Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 47(6); 2013 > Article
-
Brief Case Report
Inflammatory Pseudotumor-like Follicular Dendritic Cell Tumor of the Spleen with Extensive Histiocytic Granulomas and Necrosis: A Case Report and Literature Review - Hyun-Jung Kim, Ji Eun Kim1, Gu-Hyun Kang, Jung Yeon Kim, Kyeongmee Park
-
Korean Journal of Pathology 2013;47(6):599-602.
DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.6.599
Published online: December 24, 2013
Department of Pathology, Inje University Sanggye Paik Hospital, Inje University College of Medicine, Seoul, Korea.
1Department of Pathology, SMG-SNU Boramae Medical Center, Seoul National University College of Medicine, Seoul, Korea.
- Corresponding Author: Hyun-Jung Kim, M.D. Department of Pathology, Inje University Sanggye-Paik Hospital, 1342 Dongil-ro, Nowon-gu, Seoul 139-707, Korea. Tel: +82-2-950-1261, Fax: +82-2-951-6964, hjkim@paik.ac.kr
© 2013 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
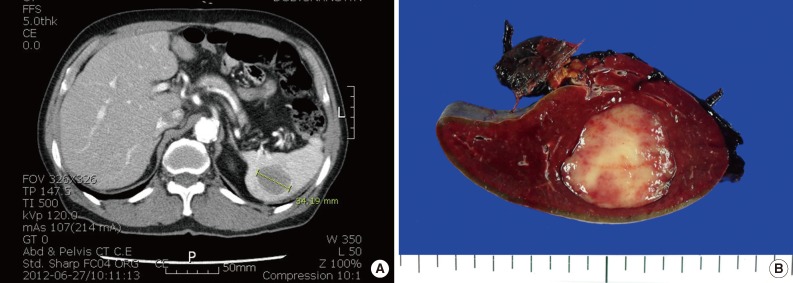
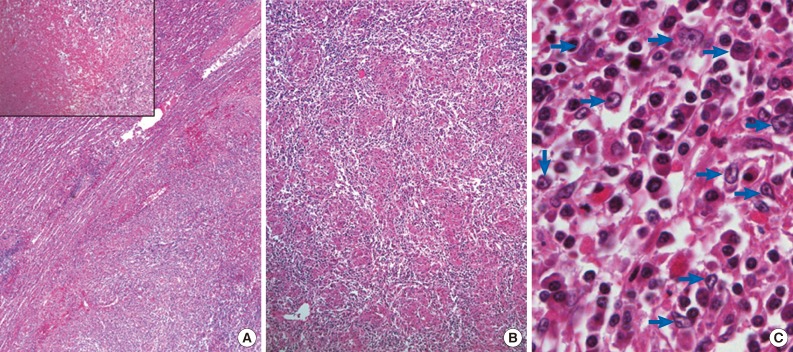
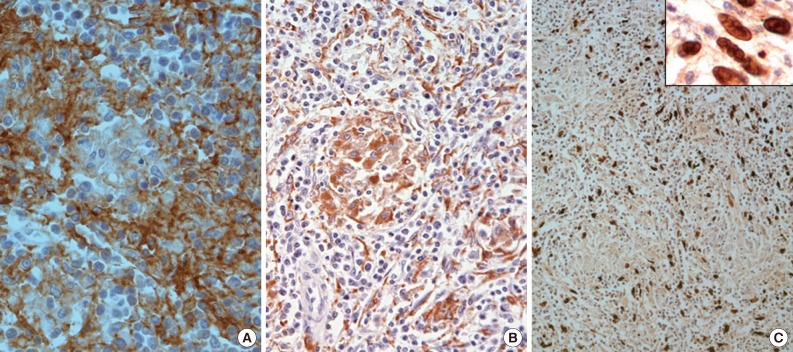
- A 76-year-old man underwent abdominal-pelvic computed tomography for follow-up of previous gastric cancer (disease-free state for five years after radical subtotal gastrectomy). A newly developed splenic mass had been increasing in size for the previous six months (1.9 to 3.4 cm) (Fig. 1A). There was no evidence of local recurrence or metastasis, even on positron emission tomography-computed tomography. A splenectomy was performed. A well-defined gray-whitish firm nodule (3.2 cm in greatest dimension) was detected (Fig. 1B). Microscopically, the well-defined lesion was composed of an admixture of inflammatory cells and spindle cells in a background of numerous histiocytic granulomas and central coagulative necrosis (Fig. 2A, B). The oval to spindle cells had pale or eosinophilic cytoplasms with indistinct cell borders. The nuclei were enlarged and twisted or irregularly folded. Small but distinct, centrally located nucleoli were often evident (Fig. 2C). Mitotic figures were not found. The infiltrating reactive inflammatory cells were predominantly composed of lymphocytes, plasma cells, and a small number of eosinophils. The immunohistochemical results are as follows: CD35+ (Fig. 3A), CD21-, smooth muscle actin (SMA)-, and anaplastic lymphoma kinase- in oval to spindle cells, mixed imfiltration of CD3+ and CD20+ lymphocytes, and CD68+ in histiocytes (Fig. 3B). The Ki-67 labeling index was about 30% in spindle cells. EBV in situ hybridization (EBV-ISH) revealed diffuse and strong positivity in oval to spindle cells (Fig. 3C). Special stains for bacteria, acid-fast bacilli and fungi showed no organisms.
