Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 52(6); 2018 > Article
-
Original Article
Loss of Nuclear BAP1 Expression Is Associated with High WHO/ISUP Grade in Clear Cell Renal Cell Carcinoma -
Young Chan Wi, Ahrim Moon1, Min Jung Jung1, Yeseul Kim, Seong Sik Bang, Kiseok Jang, Seung Sam Paik, Su-Jin Shin

-
Journal of Pathology and Translational Medicine 2018;52(6):378-385.
DOI: https://doi.org/10.4132/jptm.2018.09.21
Published online: October 1, 2018
Department of Pathology, Hanyang University College of Medicine, Seoul, Korea
1Department of Pathology, Soonchunhyang University Bucheon Hospital, Soonchunhyang University College of Medicine, Bucheon, Korea
- Corresponding Author Su-Jin Shin, MD, PhD Department of Pathology, Hanyang University College of Medicine, 222-1 Wangsimni-ro, Seongdong-gu, Seoul 04763, Korea Tel: +82-2-2220-8250 Fax: +82-2-2296-7502 E-mail: charm@hanyang.ac.kr
© 2018 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background
- BRCA1-associated protein 1 (BAP1) mutations are frequently reported in clear cell renal cell carcinoma (ccRCC); however, very few studies have evaluated the role of these mutations in other renal cell carcinoma (RCC) subtypes. Therefore, we analyzed BAP1 protein expression using immunohistochemistry in several RCC subtypes and assessed its relationship with clinicopathological characteristics of patients.
-
Methods
- BAP1 expression was immunohistochemically evaluated in tissue microarray blocks constructed from 371 samples of RCC collected from two medical institutions. BAP1 expression was evaluated based on the extent of nuclear staining in tumor cells, and no expression or expression in < 10% of tumor cells was defined as negative.
-
Results
- Loss of BAP1 expression was observed in ccRCC (56/300, 18.7%), chromophobe RCC (6/26, 23.1%), and clear cell papillary RCC (1/4, 25%), while we failed to detect BAP1 expression loss in papillary RCC, acquired cystic disease-associated RCC, or collecting duct carcinoma. In ccRCC, loss of BAP1 expression was significantly associated with high World Health Organization (WHO)/International Society of Urological Pathology (ISUP) grade (p = .002); however, no significant correlation was observed between loss of BAP1 expression and survival in ccRCC. Loss of BAP1 expression showed no association with prognostic factors in chromophobe RCC.
-
Conclusions
- Loss of BAP1 nuclear expression was observed in both ccRCC and chromophobe RCC. In addition, BAP1 expression loss was associated with poor prognostic factors such as high WHO/ISUP grade in ccRCC.
- Patient selection
- A total of 371 samples were retrospectively obtained from Hanyang University Hospital (247 cases, 2005–2017) and Soonchunhyang University Bucheon Hospital (124 cases, 2001–2013). Formalin-fixed, paraffin-embedded tissue samples obtained from surgically resected primary tumors at the time of initial diagnosis were collected. The pathologist in each institution reviewed the slides and selected a representative block for each case, and 3.0 mm of core tissue microarray (TMA) blocks were constructed, with two representative cores for each case. The patient and tumor characteristics, including age, type of surgery, histological type, histological grade, and follow-up data, were acquired. The histological subtypes were classified according to the 2016 World Health Organization (WHO) Tumor Classification. We graded ccRCC and papillary RCC according to the 2013 WHO/International Society of Urological Pathology (ISUP) grading system [17,18]. Chromophobe RCC was graded according to the published parameters [19]. All cases were reviewed by two pathologists for tumor type and WHO/ISUP grade. This study was approved by the Institutional Review Board of the Hanyang University Hospital (HYUH 2018-05-005), and the requirement for informed consent was waived.
- Immunohistochemistry for BAP1 expression
- Sections from the TMA blocks were immunostained using the Bond-max Automated immunohistochemistry (IHC)/in situ hybridization stainer (Leica Biosystems, Nussloch, Germany) according to the manufacturer’s protocol. Sections (4-μm thickness) were immunostained with a primary antibody against BAP1 (1:100, sc-28383, mouse monoclonal, Santa Cruz Biotechnology, Santa Cruz, CA, USA). BAP1 expression level was evaluated according to the extent of nuclear staining in the tumor cells. The staining was scored as negative (no expression or expression in < 10% of tumor cells) or positive (expression in ≥ 10% of tumor cells).
- Statistical analysis
- All of the statistical analyses were performed using SPSS ver. 24.0 (IBM Corp., Armonk, NY, USA). The relationships between the groups were compared using the chi-square test, Fisher exact test, or Student’s t test. Cancer-specific survival (CSS) was defined as the time interval between the date of surgical resection and the date of death due to RCC. Recurrence-free survival (RFS) was defined as the time interval between surgical resection and the date of any recurrence. The Kaplan-Meier method with the log-rank test and the Cox proportional hazard regression model were used for survival analyses. Two-sided p-values of < .05 were considered to indicate statistically significant differences.
MATERIALS AND METHODS
- Patient characteristics
- The clinicopathological characteristics of the patients are summarized in Table 1. Among 371 RCC cases, the most common subtype was ccRCC (300 cases, 80.9%). The other subtypes included in this study comprised 36 cases of papillary RCC (13 type 1 and 23 type 2 papillary RCC, 9.7%), 26 cases of chromophobe RCC (7.0%), four cases of clear cell papillary RCC, four cases of acquired cystic disease-associated RCC, and one case of collecting duct carcinoma. The age of the patients ranged from 13 to 90 years, with a median of 60 years. The median follow-up period for the patients in this study was 66 months (range, 0.1 to 167.6 months). Of the 371 patients, 11 (3.0%) had metastatic disease at the time of initial diagnosis (i.e., nephrectomy), 30 (8.1%) had experienced metastasis or relapse during the follow-up period, and 34 (9.2%) had died due to RCC by the time of analysis.
