Search
- Page Path
- HOME > Search
Review
- Inflammatory bowel disease–associated intestinal fibrosis
- Ji Min Park, Jeongseok Kim, Yoo Jin Lee, Sung Uk Bae, Hye Won Lee
- J Pathol Transl Med. 2023;57(1):60-66. Published online January 10, 2023
- DOI: https://doi.org/10.4132/jptm.2022.11.02
- 21,638 View
- 474 Download
- 35 Web of Science
- 37 Crossref
-
 Abstract
Abstract
 PDF
PDF - Fibrosis is characterized by a proliferation of fibroblasts and excessive extracellular matrix following chronic inflammation, and this replacement of organ tissue with fibrotic tissue causes a loss of function. Inflammatory bowel disease (IBD) is a chronic inflammation of the gastrointestinal tract, and intestinal fibrosis is common in IBD patients, resulting in several complications that require surgery, such as a stricture or penetration. This review describes the pathogenesis and various factors involved in intestinal fibrosis in IBD, including cytokines, growth factors, epithelial-mesenchymal and endothelial-mesenchymal transitions, and gut microbiota. Furthermore, histopathologic findings and scoring systems used for stenosis in IBD are discussed, and differences in the fibrosis patterns of ulcerative colitis and Crohn’s disease are compared. Biomarkers and therapeutic agents targeting intestinal fibrosis are briefly mentioned at the end.
-
Citations
Citations to this article as recorded by- Short-Chain Fatty Acids Elicit Differential Expression of Growth Factors and Pro-Inflammatory Cytokines in Immortalized Rat Enteric Glial Cells
Michelle M. Beltran, Danielle M. Defries
Nutrients.2026; 18(3): 436. CrossRef - A Developmental Perspective on the Intestinal Microbiota in Crohn’s Disease
Marcello Imbrizi, Daniela Oliveira Magro, Andrey Santos, Heloisa Balan Assalin, Dioze Guadagnini, Mario José Abdalla Saad, Claudio Saddy Rodrigues Coy
International Journal of Molecular Sciences.2026; 27(5): 2144. CrossRef - IL1β+ macrophages promote intestinal fibrosis in Crohn’s disease by secreting AREG to activate PI16+ fibroblasts
Hanlin Xie, Xiaofeng Wen, Tao Ma, Lin Wang, Yanxu Guo, Guanzhan Liang, Jing Chen, Ruibing Li, Yuxi Pan, Zhenyu Xian, Chuanyuan Liu, Yimamu Baihetiyaer, Abudumaimaitijiang Tuersun, Xiaowen He, Jia Ke, Chunbo He, Lei Lian, Abuduhalike Abulimiti, Tuo Hu, Tai
Journal of Translational Medicine.2026;[Epub] CrossRef - Leveraging Organ‐on‐Chip Models to Investigate Host–Microbiota Dynamics and Targeted Therapies for Inflammatory Bowel Disease
Tim Kaden, Raquel Alonso‐Román, Johannes Stallhofer, Mark S. Gresnigt, Bernhard Hube, Alexander S. Mosig
Advanced Healthcare Materials.2025;[Epub] CrossRef - Prominence of Microbiota to Predict Fibrous Stenosis in Crohn’s Disease
Xue Yang, Yan Pan, Cai-Ping Gao, Hang Li, Ying-Hui Zhang, Chun-Li Huang, Lu Cao, Shi-Yu Xiao, Zhou Zhou
