Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 49(2); 2015 > Article
-
Brief Case Report
Unicystic Granulosa Cell Tumor - Nalli R. Sumitra Devi, Sathya Lakshmi Ramu, Arun Prabhakaran, Deepa Devi Govindaswamy
-
Journal of Pathology and Translational Medicine 2015;49(2):167-170.
DOI: https://doi.org/10.4132/jptm.2014.04.02
Published online: March 12, 2015
Department of Pathology, Stanley Medical College, Chennai, Tamil Nadu, India
- Corresponding Author: Nalli R. Sumitra Devi, M.D. Stanley Medical College, 5E, Old Tower Block, Nandanam Extension, Chennai 600035, Tamil Nadu, India Tel: +91-9445001778, E-mail: drnallisumitra@yahoo.co.in
• Received: January 24, 2014 • Revised: March 22, 2014 • Accepted: April 2, 2014
© 2015 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 11,459 Views
- 73 Download
- 1 Scopus
- A 57-year-old woman presented with lower abdominal pain and abdominal distention for 3 months duration. The patient reached menopause 10 years prior. She had no symptoms or signs of hyperestrinisim or virilization. Abdominal examination revealed a mass consistent with 20 weeks of pregnancy extending to the umbilicus. On palpation, the mass was mobile and cystic. Ultrasound examination showed a mixed echogenic mass measuring 13×8.8 cm, which arised from the left side of the pelvis (Fig. 1A). A computed tomography (CT) scan revealed a large cystic space occupying lesion with thick septa measuring 18.5×11.9×14.4 cm arising from the pelvis (Fig. 1B). A possible diagnosis of a mucinous cyst adenoma/carcinoma was made. Lab investigations were within normal limits with cancer antigen 125 levels being 5–12 U/mL (normal value, 0 to 35 U/mL). The patient underwent a total abdominal hysterectomy with bilateral salphingo-oopherectomy. Grossly, the left ovarian cyst measured 20×14×10 cm. The external surface of the cyst was smooth with prominent vasculature and the cut surface revealed a unilocular and thin-walled cyst filled with 500 mL of hemorrhagic fluid. The inner surface was smooth with tiny focal papillary projections (Fig. 2). Histomorphology revealed a unicystic lesion lined by multi-layered granulosa cells with interspersed Call-Exner bodies (Fig. 3A, B). The neoplastic cells were round to polygonal with moderate to scant cytoplasm and round to oval nuclei with some showing prominent grooving (Fig. 3C). The immunohistochemical markers, inhibin and vimentin, were positive (Fig. 3D, E). A final diagnosis of unicystic granulosa cell tumor was made.
CASE REPORT
- Sex cord stromal tumors comprise approximately 8% of primary ovarian neoplasms, and among these tumors, the granulosa cell tumor is the most common and accounts for approximately 1.5% of primary ovarian tumors. Granulosa cell tumors were first described by Rokitansky in the year 1859 [4]. Histogenesis of sex cord stromal tumors is uncertain; however, at present, the origin is considered to be coelomic epithelium or gonadal sex cord [2] There are two well-defined patterns of granulosa cell tumor, the common adult granulosa cell tumor and the less frequent juvenile type, which are based on clinical and histopathological features. The adult granulosa cell tumor accounts for 95% of all ovarian tumors, and most commonly presents in the peri or postmenopausal period with a peak incidence between 50–54 years [5].
- The usual presentation of these tumors are symptoms associated with hyperestrinism leading to isosexual pseudoprecocity in children and metrorrhagia in adults. A large number of androgenic granulosa cell tumors present as unilocular or multilocular cysts [6]. The association with androgen production and the formation of unilocular cystic type of granulosa cell tumor remains an enigma [7]. Sonographically and based on CT images, five morphological patterns were categorized including multilocular cystic, thick-walled unilocular cystic, thin-walled unilocular cystic, homogenously solid, and heterogeneously solid masses.
- Grossly, granulosa cell tumors are usually unilateral and encapsulated with a smooth lobulated outline and predominantly solid or solid and cystic with a yellow to white cut surface. Cystic degeneration and hemorrhage are common. Occasionally, the tumors may resemble a thin-walled unilocular or multilocular cystadenoma [2].