- BAP1 expression and tumor type evaluation
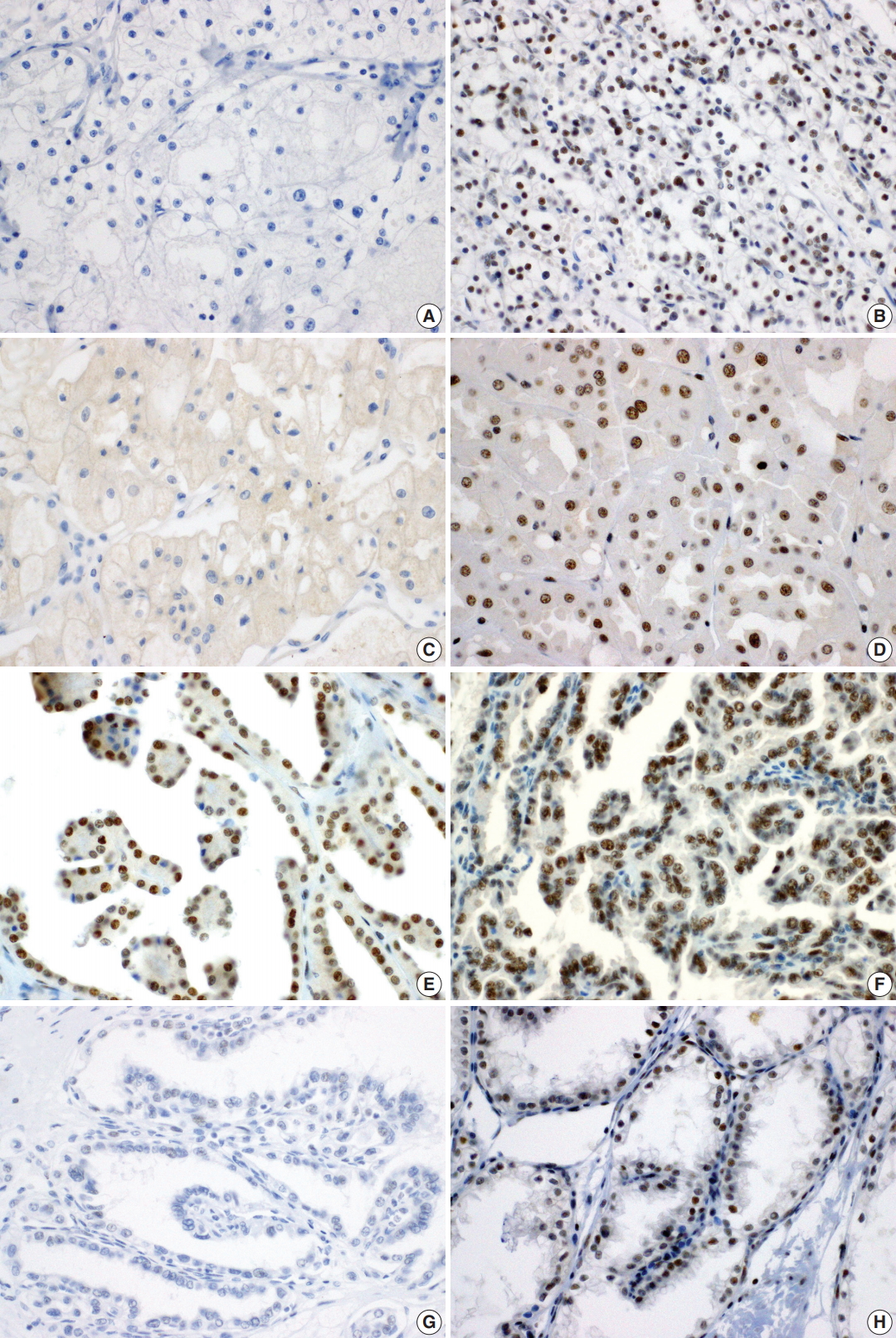
- A total of 371 successfully stained cases with adequate clinical follow-up were classified as either BAP1 negative (n = 63, 17.0%) or BAP1 positive (n = 308, 83.0%). Representative images of BAP1 staining are shown in Fig. 1. Loss of BAP1 expression was frequently observed in ccRCC (18.7%) and chromophobe RCC (23.1%), while we failed to observe BAP1 expression loss in other renal tumor subtypes, including papillary RCC, acquired cystic disease-associated RCC, and collecting duct carcinoma. In clear cell papillary RCC, one case showed loss of BAP1 expression (Table 2).
- BAP1 expression and clinicopathological features of patients with ccRCC and chromophobe RCC
- In ccRCC, loss of BAP1 expression was significantly associated with female sex (p = .046) and high WHO/ISUP grade (p = .002). Furthermore, BAP1 expression loss was more frequent in pT2 than in pT1 category (Table 3). Other clinicopathological parameters such as vascular invasion, tumor necrosis, sarcomatoid feature, and lymph node status showed no significant association with BAP1 expression (Table 3).
- In chromophobe RCC, no significant correlation was observed between BAP1 expression and clinicopathological parameters (Table 3).
- BAP1 expression and survival in ccRCC
- Of 300 patients with ccRCC, 10 (3.3%) had metastatic disease at the time of initial diagnosis (i.e., nephrectomy), 23 (7.7%) had experienced metastasis or relapse during the follow-up period, and 26 (8.7%) had died due to RCC by the time of analysis.
