Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 50(1); 2016 > Article
-
Original Article
Immunohistochemical Expression and Clinical Significance of Suggested Stem Cell Markers in Hepatocellular Carcinoma - Jong Jin Sung, Sang Jae Noh, Jun Sang Bae, Ho Sung Park, Kyu Yun Jang, Myoung Ja Chung, Woo Sung Moon
-
Journal of Pathology and Translational Medicine 2016;50(1):52-57.
DOI: https://doi.org/10.4132/jptm.2015.10.09
Published online: November 18, 2015
Department of Pathology, Research Institute of Clinical Medicine of Chonbuk National University, Biomedical Research Institute of Chonbuk National University Hospital and Research Institute for Endocrine Sciences, Chonbuk National University Medical School, Jeonju, Korea
- Corresponding Author: Woo Sung Moon, MD, PhD Department of Pathology, Chonbuk National University Medical School, 567 Baekje-daero, Deokjin-gu, Jeonju 54896, Korea Tel: +82-63-270-3086 Fax: +82-63-270-3135 E-mail: mws@chonbuk.ac.kr
© 2016 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background:
- Increasing evidence has shown that tumor initiation and growth are nourished by a small subpopulation of cancer stem cells (CSCs) within the tumor mass. CSCs are posited to be responsible for tumor maintenance, growth, distant metastasis, and relapse after curative operation. We examined the expression of CSC markers in paraffin-embedded tissue sections of hepatocellular carcinoma (HCC) and correlated the results with clinicopathologic characteristics.
-
Methods:
- Immunohistochemical staining for the markers believed to be expressed in the CSCs, including epithelial cell adhesion molecule (EpCAM), keratin 19 (K19), CD133, and CD56, was performed in 82 HCC specimens.
-
Results:
- EpCAM expression was observed in 56% of the HCCs (46/82) and K19 in 6% (5/82). EpCAM expression in HCC significantly correlated with elevated α-fetoprotein level, microvessel invasion of tumor cells, and high histologic grade. In addition, EpCAM expression significantly correlated with K19 expression. The overall survival and relapsefree survival rates in patients with EpCAM-expressing HCC were relatively lower than those in patients with EpCAM-negative HCC. All but two of the 82 HCCs were negative for CD133 and CD56, respectively.
-
Conclusions:
- Our results suggest that HCCs expressing EpCAM are associated with unfavorable prognostic factors and have a more aggressive clinical course than those not expressing EpCAM. Further, the expression of either CD133 or CD56 in paraffin-embedded HCC tissues appears to be rare.
- Patients and specimens
- This study was approved by the Institutional Review Board (IRB) of Chonbuk National University Hospital. Informed consent was obtained from all patients who underwent surgery according to the Helsinki Declaration. To examine the location and expression of four suggested CSC markers, we collected 91 surgical specimens of formalin-fixed, paraffin-embedded HCCs resected in the Department of Pathology, Chonbuk National University Hospital, between January 2011 and December 2013. Among these patients, nine underwent transarterial chemoembolization, which resulted in near total necrosis of the tissue. The remaining 82 patients were analyzed in our study. In each case, clinicopathologic findings, including age, gender, etiology, background liver disease, ascites, serological data including serum albumin level and α-fetoprotein (AFP) level, microvessel invasion, intrahepatic metastasis, histologic grade, and follow-up data, were obtained from hospital records. Tumors were staged according to the criteria of the 2010 American Joint Committee on Cancer (AJCC) TNM classification [12]. Follow-up period was defined as the period from the date of initial surgery to the date of either last follow-up or death.
- Immunohistochemistry
- For immunohistochemical (IHC) staining, 10% formalin-fixed, paraffin-embedded tissue sections of representative areas of tumor were prepared into 4-μm-thick tissue samples. IHC staining was performed using a fully automated IHC system with the Bond Polymer Refine Detection Kit (Leica Bond, Newcastle upon Tyne, UK) according to the manufacturer’s instructions. The sources of antibodies used in this study and conditions of the procedure are listed in Table 1. Peroxidase activity was detected with the enzyme substrate 3-amino-9-ethyl carbazole. The immunoreactivity of the specimens was interpreted according to the intensity of staining and proportion of positive cells. The intensity of cytoplasmic and membranous staining was graded into four levels: no immunostaining (0), weak (1), moderate (2), and intense (3). The proportion of positive cells was scored as follows: 0 (none), 1 (1%), 2 (2%–10%), 3 (11%–33%), 4 (34%–66%), and 5 (67%–100%). The sum index was obtained by totaling the scores of intensity and proportion of staining. If the final score was equal to or greater than 4, the immunoreactivity was considered positive; otherwise, the immunoreactivity was considered negative. For negative controls, sections were treated in the same way, except that they were incubated with Tris-buffered saline instead of primary antibodies.
