Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 51(5); 2017 > Article
-
Brief Case Report
Iatrogenic Gastric Pseudolipomatosis during Endoscopic Submucosal Dissection - Sang Wook Kim, Woo Sung Moon1
-
Journal of Pathology and Translational Medicine 2017;51(5):513-515.
DOI: https://doi.org/10.4132/jptm.2017.04.25
Published online: July 31, 2017
Division of Gastroenterology, Department of Internal Medicine, Research Institute of Clinical Medicine of Chonbuk National University-Biomedical Research Institute of Chonbuk National University Hospital and Research Institute for Endocrine Sciences, Chonbuk National University Medical School, Jeonju, Korea
1Department of Pathology, Research Institute of Clinical Medicine of Chonbuk National University-Biomedical Research Institute of Chonbuk National University Hospital and Research Institute for Endocrine Sciences, Chonbuk National University Medical School, Jeonju, Korea
- Corresponding Author Woo Sung Moon, MD, PhD Department of Pathology, Chonbuk National University Medical School, 567 Baekje-daero, Deokjin-gu, Jeonju 54896, Korea Tel: +82-63-270-3086, Fax: +82-63-270-3135, E-mail: mws@chonbuk.ac.kr
© 2017 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- The patient had provided written informed consent for publication of this case study.
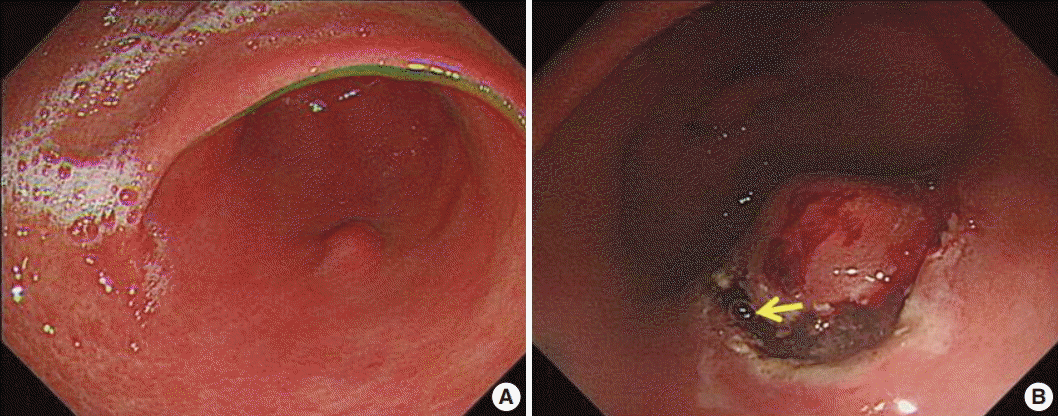
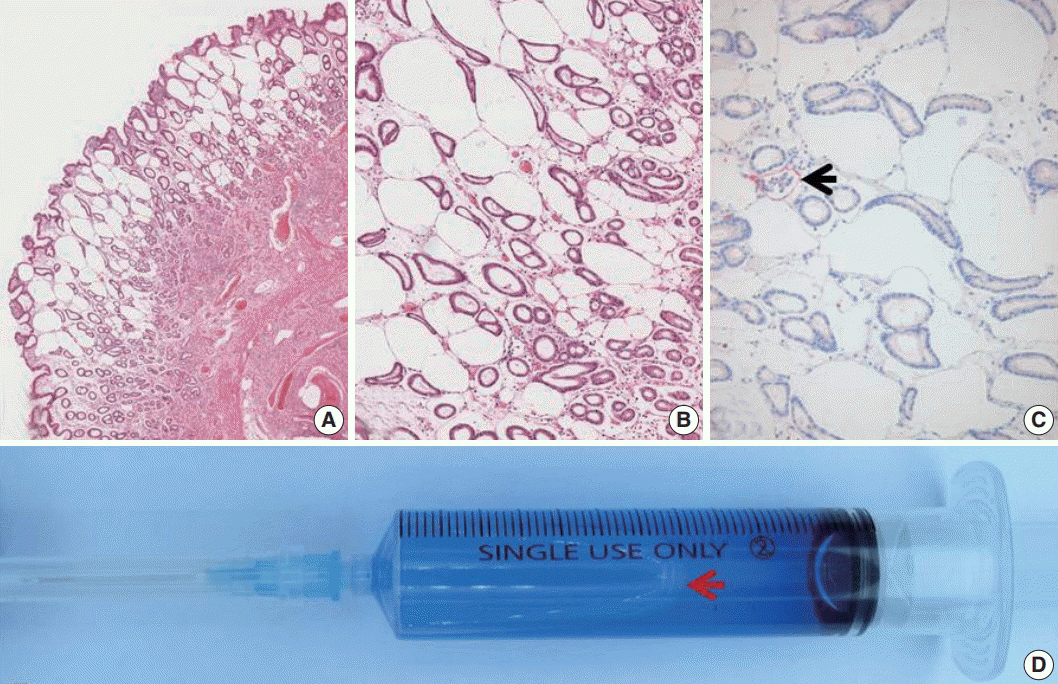
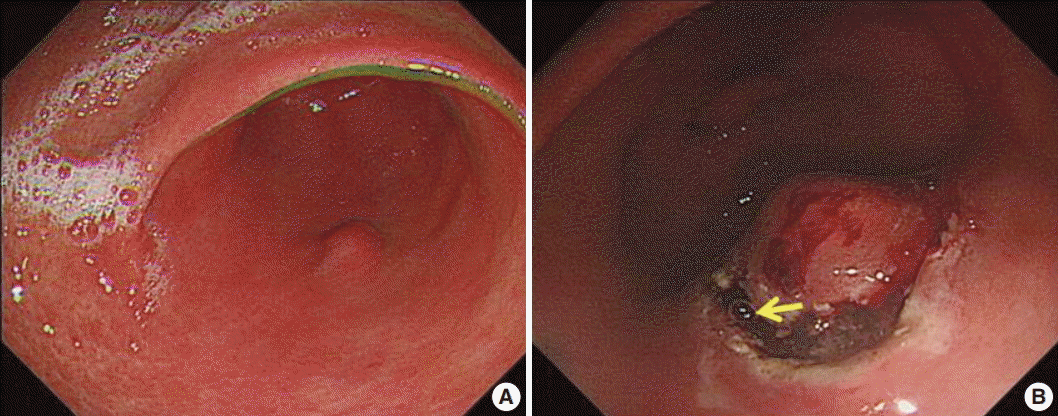
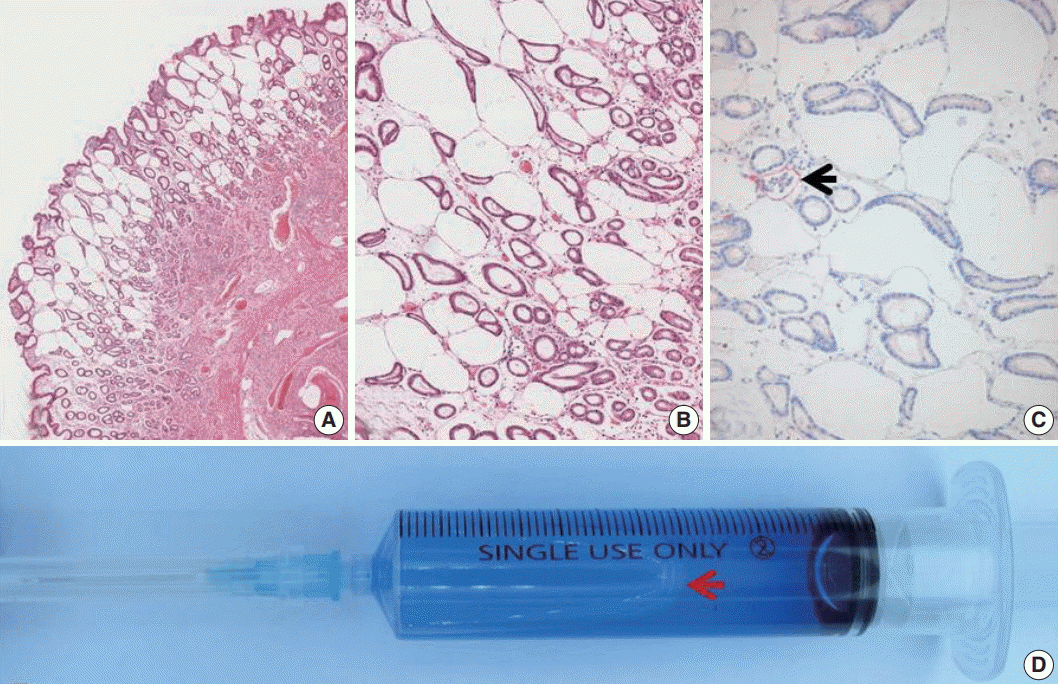