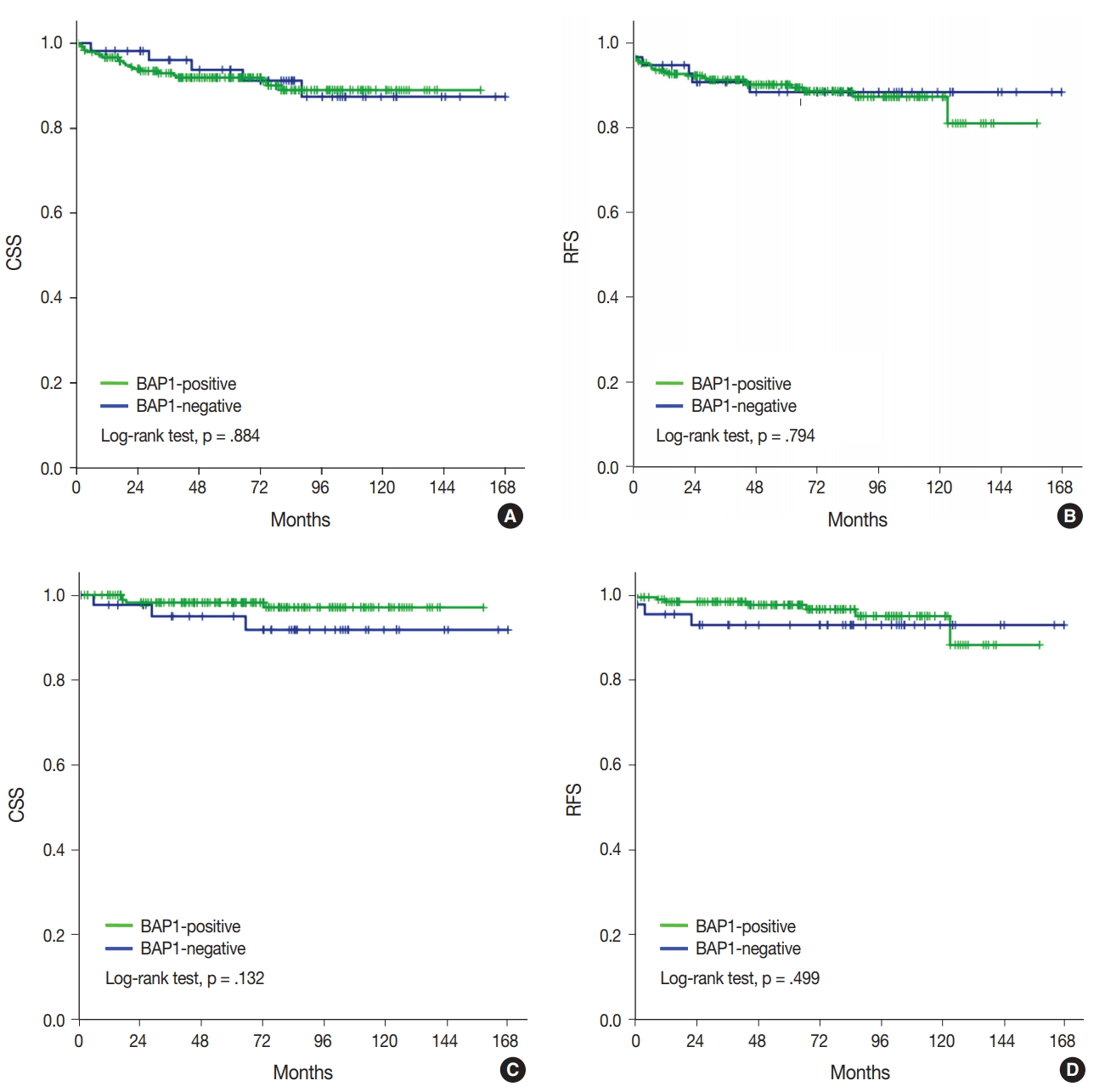
- Kaplan-Meier analysis and Cox regression analysis were applied to evaluate the prognostic value of BAP1 loss. Univariate analysis revealed that high WHO/ISUP grade, vascular invasion, tumor necrosis, sarcomatoid feature, high pT category, and lymph node metastasis predicted a poor outcome in ccRCC (Table 4). However, BAP1 expression showed no association with CSS and RFS (Fig. 2A, B). Even in cases with low pT (pT1/2) ccRCC, loss of BAP1 expression showed no statistically significant correlation with CSS and RFS (Fig. 2C, D).
RESULTS
- In this study, we demonstrated the loss of BAP1 nuclear expression in chromophobe RCC and clear cell papillary RCC as well as ccRCC. Furthermore, the loss of BAP1 nuclear expression was associated with adverse clinicopathological features such as high WHO/ISUP grade in ccRCC but showed no relationship with CSS or RFS in patients with ccRCC.
- The Cancer Genome Atlas (TCGA) research network recently reported the molecular characterization of RCC and included 488 ccRCC, 160 papillary type 1 RCC, 70 papillary type 2 RCC, and 81 chromophobe RCC. BAP1 mutation, a chromatin remodeling gene mutation, was reported in ccRCC (11.0%) and papillary RCC (5.6%) but not in chromophobe RCC [20]. BAP1 mutation was also shown to be correlated with decreased survival in ccRCC [20].
- The ratio of BAP1 loss in the present study (18.7%) was similar to that reported in previous studies [21,22]. We also found that the loss of BAP1 expression was significantly common in female sex (p = .046). BAP1 mutation was more frequent in female patients as per TCGA data [20,23]. We observed that BAP1 nuclear expression loss was associated with high WHO/ISUP grade in ccRCC and showed no correlation with CSS and RFS. In several studies, loss of BAP1 expression served as an independent marker of prognosis in patients with ccRCC and low-grade ccRCC [24,25]. On the other hand, in other studies, no significant association was reported between BAP1 loss and CSS or RFS, although BAP1 loss significantly correlated with poor clinicopathological parameters [16,21]. Differences in the prognostic associations may be related to differences in cohorts among studies. Our cohort had relatively low-grade RCC and a short follow-up period; therefore, overall cancer-specific death rate was lower than that recorded in the previous TGCA report (8% vs 33%) [20].
- Among non-ccRCC, papillary RCC, chromophobe RCC, clear cell papillary RCC, acquired cystic disease-associated RCC, and collecting duct carcinoma were evaluated for BAP1 expression. We observed the loss of BAP1 expression in 23.1% of chromophobe RCC (6/26) cases and in one clear cell papillary RCC case. No significant association was detected between BAP1 expression and adverse clinicopathological parameters in chromophobe RCC. Unfortunately, the number of patients with chromophobe RCC and clear cell papillary RCC was too small to evaluate proper clinical relevance. In addition, during the follow-up period, one patient died due to chromophobe RCC; therefore, survival analysis could not be performed. An additional analysis is needed to further elucidate the role of BAP1 and the relationship between loss of BAP1 expression in IHC and BAP1 mutation in chromophobe RCC and clear cell papillary RCC.
