Search
- Page Path
- HOME > Search
Review
- Cervical intraepithelial neoplasia and cervical cytology in pregnancy
- Ji-Young Kim, Jeong Yun Shim
- J Pathol Transl Med. 2024;58(6):283-290. Published online November 7, 2024
- DOI: https://doi.org/10.4132/jptm.2024.10.17
- 3,666 View
- 312 Download
-
 Abstract
Abstract
 PDF
PDF - Cervical cancer screening during pregnancy presents unique challenges for cytologic interpretation. This review focuses on pregnancy-associated cytomorphological changes and their impact on diagnosis of cervical intraepithelial neoplasia (CIN) and cervical cancer. Pregnancy-induced alterations include navicular cells, hyperplastic endocervical cells, immature metaplastic cells, and occasional decidual cells or trophoblasts. These changes can mimic abnormalities such as koilocytosis, adenocarcinoma in situ, and high-grade squamous intraepithelial lesions, potentially leading to misdiagnosis. Careful attention to nuclear features and awareness of pregnancy-related changes are crucial for correct interpretation. The natural history of CIN during pregnancy shows higher regression rates, particularly for CIN 2, with minimal risk of progression. Management of abnormal cytology follows modified risk-based guidelines to avoid invasive procedures, with treatment typically deferred until postpartum. The findings reported in this review emphasize the importance of considering pregnancy status in cytological interpretation, highlight potential problems, and provide guidance on differentiating benign pregnancy-related changes from true abnormalities. Understanding these nuances is essential for accurate diagnosis and proper management of cervical abnormalities in pregnant women.
Original Article
- Diagnostic distribution and pitfalls of glandular abnormalities in cervical cytology: a 25-year single-center study
- Jung-A Sung, Ilias P. Nikas, Haeryoung Kim, Han Suk Ryu, Cheol Lee
- J Pathol Transl Med. 2022;56(6):354-360. Published online November 9, 2022
- DOI: https://doi.org/10.4132/jptm.2022.09.05
- 5,245 View
- 128 Download
- 3 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Detection of glandular abnormalities in Papanicolaou (Pap) tests is challenging. This study aimed to review our institute’s experience interpreting such abnormalities, assess cytohistologic concordance, and identify cytomorphologic features associated with malignancy in follow-up histology.
Methods
Patients with cytologically-detected glandular lesions identified in our pathology records from 1995 to 2020 were included in this study.
Results
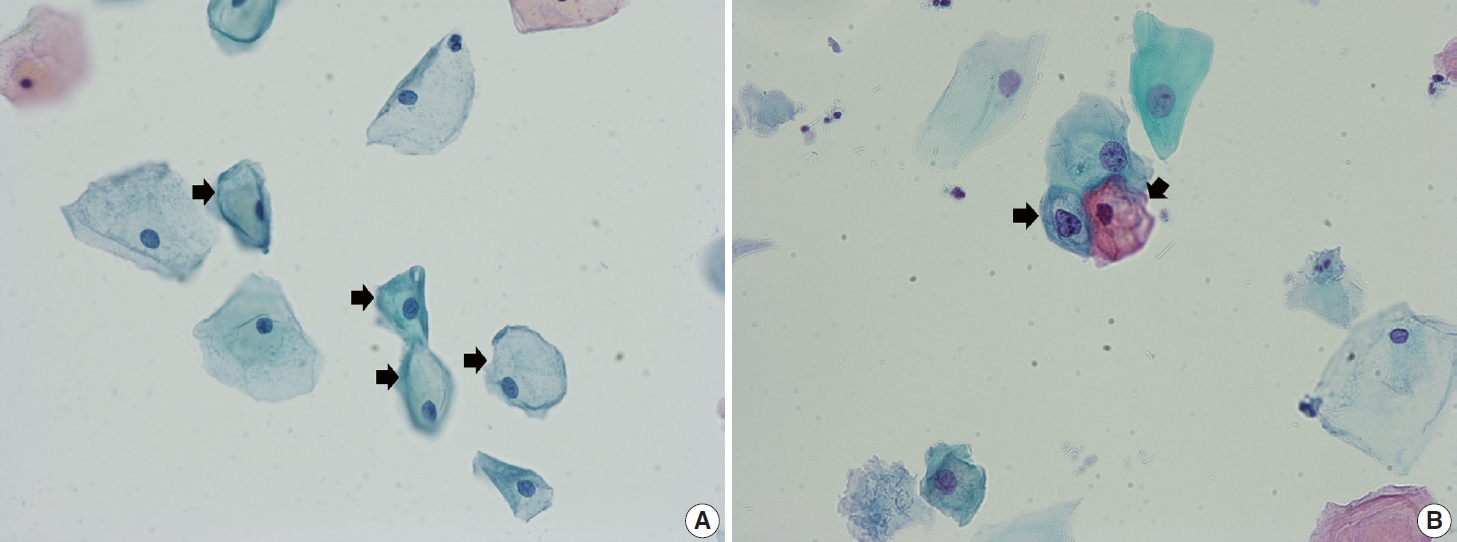
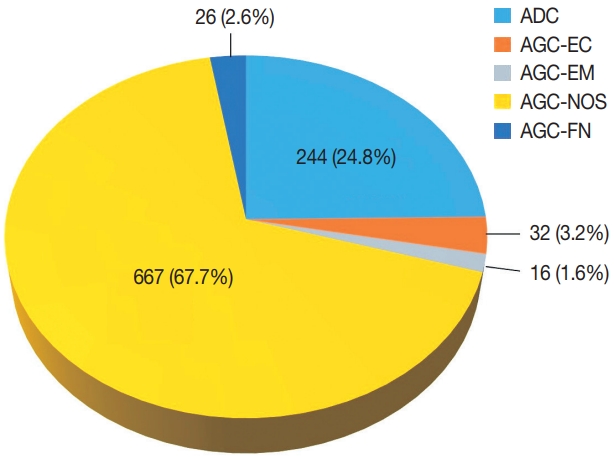
Of the 683,197 Pap tests performed, 985 (0.144%) exhibited glandular abnormalities, 657 of which had tissue follow-up available. One hundred eighty-eight cases were cytologically interpreted as adenocarcinoma and histologically diagnosed as malignant tumors of various origins. There were 213 cases reported as atypical glandular cells (AGC) and nine cases as adenocarcinoma in cytology, yet they were found to be benign in follow-up histology. In addition, 48 cases diagnosed with AGC and six with adenocarcinoma cytology were found to have cervical squamous lesions in follow-up histology, including four squamous cell carcinomas. Among the cytomorphological features examined, nuclear membrane irregularity, three-dimensional clusters, single-cell pattern, and presence of mitoses were associated with malignant histology in follow-up.
