Search
- Page Path
- HOME > Search
- Revisiting human sparganosis: a pathologic review from a single institution
- Jeemin Yim, Young A Kim, Jeong Hwan Park, Hye Eun Park, Hyun Beom Song, Ji Eun Kim
- J Pathol Transl Med. 2026;60(1):83-91. Published online January 9, 2026
- DOI: https://doi.org/10.4132/jptm.2025.10.14
- 1,735 View
- 97 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Sparganosis is a rare parasitic infection caused by Spirometra species. Although it was relatively common in the past, it is now often overlooked. In this study, we review cases diagnosed through histopathological examination at a single institution in recent years to raise awareness of this neglected parasitic disease. Methods: We retrospectively analyzed cases of human sparganosis identified in the pathology archives of a single institution in South Korea between 2004 and 2025. A comprehensive review was conducted, including demographic data, clinical features, lesion locations, imaging findings, exposure history (such as dietary habits), and histopathologic findings. Results: A total of 15 patients were identified, including 10 females and 5 males, with a mean age of 65.1 years. Lesions were most commonly located in the lower extremities and breast. Imaging findings were largely nonspecific, with ultrasonography being the most frequently used modality. In most cases, clinical suspicion of sparganosis was absent, and excision was performed under the impression of a benign or malignant tumor. Histologically, variably degenerated parasitic structures were identified within granulomatous inflammation. However, preserved features such as calcospherules and tegumental structures facilitated definitive diagnosis. Conclusions: This study underscores the importance of recognizing the characteristic histopathological features of sparganosis, which can allow for accurate diagnosis even in the absence of clinical suspicion. Although rare, sparganosis remains a relevant diagnostic consideration in endemic regions, particularly in East Asia.
- Solitary fibrous tumor: an updated review
- Joon Hyuk Choi
- J Pathol Transl Med. 2026;60(1):20-46. Published online December 29, 2025
- DOI: https://doi.org/10.4132/jptm.2025.10.08
- 2,085 View
- 193 Download
-
 Abstract
Abstract
 PDF
PDF - Solitary fibrous tumor (SFT) is a fibroblastic neoplasm characterized by a branching, thin-walled dilated staghorn-shaped (hemangiopericytoma-like) vasculature and a NAB2::STAT6 gene fusion. SFTs can occur in almost any anatomical location, including superficial and deep soft tissues, visceral organs, and bone. They most commonly occur in extrapleural locations, equally affect both sexes, and are typically present in adults. Although metastasis is rare, SFTs frequently show local recurrence. The diagnosis of SFTs is difficult because of their broad histological and morphological overlap with other neoplasms. An accurate diagnosis is important for guiding disease management and prognosis. Despite advances in molecular diagnostics and therapeutic strategies, the biological complexity and unpredictable clinical behavior of SFTs present significant challenges. This review provides an updated overview of SFT, with a focus on its molecular genetics, histopathological features, and diagnostic considerations.
- Diagnostic challenge in Burkitt lymphoma of the mandible initially misdiagnosed as osteomyelitis: a case report
- Jiwon Do, Jin-Young Choi
- J Pathol Transl Med. 2025;59(6):460-466. Published online November 14, 2025
- DOI: https://doi.org/10.4132/jptm.2025.09.18
- 3,110 View
- 102 Download
-
 Abstract
Abstract
 PDF
PDF - Burkitt lymphoma (BL) is a highly aggressive B-cell neoplasm that rarely involves the mandible in elderly without apparent immunodeficiency. We report a case of a 72-year-old male who presented with persistent mandibular pain following extraction of tooth #46. Initial imaging findings were consistent with incipient osteomyelitis, and the patient was treated with antibiotics. Despite treatment, pain persisted, and follow-up imaging revealed swelling and diffusion restriction in the lateral pterygoid muscle without evidence of a distinct mass. Biopsy revealed BL confirmed by immunohistochemistry: CD10+, BCL6+, c-MYC+, Ki-67 >95%, and negative for BCL2, MUM-1, and Epstein-Barr virus. Although c-MYC immunopositivity was demonstrated, fluorescence in situ hybridization for MYC rearrangement could not be performed due to limited tissue, representing a diagnostic limitation. Notably, the patient had no trismus despite deep muscle involvement, but complained of facial paresthesia and showed remote swelling in the scapular area during hospitalization. Systemic staging with imaging, cerebrospinal fluid cytology, and imaging revealed disseminated nodal and extranodal involvement including the central nervous system, corresponding to stage IV disease by Lugano classification. This case highlights the diagnostic challenge of distinguishing lymphoma from osteomyelitis and underscores the importance of considering malignancy in cases of refractory mandibular inflammation with atypical features.
