Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 47(4); 2013 > Article
-
Case Study
Fine Needle Aspiration Cytology of Hepatic Hydatid Cyst: A Case Study - Ae Ri Kim, Seok Ju Park, Mi Jin Gu, Joon Hyuk Choi, Hong Jin Kim1
-
Korean Journal of Pathology 2013;47(4):395-398.
DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.4.395
Published online: August 26, 2013
Department of Pathology, Yeungnam University College of Medicine, Daegu, Korea.
1Department of Surgery, Yeungnam University College of Medicine, Daegu, Korea.
- Corresponding Author: Joon Hyuk Choi, M.D. Department of Pathology, Yeungnam University College of Medicine, 170 Hyeonchung-ro, Nam-gu, Daegu 705-717, Korea. Tel: +82-53-620-3335, Fax: +82-53-656-1429, joonhyukchoi@ynu.ac.kr
• Received: November 27, 2012 • Revised: December 27, 2012 • Accepted: January 18, 2013
© 2013 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
- Hydatid cysts (echinococcosis) are caused by an infestation with larval tapeworms of the genus Echinococcus. The disease is extensively distributed worldwide, and it has been rarely reported in Korea. We describe the cytologic features of a case of hepatic hydatid cyst in a 28-year-old male. Computed tomography revealed a cystic mass in the right lobe of the liver. A right hemihepatectomy was performed. The aspirated fluid from the hepatic cystic mass was clear. The smears showed protoscolices, hooklets, and a laminated membrane.
- A 28-year-old man presented with abdominal pain that had persisted for the past three months. The patient was a foreign worker from Uzbekistan. Physical examination revealed no abdominal mass. He had undergone partial hepatic resection due to a hydatid cyst 14 years ago. Abdominal computed tomography scan revealed a cystic mass in the right hepatic lobe (Fig. 1). Serologic testing for hydatid cysts was not performed. However, the clinical impression was a hydatid cyst. A right hemihepatectomy was performed, and the resected specimen was sent for intraoperative consultation. FNAC of the cystic mass was performed. The aspirated fluid was clear. Both smears and a cell block preparation were carried out. The smears were stained using Papanicolaou and hematoxylin and eosin stains.
- The smears showed many protoscolices in the shape of a mushroom, with hooklets (Fig. 2). Amorphous necrotic debris and inflammatory cells were present in the background. Degenerated protoscolices were also found. Detached hooklets with refractile structures were seen. Fragments of laminated membranes stained pinkish-red on hematoxylin-eosin stain. Therefore, the diagnosis of a hydatid cyst was made.
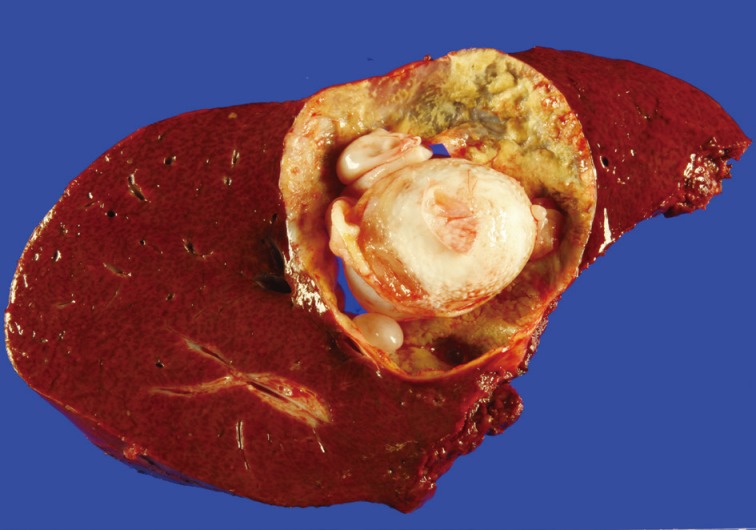
- On gross examination, the right hemihepatectomy specimen measured 15.3×14.8×8.5 cm in size. A 6.5×5.0×4.5 cm hepatic cyst was present (Fig. 3). The cyst contained multiple daughter cysts of variable sizes. The wall of the cyst was grayish white. Histologic examination revealed that the cyst wall was composed of an outer laminated membrane and an inner germinal layer (Fig. 4). Protoscolices and a brood capsule were seen. The laminated membrane was acellular and the germinal layer contained nuclei. The surrounding liver parenchyma showed a fibrinous wall and inflammatory cells infiltration including lymphocytes, eosinophils, and histiocytes. The patient has been alive for 16 months following this surgery without evidence of recurrence.