- The histomorphology of adult granulosa cell tumors includes well-differentiated and less well-differentiated types. The well-differentiated group is composed of microfollicular, macrofollicular, trabecular, and insular patterns with the microfollicular pattern being the most common of all subtypes and contains Call-Exner bodies. Diffuse and watered silk or gyriform patterns fall under the less well differentiated group. Sclerotic stroma is a secondary degenerative change commonly seen in granulosa cell tumors, which most likely arises due to ischemia [7,8]. Differential diagnosis for granulosa cell tumors include low-grade stromal sarcomas, small cell carcinomas, and carcinoid tumors on low power magnification. These tumors lack nuclear grooving, are more hyperchromatic, and often contain more mitotic figures than typical granulosa cell tumors. The nuclear appearance, mitotic rate, and presence of Call-Exner bodies have a diagnostic value in differentiating granulosa cell tumors from other malignant tumors.
- Elevated levels of alpha inhibin and/or Müllerian-inhibiting substance (MIS) or anti-Müllerian hormone are useful and specific markers for early diagnosis and follow-up of granulosa cell tumors. This case was positive for alpha inhibin and vimentin. Therefore, the diagnosis of unilocular cystic granulosa cell tumors is based on the histological examination with a monotonous population of round to oval cells with Call-Exner bodies, nuclear grooves, low mitotic activity, infrequent diagnostic serum markers, and immunohistochemical profile. The spectrum of