- In conclusion, we revealed that BAP1 expression is associated with high WHO/ISUP grade in patients with ccRCC and that BAP1 expression loss is also observed in chromophobe RCC and clear cell papillary RCC. Further studies are needed to assess larger cohorts and associated pathological features.
DISCUSSION
Acknowledgments
| Characteristic | Value (n = 371) |
|---|---|
| Tumor type | |
| Clear cell RCC | 300 (80.9) |
| Chromophobe RCC | 26 (7.0) |
| Papillary RCC, type 1 | 13 (3.5) |
| Papillary RCC, type 2 | 23 (6.2) |
| Others | 9 (2.4) |
| Age (yr) | 60.0 (13–90) |
| Sex | |
| Male | 246 (66.3) |
| Female | 125 (33.7) |
| Tumor size | 3.77 (0.7–15) |
| WHO/ISUP grade (clear and papillary RCC) | |
| 1 | 33 (9.8) |
| 2 | 160 (47.6) |
| 3 | 113 (33.6) |
| 4 | 30 (8.9) |
| Chromophobe grade (chromophobe RCC) | |
| 1 | 19 (73.1) |
| 2 | 7 (26.9) |
| Vascular invasiona | |
| Absent | 323 (87.1) |
| Present | 48 (12.9) |
| Tumor necrosis | |
| Absent | 219 (84.2) |
| Present | 41 (15.8) |
| Sarcomatoid feature | |
| Absent | 350 (94.3) |
| Present | 21 (5.7) |
| Lymph node metastasis | |
| Absent | 362 (97.6) |
| Present | 9 (2.4) |
| pT category | |
| 1 | 258 (69.5) |
| 2 | 36 (9.7) |
| 3 | 74 (19.9) |
| 4 | 3 (0.8) |
|
Clear cell RCC (n = 300) |
Chromophobe RCC (n = 26) |
|||||
|---|---|---|---|---|---|---|
| Negative (n = 56) | Positive (n = 244) | p-value | Negative (n = 6) | Positive (n = 20) | p-value | |
| Sex | .046 | .664 | ||||
| Male | 32 (15.6) | 173 (84.4) | 3 (27.3) | 8 (72.7) | ||
| Female | 24 (25.3) | 71 (74.7) | 3 (20.0) | 12 (80.0) | ||
| WHO/ISUP grade | .002 | |||||
| 1 | 0 | 25 (100) | ||||
| 2 | 20 (14.1) | 122 (85.9) | ||||
| 3 | 27 (25.7) | 78 (74.3) | ||||
| 4 | 9 (32.1) | 19 (67.9) | ||||
| Chromophobe grade | .146 | |||||
| 1 | 6 (31.6) | 13 (68.4) | ||||
| 2 | 0 | 7 (100) | ||||
| Vascular invasion | .664 | .231 | ||||
| Absent | 49 (19.1) | 203 (80.9) | 5 (20.0) | 20 (80.0) | ||
| Present | 7 (16.3) | 36 (83.7) | 1 (100) | 0 | ||
| Tumor necrosis | .437 | |||||
| Absent | 28 (16.8) | 139 (83.2) | 6 (23.1) | 20 (76.9) | ||
| Present | 8 (22.2) | 28 (77.7) | ||||
| Sarcomatoid feature | .346 | |||||
| Absent | 51 (18.1) | 231 (81.9) | 6 (23.1) | 20 (76.9) | ||
| Present | 5 (27.8) | 13 (72.2) | ||||
| pT categorya | .037 | .606 | ||||
| pT1 | 35 (16.9) | 172 (83.1) | 3 (18.8) | 13 (81.3) | ||
| pT2 | 10 (37.0) | 17 (63.0) | 2 (40.0) | 3 (60.0) | ||
| pT3/4 | 11 (16.7) | 55 (83.3) | 1 (20.0) | 4 (80.0) | ||
| pN categorya | .899 | > .999 | ||||
| pN0 | 55 (18.7) | 239 (81.3) | 6 (24.0) | 19 (76.0) | ||
| pN1 | 1 (16.7) | 5 (83.3) | 0 | 1 (100) | ||
- 1. Rini BI, Campbell SC, Escudier B. Renal cell carcinoma. Lancet 2009; 373: 1119-32. ArticlePubMed
- 2. Dalgliesh GL, Furge K, Greenman C, et al. Systematic sequencing of renal carcinoma reveals inactivation of histone modifying genes. Nature 2010; 463: 360-3. ArticlePubMedPMCPDF
