Search
- Page Path
- HOME > Search
Original Articles
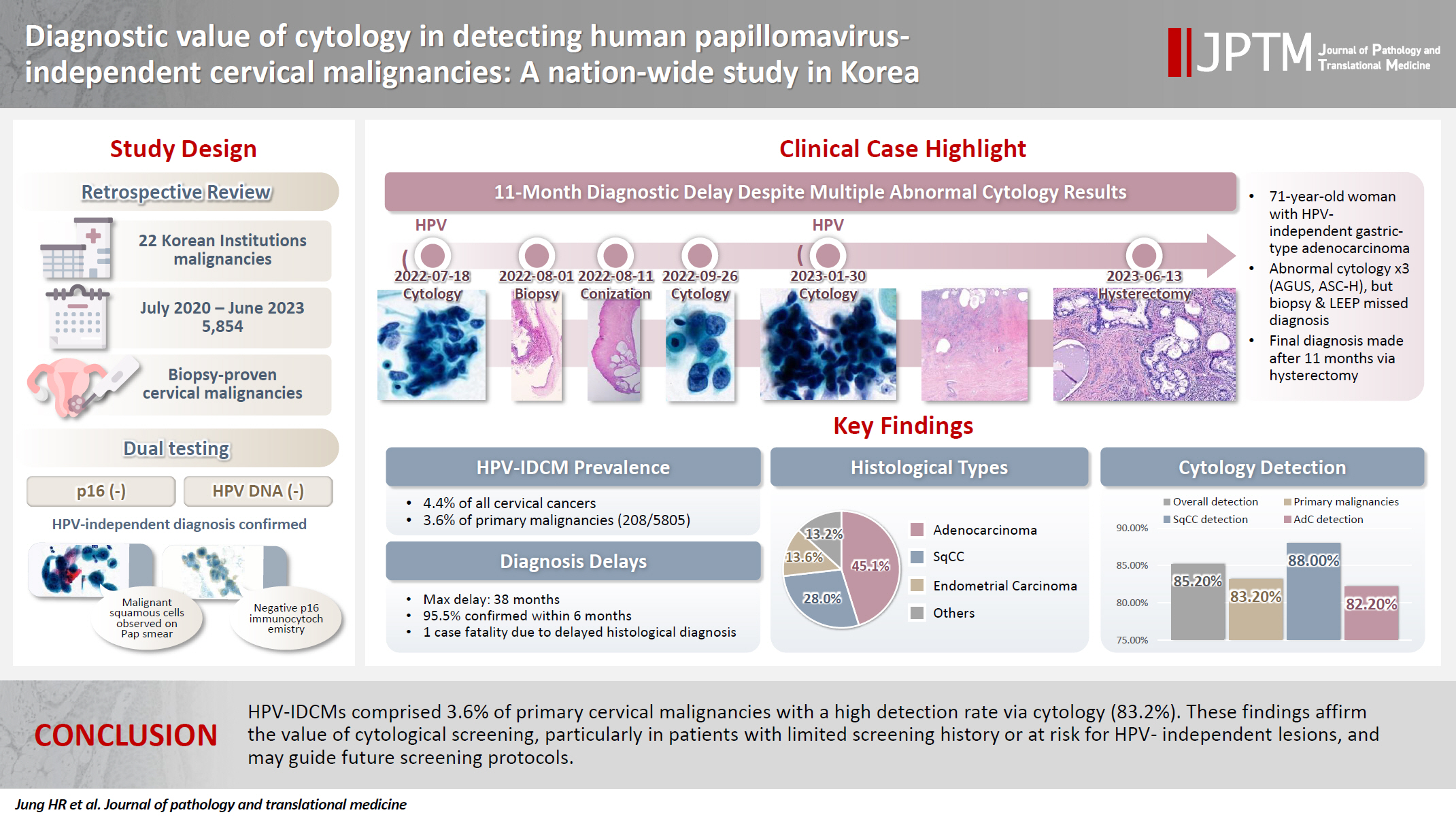
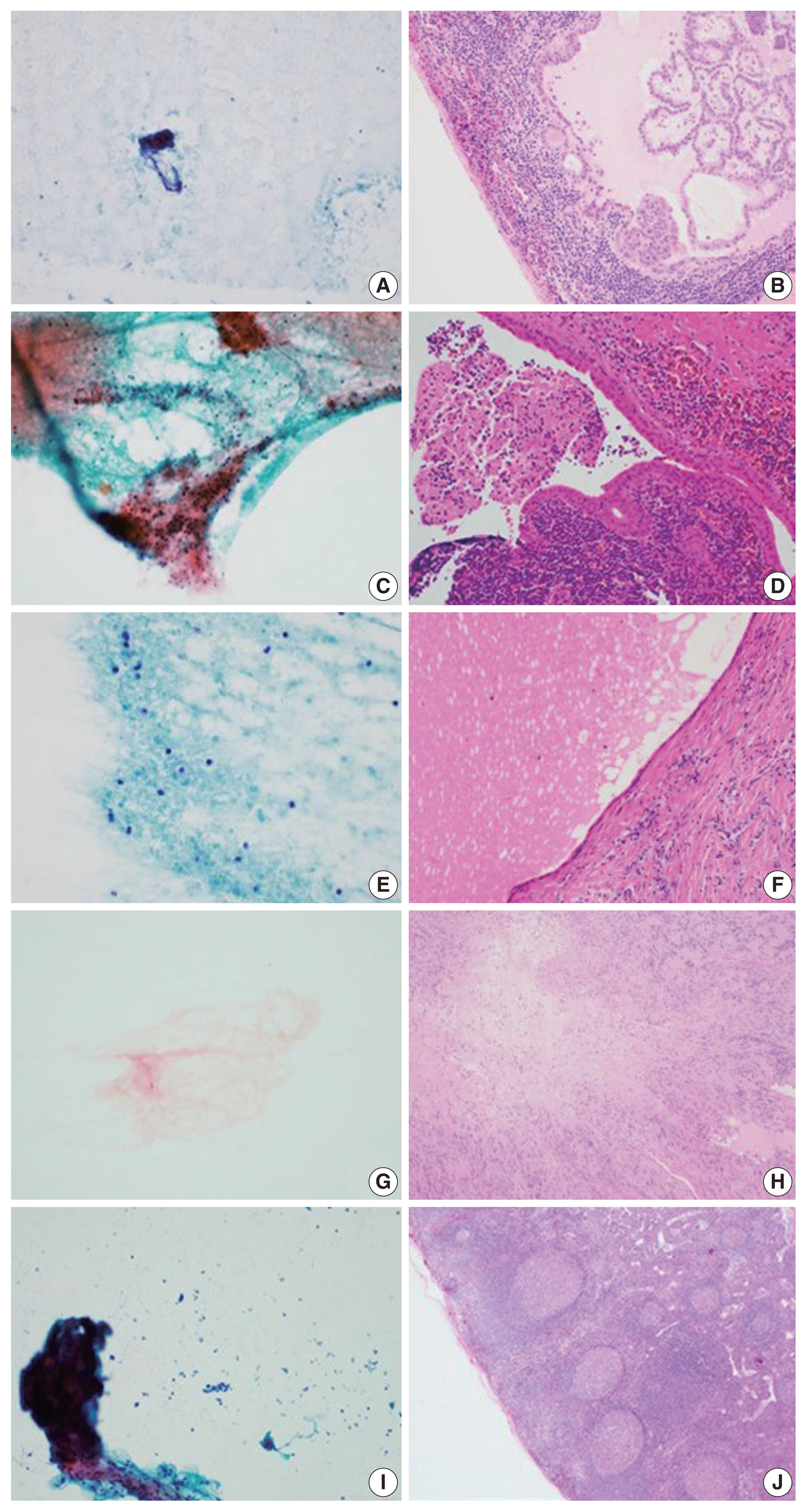
- Diagnostic value of cytology in detecting human papillomavirus–independent cervical malignancies: a nation-wide study in Korea
- Hye-Ra Jung, Junyoung Shin, Chong Woo Yoo, Eun Na Kim, Cheol Lee, Kyeongmin Kim, Ho-chang Lee, Yonghee Lee, Ji Hye Kim, Soo Jin Jung, Yumin Chung, Joo Yeon Kim, Hye Eun Park, Tae Hoen Kim, Wonae Lee, Min-Sun Cho, Ran Hong, Yoon Jung Choi, Younghee Choi, Young Sub Lee, Sang-Ryung Lee, Myunghee Kang, Young Jin Seo, Seung-Sook Lee, Yoon-Jung Hwang, Hyun-Jung Kim
- J Pathol Transl Med. 2025;59(6):444-452. Published online November 11, 2025
- DOI: https://doi.org/10.4132/jptm.2025.10.21
- 4,969 View
- 153 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) independent cervical malignancies (HPV-IDCMs) have recently been classified by the World Health Organization (WHO) 5th edition. These malignancies have historically received limited attention due to their rarity and the potential for evasion of HPV-based screening.
Methods
We retrospectively reviewed 5,854 biopsy-confirmed cervical malignancies from 22 institutions over 3 years (July 2020–June 2023). Histologic classification followed the WHO guidelines. HPV independence was confirmed by dual negativity for p16 and HPV; discordant cases (p16-positive/HPV-negative) underwent additional HPV testing using paraffin-embedded tissue. Cytological results were matched sequentially to histological confirmation.