- Statistical analysis
- SPSS ver. 15.0 software (SPSS Inc., Chicago, IL, USA) was used for statistical analysis. Associations between the clinicopathological factors and expression of antibodies were tested using a chi-square test. Univariate and multivariate Cox proportional regression analyses for overall survival and relapse-free survival were performed. A p-value of <.05 was considered statistically significant.
MATERIALS AND METHODS
- Clinical features
- The 82 patients included 72 males and 10 females with a mean age of 57 years (range, 26 to 77 years). HCC formation was attributed to the presence of hepatitis B virus (HBV) surface antigen in 64 patients, alcohol-related complication in seven patients, presence of anti–hepatitis C virus antibody in four patients, and unknown etiology in seven patients. The surrounding liver tissue showed cirrhosis in 56% of the patients (46/82) and chronic hepatitis with varying degrees of fibrosis in the remaining 44% of the patients (36/82).
- Expression of suggested CSC markers
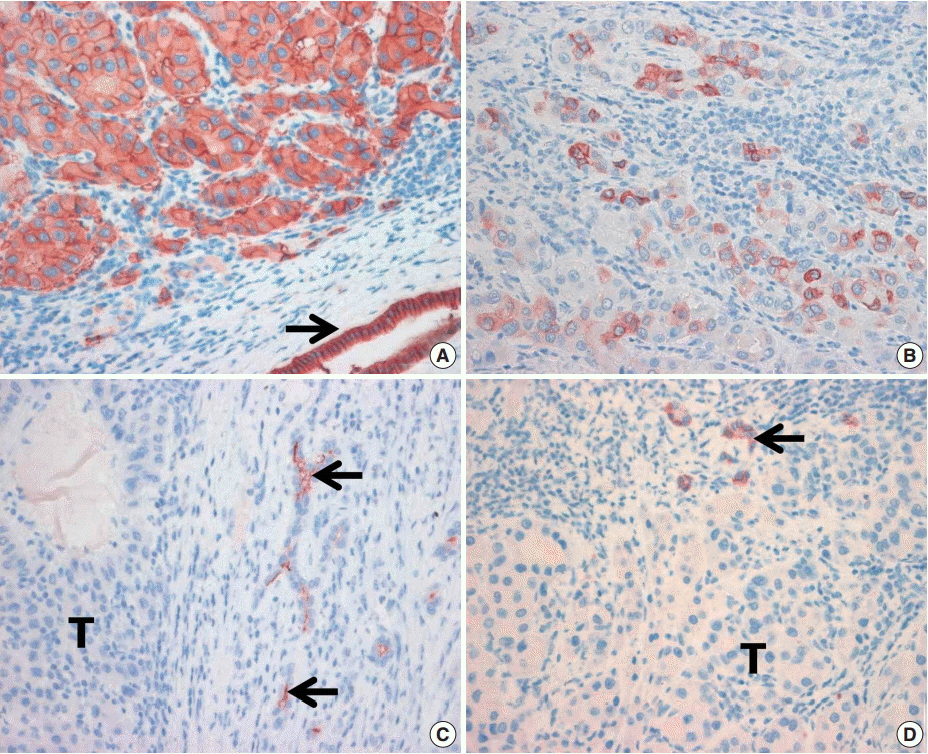
- In cirrhotic livers, all four examined markers showed intense immunoreactivity in proliferating reactive bile ductules. These ductules are thought to originate from hepatic progenitor cells and thus were considered as an internal positive control. EpCAM expression in HCC tissues showed intense cytoplasmic and/or membranous staining (Fig. 1). In 82 HCC samples, 46 were EpCAM-positive (56%) and five were K19-positive (6%). Of the 82 HCCs, only two cases showed CD133 and CD56 expression, respectively.