Conclusions
This study showed our institute’s experience detecting glandular abnormalities in cervical cytology over a 25-year period, revealing the difficulty of this task. Nonetheless, the present study indicates that several cytological findings such as membrane irregularity, three-dimensional clusters, single-cell pattern, and evidence of proliferation could help distinguishing malignancy from a benign lesion. -
Citations
Citations to this article as recorded by- Analysis of atypical glandular cells in ThinPrep Pap smear and follow-up histopathology
Tengfei Wang, Yinan Hua, Lina Liu, Bing Leng
Baylor University Medical Center Proceedings.2024; 37(3): 403. CrossRef
- Analysis of atypical glandular cells in ThinPrep Pap smear and follow-up histopathology
Review
- Clinical management of abnormal Pap tests: differences between US and Korean guidelines
- Seyeon Won, Mi Kyoung Kim, Seok Ju Seong
- J Pathol Transl Med. 2020;54(3):213-219. Published online April 15, 2020
- DOI: https://doi.org/10.4132/jptm.2020.03.11
- 7,989 View
- 159 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
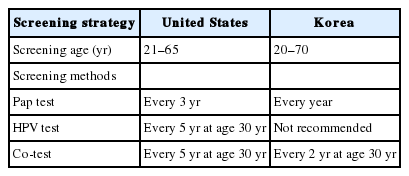
PDF - Cervical cancer has been the most common gynecological cancer in Korea but has become a preventable disease with regular screening and proper vaccination. If regular screening is provided, cervical cancer does not progress to more than carcinoma in situ, due to its comparatively long precancerous duration (years to decades). In 2012, the American Society for Colposcopy and Cervical Pathology published guidelines to aid clinicians in managing women with abnormal Papanicolaou (Pap) tests, and they soon became the standard in the United States. Not long thereafter, the Korean Society of Gynecologic Oncology and the Korean Society for Cytopathology published practical guidelines to reflect the specific situation in Korea. The detailed screening guidelines and management options in the case of abnormal Pap test results are sometimes the same and sometimes different in the United States and Korean guidelines. In this article, we summarize the differences between the United States and Korean guidelines in order to facilitate physicians’ proper management of abnormal Pap test results.
-
Citations
Citations to this article as recorded by- Analysis of HR-HPV Infection Concordance Rates in Cervical and Urine Specimens; Proposal of Additional Cervical Screening Process for Women Who Refuse Invasive Cervical Sampling
Dong Hyeok Kim, Hyunwoo Jin, Kyung Eun Lee
Journal of Personalized Medicine.2022; 12(12): 1949. CrossRef - Analysis of HR-HPV Prevalence among Unvaccinated Busan Women
Dong Hyeok Kim, Kyung Eun Lee
Biomedical Science Letters.2022; 28(4): 229. CrossRef
- Analysis of HR-HPV Infection Concordance Rates in Cervical and Urine Specimens; Proposal of Additional Cervical Screening Process for Women Who Refuse Invasive Cervical Sampling
Original Article
- Comparison of papanicolaou smear and human papillomavirus (HPV) test as cervical screening tools: can we rely on HPV test alone as a screening method? An 11-year retrospective experience at a single institution
- Myunghee Kang, Seung Yeon Ha, Hyun Yee Cho, Dong Hae Chung, Na Rae Kim, Jungsuk An, Sangho Lee, Jae Yeon Seok, Juhyeon Jeong
- J Pathol Transl Med. 2020;54(1):112-118. Published online January 15, 2020
- DOI: https://doi.org/10.4132/jptm.2019.11.29
- 10,598 View
- 251 Download
- 19 Web of Science
- 20 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The decrease in incidence of cervical dysplasia and carcinoma has not been as dramatic as expected with the development of improved research tools and test methods. The human papillomavirus (HPV) test alone has been suggested for screening in some countries. The National Cancer Screening Project in Korea has applied Papanicolaou smears (Pap smears) as the screening method for cervical dysplasia and carcinoma. We evaluated the value of Pap smear and HPV testing as diagnostic screening tools in a single institution.
Methods
Patients co-tested with HPV test and Pap smear simultaneously or within one month of each other were included in this study. Patients with only punch biopsy results were excluded because of sampling errors. A total of 999 cases were included, and the collected reports encompassed results of smear cytology, HPV subtypes, and histologic examinations.