Journal of Inflammation Research.2025; Volume 18: 1413. CrossRef - Fibrosierende Erkrankungen im Gastrointestinaltrakt
Elke Roeb
Die Innere Medizin.2025; 66(7): 695. CrossRef - Roles of fibroblasts in the pathogenesis of inflammatory bowel diseases and IBD-associated fibrosis
Takayoshi Ito, Hisako Kayama
International Immunology.2025; 37(7): 379. CrossRef - Disease Clearance in Ulcerative Colitis: A Narrative Review
Silvio Danese, Laurent Peyrin‐Biroulet, Vipul Jairath, Ferdinando D'Amico, Shashi Adsul, Christian Agboton, Fernando Magro
United European Gastroenterology Journal.2025; 13(6): 902. CrossRef - Gut Microbiota as a Mediator Between Intestinal Fibrosis and Creeping Fat in Crohn's Disease
Caiguang Liu, Rongchang Li, Jing Nie, Jinshen He, Zihao Lin, Xiaomin Wu, Jinyu Tan, Zishan Liu, Longyuan Zhou, Xiaozhi Li, Zhirong Zeng, Minhu Chen, Shixian Hu, Yijun Zhu, Ren Mao
United European Gastroenterology Journal.2025; 13(7): 1092. CrossRef - Per- and polyfluoroalkyl substances (PFAS): immunotoxicity at the primary sites of exposure
Emma Arnesdotter, Charlotte B. A. Stoffels, Wiebke Alker, Arno C. Gutleb, Tommaso Serchi
Critical Reviews in Toxicology.2025; 55(4): 484. CrossRef - Disease-Specific Novel Role of Growth Differentiation Factor 15 in Organ Fibrosis
Harshal Sawant, Alip Borthakur
International Journal of Molecular Sciences.2025; 26(12): 5713. CrossRef - Galectin-3—Insights from Inflammatory Bowel Disease and Primary Sclerosing Cholangitis
Thomas Grewal, Hauke Christian Tews, Christa Buechler
International Journal of Molecular Sciences.2025; 26(13): 6101. CrossRef - Revealing Fibrosis Genes as Biomarkers of Ulcerative Colitis: A Bioinformatics Study Based on ScRNA and Bulk RNA Datasets
Yandong Wang, Li Liu, Weihao Wang
Endocrine, Metabolic & Immune Disorders - Drug Targets.2025; 25(9): 710. CrossRef - Fibrosis in Immune-Mediated and Autoimmune Disorders
Magdalena Żurawek, Iwona Ziółkowska-Suchanek, Katarzyna Iżykowska
Journal of Clinical Medicine.2025; 14(18): 6636. CrossRef - Plasma-activated media inhibits epithelial-mesenchymal transition and ameliorates intestinal fibrosis through the PPARγ/TGF-β1/SMAD3 pathway
Yi You, Yaping Shen, Yan Yang, Xiaoyang Wei, Yuheng Zhou, Foxing Tan, Longcheng Deng, Haolin Du, Sen Wang, Cheng Wang, Yan Huang, Vinay Kumar,
PLOS One.2025; 20(10): e0335225. CrossRef - (R)-Bambuterol attenuates DSS-induced chronic colitis by suppressing inflammation, repairing intestinal barrier, and modulating gut microbiota and serum metabolomic profile
Liangjun Deng, Le Tian, Dan Su, Jiukun Xie, Yuer Qian, Yipeng Li, Shidong Zhang, Shanping Wang, Zhihua Liu
European Journal of Pharmacology.2025; 1008: 178346. CrossRef - Beyond inflammation: what drives the self-perpetuating cycle of fibrosis in IBD?
Yutong Wei, Zhou Zhou, Shiyu Xiao