Results
The prevalence of HPV-IDCM was 4.4% (257/5,854) overall and was 3.6% (208/5,805 cases) among primary cervical malignancy. Patient age of HPV-IDCM was 29 to 89 years (median, 57.79). Its histologic subtypes included primary adenocarcinoma (n = 116), endometrial adenocarcinoma (n = 35), squamous cell carcinoma (n = 72), metastatic carcinoma (n = 14), carcinoma, not otherwise specified (n = 10), neuroendocrine carcinoma (n = 3), and others (n = 7). Among 155 cytology-histological matched cases, the overall and primary Pap test detection rates were 85.2% (132/155) and 83.2% (104/125), respectively. The interval between cytology and histologic confirmation extended up to 38 months.
Conclusions
HPV-IDCMs comprised 3.6% of primary cervical malignancies with a high detection rate via cytology (83.2%). These findings affirm the value of cytological screening, particularly in patients with limited screening history or at risk for HPV-independent lesions, and may guide future screening protocols.
- Causes of necrotic features in fine-needle aspirates from cervical lymph nodes
- Young Jin Seo, Hyeongchan Shin, Hye Won Lee, Hye Ra Jung
- J Pathol Transl Med. 2021;55(1):60-67. Published online November 27, 2020
- DOI: https://doi.org/10.4132/jptm.2020.09.28
- 19,854 View
- 211 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Lymph node fine-needle aspiration (LN FNA) cytology indicates necrosis in various diseases. Dominant necrotic features make the diagnosis of underlying conditions very difficult.
Methods
We retrospectively reviewed 460 patients who underwent cervical LN aspiration cytology that revealed necrotic findings at Keimyung University Dongsan Hospital in Daegu, Korea, from 2003–2017. Each specimen was evaluated and analyzed in association with the clinical findings, biopsy findings, and/or other ancillary tests, including acid-fast bacilli staining and molecular testing for Mycobacterium tuberculosis.
Results
When necrotic features were noted upon cervical LN FNA cytology, the most common pathologic LN FNA category was necrosis alone (31.5%). The second most common category was granulomatous inflammation (31.3%), followed by Kikuchi disease (20.0%) and malignant neoplasm (8.7%). In cases where the cervical LN FNA revealed necrosis alone, the most common final diagnosis was tuberculosis. In young patients, Kikuchi disease should be considered as one cervical LN FNA category, while metastatic carcinoma should be suspected in older patients.
Conclusions
Even when necrosis alone is observed in LN FNA cytology, it is important to determine the cause through further evaluation. -
Citations
Citations to this article as recorded by- Necrosis of a Metastatic Axillary Lymph Node in Breast Cancer Possibly Induced by Fine-Needle Aspiration Cytology: A Case Report
Yoshiko Masuda, Mikiko Aoki, Masumi Tanaka, Yukari Koga, Kyoko Eto, Yasuteru Yoshinaga, Toshihiko Sato
Case Reports in Oncology.2026; 19(1): 349. CrossRef - The Potential Use of Peptides in the Fight against Chagas Disease and Leishmaniasis
Hayelom Berhe, Mahesh Kumar Cinthakunta Sridhar, Mulate Zerihun, Nir Qvit
Pharmaceutics.2024; 16(2): 227. CrossRef - Tips and tricks for a proper radiological assessment of abdominal and pelvic lymph nodes
Ana Laura Lopes Potente, Cynthia Lopes Pereira de Borborema, Iza Campos Pedra Vieira, Aley Talans, Eduardo Oliveira Pacheco, Lucas Rios Torres, Serli Kiyomi Nakao Ueda, Fernanda Lopez Mazzucato, Andrei Saraiva Purysko, Daniel Lahan Martins, Ulysses Santos
Abdominal Radiology.2024; 49(11): 4057. CrossRef - Does the Necrotic Portion of Metastatic Lymphadenopathy from Squamous Cell Carcinoma Still Have Tumoral Oncologic Information? Differential Diagnosis of Benign Necrotic Lymphadenopathy Using microRNA
Eun Shin, Seung Hoon Han, Il-Seok Park, Jee Hye Wee, Joong Seob Lee, Heejin Kim
Biomedicines.2023; 11(9): 2407. CrossRef - Impact of HPV status in T1–2 oropharyngeal squamous cell carcinoma with bulky N3 nodes: a multicenter GETTEC study
Charles Hurel, Florent Carsuzaa, Julia Salleron, Philippe Gorphe, Christian Righini, Maximilien Rogé, Erwan de Mones, Sylvain Morinière, Sébastien Vergez, Juliette Thariat, Xavier Dufour
European Archives of Oto-Rhino-Laryngology.2023; 280(2): 847. CrossRef - Lymph nodes in health and disease – A pathologist's perspective
N S Priya
Journal of Oral and Maxillofacial Pathology.2023; 27(1): 6. CrossRef
- Necrosis of a Metastatic Axillary Lymph Node in Breast Cancer Possibly Induced by Fine-Needle Aspiration Cytology: A Case Report

 E-submission
E-submission

 First
First Prev
Prev