Results
Sensitivity and specificity of detecting high-grade squamous intraepithelial lesion (HSIL) and squamous cell carcinoma (SCC) were higher for Pap smears than for HPV tests (sensitivity, 97.14%; specificity, 85.58% for Pap smears; sensitivity, 88.32%; specificity, 54.92% for HPV tests). HPV tests and Pap smears did not differ greatly in detection of low-grade squamous intraepithelial lesion (85.35% for HPV test, 80.31% for Pap smears). When atypical glandular cells were noted on Pap smears, the likelihood for histologic diagnosis of adenocarcinoma following Pap smear was higher than that of high-risk HPV test results (18.8 and 1.53, respectively).
Conclusions
Pap smears were more useful than HPV tests in the diagnosis of HSIL, SCC, and glandular lesions. -
Citations
Citations to this article as recorded by- Detection of cervical precancerous lesions and cancer by small-scale RT-qPCR analysis of oppositely deregulated mRNAs pairs in cytological smears
Anastasia A. Artyukh, Mikhail K. Ivanov, Sergei E. Titov, Victoria V. Dzyubenko, Sergey E. Krasilnikov, Anastasia O. Shumeikina, Nikita A. Afanasev, Anastasia V. Malek, Sergei A. Glushkov, Eduard F. Agletdinov
Frontiers in Oncology.2025;[Epub] CrossRef - High burden of abnormal cervical smears in South African primary health care: health programmes implications
Olufemi B Omole, Joel M Francis, John M Musonda, Pumla P Sodo, Elizabeth Reji, Nyundu S J Phukuta, Honey L M Mabuza, Joyce S Musonda, Jimmy Akii, John V Ndimande, Olalekan A Ayo-Yusuf
Health Promotion International.2025;[Epub] CrossRef - Bibliometric analysis: a study of the microenvironment in cervical cancer (2000-2024)
Yun-Tao Zhang, Yan-Ni Wei, Chen-Chen Liu, Mai-Qing Yang
Frontiers in Oncology.2025;[Epub] CrossRef - Challenges in the diagmosis of cervical pathologies
D. Y. Chernov, O. A. Tikhonovskaya, S. V. Logvinov, I. A. Petrov, Y. S. Yuriev, A. A. Zhdankina, A. V. Gerasimov, I. V. Zingalyuk, G. A. Mikheenko
Bulletin of Siberian Medicine.2024; 22(4): 201. CrossRef - “Barriers and Advantages of Self-Sampling Tests, for HPV Diagnosis: A Qualitative Field Experience Before Implementation in a Rural Community in Ecuador”
Bernardo Vega-Crespo, Vivian Alejandra Neira, Ruth Maldonado - Rengel, Diana López, Dayanara Delgado-López, Gabriela Guerra Astudillo, Veronique Verhoeven
International Journal of Women's Health.2024; Volume 16: 947. CrossRef - Cervical Human Papillomavirus Testing
Carol N. Rizkalla, Eric C. Huang
Surgical Pathology Clinics.2024; 17(3): 431. CrossRef - Segmentation of Overlapping Cells in Cervical Cytology Images: A Survey
E Chen, Hua-Nong Ting, Joon Huang Chuah, Jun Zhao
IEEE Access.2024; 12: 114170. CrossRef - Knowledge and awareness regarding pap test and HPV typing for cervical cancer screening in Edo North, Nigeria
Amina Momodu, Johnsolomon Eghosa Ohenhen, Godfrey Innocent Iyare, Musa Abidemi Muhibi, Godwin Avwioro
Discover Public Health.2024;[Epub] CrossRef - Colposcopy Value in Young Child-bearing Women: Is New Recommendations Necessary?
Fahimeh Sabet, Avishan Aminizad, Fariba Behnamfar, Tajossadat Allameh, Seyedeh Ghazal Shahrokh, Rostami Koushan, Amirmohammad Taravati, Leila Mousavi Seresht
Advanced Biomedical Research.2024;[Epub] CrossRef - Selection of endogenous control and identification of significant microRNA deregulations in cervical cancer
T. Stverakova, I. Baranova, P. Mikyskova, B. Gajdosova, H. Vosmikova, J. Laco, V. Palicka, H. Parova
Frontiers in Oncology.2023;[Epub] CrossRef - Cytology Versus Molecular Diagnosis of HPV for Cervical Cancer Screening. Comparison of the Diagnostic Properties of Four Tests in a Rural Community of Cuenca Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, Rocío Murillo, Cristina Ochoa Avilés
ESPOCH Congresses: The Ecuadorian Journal of S.T.E.A.M..2023; 3(1): 139. CrossRef - Attitudes towards prevention of cervical cancer and early diagnosis among female academicians
Nurhan Doğan, Gamze Fışkın
Journal of Obstetrics and Gynaecology Research.2022; 48(6): 1433. CrossRef - Role of Self-Sampling for Cervical Cancer Screening: Diagnostic Test Properties of Three Tests for the Diagnosis of HPV in Rural Communities of Cuenca, Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, José Ortíz Segarra, Ruth Maldonado Rengel, Diana López, María Paz Orellana, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, Veronique Verhoeven
International Journal of Environmental Research and Public Health.2022; 19(8): 4619. CrossRef - Utility of Scoring System for Screening and Early Warning of Cervical Cancer Based on Big Data Analysis
Dan Hou, Binjie Yang, Yangdan Li, Ming Sun
Frontiers in Public Health.2022;[Epub] CrossRef - Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, José Ortíz S, Ruth Maldonado-Rengel, Diana López, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, Veronique Verhoeven
Healthcare.2022; 10(9): 1614. CrossRef - Diagnostic distribution and pitfalls of glandular abnormalities in cervical cytology: a 25-year single-center study
Jung-A Sung, Ilias P. Nikas, Haeryoung Kim, Han Suk Ryu, Cheol Lee
Journal of Pathology and Translational Medicine.2022; 56(6): 354. CrossRef - Primary screening of cervical cancer by Pap smear in women of reproductive age group
Ruchi Mishra, Dakshina Bisht, Manisha Gupta
Journal of Family Medicine and Primary Care.2022; 11(9): 5327. CrossRef - Comparison of Learning Transfer Using Simulation Problem-Based Learning and Demonstration: An Application of Papanicolaou Smear Nursing Education