Annals of Medicine.2025;[Epub] CrossRef - Neurokinin-1 Receptor Regulation of Fibroblast Phenotype and Function
Scott P. Levick
Receptors.2025; 4(4): 23. CrossRef - Tumor Development in Ulcerative Colitis: Perspectives From Biomechanical Characteristics
Hirotaka Tao
Development, Growth & Differentiation.2025; 67(9): 487. CrossRef - Effects of maternal overnutrition and metabolic challenge in adult life on the histological integrity of the liver and intestinal epithelium in rabbits
Lucía Carolina Cano, Erika Navarrete, Pedro Medina, Juan Pablo Ochoa-Romo, Georgina Díaz, Rodrigo Montúfar-Chaveznava, Rosa María Vigueras-Villaseñor, Ivette Caldelas
Frontiers in Nutrition.2025;[Epub] CrossRef - Minimally Invasive Full-Thickness Resection of a Non-Lifting Adenoma in an Ulcerative Colitis Patient Using OVESCO: A Case Report
Fei Yang Pan, Rupert Leong, Saurabh Gupta, Talia Fuchs, Viraj Kariyawasam
Case Reports in Gastroenterology.2025; 19(1): 682. CrossRef - Resistance to apoptosis in complicated Crohn's disease: Relevance in ileal fibrosis
M. Seco-Cervera, D. Ortiz-Masiá, D.C. Macias-Ceja, S. Coll, L. Gisbert-Ferrándiz, J. Cosín-Roger, C. Bauset, M. Ortega, B. Heras-Morán, F. Navarro-Vicente, M. Millán, J.V. Esplugues, S. Calatayud, M.D. Barrachina
Biochimica et Biophysica Acta (BBA) - Molecular Basis of Disease.2024; 1870(2): 166966. CrossRef - Characterization of patient-derived intestinal organoids for modelling fibrosis in Inflammatory Bowel Disease
Ilaria Laudadio, Claudia Carissimi, Noemi Scafa, Alex Bastianelli, Valerio Fulci, Alessandra Renzini, Giusy Russo, Salvatore Oliva, Roberta Vitali, Francesca Palone, Salvatore Cucchiara, Laura Stronati
Inflammation Research.2024; 73(8): 1359. CrossRef - Food additives impair gut microbiota from healthy individuals and IBD patients in a colonic in vitro fermentation model
Irma Gonza, Elizabeth Goya-Jorge, Caroline Douny, Samiha Boutaleb, Bernard Taminiau, Georges Daube, Marie–Louise Scippo, Edouard Louis, Véronique Delcenserie
Food Research International.2024; 182: 114157. CrossRef - Epigenetic Regulation of EMP/EMT-Dependent Fibrosis
Margherita Sisto, Sabrina Lisi
International Journal of Molecular Sciences.2024; 25(5): 2775. CrossRef - Mechanisms and therapeutic research progress in intestinal fibrosis
Yanjiang Liu, Tao Zhang, Kejian Pan, He Wei
Frontiers in Medicine.2024;[Epub] CrossRef - Disease clearance in ulcerative colitis: A new therapeutic target for the future
Syed Adeel Hassan, Neeraj Kapur, Fahad Sheikh, Anam Fahad, Somia Jamal
World Journal of Gastroenterology.2024; 30(13): 1801. CrossRef - Urinary Hydroxyproline as an Inflammation-Independent Biomarker of Inflammatory Bowel Disease
Muriel Huss, Tanja Elger, Johanna Loibl, Arne Kandulski, Benedicta Binder, Petra Stoeckert, Patricia Mester, Martina Müller, Christa Buechler, Hauke Christian Tews