- A 63-year-old woman was admitted for evaluating gastric submucosal lesion incidentally detected during a health check-up. Upon endoscopic examination, a single smooth surfaced polypoid lesion sized 1 cm was identified. Under the clinical impression of submucosal benign mesenchymal tumor, ESD was performed. Normal saline and indigo carmine dye mixed with hyaluronic acid was injected into the submucosal layer to lift up the lesion and distinguish the muscle layer from the submucosal layer. The endoscopist did not detect any visible mucosal changes before injecting the solution (Fig. 1A). However, the release of air bubbles from the lesion was clearly observed during the submucosal dissection (Fig. 1B). Microscopic examination of the submucosal tumor was consistent with inflammatory fibroid polyp. The lamina propria contained numerous unlined empty spaces without inflammatory reaction, measuring 40–600 μm in diameter and extending to the submucosa and submucosal tumor (Fig. 2A, B). Neither specific cytological abnormalities nor architectural destruction was found in the mucosa. Helicobacter pylori was not identified. The lesion showed negative immunohistochemical staining results for D2-40, CD31, CD34, vimentin, and S100 protein. Therefore, lymphangiomatous lesion and lipomatous metaplasia were ruled out (Fig. 2C). These histologic findings were similar, if not identical, to those of gastrointestinal pseudolipomatosis reported previously [1,2]. Based on histological and immunohistochemical findings, a final diagnosis of gastric pseudolipomatosis was made.