Jeongim Lee, Hae Kyoung Son
International Journal of Environmental Research and Public Health.2021; 18(4): 1765. CrossRef - Investigating host-virus interaction mechanism and phylogenetic analysis of viral proteins involved in the pathogenesis
Ahmad Abu Turab Naqvi, Farah Anjum, Alaa Shafie, Sufian Badar, Abdelbaset Mohamed Elasbali, Dharmendra Kumar Yadav, Md. Imtaiyaz Hassan, Timir Tripathi
PLOS ONE.2021; 16(12): e0261497. CrossRef - Utility of Human Papillomavirus Testing for Cervical Cancer Screening in Korea
Mee-seon Kim, Eun Hee Lee, Moon-il Park, Jae Seok Lee, Kisu Kim, Mee Sook Roh, Hyoun Wook Lee
International Journal of Environmental Research and Public Health.2020; 17(5): 1726. CrossRef
- Detection of cervical precancerous lesions and cancer by small-scale RT-qPCR analysis of oppositely deregulated mRNAs pairs in cytological smears
Review
- Current Status of and Perspectives on Cervical Cancer Screening in Korea
- Sung-Chul Lim, Chong Woo Yoo
- J Pathol Transl Med. 2019;53(4):210-216. Published online May 16, 2019
- DOI: https://doi.org/10.4132/jptm.2019.04.11
- 10,015 View
- 270 Download
- 8 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - Since the introduction of the Papanicolaou (Pap) smear system in 1943, cervicovaginal cytology has been used as a standard screening test for cervical cancer. The dissemination of this test contributed to reductions of the incidence and mortality of cervical cancer worldwide. In Korea, regular health check-ups for industrial workers and their family members were introduced in 1988 and were performed as part of the National Cancer Screening Program in 1999. As a result, the incidence of cervical cancer in Korea has been steadily decreasing. However, about 800 cases of cervical cancer-related deaths are reported each year due to false-negative test results. Hence, new screening methods have been proposed. Liquid-based cytology (LBC) was introduced in 1996 to overcome the limitations of conventional Pap smears. Since then, other LBC methods have been developed and utilized, including the human papilloma virus test—a method with higher sensitivity that requires fewer screenings. In this study, we review current issues and future perspectives related to cervical cancer screening in Korea.
-
Citations
Citations to this article as recorded by- A questionnaire study on disparity of cervical cancer prevention programs in Asia‐Oceania
Ka Yu Tse, Kimio Ushijima, Ai Ling Tan, Perapong Intasorn, Jitendra Pariyar, Chih‐Long Chang, Efren J. Domingo, Hiralal Konar, Suresh Kumarasamy, Brahmana Askandar Tjokroprawiro, Sarikapan Wilailak
Journal of Obstetrics and Gynaecology Research.2023; 49(4): 1230. CrossRef - Current state of cytopathology residency training: a Korean national survey of pathologists
Uiju Cho, Tae Jung Kim, Wan Seop Kim, Kyo Young Lee, Hye Kyoung Yoon, Hyun Joo Choi
Journal of Pathology and Translational Medicine.2023; 57(2): 95. CrossRef - Meeting the challenges of cervical cancer screening and HPV vaccination in the UK
Roxanne Westwood, Joanna Lavery
Primary Health Care.2022; 32(01): 22. CrossRef - Local and Metastatic Relapses in a Young Woman with Papillary Squamous Cell Carcinoma of the Uterine Cervix
Ha Young Woo, Hyun-Soo Kim
Diagnostics.2022; 12(3): 599. CrossRef - Serum Human Epididymis Protein 4 as a Prognostic Marker in Cervical Cancer
Woo Yeon Hwang, Dong Hoon Suh, Kidong Kim, Yong Beom Kim, Jae Hong No
Cancer Control.2022;[Epub] CrossRef - HPV detection and/or cytological diagnostics
Sanja Milenković
Glasnik javnog zdravlja.2022; 96(3): 313. CrossRef - Clinical management of abnormal Pap tests: differences between US and Korean guidelines
Seyeon Won, Mi Kyoung Kim, Seok Ju Seong
Journal of Pathology and Translational Medicine.2020; 54(3): 213. CrossRef - Current status of cytopathology practices in Korea: annual report on the Continuous Quality Improvement program of the Korean Society for Cytopathology for 2018
Yosep Chong, Haeyoen Jung, Jung-Soo Pyo, Soon Won Hong, Hoon Kyu Oh
Journal of Pathology and Translational Medicine.2020; 54(4): 318. CrossRef - Cytomorphological Features of Hyperchromatic Crowded Groups in Liquid-Based Cervicovaginal Cytology: A Single Institutional Experience
Youngeun Lee, Cheol Lee, In Ae Park, Hyoung Jin An, Haeryoung Kim
Journal of Pathology and Translational Medicine.2019; 53(6): 393. CrossRef
- A questionnaire study on disparity of cervical cancer prevention programs in Asia‐Oceania
Original Articles
- Comparison of Unsatisfactory Samples from Conventional Smear versus Liquid-Based Cytology in Uterine Cervical Cancer Screening Test
- Hoiseon Jeong, Sung Ran Hong, Seoung-Wan Chae, So-Young Jin, Hye Kyoung Yoon, Juhie Lee, Eun Kyung Kim, Sook Tai Ha, Sung Nam Kim, Eun-Jung Park, Jong Jae Jung, Sun Hee Sung, Sung-chul Lim
- J Pathol Transl Med. 2017;51(3):314-319. Published online April 17, 2017
- DOI: https://doi.org/10.4132/jptm.2017.03.17
- 12,189 View
- 325 Download
- 17 Web of Science
- 20 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Cervical cytology for uterine cervical cancer screening has transitioned from conventional smear (CS) to liquid-based cytology (LBC), which has many advantages. The aim of this study was to compare the proportion of unsatisfactory specimens from CS versus LBC at multiple institutions including general hospitals and commercial laboratories.