- 3. Guo G, Gui Y, Gao S, et al. Frequent mutations of genes encoding ubiquitin-mediated proteolysis pathway components in clear cell renal cell carcinoma. Nat Genet 2011; 44: 17-9. ArticlePubMedPDF
- 4. Varela I, Tarpey P, Raine K, et al. Exome sequencing identifies frequent mutation of the SWI/SNF complex gene PBRM1 in renal carcinoma. Nature 2011; 469: 539-42. PubMedPMC
- 5. Hakimi AA, Ostrovnaya I, Reva B, et al. Adverse outcomes in clear cell renal cell carcinoma with mutations of 3p21 epigenetic regulators BAP1 and SETD2: a report by MSKCC and the KIRC TCGA research network. Clin Cancer Res 2013; 19: 3259-67. ArticlePubMedPMCPDF
- 6. Peña-Llopis S, Vega-Rubín-de-Celis S, Liao A, et al. BAP1 loss defines a new class of renal cell carcinoma. Nat Genet 2012; 44: 751-9. ArticlePubMedPMCPDF
- 7. White AE, Harper JW. Cancer: emerging anatomy of the BAP1 tumor suppressor system. Science 2012; 337: 1463-4. ArticlePubMed
- 8. Bhattacharya S, Hanpude P, Maiti TK. Cancer associated missense mutations in BAP1 catalytic domain induce amyloidogenic aggregation: a new insight in enzymatic inactivation. Sci Rep 2015; 5: 18462.ArticlePubMedPMCPDF
- 9. Murali R, Wiesner T, Scolyer RA. Tumours associated with BAP1 mutations. Pathology 2013; 45: 116-26. ArticlePubMed
- 10. Rai K, Pilarski R, Cebulla CM, Abdel-Rahman MH. Comprehensive review of BAP1 tumor predisposition syndrome with report of two new cases. Clin Genet 2016; 89: 285-94. PubMed
- 11. Harbour JW, Onken MD, Roberson ED, et al. Frequent mutation of BAP1 in metastasizing uveal melanomas. Science 2010; 330: 1410-3. ArticlePubMedPMC
- 12. Bott M, Brevet M, Taylor BS, et al. The nuclear deubiquitinase BAP1 is commonly inactivated by somatic mutations and 3p21.1 losses in malignant pleural mesothelioma. Nat Genet 2011; 43: 668-72. ArticlePubMedPMCPDF
- 13. Andrici J, Sheen A, Sioson L, et al. Loss of expression of BAP1 is a useful adjunct, which strongly supports the diagnosis of mesothelioma in effusion cytology. Mod Pathol 2015; 28: 1360-8. ArticlePubMedPMCPDF
- 14. Koopmans AE, Verdijk RM, Brouwer RW, et al. Clinical significance of immunohistochemistry for detection of BAP1 mutations in uveal melanoma. Mod Pathol 2014; 27: 1321-30. ArticlePubMedPDF
- 15. Oka S, Inoshita N, Miura Y, et al. The loss of BAP1 protein expression predicts poor prognosis in patients with nonmetastatic clear cell renal cell carcinoma with inferior vena cava tumor thrombosis. Urol Oncol 2018; 36: 365e9-e14. Article
- 16. Minardi D, Lucarini G, Milanese G, Montironi R, Di Primio R. Prognostic role of BAP1 in pT1 clear cell carcinoma in partial nephrectomy specimens. Virchows Arch 2017; 471: 99-105. ArticlePubMedPDF