- Correlations between expression of suggested CSC markers and clinicopathological features
- Analysis of the relationships between expression of K19, CD133, and CD56 and clinicopathologic features was not meaningful, since the number of cases with K19, CD133, and CD56 expression was very small. However, EpCAM expression significantly correlated with higher histologic grade (p=.006), elevated AFP level (p=.001), and microvessel invasion of the tumor cells (p=.030) (Table 2). Additionally, EpCAM expression was strongly associated with K19 expression (p=.041).
- Outcome
- In 82 patients with HCC, follow-up intervals ranged from 0.1 to 69 months (mean of 23 months). Eleven patients died, and 16 showed local recurrence or latent distant metastasis. The mean overall survival time of patients with EpCAM-expressing HCC was 57.2±3.7 months, while that of EpCAM-negative HCC was 62.0±2.9 months. The mean relapse-free survival time of patients with EpCAM-expressing HCC was 40.5±5.9 months, while that of patients with EpCAM-negative HCC was 53.8±5.0 months. However, these results were not statistically significant. In univariate Cox regression analysis, T category significantly correlated with poor patient overall survival (p=.003). Additionally, T category, preoperative serum AFP level, and vascular invasion were associated with decreased relapse-free survival (p=.019, p=.048, and p=.011, respectively). Multivariate analysis revealed that T category and vascular invasion were independent indicators of relapse (p=.011 and p=.007, respectively).
RESULTS
- Carcinogenesis is currently explained using two models, one involving a traditional stochastic onset and a second based on the role of CSCs. According to the CSC model, only a small population of tumor cells has the ability to divide and repopulate within the tumor [7,13]. CSCs are responsible for tumor initiation, maintenance, growth, metastasis, and relapse after therapy [3-6]. The expression of several proposed CSC markers in HCC has been reported and might prove to be useful for predicting the prognosis of HCC patients [11,14-16]. However, little is known about the relationships between the IHC expression of CSC markers in paraffin-embedded tissue sections and clinicopathologic factors or clinical outcomes of HCC.
- EpCAM is a transmembrane intercellular protein that was initially posed as a homophilic cell adhesion molecule [17] and is highly up-regulated in most human epithelial cancers, including HCC [14-16,18]. EpCAM has been validated as a marker of stem cells in the liver, and EpCAM-positive HCC is likely to have originated from hepatic stem cells [8,15,16,19]. In the present study, we observed that EpCAM expression significantly correlated with tumor progression factors of HCC, such as elevated AFP level, vascular invasion, and high tumor grade. These findings are in agreement with previous studies showing that expression level of EpCAM correlates with de-differentiation [11] and vascular invasion and is associated with the high AFP level in HCC [20,21]. The prognosis of patients with EpCAM-negative HCC is considered to be better than that of those with EpCAM-positive HCC [11,14-16,20,21]. Although EpCAM expression was not found to be an independent predictor of survival in patients with HCC in this study, EpCAM expression was found to be associated with well-known unfavorable prognostic factors in HCC. Thus, the use of EpCAM expression as an unfavorable prognostic factor of HCC is reasonable. Furthermore, gene expression profile study has demonstrated that EpCAM-positive and AFP-positive HCCs have more aggressive behavior and poor clinical outcome, whereas EpCAM-negative and AFP-negative HCCs have good prognosis [20]. Based on these observations, EpCAM has attracted considerable attention as a possible therapeutic target for patients with HCC [7,8,13]. Taken together, our findings suggest that EpCAM is a critical player in facilitating vascular invasion of tumor cells, leading to de-differentiation in HCC with high serum AFP level, and might be useful for predicting the prognosis of HCC patients. In this study, a proportion of HCCs (56%) expressed EpCAM, and EpCAM expression was associated with K19 expression. These findings are in agreement with previous reports showing that the expression of EpCAM and K19 was positively correlated [15,21]. The proportion of tissues expressing EpCAM in this study was a little higher than in earlier series, which reported EpCAM in 15.9%–48.7% of HCCs [15-17,20-23]. Kimura et al. [23] have demonstrated that EpCAM expression was observed more often in HCC patients with HBV than in those with other etiologies, and the immunoreactivity of EpCAM has been found in up to 78% of HCC patients with HBV. The high proportion of HCC patients with HBV (74%) examined in this study might be a possible explanation for the higher EpCAM-positive rate. It has been hypothesized that the transformation of hepatic stem/progenitor cells (maturation arrest theory) underlies the occurrence of HCC expressing CSC markers. However, the concept of the CSC model is still debated. The expression of CSC markers in HCC can develop as an acquisition of progenitor cell features during the de-differentiation of cancer cells (de-differentiation theory) [5,15]. Kim and Park [24] have proposed that HCC expressing CSC markers should be designated as “HCC with stemness-related marker expression” in order to avoid the implication that these HCCs originated from hepatic stem/progenitor cells.