Methods
Each participating institution provided a minimum of 500 Papanicolaou (Pap) test results for analysis. Pap tests were classified according to the participating institution (commercial laboratory or general hospital) and the processing method (CS, ThinPrep, SurePath, or CellPrep). The causes of unsatisfactory results were classified as technical problems, scant cellularity, or complete obscuring factors.
Results
A total of 38,956 Pap test results from eight general hospitals and three commercial laboratories were analyzed. The mean unsatisfactory rate of LBC was significantly lower than that of CS (1.26% and 3.31%, p = .018). In the LBC method, samples from general hospitals had lower unsatisfactory rates than those from commercial laboratories (0.65% vs 2.89%, p = .006). The reasons for unsatisfactory results were heterogeneous in CS. On the other hand, 66.2% of unsatisfactory results in LBC were due to the scant cellularity.
Conclusions
Unsatisfactory rate of cervical cancer screening test results varies according to the institution and the processing method. LBC has a significantly lower unsatisfactory rate than CS. -
Citations
Citations to this article as recorded by- Poor Performance of Applicator Tampon‐Based Self‐Collection for Liquid‐Based Cytology Among Women Attending a Tertiary Hospital in South Africa
Teboho Amelia Tiiti, Varsetile Varster Nkwinika, Tebogo Loraine Mashishi, Kgotlaethata Aaron Molefi, Thembeni Lucia Msibi, Moshawa Khaba, Johannes Bogers, Ramokone Lisbeth Lebelo
Diagnostic Cytopathology.2025; 53(4): 150. CrossRef - The state of cervical cancer screening in Vanuatu: A retrospective analysis (2015–2020)
Emma R. Allanson, Vera Velanova, Boniface Damutalau, Harriet Obed, Geetha Warrier, Ian H. Frazer, Margaret McAdam
Malignancy Spectrum.2025; 2(1): 46. CrossRef - Comparison of conventional Pap smear and liquid-based cytology in detecting cervical abnormalities
Đelila Šečerović
Sanamed.2024; 19(2): 227. CrossRef - The possibilities of adapting the re-processing protocol in the practice of the ThinPrep Pap test usage
Artem K. Aksamentov, Nadezhda V. Melnikova, Eugenia V. Moshnina, Nadezhda A. Kolyshkina, Olga N. Kucherova, Vladimir P. Baklaushev
Journal of Clinical Practice.2023; 14(1): 108. CrossRef - The Role of p16/Ki67 Dual Staining in Cervical Cancer Screening
Andraž Dovnik, Alenka Repše Fokter
Current Issues in Molecular Biology.2023; 45(10): 8476. CrossRef - Evaluation of a Novel Fixative Solution for Liquid-Based Cytology in Diagnostic Cytopathology
Nadia Casatta, Alessia Poli, Sara Bassani, Gianna Veronesi, Giulio Rossi, Clarissa Ferrari, Carmelo Lupo
Diagnostics.2023; 13(24): 3601. CrossRef - Liquid-Based Cytology in the Detection of Premalignant Lesions in Patients with “Atypia in Squamous Cells” in Conventional Cytology
Lia Barrios, Yoled Vizcaíno, Ines Benedetti
Journal of Cytology.2022; 39(4): 148. CrossRef - Meeting the challenges of cervical cancer screening and HPV vaccination in the UK
Roxanne Westwood, Joanna Lavery
Primary Health Care.2022; 32(01): 22. CrossRef - Method for preservation of DNA stability of liquid-based cytology specimens from a lung adenocarcinoma cell line
Yukiko Matsuo, Kazuya Yamashita, Tsutomu Yoshida, Yukitoshi Satoh
Virchows Archiv.2021; 478(3): 507. CrossRef - High-risk human papillomavirus test in anal smears: can it optimize the screening for anal cancer?