CASE REPORT
- Hydatid cyst is a parasite disease caused by the larval forms of Echinococcus tapeworms. Infections by E. granulosus are the most common. Humans are accidental intermediate hosts and become infected by ingestion of food contaminated with eggs shed by dogs or foxes. After ingestion, the eggs of E. granulosus hatch, and the larval oncospheres pass to the liver by the portal vein. Three quarters of infected individuals develop one or more hepatic cysts. The majority occurs in the right lobe, but they may be multiple and involve all lobes of the liver. A hydatid cyst is white, spherical, and filled with fluid. It varies from a few millimeters to many centimeters in diameter.1 Because of its slow growth, the diagnosis may be delayed for months to years after the initial infection. Clinical manifestations include hepatomegaly, obstructive jaundice, and cholangitis. Complications include cholangitis and rupture. If the patient is untreated, the hydatid cyst can be fatal.
- The adult E. granulosus is a small tapeworm capped by a scolex at the anterior terminus, and measures 3 to 5 mm in length. Four suckers and a double crown of 28-50 hooks emerge from the scolex.9 The cyst wall has a laminated membrane lined by a germinal layer. This membrane is about 1 mm thick and has no nuclei. The germinal layer is 10 to 25 µm in thickness and contains nuclei. In Korea, hydatid cysts are uncommon and are typically imported by travelers or workers from endemic areas.2-4 In the present case, the patient was a foreign worker who had lived the first 26 years of his life in an endemic area. Therefore, this infection probably originated in an endemic area.
- Cytologically, protoscolices, hooklets, and fragments of the laminated membrane are commonly found in hydatid cysts.5-8 In some cases, only laminated membranes were present in the inflammatory background.10-12 In the current case, protoscolices, hooklets, and laminated membranes were identified and the background showed necrotic debris and inflammatory cells. The liver is the most frequently involved organ. In cases of hydatid cysts that involve atypical locations and other organs, the diagnosis can be difficult. FNAC appears to be a safe and useful method in the diagnosis of hydatid cyst, although arguments regarding this issue persist.13 Cytologic diagnosis of hydatid cysts has been reported in the lung,14 omentum,15 muscle,16 soft tissue,10,12 brain,17 orbit,18 and joints.11
- The differential diagnosis of hepatic hydatid cyst includes abscess, hemangioma, and non-parasitic cysts such as solitary bile duct cyst and hepatobiliary cystadenoma. It may be difficult to find protoscolices in FNAC. Hydatid cyst should be considered when fragments suggestive of a laminated membrane are present on smears without evidence of protoscolices.12 A definite diagnosis of hydatid cyst is confirmed by identification of protoscolices, refractile hooklets or fragments of a laminated membrane. Surgical excision of the intact hydatid cyst without rupture is the treatment of choice, to reduce the chance of seeding and recurrence.9
- There have been significant advances in the knowledge of Echinococcus biology and the development of more specific and sensitive immunological tests.19 Early diagnosis of hydatid cyst by serology may provide opportunities for early treatment and more effective chemotherapy.20
- In conclusion, we presented the cytological features in a case of a hepatic hydatid cyst. FNAC is useful in making a diagnosis of a hydatid cyst of the liver. It is important to include hydatid cyst in the differential diagnosis of cystic lesions in the liver, particularly in those who have lived or traveled in endemic areas.