- Either CD133 or CD56 expression in this study was rare. Only two of 82 HCC specimens showed positive staining for CD133 and CD56, suggesting that CD133 and CD56 expression is rare in paraffin-embedded HCC tissues. It has been reported that 0%–88% [11,15,16,25] of human HCC tissue samples express CD133, and the expression of which is negatively correlated with presence of HBV [26]. Several IHC studies have demonstrated CD56 expression in 0%–9.7% of human HCCs [11,25,27,28]. The reason for this high discrepancy of positive rate of CD133 and CD56 in HCC is unclear. In our study, we employed the bond polymer IHC staining method to avoid endogenous biotin contamination, and all four examined markers always showed strong immunoreactivity in reactive bile ductules, which were considered as internal positive controls. The discrepancy in the expression rates of CD133 and CD56 is not easily explained but might be related to the different criteria for positivity, the quality of tissue samples analyzed, and the unique antibodies and immunostaining methods used in different studies. Our negative results in analysis of CD133 and CD56 through the use of specific antibodies in an established automated IHC system does not exclude the presence of these markers and can be linked to the different etiologies according to geographic background. Additional investigations with a larger population of HCC and strict criteria for positive immunoreactivity are necessary to determine the expression and clinical implication of these markers.
- In conclusion, we showed that the EpCAM expression in paraffin-embedded tissue sections of HCC is associated with tumor progression factors and might be useful for predicting the prognosis of HCC patients. The high proportion of EpCAM expression in HCCs and its associations with unfavorable prognostic factors of HCC provide a basis for further investigation of anti-EpCAM–targeted therapy.
DISCUSSION
Acknowledgments
- 1. Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin 2015; 65: 87-108. ArticlePubMedPDF
- 2. El-Serag HB, Marrero JA, Rudolph L, Reddy KR. Diagnosis and treatment of hepatocellular carcinoma. Gastroenterology 2008; 134: 1752-63. ArticlePubMed
- 3. Visvader JE. Cells of origin in cancer. Nature 2011; 469: 314-22. ArticlePubMedPDF
- 4. Clarke MF, Dick JE, Dirks PB, et al. Cancer stem cells: perspectives on current status and future directions: AACR Workshop on cancer stem cells. Cancer Res 2006; 66: 9339-44. ArticlePubMedPDF
- 5. Bomken S, Fiser K, Heidenreich O, Vormoor J. Understanding the cancer stem cell. Br J Cancer 2010; 103: 439-45. ArticlePubMedPMCPDF
- 6. Bjerkvig R, Tysnes BB, Aboody KS, Najbauer J, Terzis AJ. Opinion: the origin of the cancer stem cell: current controversies and new insights. Nat Rev Cancer 2005; 5: 899-904. ArticlePubMedPDF
- 7. Marquardt JU, Factor VM, Thorgeirsson SS. Epigenetic regulation of cancer stem cells in liver cancer: current concepts and clinical implications. J Hepatol 2010; 53: 568-77. ArticlePubMedPMC
- 8. Yamashita T, Ji J, Budhu A, et al. EpCAM-positive hepatocellular carcinoma cells are tumor-initiating cells with stem/progenitor cell features. Gastroenterology 2009; 136: 1012-24. ArticlePubMedPMC
- 9. Durnez A, Verslype C, Nevens F, et al. The clinicopathological and prognostic relevance of cytokeratin 7 and 19 expression in hepatocellular carcinoma: a possible progenitor cell origin. Histopathology 2006; 49: 138-51. ArticlePubMed
- 10. Zhu Z, Hao X, Yan M, et al. Cancer stem/progenitor cells are highly enriched in CD133+CD44+ population in hepatocellular carcinoma. Int J Cancer 2010; 126: 2067-78. ArticlePubMed
- 11. Chan AW, Tong JH, Chan SL, Lai PB, To KF. Expression of stemness markers (CD133 and EpCAM) in prognostication of hepatocellular carcinoma. Histopathology 2014; 64: 935-50. ArticlePubMed
- 12. Edge SB, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A. AJCC cancer staging manual. 7th ed. New York: Springer, 2010.