Cintia M.S. Kimura, Caio S.R. Nahas, Edésio V. Silva-Filho, Vinícius L. Ribeiro, Aluisio C. Segurado, Flávio F.P. Alcântara, Ivan Cecconello, Sergio C. Nahas
AIDS.2021; 35(5): 737. CrossRef - Automatic model for cervical cancer screening based on convolutional neural network: a retrospective, multicohort, multicenter study
Xiangyu Tan, Kexin Li, Jiucheng Zhang, Wenzhe Wang, Bian Wu, Jian Wu, Xiaoping Li, Xiaoyuan Huang
Cancer Cell International.2021;[Epub] CrossRef - The cytological component of cervical cancer screening: causes of false negative and false positive results, and ways to avoid them
O.A. Burka, N.F. Lygyrda, V.V. Kutsovol, A.V. Svintsitska
REPRODUCTIVE ENDOCRINOLOGY.2021; (57): 61. CrossRef - Comparison of liquid-based cytology with conventional smear cytology for EUS-guided FNA of solid pancreatic masses: a prospective randomized noninferiority study
Jung Won Chun, Kyoungbun Lee, Sang Hyub Lee, Haeryoung Kim, Min Su You, Yoon Jung Hwang, Woo Hyun Paik, Ji Kon Ryu, Yong-Tae Kim
Gastrointestinal Endoscopy.2020; 91(4): 837. CrossRef - Effective reduction in inadequate Pap smears by using a saline-lubricated speculum and two glass slides
Chi-Jui Chen, Mun-Kun Hong, Dah-Ching Ding
Taiwanese Journal of Obstetrics and Gynecology.2020; 59(6): 906. CrossRef - Characterizing the Effect of Automated Cell Sorting Solutions on Cytomorphological Changes
Katsuhide Ikeda, Shouichi Sato, Hiroshi Chigira, Yasuo Shibuki, Nobuyoshi Hiraoka
Acta Cytologica.2020; 64(3): 232. CrossRef - Comparison between Conventional Cytology and Liquid-Based Cytology in the Tertiary Brazilian Navy Hospital in Rio de Janeiro
Antônio Carlos Almeida de Oliveira, Miguel Fontes Domingues, Paulo Murilo Neufeld, Marcos Fleury, José Firmino Nogueira Neto
Acta Cytologica.2020; 64(6): 539. CrossRef - Follow‐up with histopathology and HPV testing on LSIL cytology in China’s largest academic woman’s hospital
Xiang Tao, Huina Zhang, Hao Zhang, Jianan Xiao, Juan Li, Xianrong Zhou, Li Wang, Chengquan Zhao
Cancer Cytopathology.2019; 127(4): 258. CrossRef - Current Status of and Perspectives on Cervical Cancer Screening in Korea
Sung-Chul Lim, Chong Woo Yoo
Journal of Pathology and Translational Medicine.2019; 53(4): 210. CrossRef - Reducing DNA damage by formaldehyde in liquid‐based cytology preservation solutions to enable the molecular testing of lung cancer specimens
Yukiko Matsuo, Tsutomu Yoshida, Kazuya Yamashita, Yukitoshi Satoh
Cancer Cytopathology.2018; 126(12): 1011. CrossRef - Cervical Cancer Screening Programs in Europe: The Transition Towards HPV Vaccination and Population-Based HPV Testing
Andreas C. Chrysostomou, Dora C. Stylianou, Anastasia Constantinidou, Leondios G. Kostrikis
Viruses.2018; 10(12): 729. CrossRef
- Poor Performance of Applicator Tampon‐Based Self‐Collection for Liquid‐Based Cytology Among Women Attending a Tertiary Hospital in South Africa
- Comparison of Cytologic Characteristics between Adenoid Cystic Carcinoma and Adenoid Basal Carcinoma in the Uterine Cervix
- Juhyeon Jeong, Seung Yeon Ha, Hyun Yee Cho, Dong Hae Chung, Jungsuk An
- J Pathol Transl Med. 2015;49(5):396-402. Published online August 17, 2015
- DOI: https://doi.org/10.4132/jptm.2015.07.08
- 9,759 View
- 95 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Adenoid cystic carcinoma (ACC) and adenoid basal carcinoma (ABC) are rare in the uterine cervix. ACC is more aggressive than ABC, thus accurate differential diagnosis is important. In this study, we identified cytologic features useful in distinguishing these two tumors for diagnosis. Methods: Three cases of ACC and five cases of ABC were selected for this study. Cervicovaginal smear slides were reviewed retrospectively, and the area, circumference, major axis, and minor axis of nuclei were measured using an image analyzer. Results: ACC displayed three-dimensional clusters with a small acini pattern. ABC displayed peripheral palisading without an acini pattern. The nuclei of ACC were more irregular and angulated than those of ABC, and the former showed a coarsely granular chromatin pattern. The nucleic area, circumference, major axis, and minor axis were 18.556±8.665 µm2, 23.320±11.412 µm, 5.664±1.537 µm, and 4.127±1.107 µm in ACC and 11.017±4.440 µm2, 15.920±5.664 µm, 4.612±1.025 µm, and 3.088±0.762 µm in the cases of ABC. All measured values showed statistically significant difference (p < .001). Conclusions: Although the nuclei of both of these tumor types were oval shaped, inferred from the ratio of minor axis to major axis (0.728 in ACC and 0.669 in ABC), the area of nuclei was approximately 1.7 times larger in ACC than in ABC. Distinguishing nucleic features, including area, morphology, and chromatin pattern, may be helpful in making a correct diagnosis. -
Citations
Citations to this article as recorded by- Adenoid basal carcinoma of the uterine cervix
Anas Mohamed, Tesfalem Korga, Ahlam Ali, Javier Laurini
International Journal of Gynecological Cancer.2025; : 101873. CrossRef - Adenoid Basal Carcinoma of the Uterine Cervix: A Case Report
Tatsuya Kanuma, Keiko Kigure, Tosio Nishimura, Yuji Ibuki, Shigeru Tsuchida, Harumi Kamiyama, Misa Iijima, Kazuto Nakamura
The KITAKANTO Medical Journal.2016; 66(1): 11. CrossRef
- Adenoid basal carcinoma of the uterine cervix
- Prevalence and Genotype Distribution of Cervical Human Papillomavirus DNA in Korean Women: A Multicenter Study.
