pathol. 2001;35(2):98-110.
- 2,128 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
A practical RNA in situ hybridization method using digoxigenin labeled RNA probes is described in order to evaluate the technical difficulties and problems in RNA in situ hybridization.
METHODS
The paraffin sections, routinely processed in the Pathology Laboratory, were tested for the possibility of RNA in situ hybridization instead of the RNase free paraffin sections, fixed in 4% paraformaldehyde and prepared using RNase protection procedures.
RESULTS
Most of the paraffin sections, fixed in 10% neutral formalin solution in fresh condition, showed relatively good reaction of RNA in situ hybridization, although the necrotic tissue and autopsy specimens showed poor reaction of RNA in situ hybridization. A refixation procedure using a 4% paraformaldehyde solution was evaluated for optimal expression of mRNA in the paraffin sections.
CONCLUSION
The treatment of 4% paraformaldehyde before the treatment of proteinase K showed better in situ hybridization than did the treatment of 4% paraformaldehyde after the treatment of proteinase K. Also a new Polymerase Chain Reaction (PCR)-based method of RNA probe production showed consistently good results.
- Fine Needle Aspiration Cytology of Pulmonary Carcinosarcoma.
- Tae Jung Jang, Kwang Gil Lee, Soon Won Hong
- J Pathol Transl Med. 1990;1(2):164-169.
- 2,628 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - Carcinosarcoma is an uncommon pulmonary malignancy characterized by carcinomatous parenchyma and sarcomatous stroma. The cytologic, immunohistochemical and ultrastructural features of a case of pulmonary carcinosarcoma suspected by fine needle aspiration cytology is presented. Only bizarre spindle cells arranged in loose groups, in microtissue fragments and in a dissociate fashion were present in the aspiration smears. They were markedly positive for vimentin. The epithelial component was not found, which was probably due to marked paucity of carcinomatous component that was proved by histologic examination of the resected tumor. The diagnosis of pulmonary carcinosarcoma should be considered whenever poorly differentiated epithelial cell groups with a malignant mesenchymal component set in a myxoid background are seen in a pulmonary cytology specimen.
- A Histopathologic Studies for Endometrium of Early Pregnancy.
- Mi Ja Lee, Kenn Hong Kee, Chae Hong Suh, Ho Jong Jeon
- Korean J Pathol. 1995;29(4):492-501.
- 1,858 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - Endometrium of early pregnancy were compared with nonpregnant endometnum by inimunohistochemical and ultrastructural techniques with respect to glandular and stromal elements of endometrium. The results obtained were as follows: 1. The AS cell in decidua has all the features of actively secreting glandular epithelium and shows the pronounced arrays of glandular endoplasmic reticulum and moderate numbers of ribosomes ultrastructually. Therefore the AS cell indicate considerable protein production, presumably contributing to both cell gowth and the production of secretions. 2. The process of decidualization can be characterized morphologically and immunohistochemically by the accumulation of basement membrane-like materials, such as laminin and type IV collagen which may be related to the hormonal stimulation occuring during pregnancy and trophoblastic attachment. 3. The decidual cells show strong positive for vimentin and some large mature decidual cells show weakly positive for lysozyme and cti- antitrypsin, which might represent more the sequential differentiation of stromal cells into decidual cells than origin of histiocytes. 4. Immunoreactivity with S-100 protein was found in glandular and stromal cells of decidua but negative in endometrium of nonpregnant women. So some humoral factors related to pregnancy stimulate expression of S-100 protein in glandular and stromal cells of decidua.
- Detection of Human Papillomavirus DNA 16/18 in Cervical Adenocarcinomas by Polymerase Chain Reaction.
- Sang Sook Lee, Nam Jo Park, Chong Guk Yoon
- Korean J Pathol. 1995;29(4):502-510.