differentiation correlates poorly with the clinical outcomes and all granulosa cell tumors are considered low grade malignancies. Granulosa cell tumors are slow growing tumors, and late recurrence is a common feature. Clinicopathologic prognostic markers include the tumor stage as well as tumor size and rupture, of which staging is the most important prognostic factor [9]. The 5-year survival rate for stage 1 disease ranges from 75% –95%. Presence of tumors greater than 10–15 cm in diameter carries a poor prognosis independent of stage. A mitotic index of more than or equal to 10 mitotic figures per high power field (×10) has a poor prognosis. Other histopathological variables used to determine prognosis include p53 status, histological pattern, disease stage, mitotic index, and lymphovascular invasion. Of these factors, mitotic index and lymphovascular invasion were the most important and are independent factors that determine prognosis [10]. Life-long follow-up with clinical examinations and measurement of tumor markers such as inhibin B are recommended.
DISCUSSION
Fig. 1.(A) Mixed echogenic mass measuring 13×8.8 cm arising from the left side of the pelvis. (B) Large cystic space-occupying lesion with thick septa measuring 18.5×11.9×14.4 cm arising from the pelvis.
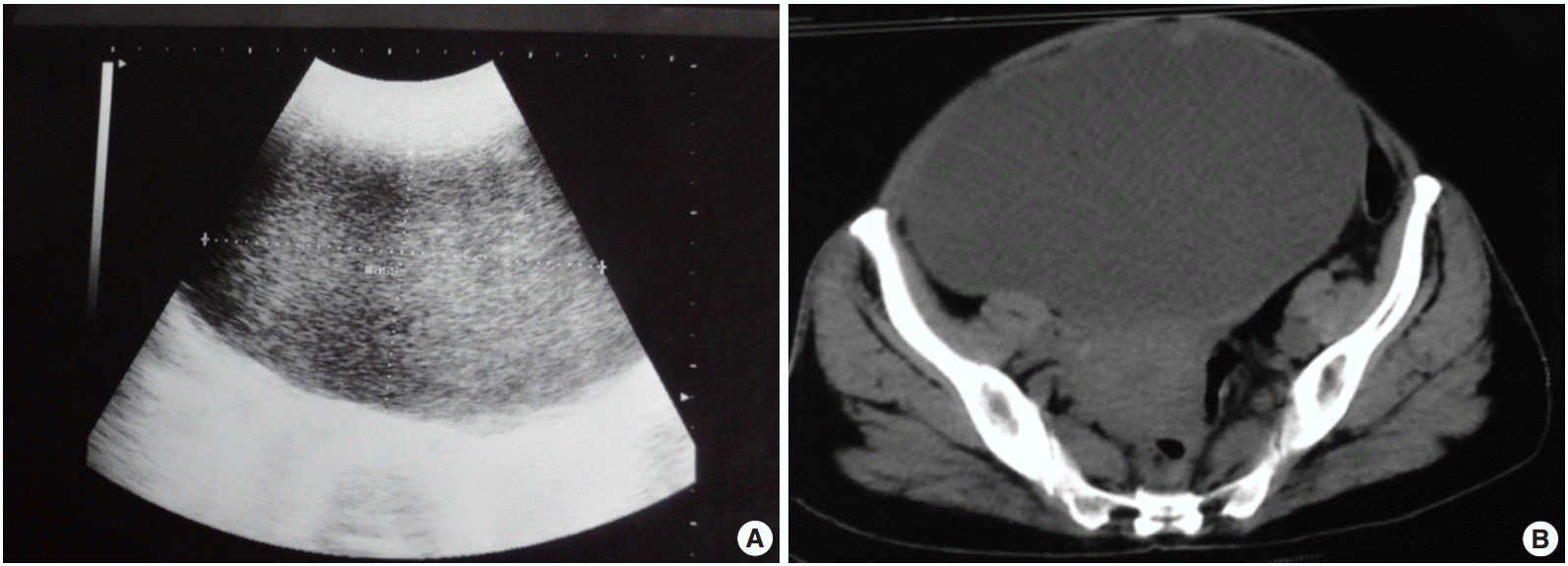

Fig. 2.Cut surface showing a thin walled unilocular cyst with a smooth inner surface and multiple tiny papillary excrescences and hemorrhagic areas.
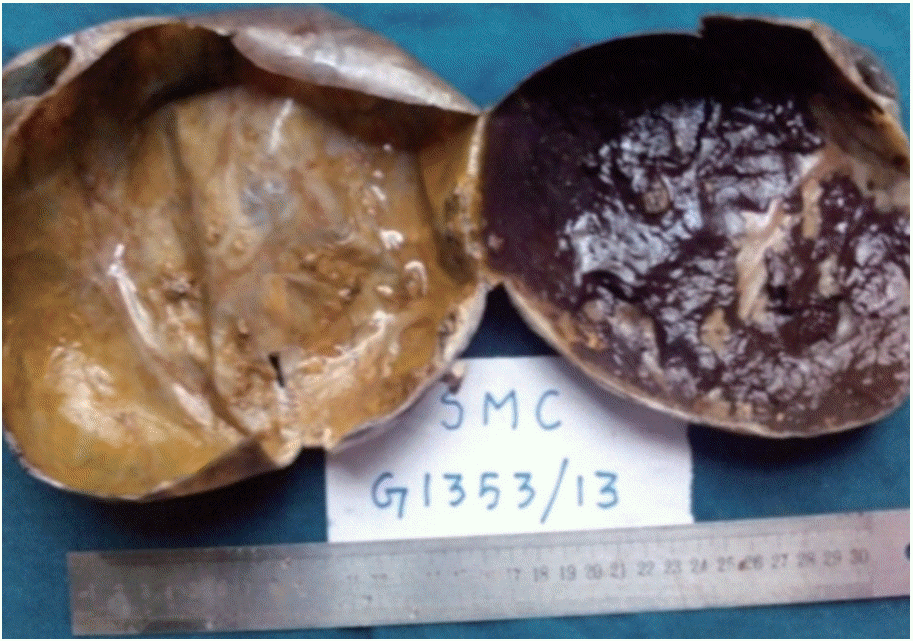

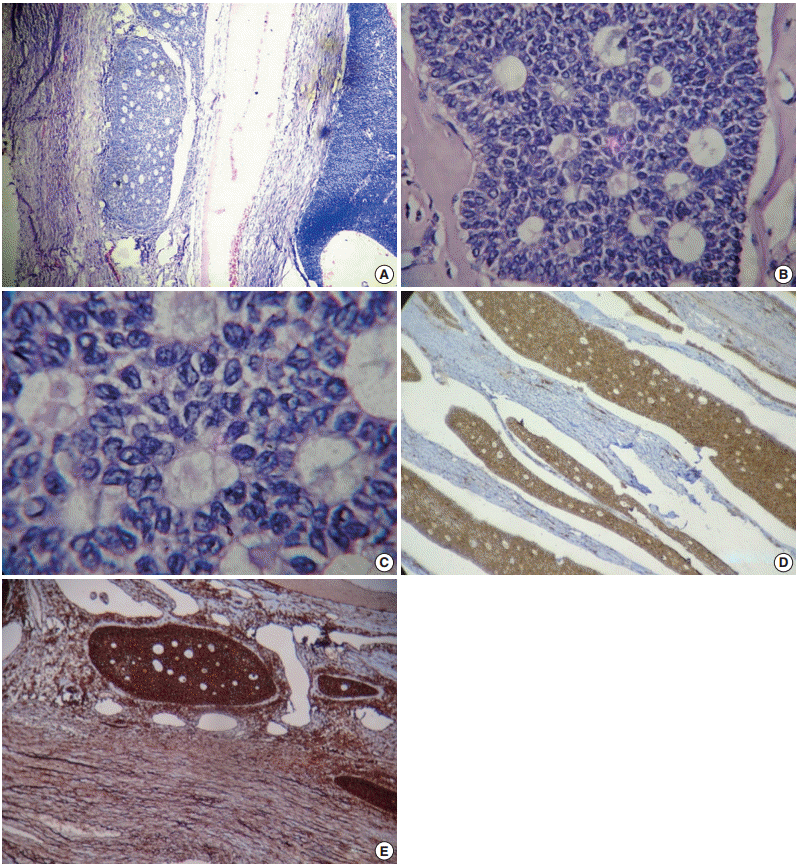