DISCUSSION
- 1. Sparks AK, Connor DH, Neafie RC. Echinococcosis. In: Binford CH, Connor DH, eds. Pathology of tropical and extraordinary diseases. Washington, DC: Armed Forces Institute of Pathology, 1976; 530-533.
- 2. Ahn MH. Traveling and imported parasitic diseases. J Korean Med Assoc 2007; 50: 993-1004. Article
- 3. Suh JH, Kim YH. Pulmonary hydatid cyst found in a foreign worker from the endemic area: a case report. Korean J Thorac Cardiovasc Surg 2008; 41: 527-531.
- 4. Byun SJ, Moon KC, Suh KS, Han JK, Chai JY. An imported case of echinococcosis of the liver in a Korean who traveled to western and central Europe. Korean J Parasitol 2010; 48: 161-165. ArticlePubMedPMC
- 5. Saenz-Santamaria J, Moreno-Casado J, Nuñez C. Role of fine-needle biopsy in the diagnosis of hydatid cyst. Diagn Cytopathol 1995; 13: 229-232. ArticlePubMed
- 6. Ciftçioğlu MA, Yildirgan MI, Akçay MN, Reis A, Safali M, Aktaş E. Fine needle aspiration biopsy in hepatic Echinococcus multilocularis. Acta Cytol 1997; 41: 649-652. PubMed
- 7. Agarwal PK, Husain N, Singh BN. Cytologic findings in aspirated hydatid fluid. Acta Cytol 1989; 33: 652-654. PubMed
- 8. Pogacnik A, Pohar-Marinsek Z, Us-Krasovec M. Fine needle aspiration biopsy in the diagnosis of liver echinococcosis. Acta Cytol 1990; 34: 765-766. PubMed
- 9. Fraiji EK Jr, Connor DH. Echinococcosis. In: Connor DH, Chandler FW, Schwartz DA, Manz HJ, Lack EE, eds. Pathology of infectious disease. Stamford: Appleton & Lange, 1997; 1405-1413.
- 10. Gupta R, Mathur SR, Agarwala S, Kaushal S, Srivastav A. Primary soft tissue hydatidosis: aspiration cytological diagnosis in two cases. Diagn Cytopathol 2008; 36: 884-886. ArticlePubMed
- 11. Wahane RN, Pangarkar MA, Bobhate SK. Fine needle aspiration cytology of a hydatid cyst of the pelvis and hip joint. Acta Cytol 2008; 52: 381-384. ArticlePubMed
- 12. Sáenz-Santamaría J, Catalina-Fernández I, Fernán de zdeMera JJ. Hydatid cyst in soft tissues mimicking malignant tumors. Diagnosis by fine needle aspiration cytology. Acta Cytol 2003; 47: 337-340. PubMed
- 13. Hira PR, Shweiki H, Lindberg LG, et al. Diagnosis of cystic hydatid disease: role of aspiration cytology. Lancet 1988; 2: 655-657. ArticlePubMed
- 14. Ingram EA, Helikson MA. Echinococcosis (hydatid disease) in Missouri: diagnosis by fine-needle aspiration of a lung cyst. Diagn Cytopathol 1991; 7: 527-531. ArticlePubMed
- 15. Rosa M, Sahoo S. Primary hydatid cyst of the omentum. Diagn Cytopathol 2009; 37: 117-118. ArticlePubMed
- 16. Das DK, El-Sharawy M, Ayyash EH, Al-Enezi NA, Iqbal JR, Madda JP. Primary hydatid cyst of the supraspinatus muscle: complete removal of the germinal layer and cytodiagnosis by fine-needle aspiration. Diagn Cytopathol 2012 9 25 [Epub]. http://dx.doi.org/10.1002/dc.22925. ArticlePMC
- 17. Sherwani RK, Abrari A, Jayrajpuri ZS, Srivastava VK. Intracranial hydatidosis: report of a case diagnosed on cerebrospinal fluid cytology. Acta Cytol 2003; 47: 506-508. PubMed
- 18. Sodhani P, Das DK, Natarajan R, Khan IU. Cytological diagnosis of orbital echinococcosis. Diagn Cytopathol 1996; 15: 52-53. ArticlePubMed
- 19. Nunnari G, Pinzone MR, Gruttadauria S, et al. Hepatic echinococcosis: clinical and therapeutic aspects. World J Gastroenterol 2012; 18: 1448-1458. ArticlePubMedPMC
- 20. McManus DP, Gray DJ, Zhang W, Yang Y. Diagnosis, treatment, and management of echinococcosis. BMJ 2012; 344: e3866.ArticlePubMed
REFERENCES
Fig. 1Abdomen computed tomography scan. A cystic mass with internal septation is present in the right hepatic lobe.