- 2,457 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - Twenty-five paraffin-embedded tumor tissues were analyzed for detection of HPV 16 and 18 in cervical adenocarcinoma by polymerase chain reaction with type specific primers and by non-radioactive Southern blot hybridization for confirmation . The suitability of paraffin-embedded tissue as PCR material was confirmed by successful amplification of 100% of cervical specimens with human -globin specific primer. Eighty four percent of the cervical adenocarcinoma tissues were positive for HPV 16 and/or 18. HPV 16 positive rate was 68%, HPV 18 was 60%. The double infection with HPV 16 and 18 was found in 44%. Three cases of the negative specimen in PCR for each type of HPV DNA 16 and 18 were positive in Southern blot hybridization. The total positive rate was 92% for HPV 16 and/or HPV 18, HPV 16 positive rate was 80%. HPV 18 was 72%. The double infection with HPV 16 and 18 was 60%. These results suggest that the pattern of HPV types 16 and 18 is closely associated with carcinogenesis of cervical cancers. HPV type 18 appears to be preferentially related to cervical adenocarcinoma and the poor prognosis of these patients. Therefore, determination of HPV DNA type in cervical carcinoma patients is important in treatment and prognosis.
- Chromophobe Renal Cell Carcinoma.
- Yeong Jin Choi, Tae Kon Hwang, Youn Soo Lee, Eun Jung Lee, Seok Jin Kang, Byung Kee Kim, Sang In Shim
- Korean J Pathol. 1999;33(4):259-266.
- 2,220 View
- 26 Download
-
 Abstract
Abstract
 PDF
PDF - We report 13 chromophobe renal cell carcinomas (10.8%) observed among 120 renal cell carcinomas in adults. The average age was 53 (range: 34-72) years old, and 6 were males and 7 females. The mean tumor size was 10 (range: 5-17) cm, mean nuclear grade 2.4, and mean Robson's stage was 1.9. There were two distinct histologic variants; typical variant (n=9) and eosinophilic variant (n=4). Both of them showed typical light microscopic features and positive reaction with Hale's colloidal iron and carbonic anhydrase II, a marker protein of intercalated cells of renal collecting ducts. A strong positive immunoreactivity for epithelial membrane antigen was noted in the cytoplasm in 12 of 13 tumors. Numerous microvesicles, 180~440 nm in diameter, were identified ultrastructurally. DNA aneuploidy was found in 3 out of 10 cases. Neither local recurrence nor metastasis have been identified during the following period of 4~144 (mean 48) months.
- ras Gene Mutations in Malignant Fibrous Histiocytoma.
- Jinyoung Yoo, Ah Won Lee, Seok Jin Kang, Byung Kee Kim
- Korean J Pathol. 2001;35(3):232-237.
- 2,007 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
ras gene mutations have been described in various human malignancies, suggesting that their activation may play a role in oncogenesis. However, there are few reports concerning ras gene alterations in malignant fibrous histiocytomas. We therefore designed a study to determine the prevalence and type of mutations in the first exons of H-ras and K-ras genes in these tumors.
METHODS
Twenty-seven malignant fibrous histiocytomas were investigated by direct sequencing analysis with the automated DNA sequencing of polymerase chain reaction-amplified ras sequences.
RESULTS
Twenty-four mutations were found in 18 (67%) of the tumors: GGC to GAC transition mutations at codon 13 of K-ras (coding for aspartic acid instead of glycine) in 18 of the samples and GGC to GTC transversions at codon 12 of H-ras (coding for valine instead of glycine) in six of the lesions.
CONCLUSIONS
Our data suggest an involvement of the ras gene mutation in conjunction with other yet unknown events in the tumorigenesis and/or progression of malignant fibrous histiocytomas. The K-ras gene activation predominated in these tumors by a mutation at codon 13. It is noteworthy that H-ras mutations were detected only in association with the lesions containing K-ras mutated genes, the significance of which remains to be determined.
- Immunohistochemical Study on the Ha-ras p21 Expression in the Gastric Carcinoma.
- Kwang Min Lee, Joo Yong Yoo
- Korean J Pathol. 1990;24(1):1-9.