- Diagnostic value of cytology in detecting human papillomavirus–independent cervical malignancies: a nation-wide study in Korea
- Hye-Ra Jung, Junyoung Shin, Chong Woo Yoo, Eun Na Kim, Cheol Lee, Kyeongmin Kim, Ho-chang Lee, Yonghee Lee, Ji Hye Kim, Soo Jin Jung, Yumin Chung, Joo Yeon Kim, Hye Eun Park, Tae Hoen Kim, Wonae Lee, Min-Sun Cho, Ran Hong, Yoon Jung Choi, Younghee Choi, Young Sub Lee, Sang-Ryung Lee, Myunghee Kang, Young Jin Seo, Seung-Sook Lee, Yoon-Jung Hwang, Hyun-Jung Kim
- J Pathol Transl Med. 2025;59(6):444-452. Published online November 11, 2025
- DOI: https://doi.org/10.4132/jptm.2025.10.21
- 4,237 View
- 140 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) independent cervical malignancies (HPV-IDCMs) have recently been classified by the World Health Organization (WHO) 5th edition. These malignancies have historically received limited attention due to their rarity and the potential for evasion of HPV-based screening.
Methods
We retrospectively reviewed 5,854 biopsy-confirmed cervical malignancies from 22 institutions over 3 years (July 2020–June 2023). Histologic classification followed the WHO guidelines. HPV independence was confirmed by dual negativity for p16 and HPV; discordant cases (p16-positive/HPV-negative) underwent additional HPV testing using paraffin-embedded tissue. Cytological results were matched sequentially to histological confirmation.
Results
The prevalence of HPV-IDCM was 4.4% (257/5,854) overall and was 3.6% (208/5,805 cases) among primary cervical malignancy. Patient age of HPV-IDCM was 29 to 89 years (median, 57.79). Its histologic subtypes included primary adenocarcinoma (n = 116), endometrial adenocarcinoma (n = 35), squamous cell carcinoma (n = 72), metastatic carcinoma (n = 14), carcinoma, not otherwise specified (n = 10), neuroendocrine carcinoma (n = 3), and others (n = 7). Among 155 cytology-histological matched cases, the overall and primary Pap test detection rates were 85.2% (132/155) and 83.2% (104/125), respectively. The interval between cytology and histologic confirmation extended up to 38 months.
Conclusions
HPV-IDCMs comprised 3.6% of primary cervical malignancies with a high detection rate via cytology (83.2%). These findings affirm the value of cytological screening, particularly in patients with limited screening history or at risk for HPV-independent lesions, and may guide future screening protocols.
- Central nervous system tumors with BCOR internal tandem duplications: a systematic review of clinical, radiological, and pathological features in 69 cases
- Ji Young Lee, Sung Sun Kim, Hee Jo Baek, Tae-Young Jung, Kyung-Sub Moon, Jae-Hyuk Lee, Kyung-Hwa Lee
- J Pathol Transl Med. 2025;59(5):273-280. Published online September 1, 2025
- DOI: https://doi.org/10.4132/jptm.2025.07.23
- 4,041 View
- 190 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Central nervous system tumors with BCL6 corepressor (BCOR) internal tandem duplications (ITDs) constitute a rare, recently characterized pediatric neoplasm with distinct molecular and histopathological features. To date, 69 cases have been documented in the literature, including our institutional case. These neoplasms predominantly occur in young children, with the cerebellum representing the most frequent anatomical location. Radiologically, these tumors present as large, well-circumscribed masses frequently demonstrating necrosis, hemorrhage, and heterogeneous enhancement. Histologically, they are characterized by a monomorphic cellular population featuring ependymoma-like perivascular pseudorosettes, myxoid stroma, and elevated mitotic activity. Immunohistochemically, these tumors exhibit sparse glial fibrillary acidic protein expression while consistently demonstrating positive staining for vimentin and CD56. The defining molecular hallmark is a heterozygous ITD within exon 15 of the BCOR gene, with insertions ranging from 9 to 42 amino acids in length. BCOR immunohistochemistry reveals nuclear positivity in 97.9% of examined cases, although this finding is not pathognomonic for BCOR ITDs. This comprehensive review synthesizes data from all published cases of this novel tumor entity, providing a detailed analysis of clinical presentation, neuroimaging findings, histopathological features with differential diagnostic considerations, therapeutic approaches, and prognostic outcomes.