- 13. Visvader JE, Lindeman GJ. Cancer stem cells: current status and evolving complexities. Cell Stem Cell 2012; 10: 717-28. ArticlePubMed
- 14. Yang XR, Xu Y, Yu B, et al. High expression levels of putative hepatic stem/progenitor cell biomarkers related to tumour angiogenesis and poor prognosis of hepatocellular carcinoma. Gut 2010; 59: 953-62. ArticlePubMed
- 15. Kim H, Choi GH, Na DC, et al. Human hepatocellular carcinomas with “Stemness”-related marker expression: keratin 19 expression and a poor prognosis. Hepatology 2011; 54: 1707-17. ArticlePubMed
- 16. Guo Z, Li LQ, Jiang JH, Ou C, Zeng LX, Xiang BD. Cancer stem cell markers correlate with early recurrence and survival in hepatocellular carcinoma. World J Gastroenterol 2014; 20: 2098-106. ArticlePubMedPMC
- 17. Litvinov SV, Balzar M, Winter MJ, et al. Epithelial cell adhesion molecule (Ep-CAM) modulates cell-cell interactions mediated by classic cadherins. J Cell Biol 1997; 139: 1337-48. ArticlePubMedPMCPDF
- 18. Went PT, Lugli A, Meier S, et al. Frequent EpCAM protein expression in human carcinomas. Hum Pathol 2004; 35: 122-8. ArticlePubMed
- 19. Breuhahn K, Baeuerle PA, Peters M, et al. Expression of epithelial cellular adhesion molecule (Ep-CAM) in chronic (necro-)inflammatory liver diseases and hepatocellular carcinoma. Hepatol Res 2006; 34: 50-6. ArticlePubMed
- 20. Yamashita T, Forgues M, Wang W, et al. EpCAM and alpha-fetoprotein expression defines novel prognostic subtypes of hepatocellular carcinoma. Cancer Res 2008; 68: 1451-61. PubMed
- 21. Govaere O, Komuta M, Berkers J, et al. Keratin 19: a key role player in the invasion of human hepatocellular carcinomas. Gut 2014; 63: 674-85. ArticlePubMedPMC
- 22. Shan YF, Huang YL, Xie YK, et al. Angiogenesis and clinicopathologic characteristics in different hepatocellular carcinoma subtypes defined by EpCAM and alpha-fetoprotein expression status. Med Oncol 2011; 28: 1012-6. ArticlePubMedPDF
- 23. Kimura O, Kondo Y, Kogure T, et al. Expression of EpCAM increases in the hepatitis B related and the treatment-resistant hepatocellular carcinoma. Biomed Res Int 2014; 2014: 172913.ArticlePubMedPMCPDF
- 24. Kim H, Park YN. Hepatocellular carcinomas expressing ‘stemness’-related markers: clinicopathological characteristics. Dig Dis 2014; 32: 778-85. ArticlePubMedPDF
- 25. Zen C, Zen Y, Mitry RR, et al. Mixed phenotype hepatocellular carcinoma after transarterial chemoembolization and liver transplantation. Liver Transpl 2011; 17: 943-54. ArticlePubMed
- 26. Yeh CT, Kuo CJ, Lai MW, et al. CD133-positive hepatocellular carcinoma in an area endemic for hepatitis B virus infection. BMC Cancer 2009; 9: 324.ArticlePubMedPMCPDF
- 27. Tsuchiya A, Kamimura H, Takamura M, et al. Clinicopathological analysis of CD133 and NCAM human hepatic stem/progenitor cells in damaged livers and hepatocellular carcinomas. Hepatol Res 2009; 39: 1080-90. ArticlePubMed