- 2,019 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - We have investigated an immunohistochemical expression of the Human-Ha-ras oncogene product p21 in tumor cells of the primary mass and metastatic lymph nodes with different histological features of gastric cancer by using avidinbiotin complex immunoperoxidase method in formalin-fixed tissue sections from 73 cases of primary tumor mass and 23 cases of metastatic lymph node. Histologic type of the gastric cancer was classification. The results obtained were as follows: 1) Expression of Ha-ras p21 was consistantly increased in the well differentiated tubular adenocarcinoma as compared with poorly differentiated tubular adenocarcinoma (p<0.01), and was substantially decreased in mucinous carcinoma and signet ring cell carcinoma. 2) Signet ring cell carcinoma showed that positive immunoperoxidase reaction for Ha-ras p21 exhibited in the majority of immature signet ring cell with scant cytoplasm rather than in the mature signet ring cells which have abundant cytoplasm filled with mucin. This findings indicate that mucin production from the tumor cell was not correlated with activation of ras gene in the tumor tissue of gastric carcinoma. 3) In general Ha-ras p21 expression was enhanced in the metastatic tumor cells of the regional lymph node compared with primary tumor, especially it was consistantly increase in the well differentiated tubular adenocarcinoma.
- Imprint Cytologic Feature of Extraskeletal Osteosarcoma: A Case Report.
- Mi Jin Gu, Young Kyung Bae, Mi Jin Kim, Joon Hyuk Choi, Won Hee Choi
- J Pathol Transl Med. 2000;11(1):59-63.
- 2,127 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - Extraskeletal osteosarcoma is an uncommon tumor originated from soft tissue without evidence of skeletal involvement. It usually affects adults and its common locations are extremity, buttock, and retroperitoneum. Although the histologic feature of this tumor is well known, there have been few reports on the fine needle aspiration cytologic findings. We report the imprint cytologic feature of extraskeletal