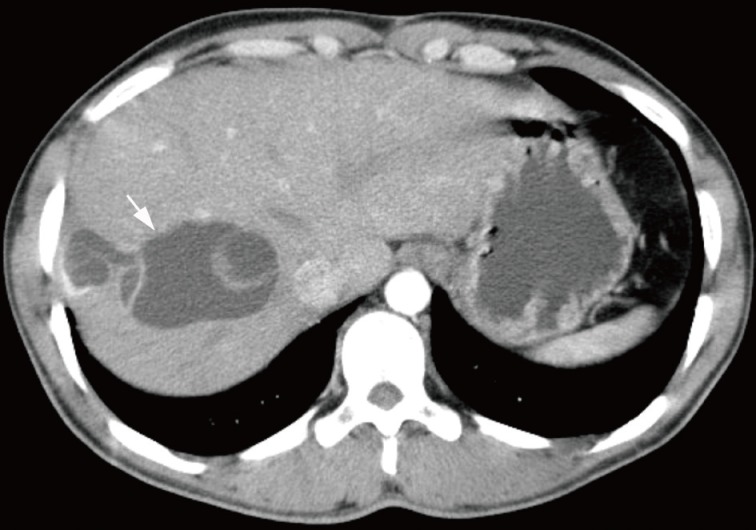

Fig. 2Cytologic findings. (A) There are many protoscolices in the shape of a mushroom. The necrotic debris is seen in the background. (B, C) Higher magnification of the protoscolices reveals hooklets. (D) Isolated refractile hooklets (arrows) are present. (E) Fragments of a laminated membrane are present.
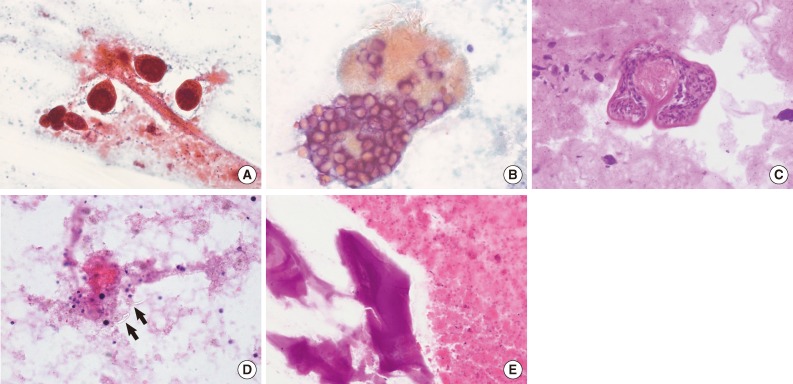

Fig. 4Histologic findings. (A) A hydatid cyst and adjacent liver parenchyma are seen. (B) The cyst wall is composed of an acellular laminated membrane and an inner nucleated germinal layer (arrow). Protoscolices and brood capsule (arrowhead) are present. (C) The liver shows a fibrinous wall and inflammatory cells infiltration, including lymphocytes, eosinophils, and histiocytes.