- 28. Tsuchiya A, Kamimura H, Tamura Y, et al. Hepatocellular carcinoma with progenitor cell features distinguishable by the hepatic stem/progenitor cell marker NCAM. Cancer Lett 2011; 309: 95-103. ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- Spatial immune scoring system predicts hepatocellular carcinoma recurrence
Gengjie Jia, Peiqi He, Tianli Dai, Denise Goh, Jiabei Wang, Mengyuan Sun, Felicia Wee, Fuling Li, Jeffrey Chun Tatt Lim, Shuxia Hao, Yao Liu, Tony Kiat Hon Lim, Nye-Thane Ngo, Qingping Tao, Wei Wang, Ahitsham Umar, Björn Nashan, Yongchang Zhang, Chen Ding
Nature.2025; 640(8060): 1031. CrossRef - Evolving Landscape of Systemic Therapy for Hepatocellular Carcinoma in 2025
Karan Kumar, Vivek A. Saraswat
Journal of Clinical and Experimental Hepatology.2025; 15(5): 102547. CrossRef - Recent Progress in Systemic Therapy for Advanced Hepatocellular Carcinoma
Narayanan Sadagopan, Aiwu Ruth He
International Journal of Molecular Sciences.2024; 25(2): 1259. CrossRef - Diagnostic value of expressions of cancer stem cell markers for adverse outcomes of hepatocellular carcinoma and their associations with prognosis: A Bayesian network meta‑analysis
Zhengrong Ou, Shoushuo Fu, Jian Yi, Jingxuan Huang, Weidong Zhu
Oncology Letters.2024;[Epub] CrossRef - Clinicopathological and prognostic value of epithelial cell adhesion molecule in solid tumours: a meta-analysis
Peiwen Ding, Panyu Chen, Jiqi Ouyang, Qiang Li, Shijie Li
Frontiers in Oncology.2023;[Epub] CrossRef - PD-L1 Downregulation and DNA Methylation Inhibition for Molecular Therapy against Cancer Stem Cells in Hepatocellular Carcinoma
Caecilia Sukowati, Loraine Kay D. Cabral, Beatrice Anfuso, Francesco Dituri, Roberto Negro, Gianluigi Giannelli, Claudio Tiribelli
International Journal of Molecular Sciences.2023; 24(17): 13357. CrossRef - EpCAM, Ki67, and ESM1 Predict Hepatocellular Carcinoma Recurrence After Liver Transplantation
Aiat Shaban Hemida, Doha Maher Taie, Moshira Mohamed Abd El-Wahed, Mohammed Ibrahim Shabaan, Mona Saeed Tantawy, Nermine Ahmed Ehsan
Applied Immunohistochemistry & Molecular Morphology.2023; 31(9): 596. CrossRef - The clinical, prognostic and therapeutic significance of liver cancer stem cells and their markers
Izabela Zarębska, Arkadiusz Gzil, Justyna Durślewicz, Damian Jaworski, Paulina Antosik, Navid Ahmadi, Marta Smolińska-Świtała, Dariusz Grzanka, Łukasz Szylberg
Clinics and Research in Hepatology and Gastroenterology.2021; 45(3): 101664. CrossRef - Detection of oncogenic mutations in paired circulating tumor DNA and circulating tumor cells in patients with hepatocellular carcinoma
Zhouhong Ge, Jean C.A. Helmijr, Maurice P.H.M. Jansen, Patrick P.C. Boor, Lisanne Noordam, Maikel Peppelenbosch, Jaap Kwekkeboom, Jaco Kraan, Dave Sprengers