- Clinicopathologic characterization of cervical metastasis from an unknown primary tumor: a multicenter study in Korea
- Miseon Lee, Uiree Jo, Joon Seon Song, Youn Soo Lee, Chang Gok Woo, Dong-Hoon Kim, Jung Yeon Kim, Sun Och Yoon, Kyung-Ja Cho
- J Pathol Transl Med. 2023;57(3):166-177. Published online May 10, 2023
- DOI: https://doi.org/10.4132/jptm.2023.04.12
- 6,686 View
- 172 Download
- 6 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Research regarding cervical metastasis from an unknown primary tumor (CUP) according to human papillomavirus (HPV) and Epstein-Barr virus (EBV) status in Korea has been sporadic and small-scale. This study aims to analyze and understand the characteristics of CUP in Korea according to viral and p16 and p53 status through a multicenter study.
Methods
Ninety-five cases of CUP retrieved from six hospitals in Korea between January 2006 and December 2016 were subjected to high-risk HPV detection (DNA in situ hybridization [ISH] or real-time polymerase chain reaction), EBV detection (ISH), and immunohistochemistry for p16 and p53.
Results
CUP was HPV-related in 37 cases (38.9%), EBV-related in five cases (5.3%), and unrelated to HPV or EBV in 46 cases (48.4%). HPV-related CUP cases had the best overall survival (OS) (p = .004). According to the multivariate analysis, virus-unrelated disease (p = .023) and longer smoking duration (p < .005) were prognostic factors for poor OS. Cystic change (p = .016) and basaloid pattern (p < .001) were more frequent in HPV-related cases, and lymphoepithelial lesion was frequent in EBV-related cases (p = .010). There was no significant association between viral status and p53 positivity (p = .341), smoking status (p = .728), or smoking duration (p = .187). Korean data differ from Western data in the absence of an association among HPV, p53 positivity, and smoking history.
Conclusions
Virus-unrelated CUP in Korea had the highest frequency among all CUP cases. HPV-related CUP is similar to HPV-mediated oropharyngeal cancer and EBVrelated CUP is similar to nasopharyngeal cancer in terms of characteristics, respectively. -
Citations
Citations to this article as recorded by- Management of squamous cell carcinoma of unknown primary in the head and neck: current evidence-based diagnostic and treatment strategies
Marcel Kloppenburg, Matthias Santer, Lukas Schmutzler, Felix Johnson, Benedikt Hofauer, Teresa Steinbichler
memo - Magazine of European Medical Oncology.2026; 19(1): 45. CrossRef - Differenzierung von benignen und malignen Halszysten – eine diagnostische Herausforderung
Christina Sauter, Matthias Sand, Karim Plath, Michaela Maria Plath
Laryngo-Rhino-Otologie.2025; 104(05): 296. CrossRef - Unlocking the Hidden: Advancing Imaging Techniques in Diagnosing Cancers of Unknown Primary in the Head and Neck Region
Daniela Messineo, Filippo Valentini, Giovanni Francesco Niccolini, Federica Zoccali, Francesca Ripari, Enrico Marotta, Marcello Caratozzolo, Pasquale Frisina
Applied Sciences.2025; 15(4): 2194. CrossRef - Characterization of undifferentiated carcinoma of the salivary gland: clinicopathological and immunohistochemical analyses in comparison with lymphoepithelial carcinoma
Sangjoon Choi, Gyuheon Choi, Hee Jin Lee, Joon Seon Song, Yoon Se Lee, Seung-Ho Choi, Kyung-Ja Cho
Journal of Pathology and Translational Medicine.2025; 59(6): 361. CrossRef - Expansion of tumor-infiltrating lymphocytes from head and neck squamous cell carcinoma to assess the potential of adoptive cell therapy