- Sung Ran Hong, In Sun Kim, Dong Won Kim, Mi Jin Kim, Ae Ree Kim, Young Ok Kim, Hye Sun Kim, Seo Hee Rha, Gyeong Sin Park, Yong Koo Park, Yong Wook Park, Ho Sung Park, Kwang Sun Suh, Jin Hee Sohn, Mi Kyung Shin, Hoon Kyu Oh, Ki Jung Yun, Hye Kyoung Yoon, Shi Nae Lee, Ah Won Lee, Hyo Jin Lee, Hyun Yee Cho, Chan Choi, Woon Won Jung
- Korean J Pathol. 2009;43(4):342-350.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.4.342
- 5,632 View
- 61 Download
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
DNA prevalence and type distribution of human papillomavirus (HPV) varies geographically. We investigated HPV prevalence and type distribution in Korean women using the MyHPV DNA chip testing. Methods: A total of 2,368 women from five regions of the country underwent Pap smear examination and MyHPV chip testing. Results: Overall HPV positivity was 15.8% and 78.4% in women with normal and abnormal cytology, respectively. High-risk HPV infection was strongly correlated with cytological atypia. In women with abnormal cytology, the five most common HPV types were 16, 58, 18, 52, and 56/53, and HPV16 was significantly the most common type in most geographical regions. After HPV16, HPV58, and 52 were the next most frequently detected types. Women with normal cytology, in contrast, showed heterogeneity in HPV type distribution. High-grade intraepithelial lesions infected with HPV16, 18, 31 or 45 are more likely to progress to carcinoma. Conclusions: The HPV chip test can provide useful data regarding HPV positivity and type. The most common HPV type in Korean women with abnormal cytology is HPV16, with HPV58 and 52 being frequently present. Our data may have important implications for vaccination programs and the development of cervical screening. -
Citations
Citations to this article as recorded by- HPV genotyping by L1 amplicon sequencing of archived invasive cervical cancer samples: a pilot study
Charles D. Warden, Preetam Cholli, Hanjun Qin, Chao Guo, Yafan Wang, Chetan Kancharla, Angelique M. Russell, Sylvana Salvatierra, Lorraine Z. Mutsvunguma, Kerin K. Higa, Xiwei Wu, Sharon Wilczynski, Raju Pillai, Javier Gordon Ogembo
Infectious Agents and Cancer.2022;[Epub] CrossRef - Enhanced disease progression due to persistent HPV-16/58 infections in Korean women: a systematic review and the Korea HPV cohort study
Jaehyun Seong, Sangmi Ryou, JeongGyu Lee, Myeongsu Yoo, Sooyoung Hur, Byeong-Sun Choi
Virology Journal.2021;[Epub] CrossRef - Comparison of FFPE histological versus LBP cytological samples for HPV detection and typing in cervical cancer
Geehyuk Kim, Hyemi Cho, Dongsup Lee, Sunyoung Park, Jiyoung Lee, Hye-young Wang, Sunghyun Kim, Kwang Hwa Park, Hyeyoung Lee
Experimental and Molecular Pathology.2017; 102(2): 321. CrossRef - Distribution of Oncogenic Human Papillomavirus Genotypes at High Grade Cervical Lesions above CIN 2 Grade with Histological Diagnosis
Geehyuk Kim, Sungyoung Park, Hye-young Wang, Sunghyun Kim, Sangjung Park, Kwangmin Yu, Boohyung Lee, Seung-Ju Ahn, Eun-Joong Kim, Dongsup Lee
Biomedical Science Letters.2016; 22(2): 37. CrossRef - Human Papillomavirus Prevalence and Genotype Distribution in Normal and ASCUS Specimens: Comparison of a Reverse Blot Hybridization Assay with a DNA Chip Test
Sunghyun Kim, In-soo Lee, Dongsup Lee
Biomedical Science Letters.2015; 21(1): 32. CrossRef - Genotype Analysis of Human Papilloma Virus Infection in Accordance with Cytological Diagnoses
Mi-Suk Park, Hyun-Wook Cho, Jin-Gak Kim, Nan-Young Bae, Dong-Sun Oh, Ho-Hyun Park
Korean Journal of Clinical Laboratory Science.2015; 47(1): 39. CrossRef - Comparison of the Cobas 4800 HPV and HPV 9G DNA Chip Tests for Detection of High-Risk Human Papillomavirus in Cervical Specimens of Women with Consecutive Positive HPV Tests But Negative Pap Smears
Sun-Young Jun, Eun Su Park, Jiyoung Kim, Jun Kang, Jae Jun Lee, Yoonjin Bae, Sang-Il Kim, Lee-So Maeng, Magdalena Grce
PLOS ONE.2015; 10(10): e0140336. CrossRef - Uncommon and Rare Human Papillomavirus Genotypes Relating to Cervical Carcinomas
Na Rae Kim, Myunghee Kang, Soon Pyo Lee, Hyunchul Kim, Jungsuk An, Dong Hae Chung, Seung Yeon Ha, Hyun Yee Cho
Korean Journal of Pathology.2014; 48(1): 43. CrossRef - Evaluation of Human Papillomavirus Genotyping from Formalin-fixed Paraffin-embedded Specimens in Cervical Cancers
Hyunwoo Jin
Journal of Life Science.2014; 24(9): 1025. CrossRef - Comparative Evaluation of the HPV28 Detection and HPV DNA Chip Test for Detecting and Genotyping Human Papillomaviruses
Eunsim Shin, Heojin Bae, Wan-Keun Song, Sun-Kyung Jung, Yoo-Sung Hwang
Laboratory Medicine Online.2013; 3(4): 234. CrossRef - Significance of HPV-58 Infection in Women Who Are HPV-Positive, Cytology-Negative and Living in a Country with a High Prevalence of HPV-58 Infection
Joon Seon Song, Eun Ju Kim, Jene Choi, Gyungyub Gong, Chang Ohk Sung, Robert D. Burk
PLoS ONE.2013; 8(3): e58678. CrossRef - REBA HPV‐ID® for efficient genotyping of human papillomavirus in clinical samples from Korean patients
Sunghyun Kim, Dongsup Lee, Sangjung Park, Tae Ue Kim, Bo‐Young Jeon, Kwang Hwa Park, Hyeyoung Lee
Journal of Medical Virology.2012; 84(8): 1248. CrossRef - Dynamin 2 expression as a biomarker in grading of cervical intraepithelial neoplasia