- 17. Eble JN, Sauter G, Epstein JI, Sesterhenn IA. World Health Organization classification of tumors: pathology and genetics of tumours of the urinary system and male genital organs. Lyon: IARC Press, 2016.
- 18. Delahunt B, Cheville JC, Martignoni G, et al. The International Society of Urological Pathology (ISUP) grading system for renal cell carcinoma and other prognostic parameters. Am J Surg Pathol 2013; 37: 1490-504. ArticlePubMed
- 19. Paner GP, Amin MB, Alvarado-Cabrero I, et al. A novel tumor grading scheme for chromophobe renal cell carcinoma: prognostic utility and comparison with Fuhrman nuclear grade. Am J Surg Pathol 2010; 34: 1233-40. PubMed
- 20. Ricketts CJ, De Cubas AA, Fan H, et al. The Cancer Genome Atlas comprehensive molecular characterization of renal cell carcinoma. Cell Rep 2018; 23: 3698.
- 21. Kim SH, Park WS, Park EY, et al. The prognostic value of BAP1, PBRM1, pS6, PTEN, TGase2, PD-L1, CA9, PSMA, and Ki-67 tissue markers in localized renal cell carcinoma: a retrospective study of tissue microarrays using immunohistochemistry. PLoS One 2017; 12: e0179610. ArticlePubMedPMC
- 22. da Costa WH, da Cunha IW, Fares AF, et al. Prognostic impact of concomitant loss of PBRM1 and BAP1 protein expression in early stages of clear cell renal cell carcinoma. Urol Oncol 2018; 36: 243e1-e8.
- 23. Ricketts CJ, Linehan WM. Gender specific mutation incidence and survival associations in clear cell renal cell carcinoma (CCRCC). PLoS One 2015; 10: e0140257. ArticlePubMedPMC
- 24. Joseph RW, Kapur P, Serie DJ, et al. Loss of BAP1 protein expression is an independent marker of poor prognosis in patients with low-risk clear cell renal cell carcinoma. Cancer 2014; 120: 1059-67. ArticlePubMed
- 25. Kapur P, Christie A, Raman JD, et al. BAP1 immunohistochemistry predicts outcomes in a multi-institutional cohort with clear cell renal cell carcinoma. J Urol 2014; 191: 603-10. ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- The Role of Homologous Recombination Deficiency (HRD) in Renal Cell Carcinoma (RCC): Biology, Biomarkers, and Therapeutic Opportunities
Alberto Bongiovanni, Pierfranco Conte, Vincenza Conteduca, Matteo Landriscina, Giuseppe Di Lorenzo, Francesco Cognetti
Current Oncology.2025; 32(12): 690. CrossRef - Clinical and Genomic Features of Patients with Renal Cell Carcinoma and Advanced Chronic Kidney Disease: Analysis of a Multi-Institutional Database
Corbin J. Eule, Junxiao Hu, Dale Hedges, Alkesh Jani, Thomas Pshak, Brandon J. Manley, Alejandro Sanchez, Robert Dreicer, Zin W. Myint, Yousef Zakharia, Elaine T. Lam
Cancers.2024; 16(10): 1920. CrossRef - Immune regulation and prognosis indicating ability of a newly constructed multi-genes containing signature in clear cell renal cell carcinoma
Ziwei Gui, Juan Du, Nan Wu, Ningning Shen, Zhiqing Yang, Huijun Yang, Xuzhi Wang, Na Zhao, Zixin Zeng, Rong Wei, Wenxia Ma, Chen Wang