Gastroenterology Insights.2024; 15(2): 486. CrossRef - Inflammatory Bowel Disease: Immune Function, Tissue Fibrosis and Current Therapies
Jesús Cosín-Roger
International Journal of Molecular Sciences.2024; 25(12): 6416. CrossRef - The Diagnosis of Intestinal Fibrosis in Crohn’s Disease—Present and Future
Sara Jarmakiewicz-Czaja, Jolanta Gruszecka, Rafał Filip
International Journal of Molecular Sciences.2024; 25(13): 6935. CrossRef - Role of gut microbiota in Crohn’s disease pathogenesis: Insights from fecal microbiota transplantation in mouse model
Qiang Wu, Lian-Wen Yuan, Li-Chao Yang, Ya-Wei Zhang, Heng-Chang Yao, Liang-Xin Peng, Bao-Jia Yao, Zhi-Xian Jiang
World Journal of Gastroenterology.2024; 30(31): 3689. CrossRef - Ultrasound of the bowel with a focus on IBD: the new best practice
Christina Merrill, Stephanie R. Wilson
Abdominal Radiology.2024; 50(2): 555. CrossRef - Unveiling the anti-inflammatory potential of 11β,13-dihydrolactucin for application in inflammatory bowel disease management
Melanie S. Matos, María Ángeles Ávila-Gálvez, Antonio González-Sarrías, Nuno-Valério Silva, Carolina Lage Crespo, António Jacinto, Ana Teresa Serra, Ana A. Matias, Cláudia Nunes dos Santos
Food & Function.2024; 15(18): 9254. CrossRef - Gut microbiota and mesenteric adipose tissue interactions in shaping phenotypes and treatment strategies for Crohn’s disease
Anis Hasnaoui, Racem Trigui, Mario Giuffrida
World Journal of Gastroenterology.2024; 30(46): 4969. CrossRef - Pathways Affected by Falcarinol-Type Polyacetylenes and Implications for Their Anti-Inflammatory Function and Potential in Cancer Chemoprevention
Ruyuf Alfurayhi, Lei Huang, Kirsten Brandt
Foods.2023; 12(6): 1192. CrossRef - Time to eRAASe chronic inflammation: current advances and future perspectives on renin-angiotensin-aldosterone-system and chronic intestinal inflammation in dogs and humans
Romy M. Heilmann, Georg Csukovich, Iwan A. Burgener, Franziska Dengler
Frontiers in Veterinary Science.2023;[Epub] CrossRef - Role of the epithelial barrier in intestinal fibrosis associated with inflammatory bowel disease: relevance of the epithelial-to mesenchymal transition
Dulce C. Macias-Ceja, M. Teresa Mendoza-Ballesteros, María Ortega-Albiach, M. Dolores Barrachina, Dolores Ortiz-Masià
Frontiers in Cell and Developmental Biology.2023;[Epub] CrossRef
- Short-Chain Fatty Acids Elicit Differential Expression of Growth Factors and Pro-Inflammatory Cytokines in Immortalized Rat Enteric Glial Cells
Case Report
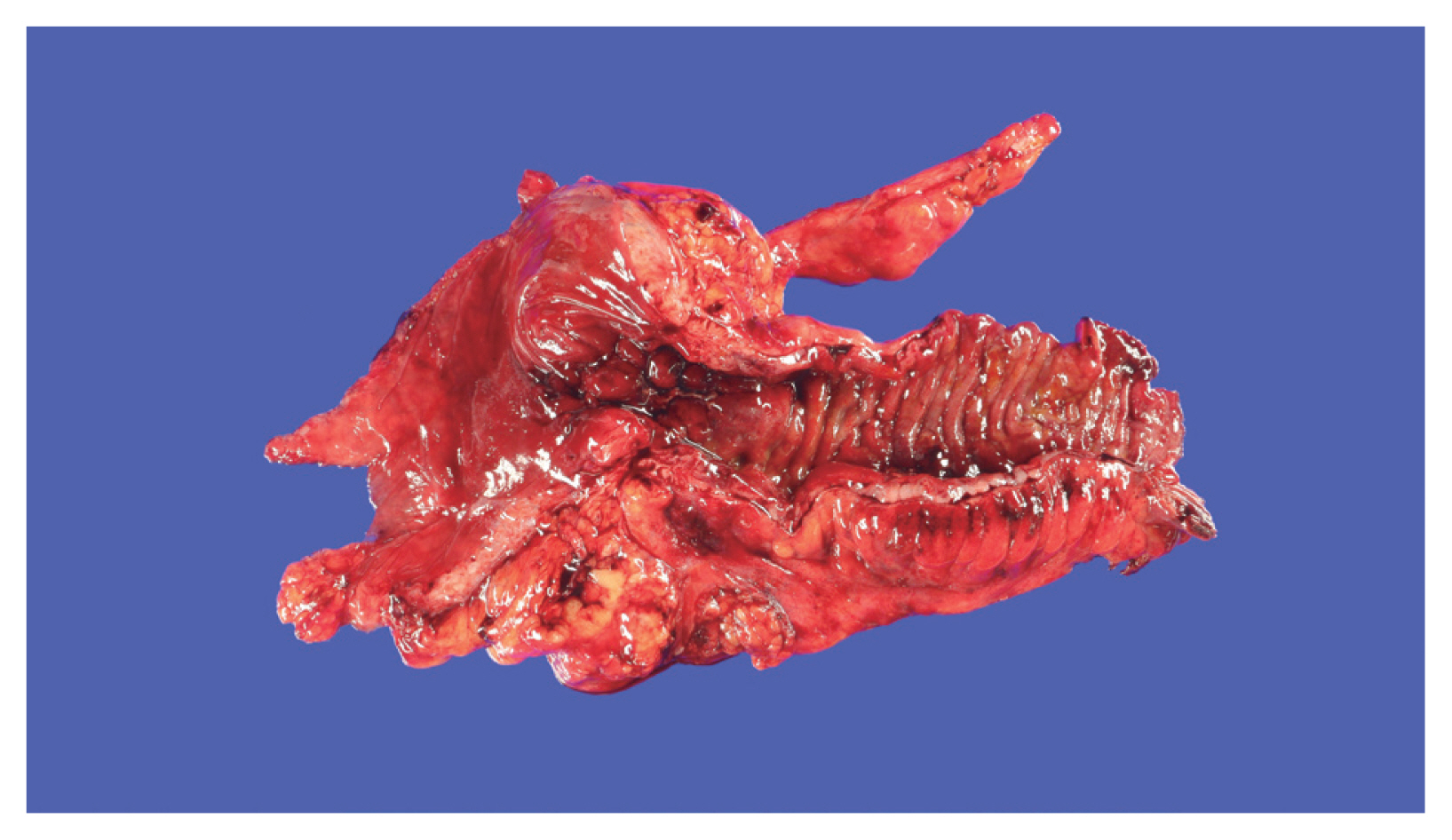
- Crohn's Disease Involving Small Intestine and Colon: 2 cases report.
- Shi Nae Lee, Sun Hee Chang, Hee Soo Yoon, Hea Soo Koo, Ok Kyung Kim, Ryung Ah Lee, Eung Beum Park
- Korean J Pathol. 1997;31(4):379-382.