CASE REPORT
- An IPT-like FDCT is extremely rare, and the pathogenesis and clinicopathologic characteristics are not clearly defined. The reviewed papers revealed seven cases in the spleen, ten cases in the liver, and one case in the peripancreas. The range of age was variable, from 19 to 77 years. The tumor size ranged from 3.5 to 22 cm. The clinical outcome was relatively fair, but three casesd disclose several recurrences and one case showed metastasis.2,9 The reported cases are summarized in the Table 1.
- The collective immunohistochemical results9 of IPT-like FDCTs are as follows: CD21/CD35-positive in spindle cells (80%), 46.2% for CD23, 16.7% for SMA and 100% for EBV-ISH, which demonstrate that the first lines of investigation for IPT-like FDCT are FDC markers and EBV-ISH. In the present case, the tumor cells were highlighted at EBV-ISH.
- The main pathogenesis of IPT-like FDCT has been hypothesized to occur through hepatic and splenic IPT-like tumors arising from a common mesenchymal cell, but using one of three different pathways; mostly myofibroblastic (SMA+), with a minor fraction via FDC lineage (CD21+, CD35+, and CD23+) or histiocyte (CD68+). CD21 expressed in FDC is a well-known EBV receptor, functionally active EBV-transformed FDC cell lines have been successfully established, and clonal EBV infection in some IPT-like FDCTs has been demonstrated. Based on these findings, it has been suggested that EBV might be involved in the pathogenesis of IPT-like FDCTs.9
- A histiocytic granuloma is a unique feature of this case, which does not seem to be a well-formed granuloma, but plump histiocytic aggregates with multinucleated giant cells. No infectious organism was detected.
- Coagulative necrosis was evident at the central portion of tumor, which may have been related with relatively rapid growth rate in a short time period. This finding has not been described yet.
- In summary, we present a case of IPT-like FDCT in the spleen of a patient with a history of gastric carcinoma. This tumor showed distinct histologic features with extensive histocytic granulomas in a mixed inflammatory background.
DISCUSSION
This case was presented at 64th fall meeting of Korean Society of Pathologist (E-poster and poster exhibition Abstract #121).
No potential conflict of interest relevant to this article was reported.