BMC Cancer.2023;[Epub] CrossRef - Radiogenomic Associations Clear Cell Renal Cell Carcinoma: An Exploratory Study
Derek H Liu, Komal A Dani, Sharath S Reddy, Xiaomeng Lei, Natalie L Demirjian, Darryl H Hwang, Bino A Varghese, Suhn Kyong Rhie, Felix Y. Yap, David I. Quinn, Imran Siddiqi, Manju Aron, Ulka Vaishampayan, Haris Zahoor, Steven Y Cen, Inderbir S Gill, Vinay
Oncology.2023; 101(6): 375. CrossRef - Immunohistochemistry for the diagnosis of renal epithelial neoplasms
Mahmut Akgul, Sean R Williamson
Seminars in Diagnostic Pathology.2022; 39(1): 1. CrossRef - BRCA1-Associated Protein 1 (BAP-1) as a Prognostic and Predictive Biomarker in Clear Cell Renal Cell Carcinoma: A Systematic Review
Shuchi Gulati, Melissa Previtera, Primo N. Lara
Kidney Cancer.2022; 6(1): 23. CrossRef - Renal Cell Carcinoma in End-Stage Renal Disease: A Review and Update
Ziad M. El-Zaatari, Luan D. Truong
Biomedicines.2022; 10(3): 657. CrossRef - CD117, BAP1, MTAP, and TdT Is a Useful Immunohistochemical Panel to Distinguish Thymoma from Thymic Carcinoma
Mounika Angirekula, Sindy Y Chang, Sarah M. Jenkins, Patricia T. Greipp, William R. Sukov, Randolph S. Marks, Kenneth R. Olivier, Stephen D. Cassivi, Anja C Roden
Cancers.2022; 14(9): 2299. CrossRef - BAP1 in cancer: epigenetic stability and genome integrity
Sabrina Caporali, Alessio Butera, Ivano Amelio
Discover Oncology.2022;[Epub] CrossRef - Bioinformatic analysis identifying FGF1 gene as a new prognostic indicator in clear cell Renal Cell Carcinoma
Xiaoqin Zhang, Ziyue Wang, Zixin Zeng, Ningning Shen, Bin Wang, Yaping Zhang, Honghong Shen, Wei Lu, Rong Wei, Wenxia Ma, Chen Wang
Cancer Cell International.2021;[Epub] CrossRef - Identification of Four Pathological Stage‐Relevant Genes in Association with Progression and Prognosis in Clear Cell Renal Cell Carcinoma by Integrated Bioinformatics Analysis
Dengyong Xu, Yuzi Xu, Yiming Lv, Fei Wu, Yunlong Liu, Ming Zhu, Dake Chen, Bingjun Bai, Rui Liu
BioMed Research International.2020;[Epub] CrossRef - Functional characterisation guides classification of novel BAP1 germline variants
Jing Han Hong, Siao Ting Chong, Po-Hsien Lee, Jing Tan, Hong Lee Heng, Nur Diana Binte Ishak, Sock Hoai Chan, Bin Tean Teh, Joanne Ngeow
npj Genomic Medicine.2020;[Epub] CrossRef - Tissue-Based Immunohistochemical Markers for Diagnosis and Classification of Renal Cell Carcinoma
Liang G Qu, Vaisnavi Thirugnanasundralingam, Damien Bolton, Antonio Finelli, Nathan Lawrentschuk
Société Internationale d’Urologie Journal.2020; 1(1): 68. CrossRef - Radiogenomics: bridging imaging and genomics
Zuhir Bodalal, Stefano Trebeschi, Thi Dan Linh Nguyen-Kim, Winnie Schats, Regina Beets-Tan
Abdominal Radiology.2019; 44(6): 1960. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
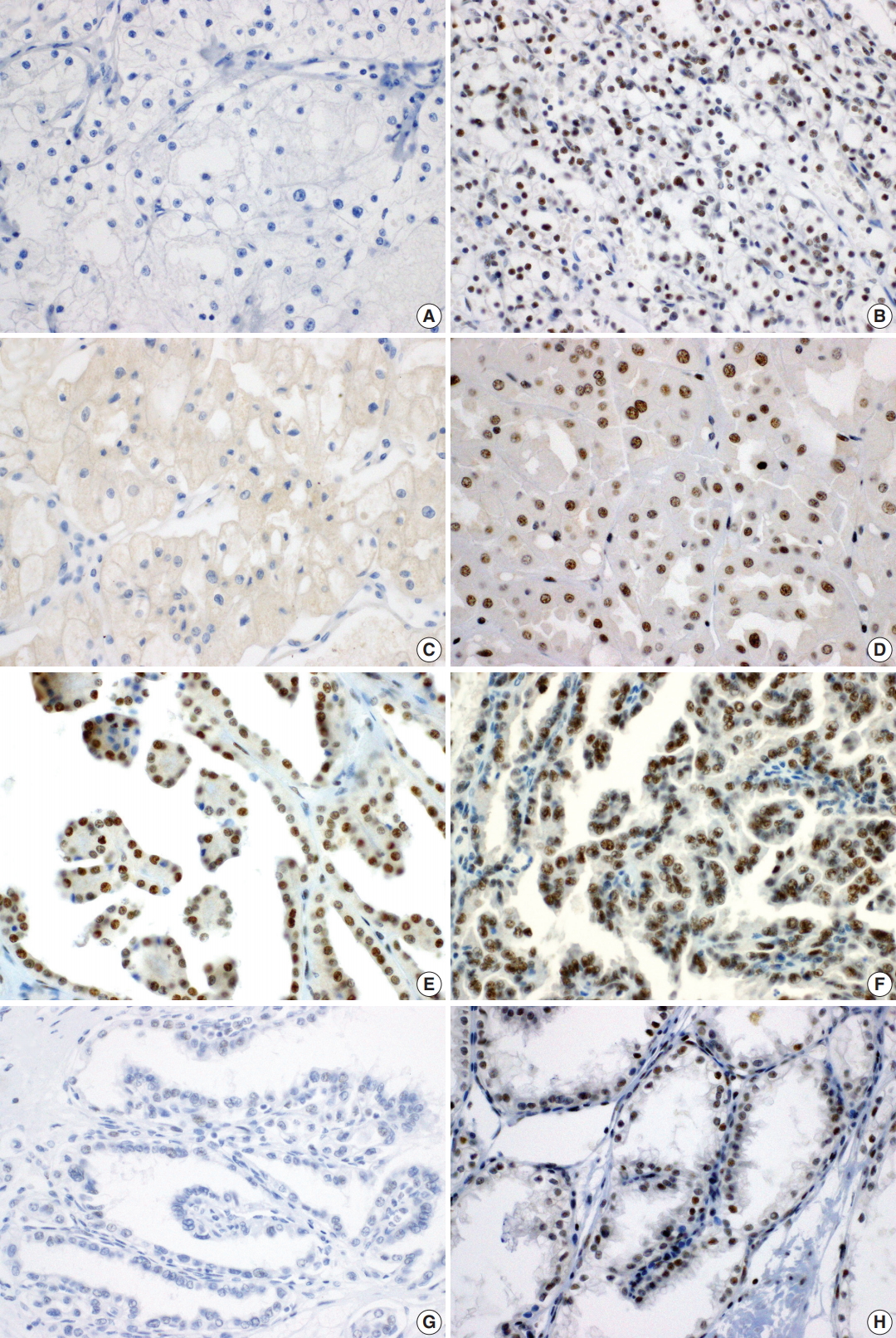
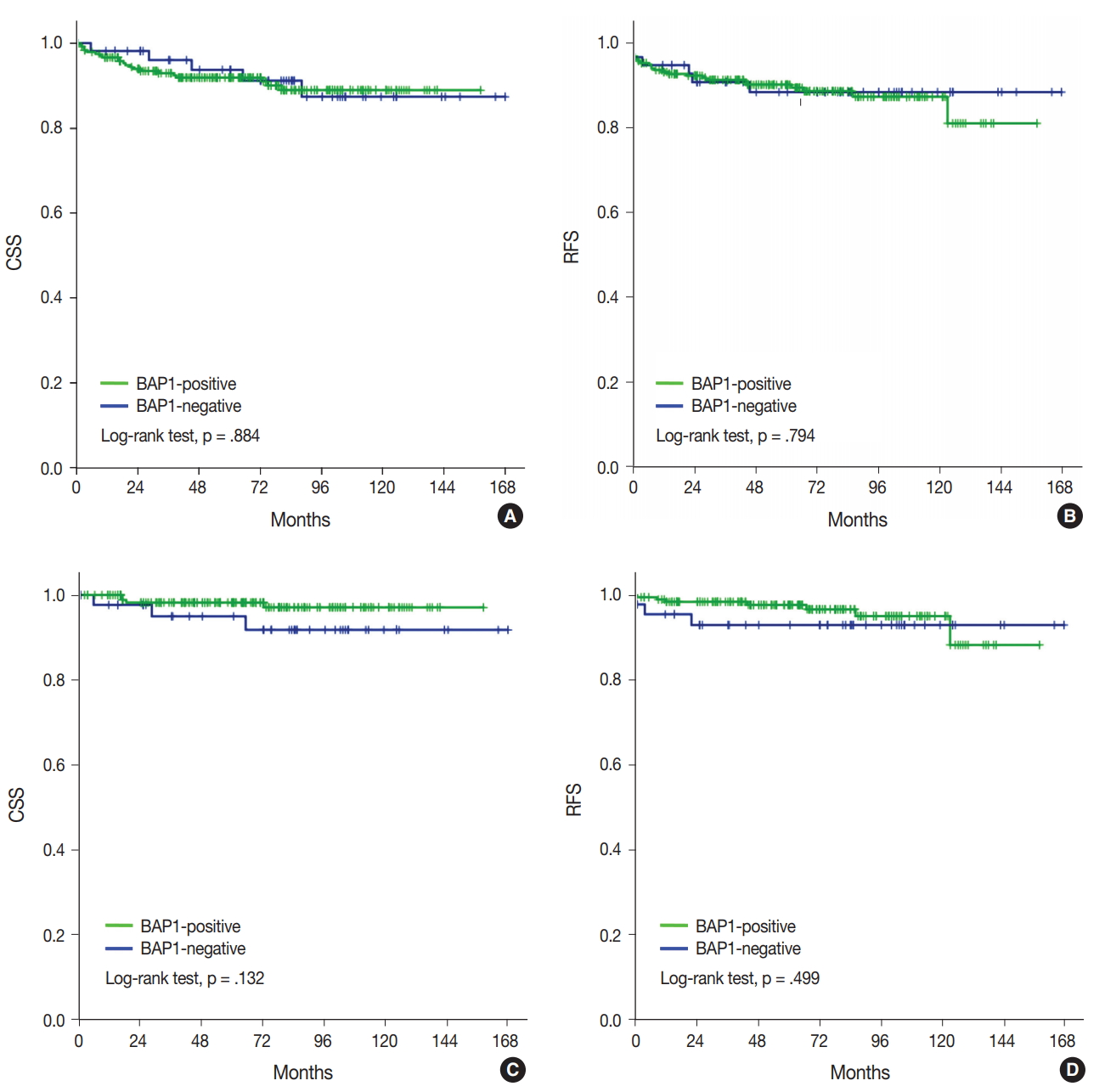
Fig. 1.
Fig. 2.