- 2,170 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - Crohn's disease was originally described as a small bowel disorder and has been known to involve the large bowel in approximately 40% of all cases with or without concomitant ileal component. We describe two cases of Crohn's diseas of small intestine and colon with a summary of differential diagnosis with ulcerative colitis. Both cases were originally diagnosed and treated as ileal tuberculosis. Grossly, there were skip lesions in both cases with prominent pseudopolyps and ulcerations in colon. Also noted were typical serpentine lesions in ileum as well as in colon. Microscopically, transmural inflammation was confirmed and one case showed scattered noncaseating granulomas in the wall. Submucosal edema and fibrosis with thickening of the wall was not prominent in colon. Polymerase chain reaction performed on paraffin block for the demonstration of Mycobacterium tuberculosis in one case showed negative reaction.
Original Articles
- Cytomegalovirus Infection in Idiopathic Inflammatory Bowel Disease: Clinicopathologic Analysis of 6 Cases.
- Won Ae Lee, Hye Sung Hahn, Woo Ho Kim, Yong Il Kim
- Korean J Pathol. 1998;32(2):125-130.
- 2,292 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - Cytomegalovirus (CMV) infection is an uncommon association with idiopathic inflammatory bowel disease (IBD) often leading to a variety of serious complications. A total of 41 resected cases of IBD were examined to elucidate the pathologic features of intestinal CMV infection which was assessed by histologic examination and confirmed by immunohistochemistry with CMV antibody. Six cases were positve for CMV antibody; five cases in 19 ulcerative colitis (UC, 26.3%) and one case in 22 Crohn's disease (CD, 4.5%). Of 7 cases of the steroid-treated UC group, five cases were superinfected with CMV (71.4%) but none in 12 cases of the steroid-untreated UC group. All of the five CMV-positive cases in UC showed deep ulceration and transmural inflammation, while none of 10 UC cases without above features were CMV positive. Fibrinoid necrosis and thrombi were found in 83.3% of the CMV infected group, while none in the CMV-negative group of UC cases (p=0.01). We conclude that IBD, particularly UC, is susceptible to the CMV infection when steroid hormone is administered, and that deep colonic ulceration, transmural inflammation and fibrinoid necrosis of vasculature may suggest superinfection of CMV in UC patients. It seems that deep colonic ulceration may be the consequence of an ischemic change following vascular luminal occlusion or vasculitis by CMV infection.
- Clinicopathologic Characteristics of Ulcerative Colitis Diagnosed by Endoscopic Biopsy Specimen: An analysis of discrepancy between clinical and pathologic diagnosis.
- Jong Yup Bae, Ho Guen Kim
- Korean J Pathol. 1996;30(12):1091-1098.
- 2,089 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - Chronic ulcerative colitis is a systemic inflammatory disease with uncertain etiology primarily involving the colonic mucosa. The mucosal biopsy interpretation is important for an evaluation of the disease state and further medical or surgical treatment. However, few clinical and pathological studies of the endoscopic diagnosis of this disease are available in Korea. Therefore, we evaluated the clinical and pathological characteristics of it diagnosed by endoscopic biopsy and analysed the reasons for the discrepancy between clinical and pathologic diagnosis for a more accurate endoscopic mucosal biopsy diagnosis in the future. A total of 702 cases of colonic mucosal biopsy specimens during Feb. 1994 and Jan. 1995 at Severance hospital, Yonsei University College of Medicine were reevaluated for the study. A clinical diagnosis of ulcerative colitis, after endoscopic examination, was made in 61(8.7%) cases. A pathological diagnosis was made when there is an increased inflammatory cell infiltration in the mucosa with evidences of a chronic crypt injury in the biopsy specimens. Using this criteria, a diagnosis was made in 32(52.3%) cases. In 29 cases the diagnosis was made in the first biopsy specimen and in the remaining 3 cases the diagnosis was made in the second or third biopsy specimens. No pathologic diagnosis of ulcerative colitis was made in the cases that clinical diagnosis was not. In the 32 cases diagnosed as ulcerative colitis, 14 cases were involved the rectum and sigmoid colon, 9 cases were involved up to the descending colon, 1 case was involved up to the transverse colon and 8 cases showed pancolonic involvement. In 29 cases, which ulcerative colitis was suspected clinically but was not consistent with it pathologically, 8 cases were proved to be ischemic colitis, 5 cases were acute infectious colitis and one case was Crohn's disease by repeat examination and follow up. Ten cases were histologically within normal range and lesions subsided spontaneously with no recurrence. A conclusive diagnosis could not be made in 5 cases during this study period. From these results, we conclude that ulcerative colitis can be diagnosed accurately by endoscopic biopsy, and clinical follow up and repeat examination are valuable in the differential diagnosis of this disease.

 E-submission
E-submission

 First
First Prev
Prev