Fig. 3.(A) A cyst wall lined by multilayered granulosa cells and Call-Exner bodies. (B) A fibrocollagenous cyst wall lined by multilayered granulosa cells with interspersed Call-Exner bodies. (C) These Call-Exner bodies showing round to polyhedral granulosa cells with scant cytoplasm and round to oval grooved coffee bean nuclei. (D) Inhibin positive cells seen in the cytoplasm of tumor cells. (E) Vimentin positive cells seen as diffuse membrane positivity.

- 1. Roth LM. Sex cord stromal tumors of the ovary. In: Fox H, Wells M, eds. Haines and Taylor obstetrical and gynaecological pathology. New York: Churchill Livingstone, 1995; 824-30.
- 2. Scully RE. Tumors of the ovary and maldeveloped gonads. In: Hartmann WH, Cowan WR, eds. Atlas of tumor pathology, series 2, fascicles 16. Washington, DC: Armed Forces Institute of Pathology, 1979; 239-312.
- 3. Zaloudek C. The ovary. In: Gompel C, Silverberg SG, eds. Pathology in gynecology and obstetrics. 4th ed. Philadelphia: Lippincott, 1994; 313-413.
- 4. Rokitansky CV. Uber abnormalitaten des corpus luteum. Wien Med Ztc 1859; 4: 253-4.
- 5. Scully RE. Juvenile granulosa cell tumor. Pediatr Pathol 1988; 8: 423-7. PubMed
- 6. Nakashima N, Young RH, Scully RE. Androgenic granulosa cell tumors of the ovary: a clinicopathologic analysis of 17 cases and review of the literature. Arch Pathol Lab Med 1984; 108: 786-91. PubMed
- 7. Kurman RJ. Blaustein’s pathology of the female genital tract. 5th ed. New York: Springer-Verlag, 2002; 907.
- 8. Al-Nafussi AI. Tumor diagnosis: practical approach and pattern analysis. 2nd ed. New York: Oxford University Press, 2005; 491-2.