| Characteristic | Value (n = 371) |
|---|---|
| Tumor type | |
| Clear cell RCC | 300 (80.9) |
| Chromophobe RCC | 26 (7.0) |
| Papillary RCC, type 1 | 13 (3.5) |
| Papillary RCC, type 2 | 23 (6.2) |
| Others | 9 (2.4) |
| Age (yr) | 60.0 (13–90) |
| Sex | |
| Male | 246 (66.3) |
| Female | 125 (33.7) |
| Tumor size | 3.77 (0.7–15) |
| WHO/ISUP grade (clear and papillary RCC) | |
| 1 | 33 (9.8) |
| 2 | 160 (47.6) |
| 3 | 113 (33.6) |
| 4 | 30 (8.9) |
| Chromophobe grade (chromophobe RCC) | |
| 1 | 19 (73.1) |
| 2 | 7 (26.9) |
| Vascular invasion |
|
| Absent | 323 (87.1) |
| Present | 48 (12.9) |
| Tumor necrosis | |
| Absent | 219 (84.2) |
| Present | 41 (15.8) |
| Sarcomatoid feature | |
| Absent | 350 (94.3) |
| Present | 21 (5.7) |
| Lymph node metastasis | |
| Absent | 362 (97.6) |
| Present | 9 (2.4) |
| pT category | |
| 1 | 258 (69.5) |
| 2 | 36 (9.7) |
| 3 | 74 (19.9) |
| 4 | 3 (0.8) |
| Negative (n = 63) | Positive (n = 308) | |
|---|---|---|
| Clear cell RCC | 56 (18.7) | 244 (81.3) |
| Chromophobe RCC | 6 (23.1) | 20 (76.9) |
| Papillary RCC type 1 | 0 | 13 (100) |
| Papillary RCC type 2 | 0 | 23 (100) |
| Clear cell papillary RCC | 1 (25) | 3 (75) |
| Acquired cystic disease-associated RCC | 0 | 4 (100) |
| Collecting duct carcinoma | 0 | 1 (100) |
| Clear cell RCC (n = 300) |
Chromophobe RCC (n = 26) |
|||||
|---|---|---|---|---|---|---|
| Negative (n = 56) | Positive (n = 244) | p-value | Negative (n = 6) | Positive (n = 20) | p-value | |
| Sex | .046 | .664 | ||||
| Male | 32 (15.6) | 173 (84.4) | 3 (27.3) | 8 (72.7) | ||
| Female | 24 (25.3) | 71 (74.7) | 3 (20.0) | 12 (80.0) | ||
| WHO/ISUP grade | .002 | |||||
| 1 | 0 | 25 (100) | ||||
| 2 | 20 (14.1) | 122 (85.9) | ||||
| 3 | 27 (25.7) | 78 (74.3) | ||||
| 4 | 9 (32.1) | 19 (67.9) | ||||
| Chromophobe grade | .146 | |||||
| 1 | 6 (31.6) | 13 (68.4) | ||||
| 2 | 0 | 7 (100) | ||||
| Vascular invasion | .664 | .231 | ||||
| Absent | 49 (19.1) | 203 (80.9) | 5 (20.0) | 20 (80.0) | ||
| Present | 7 (16.3) | 36 (83.7) | 1 (100) | 0 | ||
| Tumor necrosis | .437 | |||||
| Absent | 28 (16.8) | 139 (83.2) | 6 (23.1) | 20 (76.9) | ||
| Present | 8 (22.2) | 28 (77.7) | ||||
| Sarcomatoid feature | .346 | |||||
| Absent | 51 (18.1) | 231 (81.9) | 6 (23.1) | 20 (76.9) | ||
| Present | 5 (27.8) | 13 (72.2) | ||||
| pT category |
.037 | .606 | ||||
| pT1 | 35 (16.9) | 172 (83.1) | 3 (18.8) | 13 (81.3) | ||
| pT2 | 10 (37.0) | 17 (63.0) | 2 (40.0) | 3 (60.0) | ||
| pT3/4 | 11 (16.7) | 55 (83.3) | 1 (20.0) | 4 (80.0) | ||
| pN category |
.899 | > .999 | ||||
| pN0 | 55 (18.7) | 239 (81.3) | 6 (24.0) | 19 (76.0) | ||
| pN1 | 1 (16.7) | 5 (83.3) | 0 | 1 (100) | ||
| Variable | Cancer-specific survival |
Recurrence-free survival |
||||
|---|---|---|---|---|---|---|
| HR | 95% CI | p-value | HR | 95% CI | p-value | |
| BAP1 | ||||||
| Positive vs negative | 1.076 | 0.405–2.859 | .884 | 1.125 | 0.462–2.740 | .795 |
| Sex | ||||||
| Female vs male | 2.140 | 0.807–5.676 | .118 | 1.879 | 0.814–4.334 | .139 |
| WHO/ISUP grade | ||||||
| 1–2 | 1 | 1 | ||||
| 3 | 3.401 | 1.138–10.165 | .028 | 2.484 | 0.997–6.185 | .051 |
| 4 | 20.883 | 7.323–59.550 | < .001 | 16.202 | 6.749–38.890 | < .001 |
| Vascular invasion | ||||||
| Absent vs present | 9.386 | 4.306–20.460 | < .001 | 8.219 | 4.130–16.355 | < .001 |
| Tumor necrosis | ||||||
| Absent vs present | 18.216 | 5.713–58.079 | < .001 | 16.980 | 5.953–48.428 | < .001 |
| Sarcomatoid feature | ||||||
| Absent vs present | 13.933 | 6.283–30.896 | < .001 | 10.823 | 5.103–22.957 | < .001 |
| pT category | ||||||
| pT1 | 1 | 1 | ||||
| pT2 | 6.298 | 1.409–28.145 | .016 | 8.249 | 2.387–28.509 | .001 |
| pT3 and pT4 | 18.200 | 6.185–53.557 | < .001 | 18.733 | 7.103–49.404 | < .001 |
| Lymph node metastasis | ||||||
| Absent vs present | 32.885 | 10.417–103.815 | < .001 | 18.940 | 6.203–57.828 | < .001 |
Values are presented as number (%) or median (range). RCC, renal cell carcinoma; WHO, World Health Organization; ISUP, International Society of Urological Pathology. Vascular invasion includes microscopic tumor invasion into small or large vessels and gross renal vein tumor thrombus.
Values are presented as number (%). BAP1, BRCA1-associated protein 1; RCC, renal cell carcinoma.
Values are presented as number (%). BAP1, BRCA1-associated protein 1; RCC, renal cell carcinoma; WHO, World Health Organization; ISUP, International Society of Urological Pathology. AJCC eighth edition.
RCC, renal cell carcinoma; HR, hazard ratio; CI, confidence interval; BAP1, BRCA1-associated protein 1; WHO, World Health Organization; ISUP, International Society of Urological Pathology.

 E-submission
E-submission