osteosarcoma. The patient was a 49-year-old man with a mass of the left anterior chest for 2 years. On the imprint preparation, the smears showed malignant round, polygonal or spindle cells with coarsely clumped chromatin and occasionally prominent nucleoli. The malignant cells occur singly, in clusters, or associated with amorphous eosinophilic osteoid. Mitotic figures are also seen.

 E-submission
E-submission


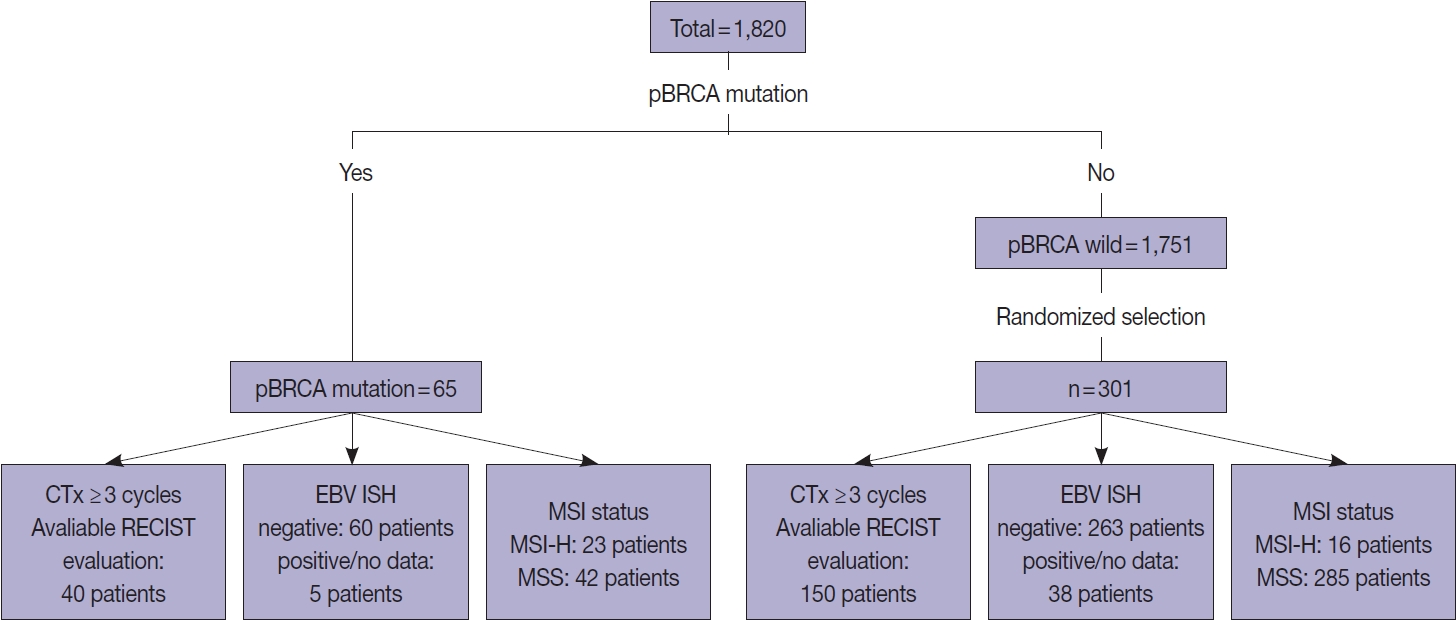

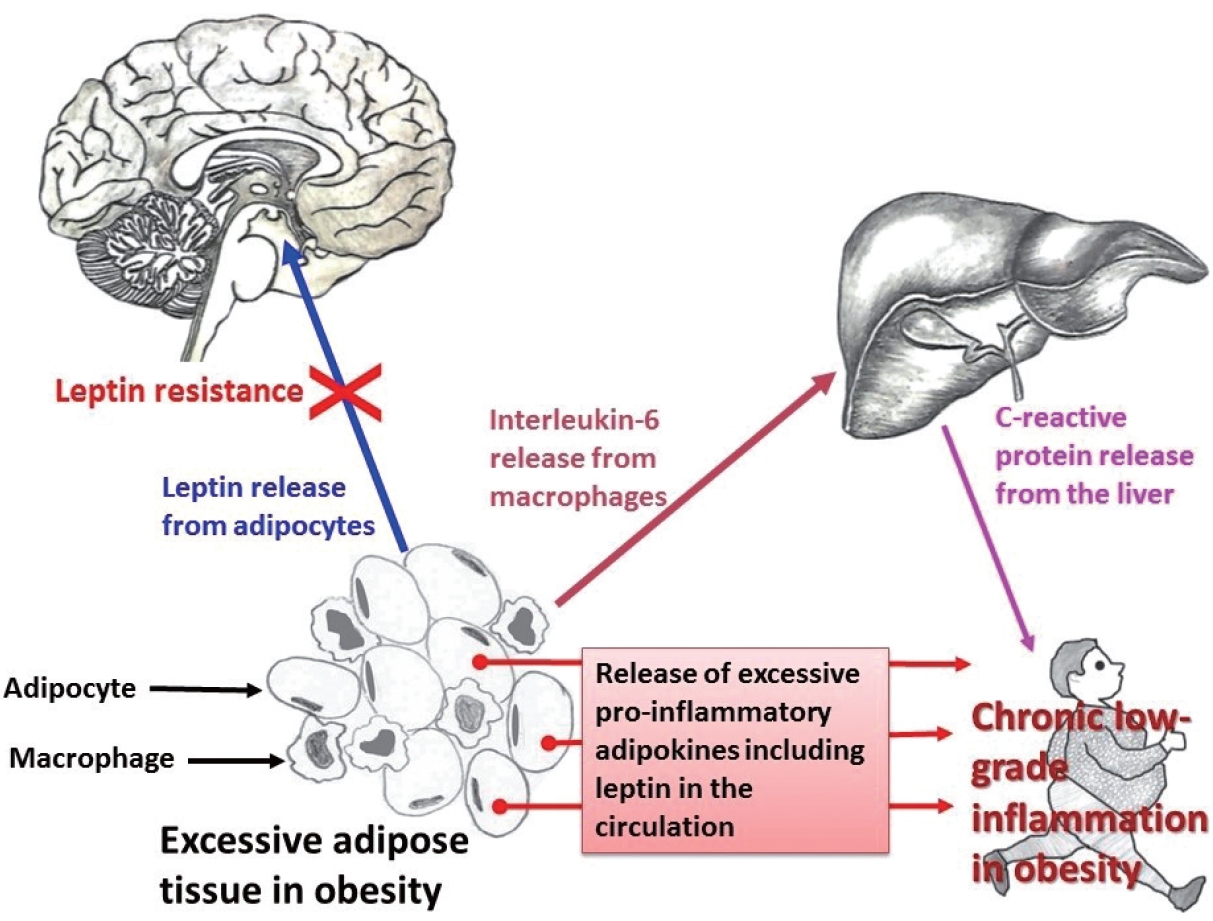
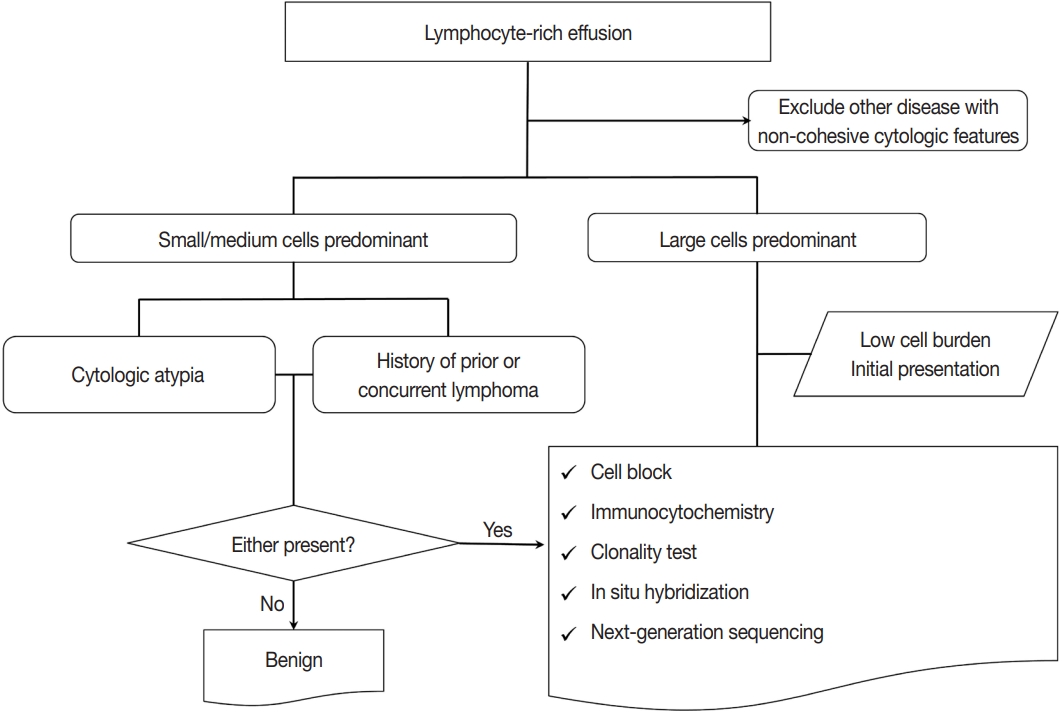
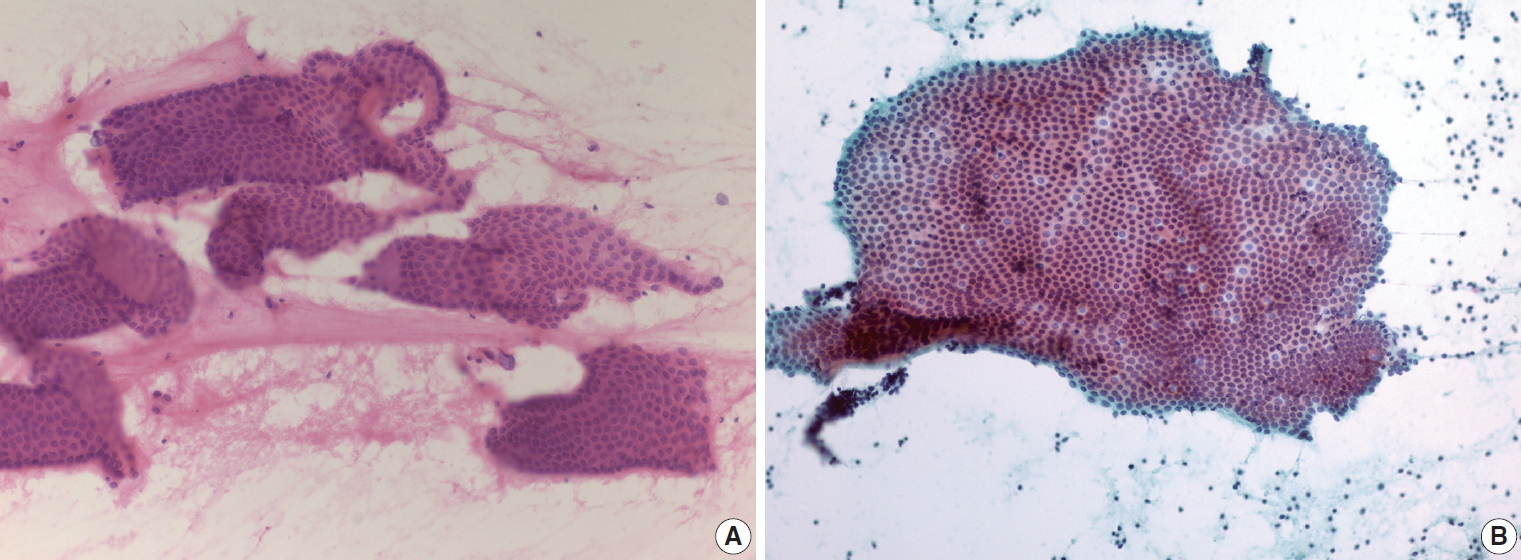
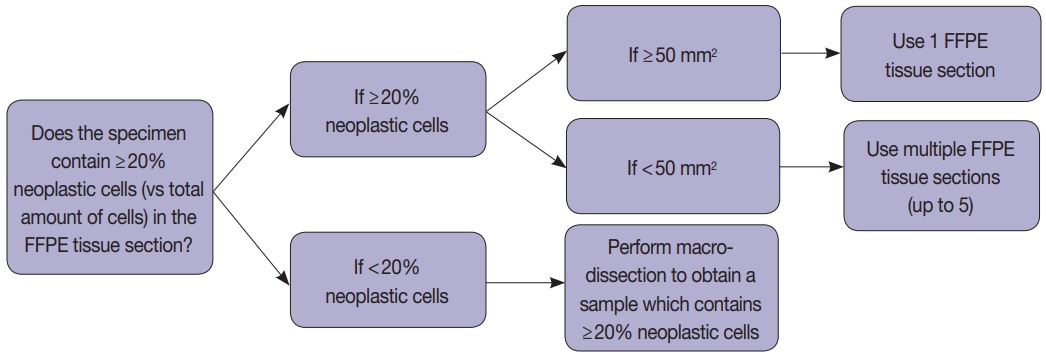
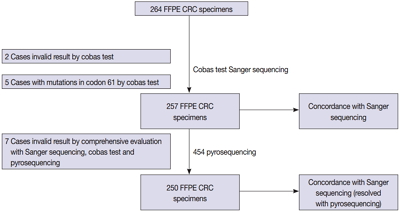
 First
First Prev
Prev