- 9. Fox H, Agrawal K, Langley FA. A clinicopathologic study of 92 cases of granulosa cell tumor of the ovary with special reference to the factors influencing prognosis. Cancer 1975; 35: 231-41. ArticlePubMed
- 10. Fujimoto T, Sakuragi N, Okuyama K, et al. Histopathological prognostic factors of adult granulosa cell tumors of the ovary. Acta Obstet Gynecol Scand 2001; 80: 1069-74. ArticlePubMed
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
Unicystic Granulosa Cell Tumor
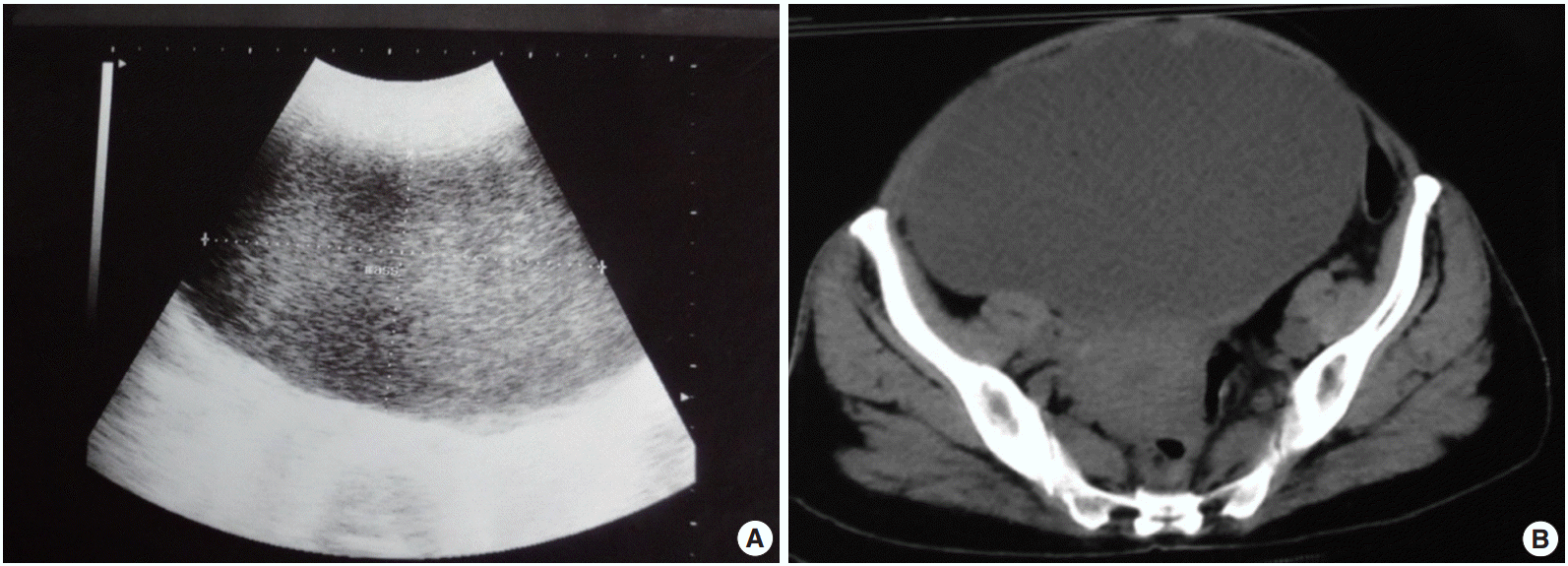
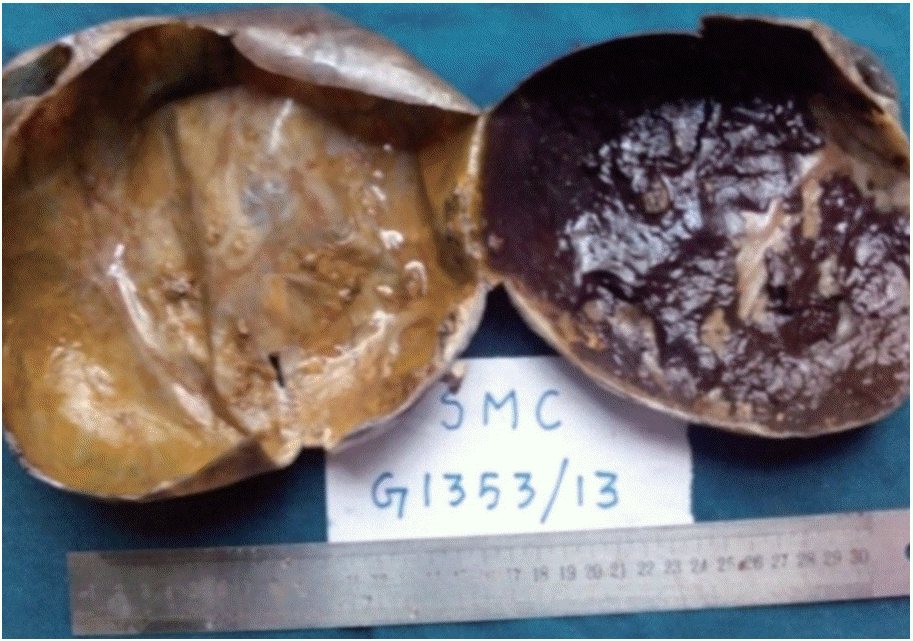
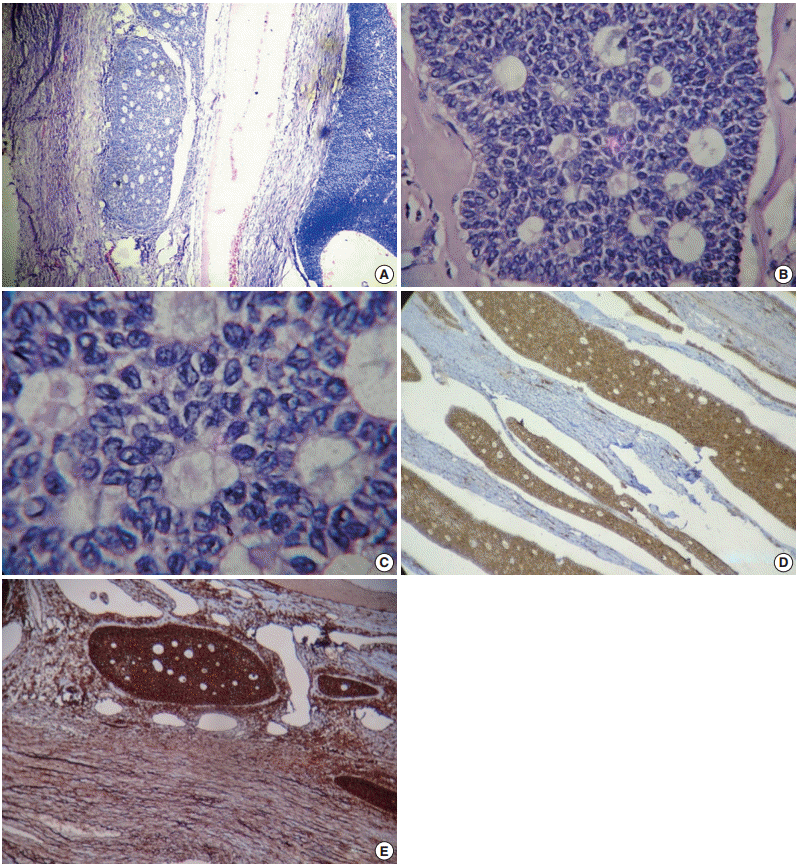
Fig. 1. (A) Mixed echogenic mass measuring 13×8.8 cm arising from the left side of the pelvis. (B) Large cystic space-occupying lesion with thick septa measuring 18.5×11.9×14.4 cm arising from the pelvis.
Fig. 2. Cut surface showing a thin walled unilocular cyst with a smooth inner surface and multiple tiny papillary excrescences and hemorrhagic areas.
Fig. 3. (A) A cyst wall lined by multilayered granulosa cells and Call-Exner bodies. (B) A fibrocollagenous cyst wall lined by multilayered granulosa cells with interspersed Call-Exner bodies. (C) These Call-Exner bodies showing round to polyhedral granulosa cells with scant cytoplasm and round to oval grooved coffee bean nuclei. (D) Inhibin positive cells seen in the cytoplasm of tumor cells. (E) Vimentin positive cells seen as diffuse membrane positivity.
Fig. 1.
Fig. 2.
Fig. 3.
Unicystic Granulosa Cell Tumor

 E-submission
E-submission