Sangjoon Choi, Mofazzal Hossain, Hyun Lee, Jina Baek, Hye Seon Park, Chae-Lyul Lim, DoYeon Han, Taehyun Park, Jong Hyeok Kim, Gyungyub Gong, Mi-Na Kweon, Hee Jin Lee
Cancer Immunology, Immunotherapy.2024;[Epub] CrossRef
- Management of squamous cell carcinoma of unknown primary in the head and neck: current evidence-based diagnostic and treatment strategies
- Neuropathologic features of central nervous system hemangioblastoma
- Rebecca A. Yoda, Patrick J. Cimino
- J Pathol Transl Med. 2022;56(3):115-125. Published online May 3, 2022
- DOI: https://doi.org/10.4132/jptm.2022.04.13
- 17,699 View
- 377 Download
- 21 Web of Science
- 26 Crossref
-
 Abstract
Abstract
 PDF
PDF - Hemangioblastoma is a benign, highly vascularized neoplasm of the central nervous system (CNS). This tumor is associated with loss of function of the VHL gene and demonstrates frequent occurrence in von Hippel-Lindau (VHL) disease. While this entity is designated CNS World Health Organization grade 1, due to its predilection for the cerebellum, brainstem, and spinal cord, it is still an important cause of morbidity and mortality in affected patients. Recognition and accurate diagnosis of hemangioblastoma is essential for the practice of surgical neuropathology. Other CNS neoplasms, including several tumors associated with VHL disease, may present as histologic mimics, making diagnosis challenging. We outline key clinical and radiologic features, pathophysiology, treatment modalities, and prognostic information for hemangioblastoma, and provide a thorough review of the gross, microscopic, immunophenotypic, and molecular features used to guide diagnosis.
-
Citations
Citations to this article as recorded by- Hemangioblastoma of the Kidney—A Comprehensive Clinical, Pathological, and Genetic Analysis of Four Cases
Boglárka Pósfai, Alex Jenei, Gertrúd Forika, Attila Fintha, Zoltán Sápi, Áron Somorácz, Borbála Dénes, Ferenc Salamon, Kornélia Veronika Eizler, Nándor Giba, Dávid Semjén, Ildikó Illyés, Kristóf Attila Kovács, Gyöngyi Munkácsy, János Papp, Fanni Sánta, He
APMIS.2026;[Epub] CrossRef - Peritumoral Cystic Meningioma With Diagnostic Challenges: Two Case Reports and a Literature Review
Wei-Chih Chen, Zi-Jie Lin, Lam Chee-Tat
Cureus.2026;[Epub] CrossRef - Belzutifan-induced tumor regression in sporadic hemangioblastoma: a case report and literature review
Rebekka E. Hooks, Niket Yadav, Mark Willy L. Mondia, Georgios Mantziaris, Alaa Saleh, Anna Vi Jones, Matthew McCord, Melike Mut, Ashok R. Asthagiri, Benjamin W. Purow
Journal of Neuro-Oncology.2026;[Epub] CrossRef - Unusual immunohistochemical profiles in hemangioblastomas and their relevance in differential diagnosis: A comprehensive study of 112 cases
Jiri Soukup, Marie Novakova, Jan Hojny, Marketa Trnkova, Martin Syrucek, Tomas Jirasek, Patricie Delongova, Ales Kohout, Tomas Vebr, Jan Sroubek, Alena Sejkorova, Radim Lipina, Radim Brabec, Tomas Cesak, David Netuka
Journal of Neuropathology & Experimental Neurology.2026;[Epub] CrossRef - Immunohistochemical Expression of PAX8 in Central Nervous System Hemangioblastomas: A Potential Diagnostic Pitfall for Neuropathologists
Giuseppe Broggi, Jessica Farina, Valeria Barresi, Francesco Certo, Giuseppe Maria Vincenzo Barbagallo, Gaetano Magro, Rosario Caltabiano
Applied Immunohistochemistry & Molecular Morphology.2025; 33(3): 160. CrossRef - Endolymphatic Sac Tumor. Post-Radiosurgery Evaluation Using Time-Resolved Imaging of Contrast Kinetics MR Angiography