Translational Oncology.2021; 14(7): 101073. CrossRef - Hepatocellular Carcinoma Score and Subclassification Into Aggressive Subtypes Using Immunohistochemical Expression of p53, β-Catenin, CD133, and Ki-67
Asmaa G. Abdou, Nanis S. Holah, Dina S. Elazab, Walaa G. El-Gendy, Mohammed T. Badr, Dalia R. Al-Sharaky
Applied Immunohistochemistry & Molecular Morphology.2021; 29(1): 20. CrossRef - The prognostic significance of neuroendocrine markers and somatostatin receptor 2 in hepatocellular carcinoma
Keigo Murakami, Hiroyuki Kumata, Shigehito Miyagi, Takashi Kamei, Hironobu Sasano
Pathology International.2021; 71(10): 682. CrossRef - Predictors of recurrence and survival of hepatocellular carcinoma: A prospective study including transient elastography and cancer stem cell markers
Hend Ibrahim Shousha, Rabab Fouad, Tamer Mahmoud Elbaz, Dina Sabry, Mohamed Mahmoud Nabeel, Ahmed Hosni Abdelmaksoud, Aisha Mahmoud Elsharkawy, Zeinab Abdellatif Soliman, Ghada Habib, Ashraf Omar Abdelaziz
Arab Journal of Gastroenterology.2020; 21(2): 95. CrossRef - Napabucasin Reduces Cancer Stem Cell Characteristics in Hepatocellular Carcinoma
Ya Li, Qiuju Han, Huajun Zhao, Quanjuan Guo, Jian Zhang
Frontiers in Pharmacology.2020;[Epub] CrossRef - The mRNA Distribution of Cancer Stem Cell Marker CD90/Thy-1 Is Comparable in Hepatocellular Carcinoma of Eastern and Western Populations
An B. Luong, Huy Q. Do, Paola Tarchi, Deborah Bonazza, Cristina Bottin, Loraine Kay D. Cabral, Long D. C. Tran, Thao P. T. Doan, Lory S. Crocè, Hoa L. T. Pham, Claudio Tiribelli, Caecilia H. C. Sukowati
Cells.2020; 9(12): 2672. CrossRef - Histological architectural classification determines recurrence pattern and prognosis after curative hepatectomy in patients with hepatocellular carcinoma
Hirohisa Okabe, Tomoharu Yoshizumi, Yo-ichi Yamashita, Katsunori Imai, Hiromitsu Hayashi, Shigeki Nakagawa, Shinji Itoh, Norifumi Harimoto, Toru Ikegami, Hideaki Uchiyama, Toru Beppu, Shinichi Aishima, Ken Shirabe, Hideo Baba, Yoshihiko Maehara, Motoyuki
PLOS ONE.2018; 13(9): e0203856. CrossRef - Overexpression of epithelial cell adhesion molecule as a predictor of poor outcome in patients with hepatocellular carcinoma
Chih‑Jan Ko, Chia‑Jung Li, Meng‑Yu Wu, Pei‑Yi Chu
Experimental and Therapeutic Medicine.2018;[Epub] CrossRef - Clinicopathologic Significance of Survivin Expression in Relation to CD133 Expression in Surgically Resected Stage II or III Colorectal Cancer
Wanlu Li, Mi-Ra Lee, EunHee Choi, Mee-Yon Cho
Journal of Pathology and Translational Medicine.2017; 51(1): 17. CrossRef - PIN1 in hepatocellular carcinoma is associated with TP53 gene status
Jun Sang Bae, Sang Jae Noh, Kyoung Min Kim, Kyu Yun Jang, Ho Sung Park, Myoung Ja Chung, Byung-Hyun Park, Woo Sung Moon
Oncology Reports.2016; 36(4): 2405. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
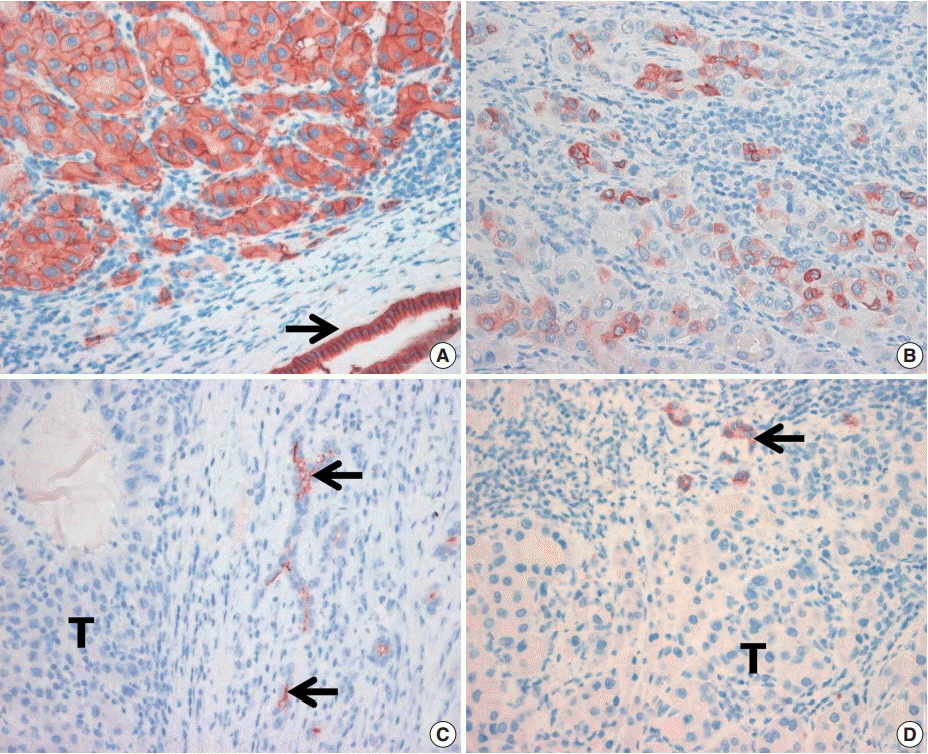
Fig. 1.