- 1. Cheuk W, Chan JK, Shek TW, et al. Inflammatory pseudotumor-like follicular dendritic cell tumor: a distinctive low-grade malignant intra-abdominal neoplasm with consistent Epstein-Barr virus association. Am J Surg Pathol 2001; 25: 721-731. PubMed
- 2. Horiguchi H, Matsui-Horiguchi M, Sakata H, et al. Inflammatory pseudotumor-like follicular dendritic cell tumor of the spleen. Pathol Int 2004; 54: 124-131. ArticlePubMed
- 3. Neuhauser TS, Derringer GA, Thompson LD, et al. Splenic inflammatory myofibroblastic tumor (inflammatory pseudotumor): a clinicopathologic and immunophenotypic study of 12 cases. Arch Pathol Lab Med 2001; 125: 379-385. PubMed
- 4. Kutok JL, Pinkus GS, Dorfman DM, Fletcher CD. Inflammatory pseudotumor of lymph node and spleen: an entity biologically distinct from inflammatory myofibroblastic tumor. Hum Pathol 2001; 32: 1382-1387. ArticlePubMed
- 5. Chen TC, Kuo TT, Ng KF. Follicular dendritic cell tumor of the liver: a clinicopathologic and Epstein-Barr virus study of two cases. Mod Pathol 2001; 14: 354-360. ArticlePubMedPDF
- 6. Brittig F, Ajtay E, Jaksó P, Kelényi G. Follicular dendritic reticulum cell tumor mimicking inflammatory pseudotumor of the spleen. Pathol Oncol Res 2004; 10: 57-60. ArticlePubMedPDF
- 7. Bai LY, Kwang WK, Chiang IP, Chen PM. Follicular dendritic cell tumor of the liver associated with Epstein-Barr virus. Jpn J Clin Oncol 2006; 36: 249-253. ArticlePubMed
- 8. Lewis JT, Gaffney RL, Casey MB, Farrell MA, Morice WG, Macon WR. Inflammatory pseudotumor of the spleen associated with a clonal Epstein-Barr virus genome: case report and review of the literature. Am J Clin Pathol 2003; 120: 56-61. ArticlePubMed
- 9. Yoon SO, Ko H, Kim BH, Kwon GY, Jeon YK, Kim CW. Epstein-Barr virus-associated inflammatory pseudotumor-like follicular dendritic cell tumor in the spleen of a patient with diffuse large B cell lymphoma: a case report and review of the literature. Korean J Pathol 2007; 41: 198-202.
REFERENCES
| Case | Age (yr) | Sex | Size (cm) | Symptoms | Treatment | Outcome | |
|---|---|---|---|---|---|---|---|
| Spleen | 1 | 70 | M | 5.5 | Asymptomatic | NA | NA |
| 2 | 58 | F | 22 | Abdominal dullness, easy bruising | Splenectomy | Alive well at 4 mo | |
| 3 | 39 | F | 7.5 | Weight loss, fever | Splenectomy | Alive at 2 mo | |
| 4 | 61 | F | 3.5 | Asymptomatic | Splenectomy | Recent case | |
| 5 | 77 | F | 11 | Epigastralgia | Splenectomy | Alive well (3 yr) | |
| 6 | 64 | F | 5.1 | NA | Splenectomy | Metastasis | |
| 7a | 76 | M | 3.2 | Asymptomatic | Splenectomy | Alive well (7 mo) | |
| Liver | 1 | 68 | F | 11 | Malaise, weight loss | Excision of mass | Alive well (2.5 yr) |
| 2 | 57 | F | 9.5 | Intermittent epigastralgia | No surgery | Enlarged to 15 cm, no metastasis (3 yr) | |
| 3 | 51 | F | 15 | Abdominal fullness, weight loss | Lt. lobectomy | Alive well (1 yr) | |