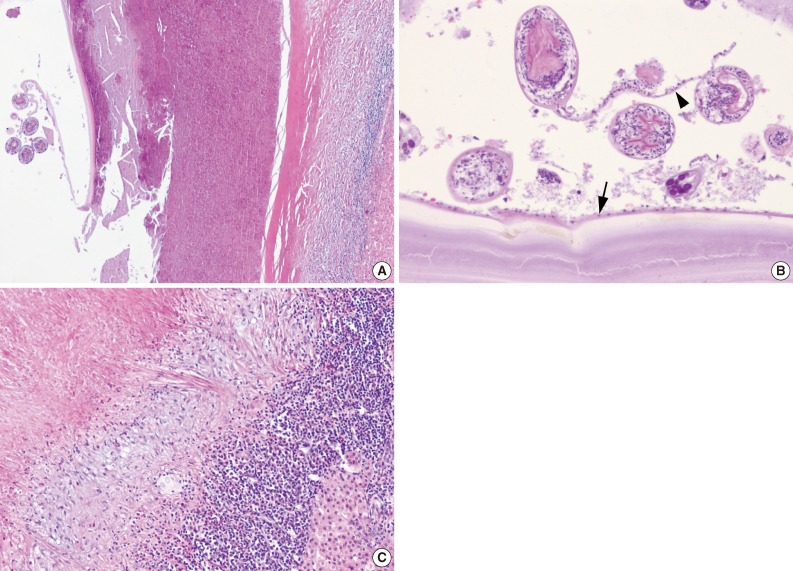

Figure & Data
References
Citations
Citations to this article as recorded by 

- Fine-Needle Aspiration Cytology of Hepatic Hydatid Disease: A Five-Year Case Series with Emphasis on Diagnostic Limitations
Fatlinda Sadiku, Ardita Qerimi, Gramoz Bunjaku, Ilir Maloku, Artina Pajaziti
Acta Cytologica.2026; : 1. CrossRef - Delayed Diagnosis of Imported Cystic Echinococcosis and Successful Treatment With Percutaneous Drainage and Albendazole in Korea: A Case Report
Won Jun Choi, Hanna Jin, Hyeon Jae Jo, Chan Mi Lee, Chang Kyung Kang, Pyoeng Gyun Choe, Wan Beom Park, Nam Joong Kim, Min-Ho Choi
Journal of Korean Medical Science.2025;[Epub] CrossRef - Imported parasitic diseases in the Republic of Korea: status and issues
Jong-Yil Chai
Journal of the Korean Medical Association.2025; 68(1): 52. CrossRef - Surgical Management of Multiple Cerebral Hydatid Cysts without Systemic Involvement: A Case Report
Roxana Radu, Miguel Azevedo, Angela Neacșu, Marius Cristian Zaharia, Radu Mircea Gorgan
Arquivos Brasileiros de Neurocirurgia: Brazilian Neurosurgery.2025; 44(03): e211. CrossRef - Different scenarios and management of complicated hepatic cystic echinococcosis: a case series
Thamer Alghamdi, Ramy Agwa, Fahad Alghamdi, Ahmed Mahmoud, Warda Othman
Journal of Surgical Case Reports.2025;[Epub] CrossRef - Hydatid Disease of the Pelvis: A Rare Manifestation With Diagnostic Challenges—A Case Report and Comprehensive Literature Review