Yoo-Young Lee, Sang Yong Song, In-Gu Do, Tae-Joong Kim, Byoung-Gie Kim, Jeong-Won Lee, Duk-Soo Bae
European Journal of Obstetrics & Gynecology and Reproductive Biology.2012; 164(2): 180. CrossRef - Cytomorphologic Features According to HPV DNA Type in Histologically Proven Cases of the Uterine Cervix
In Ho Choi, So-Young Jin, Dong Wha Lee, Dong Won Kim, Yoon Mi Jeen
The Korean Journal of Pathology.2011; 45(6): 612. CrossRef - Human Papillomavirus Prevalence in Gangwon Province Using Reverse Blot Hybridization Assay
Dongsup Lee, Sunghyun Kim, Sangjung Park, Hyunwoo Jin, Tae Ue Kim, Kwang Hwa Park, Hyeyoung Lee
The Korean Journal of Pathology.2011; 45(4): 348. CrossRef - Pediatric vulvar squamous cell carcinoma in a liver transplantation recipient: a case report
Na-Rae Kim, Soyi Lim, Hyun Yee Cho
Journal of Gynecologic Oncology.2011; 22(3): 207. CrossRef
- HPV genotyping by L1 amplicon sequencing of archived invasive cervical cancer samples: a pilot study
Review Article
- Liquid-Based Cytology in Gynecologic Cytology.
- Yonghee Lee
- Korean J Pathol. 2009;43(4):291-300.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.4.291
- 3,832 View
- 61 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Conventional cervical smears have been a great tool to reduce the incidence of cervical cancer; however, many studies have revealed significant false negative rates. To resolve this problem, the liquid based cytology (LBC) method was developed. The LBC method reduces the number of false positive and false negative smear results because LBC achieves an even distribution of monolayered cells, eliminated the obscuring effects of inflammation and blood. Although the LBC method has many advantages, there are several drawbacks. The LBC method requires an adaptation period for cytopathologists and cytotechnicians. Another drawback is the expense of the method. Thus, the LBC method has been questioned, and criticism has been raised regarding the design of the studies that assert its superiority. With a focus on the cytomorphologic and technical differences of LBC compared with conventional cervical smears, a review of the clinical and cost effectiveness of LBC, a brief comparison of two popular LBC methods, and the basic concepts of study design with respect to LBC are presented in this review.
-
Citations
Citations to this article as recorded by- The efficacy of pancreatic juice cytology with liquid-based cytology for evaluating malignancy in patients with intraductal papillary mucinous neoplasm
Kazuya Miyamoto, Kazuyuki Matsumoto, Hironari Kato, Ryuichi Yoshida, Yuzo Umeda, Hirohumi Inoue, Takehiro Tanaka, Akihiro Matsumi, Yosuke Saragai, Yuki Fujii, Tatsuhiro Yamazaki, Daisuke Uchida, Takeshi Tomoda, Shigeru Horiguchi, Takahito Yagi, Hiroyuki O
BMC Gastroenterology.2020;[Epub] CrossRef - Comparison of liquid-based cytology (CellPrepPlus) and conventional smears in pancreaticobiliary disease
Myeong Ho Yeon, Hee Seok Jeong, Hee Seung Lee, Jong Soon Jang, Seungho Lee, Soon Man Yoon, Hee Bok Chae, Seon Mee Park, Sei Jin Youn, Joung-Ho Han, Hye-Suk Han, Ho Chang Lee
The Korean Journal of Internal Medicine.2018; 33(5): 883. CrossRef
- The efficacy of pancreatic juice cytology with liquid-based cytology for evaluating malignancy in patients with intraductal papillary mucinous neoplasm
Original Article
- Clinical Efficacy of Manual Liquid-Based Cervicovaginal CytologyPreparation: Comparative Study with Conventional Papanicolaou Test.
- Jong Myoung Park, Jong Gi Lee, In Soo Suh
- Korean J Cytopathol. 2005;16(1):10-17.
- 1,873 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - This study was performed to compare manual liquid-based preparation with conventional Papanicolaou tests in view of the cytologic diagnoses and specimen adequacy. The specimens of 5,979 women from 33 local clinics and 1 general hospital were prepared by both manual liquid-based preparation and conventional Papanicolaou test. The cytologic diagnoses and specimen adequacy were evaluated in Department of Pathology in Kyoungpook National University School of Medicine. A conventional Papanicolaou test was always prepared first, after that residual material on the sampling device was rinsed into a liquid preservative, and then thin-layer slides were prepared using manual method of liquid-based cervicovaginal cytology. Conventional and liquid-based slides were read independently, and cytologic diagnoses and specimen adequacy were classified using the Bethesda System. Of the cases, 5,763(96.3%) had the same interpretation, and there was no significant diagnostic difference in 5,853(97.8%) cases. When evaluating cases with more than one diagnostic class difference, the manual liquid-based preparation demonstrated a statistically significant overall improvement(2.1%) in the detection of squamous intraepithelial lesion and invasive cancer. Using manual method of liquid- based preparation, there was 14.1% reduction in unsatisfactory slides through excellent cellular presentations. In conclusion, the manual liquid-based preparation produces standardized quality, superior sensitivity and improved adequacy as compared to the conventional method.

 E-submission
E-submission


 First
First Prev
Prev