Antonella Blandino, Allegra Romano, Chiara Filippi, Sofia Pizzolante, Andrea Romano, Giulia Moltoni, Edoardo Covelli, Maurizio Barbara, Alessandro Bozzao
Ear, Nose & Throat Journal.2025;[Epub] CrossRef - Stereotactic radiosurgery in the management of central nervous system hemangioblastomas: a systematic review and meta-analysis
Amirhossein Zare, Amirhessam Zare, Alireza Soltani Khaboushan, Bardia Hajikarimloo, Jason P. Sheehan
Neurosurgical Review.2025;[Epub] CrossRef - Cerebellar medullary cistern hemangioblastoma
Dahai Cao, Qiang Zhang
Asian Journal of Surgery.2025; 48(9): 5843. CrossRef - Navigating rare vascular brain tumors: A retrospective observational study
Sana Ahuja, Dipanker S Mankotia, Naveen Kumar, Vyomika Teckchandani, Sufian Zaheer
Cancer Research, Statistics, and Treatment.2025; 8(2): 92. CrossRef - A potential new entity pending further validation of pulmonary primary interstitial Tumor: Lymphangioleiomyomatosis-like
Lingyu Zhao, Xiaochen Shen, Yun Niu, Huang Chen, Dingrong Zhong
Respiratory Medicine Case Reports.2025; 57: 102241. CrossRef - Renal cell carcinoma with fibromyomatous stroma (RCC FMS) and with hemangioblastoma‐like areas is part of the RCC FMS spectrum in patients with tuberous sclerosis complex
Katherina Baranova, Jacob A Houpt, Deaglan Arnold, Andrew A House, Laura Lockau, Lindsay Ninivirta, Stephen Pautler, Haiying Chen, Madeleine Moussa, Rola Saleeb, Jose A Gomez, Asli Yilmaz, Farshid Siadat, Adrian Box, Douglas J Mahoney, Franz J Zemp, Manal
Histopathology.2025; 87(5): 687. CrossRef - Renal hemangioblastoma and renal cell carcinoma with fibromyomatous stroma and hemangioblastoma-like areas belong to the spectrum of one entity
Kiril Trpkov, Norel Salut, Inmaculada Ribera-Cortada, Elías Tasso Xipell, Isabel Trias Puigsureda, Asli Yilmaz, Arjumand Riyaz Husain, Erik Nohr, Adrian Box, Farshid Siadat, Katherina Baranova, Rola M. Saleeb, Robert Stoehr, Arndt Hartmann, Abbas Agaimy
Virchows Archiv.2025;[Epub] CrossRef - Primary hemangioblastoma of rectum: a rare case report and review of literature
Aiping Zheng, Shaojuan Zhang, Qiang Ma, Wenxu Yang, Hualiang Xiao, Xinyu Liang
Journal of Cancer Research and Clinical Oncology.2025;[Epub] CrossRef - Cerebellar Hemangioblastoma Resection Complicated by Postoperative Vasogenic Edema in the Setting of Concurrent Immunotherapy Treatment
Aashka Sheth, Nicholas Dietz, Andrea Becerril-Gaitan, Rahim Kasem, Akshitkumar Mistry, Brian J Williams, Dale Ding, Isaac Abecassis
Cureus.2025;[Epub] CrossRef - Familial Von Hippel–Lindau Disease: A Case Series of Cerebral Hemangioblastomas with MRI, Histopathological, and Genetic Correlations
Claudiu Matei, Ioana Boeras, Dan Orga Dumitriu, Cosmin Mutu, Adriana Popescu, Mihai Gabriel Cucu, Alexandru Calotă-Dobrescu, Bogdan Fetica, Diter Atasie
Life.2025; 15(11): 1649. CrossRef - Characterization of spinal hemangioblastomas in patients with and without von Hippel-Lindau, and YAP expression
Ana-Laura Calderón-Garcidueñas, Steven-Andrés Piña-Ballantyne, Eunice-Jazmín Espinosa-Aguilar, Rebeca de Jesús Ramos-Sánchez
Revista Española de Patología.2024; 57(3): 160. CrossRef - Patients With Hemangioblastoma: Mood Disorders and Sleep Quality
Ali Riazi, Yaser Emaeillou, Nima Najafi, Mohammad Hoseinimanesh, Mohammad Ibrahim Ashkaran, Donya Sheibani Tehrani
Brain Tumor Research and Treatment.2024; 12(2): 87. CrossRef - Radiosurgically Treated Recurrent Cerebellar Hemangioblastoma: A Case Report and Literature Review