| 4 | 19 | F | 12 | RUQ abdominal pain, weight loss | Surgical excision | Alive well (40 mo) | |
| 5 | 56 | F | 15 | Gastointestinal upset | Rt. lobectomy | Recur (× 3), alive with disease (56 mo) | |
| 6 | 40 | F | 12.5 | Epigastric pain, weight loss | Lt. hepatectomy | Intra-abdominal recurrence | |
| 7 | 49 | F | 4.2 | Asymptomatic | Surgical excision | Alive well (9 mo) | |
| 8 | 37 | M | 15 | Malaise, weight loss, gross hepatomegaly | Rt. trisegmentectomy | Alive well (42 mo) | |
| 9 | 35 | F | 20 | Epigastric discomfort, fever, weight loss | Rt. hemihepatectomy | Recur (× 3), died for dissemination (95 mo) | |
| 10 | 31 | F | 15 | Abdominal distension, weight loss | Rt. hemihepatectomy | Subtle involvement of porta hepatis LN; alive well (60 mo) | |
| 11 | 49 | F | 9.5 | Abdominal distension (peripancreas) | Whipple’s operation | Recent case |
Figure & Data
References
Citations

- Epstein-Barr virus-positive inflammatory follicular dendritic cell sarcoma with significant granuloma: case report and literature review
Chenchen Nie, Xun Xie, Hangyan Li, Yangcan Li, Zhihong Chen, Yanchun Li, Zhenfeng Li
Diagnostic Pathology.2024;[Epub] CrossRef - Case report: Hepatic inflammatory pseudotumor-like follicular dendritic cell sarcoma: A rare case and minireview of the literature
Fan Ding, Chao Wang, Chi Xu, Hui Tang
Frontiers in Medicine.2022;[Epub] CrossRef - Inflammatory pseudotumor-like follicular dendritic cell sarcoma: Literature review of 67 cases
Hao Wu, Peng Liu, Xiao-Ran Xie, Jing-Shu Chi, Huan Li, Can-Xia Xu
World Journal of Meta-Analysis.2021; 9(1): 1. CrossRef - Granuloma With an Underlying Lymphoma: A Diagnostic Challenge and a Wider Histologic Spectrum Including Adult T-Cell Leukemia/Lymphoma
Chih-Ying Wu, Ren-Ching Wang, Bo-Jung Chen, Wei-Yu Chen, Jie-Yang Jhuang, Ming-Chih Chang, Yu-Hung Wu, Norihiro Nakada, Kennosuke Karube, Shih-Sung Chuang
Applied Immunohistochemistry & Molecular Morphology.2020; 28(4): 316. CrossRef - A Case of Laparoscopically Resected EBV-related Inflammatory Pseudotumor-Like Follicular Dendritic Cell Tumor of the Spleen
Tomoya HIRAI, Yuki HOMMA, Yasuhiro SHIMIZU, Takahumi KUMAMOTO, Ryusei MATSUYAMA, Shoji YAMANAKA, Itaru ENDO
Nihon Rinsho Geka Gakkai Zasshi (Journal of Japan Surgical Association).2020; 81(8): 1631. CrossRef - Histiocytic and Dendritic Cell Neoplasms
Zenggang Pan, Mina L. Xu
Surgical Pathology Clinics.2019; 12(3): 805. CrossRef - Inflammatory pseudotumor-like follicular dendritic cell sarcoma: A brief report of two cases
Bi-Xi Zhang, Zhi-Hong Chen, Yu Liu, Yuan-Jun Zeng, Yan-Chun Li
World Journal of Gastrointestinal Oncology.2019; 11(12): 1231. CrossRef - Diagnosis of EBV-Associated Inflammatory Pseudotumor in the Spleen: A Case Report
Dmitrii Il’ich Chebotarev, A. M. Kovrigina, S. M. Korzhova, K. I. Danishyan, K. R. Sabirov