Saurav Jha, Matsendra Jha, Sweta Singh, Sulav Kumar Jha, Bistrit Dahal, Anamika Adhikari, Sanskriti Dev
Clinical Case Reports.2025;[Epub] CrossRef - Chemical compounds, antioxidant and scolicidal potencies of Thymus fontanesii essential oil
Sidi Mohammed Ammar Selles, Belkacem Tahar Belhamiti, Mokhtaria Kouidri, Amar Ait Amrane, Yamina Kadari, Zohra Kaddour, Souad Kabrit
Experimental Parasitology.2024; 257: 108699. CrossRef - Complicated Liver Cystic Echinococcosis—A Comprehensive Literature Review and a Tale of Two Extreme Cases
Valentin Calu, Octavian Enciu, Elena-Adelina Toma, Radu Pârvuleţu, Dumitru Cătălin Pîrîianu, Adrian Miron
Tomography.2024; 10(6): 922. CrossRef - A rare case of hydatid cyst of the neck with concurrent pulmonary hydatid disease
Amarendra Kumar Shukla, Amrutha Peter, Veerendra Arya, Vineet Dwivedi, Manish Kumar Gupta, Nimish Rai, Pawan Tiwari, Jitendra Kishore Bhargava
Journal of Parasitic Diseases.2022; 46(4): 941. CrossRef - Hepatic Hydatid Cyst: A Case Report
Wan Chul Kim, Jae Uk Shin, Su Sin Jin
The Korean Journal of Gastroenterology.2021; 77(1): 35. CrossRef - An Imported Case of Disseminated Echinococcosis in Korea
Dong Hoon Shin, Hae Chan Jo, Jeong-Han Kim, Kang Il Jun, Wan Beom Park, Nam-Joong Kim, Min-Ho Choi, Chang Kyung Kang, Myoung-don Oh
The Korean Journal of Parasitology.2019; 57(4): 429. CrossRef - Cytology of hydatid cyst mimicking intra‐abdominal sarcoma, diagnosed by fine‐needle aspiration