François Fabi, Ève Chamberland, Myreille D’Astous, Karine Michaud, Martin Côté, Isabelle Thibault
Current Oncology.2024; 31(7): 3968. CrossRef - Dual manifestations: spinal and cerebellar hemangioblastomas indicative of von Hippel-Lindau syndrome
Nurhuda Hendra Setyawan, Rachmat Andi Hartanto, Rusdy Ghazali Malueka, Ery Kus Dwianingsih, Dito Pondra Dharma
Radiology Case Reports.2024; 19(11): 5000. CrossRef - Phenotypic and Genotypic Features of a Chinese Cohort with Retinal Hemangioblastoma
Liqin Gao, Feng Zhang, J. Fielding Hejtmancik, Xiaodong Jiao, Liyun Jia, Xiaoyan Peng, Kai Ma, Qian Li
Genes.2024; 15(9): 1192. CrossRef - Hemangioblastoma Incidentally Discovered at CT Scan in Bamako: About a Case
Traore Ousmane, N’Diaye Mamadou, Dembélé Mamadou, Dembélé Adama, Diakité Siaka, Sidibé Mansa Drissa, Camara Nagnoumague, Keita Adama Diaman
Open Journal of Medical Imaging.2024; 14(03): 123. CrossRef - Case report: Hemangioblastoma in the brainstem of a dog
Kirsten Landsgaard, Samantha St. Jean, Stephanie Lovell, Jonathan Levine, Christine Gremillion, Brian Summers, Raquel R. Rech
Frontiers in Veterinary Science.2023;[Epub] CrossRef - Intramedullary hemangioblastoma of the thoracic cord with a microsurgical approach: A case report and literature review
Eduardo Cattapan Piovesan, Werner Petry Silva, Adroaldo Baseggio Mallmann, Felipe Severo Lanzini, Bruna Zanatta de Freitas, Francisco Costa Beber Lemanski, Charles André Carazzo
Surgical Neurology International.2023; 14: 137. CrossRef - Secondary Holocord Syringomyelia Associated With Spinal Hemangioblastoma in a 29-Year-Old Female
Eric Chun-Pu Chu, Edouard Sabourdy, Benjamin Cheong
Cureus.2023;[Epub] CrossRef - Belzutifan in adults with VHL-associated central nervous system hemangioblastoma: a single-center experience
Bryan J. Neth, Mason J. Webb, Jessica White, Joon H. Uhm, Pavel N. Pichurin, Ugur Sener
Journal of Neuro-Oncology.2023; 164(1): 239. CrossRef - Resection of Intramedullary Hemangioblastoma: Timing of Surgery and Its Impact on Neurological Outcome and Quality of Life
Michael Schwake, Sarah Ricchizzi, Sophia Krahwinkel, Emanuele Maragno, Stephanie Schipmann, Walter Stummer, Marco Gallus, Markus Holling
Medicina.2023; 59(9): 1611. CrossRef
- Hemangioblastoma of the Kidney—A Comprehensive Clinical, Pathological, and Genetic Analysis of Four Cases
- Adrenal hemangioblastoma
- Joo-Yeon Koo, Kyung-Hwa Lee, Joon Hyuk Choi, Ho Seok Chung, Chan Choi
- J Pathol Transl Med. 2022;56(3):161-166. Published online February 28, 2022
- DOI: https://doi.org/10.4132/jptm.2021.12.28
- 5,862 View
- 157 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Hemangioblastoma (HB) is a rare benign tumor that most commonly occurs in the cerebellum. HB is composed of neoplastic stromal cells and abundant small vessels. However, the exact origin of stromal cells is controversial. Extraneural HBs have been reported in a small series, and peripheral HBs arising in the adrenal gland are extremely rare. Herein, we report a case of sporadic adrenal HB in a 54-year-old woman. The tumor was a well-circumscribed, yellow mass measuring 4.2 cm in diameter. Histologically, the tumor was composed of small blood vessels and vacuolated stromal cells with clear cytoplasm. On immunohistochemical stain, the stromal cells were positive for S-100 protein, neuron-specific enolase, and synaptophysin. The tumor did not reveal mutation of VHL alleles. We herein present a case of HB of the adrenal gland and review of the literature.