CASE REPORT
- Gastrointestinal pseudolipomatosis is characterized by the presence of gas-filled vacuoles of various sizes within the lamina propria. It is named as gastrointestinal pseudolipomatosis because it resembles fatty infiltration [1,2]. Histologically, differential diagnoses of pseudolipomatosis include lymphangiomatous lesion and lipomatous metaplasia which can be easily excluded by using appropriate immunohistochemical staining. The etiology of pseudolipomatosis is unclear. Penetration of gas into the injured mucosa associated with air pressure during endoscopy [1], H. pylori infection [3], and the use of disinfectant hydrogen peroxide solution have been proposed as possible etiologies [4]. We propose that our case is an artifact caused by infusion of incompletely removed air inside the syringe caused by inadequate flushing when injecting the submucosal solution (Fig. 2D). Several facts support this notion. First, there were no apparent etiologic factors in our case. There was no mucosal lesion such as atrophy or ulcer. In addition, H. pylori was not identified. Hydrogen peroxide was not used either. Second, there was no inflammatory or fibroblastic reaction in the vicinity of unlined empty spaces, suggesting short duration of this lesion. Third, the endoscopist noted incompletely removed air in the syringe containing submucosal solution and observed air bubbles being released from the gastric tissue during submucosal dissection. This lesion may represent a gastric pseudolipomatosis with an undescribed unique iatrogenic artifact while performing injection of submucosal solution during ESD procedure. Recognition of this iatrogenic artifact is important to endoscopists and pathologists because it is preventable. In addition, it might mimic other lesions, such as mucosal lymphangioma or lipomatous metaplasia.
DISCUSSION
Acknowledgments
- 1. Stebbing J, Wyatt JI. Gastric ‘pseudolipomatosis’. Histopathology 1998; 32: 283-4. ArticlePubMedPDF
- 2. Snover DC, Sandstad J, Hutton S. Mucosal pseudolipomatosis of the colon. Am J Clin Pathol 1985; 84: 575-80. ArticlePubMedPDF
- 3. Alper M, Akcan Y, Belenli OK, Cukur S, Aksoy KA, Suna M. Gastric pseudolipomatosis, usual or unusual? Re-evaluation of 909 endoscopic gastric biopsies. World J Gastroenterol 2003; 9: 2846-8. ArticlePubMedPMC
- 4. Jonas G, Mahoney A, Murray J, Gertler S. Chemical colitis due to endoscope cleaning solutions: a mimic of pseudomembranous colitis. Gastroenterology 1988; 95: 1403-8. ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- A Rare Case Report of Colonic Pseudolipomatosis with Distinct Endoscopic and Histological Features
Qi Zhao, Hai-Tao Yu, Qun-Ying Wang, Wei Zhang, Wen-Zhu Dong
Case Reports in Gastroenterology.2025; 19(1): 127. CrossRef - Endoscope disinfectant-induced colonic pseudolipomatosis: case series of a rare condition
Charfeddine Baccouche, Myriam Ayari, Imen Abdelaali, Amen Dhaoui, Taieb Jomni, Mohamed Hedi Douggui
Future Science OA.2024;[Epub] CrossRef - Unusual mucosal lesion: A case of rectal pseudolipomatosis in a 60-year-old patient
Boubacar Efared, Balandougou Sylla, Nawal Hammas, Hinde El Fatemi, Laila Chbani
SAGE Open Medical Case Reports.2019;[Epub] CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure

 E-submission
E-submission