| Antibody | Clone | Source | Dilution | Antigen retrieval | Antibody incubation |
|---|---|---|---|---|---|
| EpCAM | VU-1D9 | Calbiochem | 1:500 | BOND ER solution I (pH 6.0), 100°C, 20 min | Room temperature, 20 min |
| K19 | BA17 | DakoCytomation | 1:100 | BOND ER solution I (pH 6.0), 100°C, 20 min | Room temperature, 20 min |
| CD133 | AC133 | Miltenyi Biotec | 1:50 | BOND ER solution II (pH 9.0), 100°C, 20 min | Room temperature, 20 min |
| CD56 | 123C3 | Zymed Laboratories | 1:400 | BOND ER solution II (pH 9.0), 100°C, 20 min | Room temperature, 20 min |
| Characteristic | No. | EpCAM |
|||
|---|---|---|---|---|---|
| Positive | Negative | p-value | |||
| Age (yr) | < 60 | 49 | 30 | 19 | .254 |
| ≥ 60 | 33 | 16 | 17 | ||
| Sex | Female | 10 | 7 | 3 | .344 |
| Male | 72 | 39 | 33 | ||
| AFP (ng/mL) | < 100 | 58 | 26 | 32 | .001 |
| ≥ 100 | 24 | 20 | 4 | ||
| Albumin (g/dL) | ≥ 3.5 | 79 | 45 | 34 | .418 |
| < 3.5 | 3 | 1 | 2 | ||
| PIVKA-II (mAU/mL) | < 50 | 26 | 25 | 1 | .798 |
| ≥ 50 | 44 | 24 | 20 | ||
| T category | I | 34 | 16 | 18 | .230 |
| II | 36 | 24 | 12 | ||
| III and IV | 12 | 6 | 6 | ||
| Cirrhosis | Absence | 36 | 24 | 12 | .088 |
| Presence | 46 | 22 | 24 | ||
| Etiology | Non-viral | 14 | 7 | 7 | .614 |
| Viral | 68 | 39 | 29 | ||
| Microvessel invasion | Absence | 39 | 17 | 22 | .030 |
| Presence | 43 | 29 | 14 | ||
| Intrahepatic metastasis | Absence | 67 | 36 | 31 | .362 |
| Presence | 15 | 10 | 5 | ||
| Ascites | Absence | 75 | 44 | 31 | .125 |
| Presence | 7 | 2 | 5 | ||
| Histologic grade | 1 and 2 | 50 | 22 | 28 | .006 |
| 3 and 4 | 32 | 24 | 8 | ||
| K19 | Negative | 77 | 41 | 36 | .041 |
| Positive | 5 | 5 | 0 | ||
EpCAM, epithelial cell adhesion molecule; K19, keratin 19.
EpCAM, epithelial cell adhesion molecule; AFP, α-fetoprotein; PIVKA-II, protein induced by vitamin K absence/antagonist-II; K19, keratin 19.

 E-submission
E-submission