Busra Ozbek, Nadir Paksoy
Diagnostic Cytopathology.2018; 46(4): 362. CrossRef - Clinical Update on Parasitic Diseases
Min Seo
Korean Journal of Medicine.2013; 85(5): 469. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
Fine Needle Aspiration Cytology of Hepatic Hydatid Cyst: A Case Study
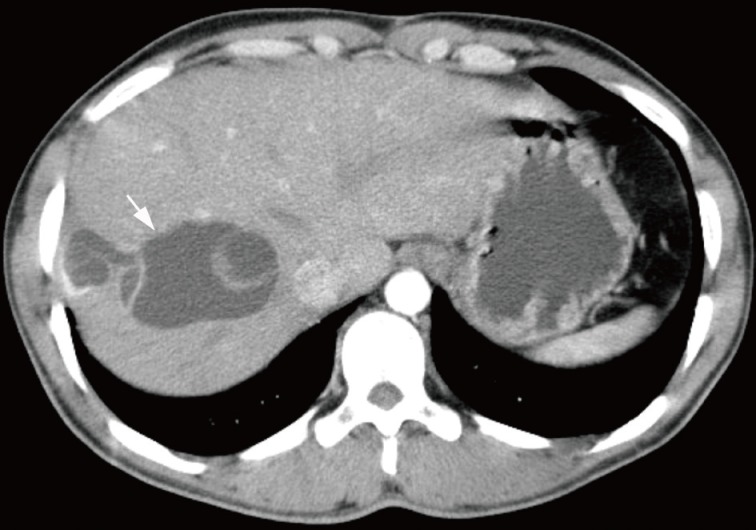
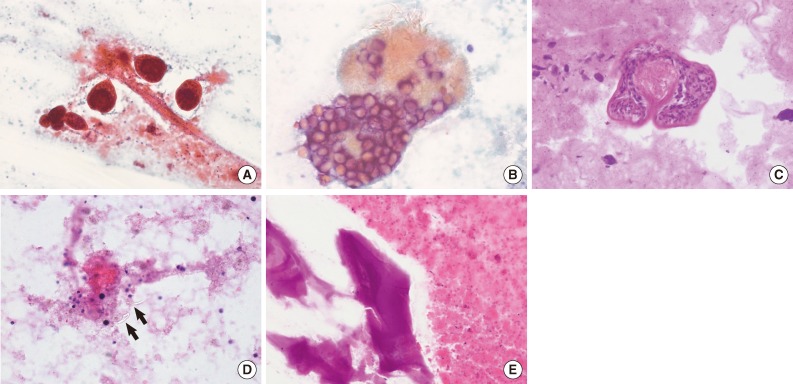
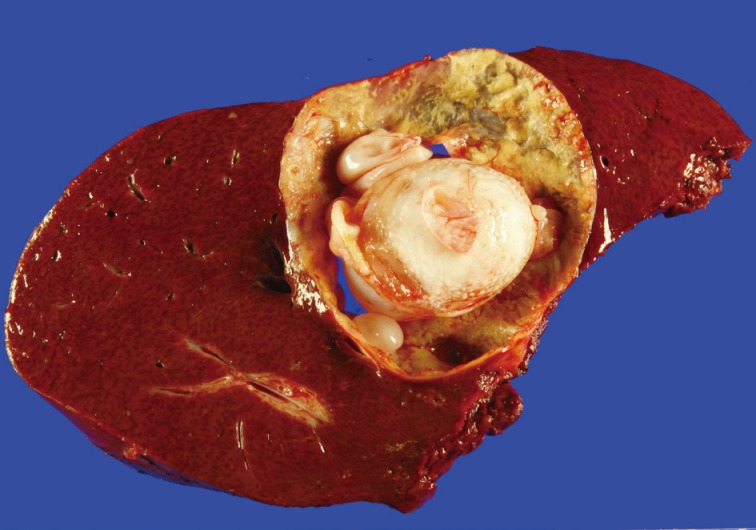
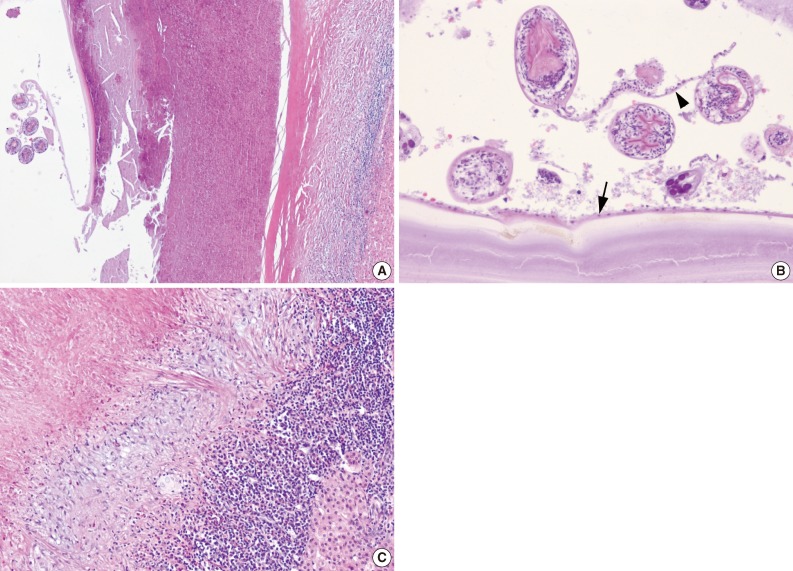
Fig. 1 Abdomen computed tomography scan. A cystic mass with internal septation is present in the right hepatic lobe.
Fig. 2 Cytologic findings. (A) There are many protoscolices in the shape of a mushroom. The necrotic debris is seen in the background. (B, C) Higher magnification of the protoscolices reveals hooklets. (D) Isolated refractile hooklets (arrows) are present. (E) Fragments of a laminated membrane are present.
Fig. 3 Gross finding. The hepatic cyst contains multiple daughter cysts.
Fig. 4 Histologic findings. (A) A hydatid cyst and adjacent liver parenchyma are seen. (B) The cyst wall is composed of an acellular laminated membrane and an inner nucleated germinal layer (arrow). Protoscolices and brood capsule (arrowhead) are present. (C) The liver shows a fibrinous wall and inflammatory cells infiltration, including lymphocytes, eosinophils, and histiocytes.
Fig. 1
Fig. 2
Fig. 3
Fig. 4
Fine Needle Aspiration Cytology of Hepatic Hydatid Cyst: A Case Study

 E-submission
E-submission