Clinical Oncohematology.2019; 12(4): 428. CrossRef - Inflammatory pseudotumor-like follicular dendritic cell tumor: an underdiagnosed neoplasia
Aline Caldart Tregnago, Diogo Lago Morbeck, Felipe D’Almeida Costa, Antonio Hugo José Froes M. Campos, Fernando Augusto Soares, José Vassallo
Applied Cancer Research.2017;[Epub] CrossRef - Clinicopathological features of inflammatory pseudotumour‐like follicular dendritic cell tumour of the abdomen
Yanyang Chen, Huijuan Shi, Hui Li, Tiantian Zhen, Anjia Han
Histopathology.2016; 68(6): 858. CrossRef - Inflammatory pseudotumour-like follicular dendritic cell tumour of the spleen
Raisuke Nishiyama, Satoshi Baba, Yoichi Watahiki, Hirotoshi Maruo
BMJ Case Reports.2015; 2015: bcr2014206373. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
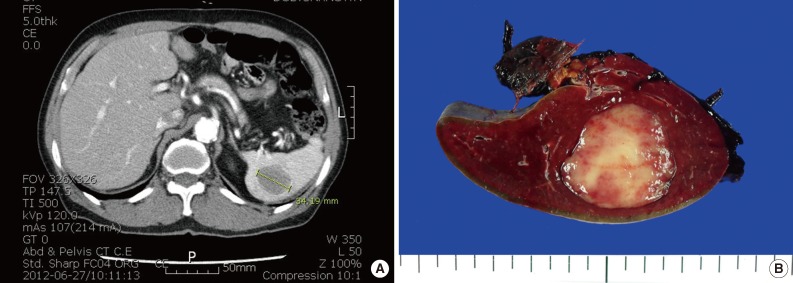
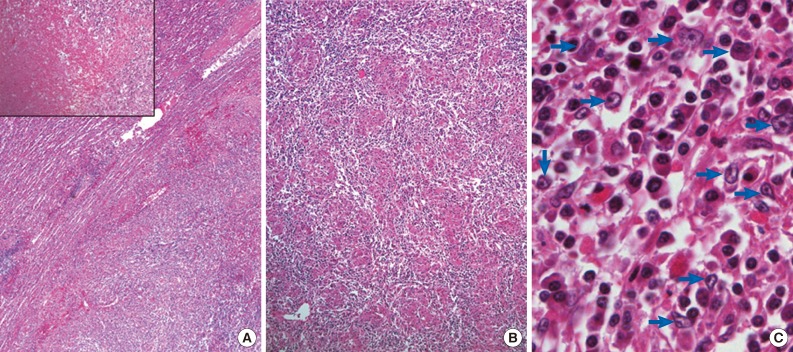
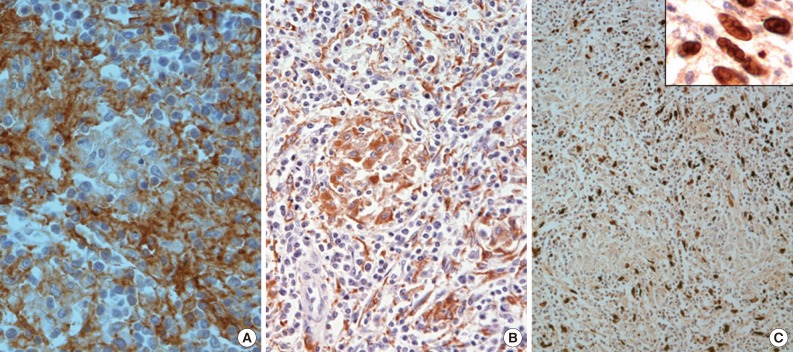
Fig. 1
Fig. 2
Fig. 3
| Case | Age (yr) | Sex | Size (cm) | Symptoms | Treatment | Outcome | |
|---|---|---|---|---|---|---|---|
| Spleen | 1 | 70 | M | 5.5 | Asymptomatic | NA | NA |
| 2 | 58 | F | 22 | Abdominal dullness, easy bruising | Splenectomy | Alive well at 4 mo | |
| 3 | 39 | F | 7.5 | Weight loss, fever | Splenectomy | Alive at 2 mo | |
| 4 | 61 | F | 3.5 | Asymptomatic | Splenectomy | Recent case | |
| 5 | 77 | F | 11 | Epigastralgia | Splenectomy | Alive well (3 yr) | |
| 6 | 64 | F | 5.1 | NA | Splenectomy | Metastasis | |
| 7 |
76 | M | 3.2 | Asymptomatic | Splenectomy | Alive well (7 mo) | |
| Liver | 1 | 68 | F | 11 | Malaise, weight loss | Excision of mass | Alive well (2.5 yr) |
| 2 | 57 | F | 9.5 | Intermittent epigastralgia | No surgery | Enlarged to 15 cm, no metastasis (3 yr) | |
| 3 | 51 | F | 15 | Abdominal fullness, weight loss | Lt. lobectomy | Alive well (1 yr) | |
| 4 | 19 | F | 12 | RUQ abdominal pain, weight loss | Surgical excision | Alive well (40 mo) | |
| 5 | 56 | F | 15 | Gastointestinal upset | Rt. lobectomy | Recur (× 3), alive with disease (56 mo) | |
| 6 | 40 | F | 12.5 | Epigastric pain, weight loss | Lt. hepatectomy | Intra-abdominal recurrence | |
| 7 | 49 | F | 4.2 | Asymptomatic | Surgical excision | Alive well (9 mo) | |
| 8 | 37 | M | 15 | Malaise, weight loss, gross hepatomegaly | Rt. trisegmentectomy | Alive well (42 mo) | |
| 9 | 35 | F | 20 | Epigastric discomfort, fever, weight loss | Rt. hemihepatectomy | Recur (× 3), died for dissemination (95 mo) | |
| 10 | 31 | F | 15 | Abdominal distension, weight loss | Rt. hemihepatectomy | Subtle involvement of porta hepatis LN; alive well (60 mo) | |
| 11 | 49 | F | 9.5 | Abdominal distension (peripancreas) | Whipple’s operation | Recent case |
IPT, inflammatory pseudotumor; FDCT, follicular dendritic cell tumor; M, male; F, female; NA, not accessible; Lt., left; RUQ, right upper quadrant; Rt., right; LN, lymph node. Presenting case.

 E-submission
E-submission