-
Citations
Citations to this article as recorded by- Familial Von Hippel–Lindau Disease: A Case Series of Cerebral Hemangioblastomas with MRI, Histopathological, and Genetic Correlations
Claudiu Matei, Ioana Boeras, Dan Orga Dumitriu, Cosmin Mutu, Adriana Popescu, Mihai Gabriel Cucu, Alexandru Calotă-Dobrescu, Bogdan Fetica, Diter Atasie
Life.2025; 15(11): 1649. CrossRef
- Familial Von Hippel–Lindau Disease: A Case Series of Cerebral Hemangioblastomas with MRI, Histopathological, and Genetic Correlations
- Clinicopathological differences in radiation-induced organizing hematomas of the brain based on type of radiation treatment and primary lesions
- Myung Sun Kim, Se Hoon Kim, Jong-Hee Chang, Mina Park, Yoon Jin Cha
- J Pathol Transl Med. 2022;56(1):16-21. Published online October 15, 2021
- DOI: https://doi.org/10.4132/jptm.2021.08.30
- 7,586 View
- 244 Download
- 4 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Radiation-induced organizing hematoma (RIOH) is a sporadic form of cavernous hemangioma (CH) that occurs after cerebral radiation. RIOH lesions are distinct histologically from de novo CH; however, detailed research on this subject is lacking. In the present study, the clinical and histological features of RIOHs were evaluated based on causative lesions.
Methods
The present study included 37 RIOHs confirmed by surgical excision from January 2009, to May 2020, in Yonsei Severance Hospital. All cases were divided into subgroups based on type of radiation treatment (gamma knife surgery [GKS], n = 24 vs. conventional radiation therapy [RT], n = 13) and pathology of the original lesion (arteriovenous malformation, n = 14; glioma, n = 12; metastasis, n = 4; other tumors, n = 7). The clinicopathological results were compared between the groups.
Results
Clinical data of multiplicity, latency, and size and wall thickness of the original tumors and RIOHs were analyzed. The GKS group showed shorter latency (5.85 ± 4.06 years vs. 11.15 ± 8.27 years, p = .046) and thicker tumor wall (693.7 ± 565.7 μm vs. 406.9 ± 519.7 μm, p = .049) than the conventional RT group. Significant difference was not found based on original pathology.
Conclusions
RIOH is more likely to occur earlier with thick tumor wall in subjects who underwent GKS than in patients who underwent conventional RT. These results indicate the clinical course of RIOH differs based on type of treatment and might help determine the duration of follow-up. -
Citations
Citations to this article as recorded by- Impact of cranial irradiation on the clinical presentation of cerebral cavernous malformations
Neerav Kumar, Jeffrey Shi, Carlos Alcocer, Sara Luck, Andrew Garton, Maricruz Rivera, Mark M. Souweidane, Philip E. Stieg
Clinical Neurology and Neurosurgery.2026; 265: 109386. CrossRef - Radiation-Induced Cavernous Malformation in the Cerebellum: Clinical Features of Two Cases
Hyoung Soo Choi, Chae-Yong Kim, Byung Se Choi, Seung Hyuck Jeon, In Ah Kim, Joo-Young Kim, Kyu Sang Lee, Gheeyoung Choe
Brain Tumor Research and Treatment.2025; 13(2): 58. CrossRef - End-stage ADPKD with a low-frequency PKD1 mosaic variant accelerated by chemoradiotherapy
Hiroaki Hanafusa, Hiroshi Yamaguchi, Naoya Morisada, Ming Juan YE, Riki Matsumoto, Hiroaki Nagase, Kandai Nozu
Human Genome Variation.2024;[Epub] CrossRef - Recapitulating the Key Advances in the Diagnosis and Prognosis of High-Grade Gliomas: Second Half of 2021 Update
Guido Frosina
International Journal of Molecular Sciences.2023; 24(7): 6375. CrossRef - Earlier Age at Surgery for Brain Cavernous Angioma-Related Epilepsy May Achieve Complete Seizure Freedom without Aid of Anti-Seizure Medication
Ayataka Fujimoto, Hideo Enoki, Keisuke Hatano, Keishiro Sato, Tohru Okanishi
Brain Sciences.2022; 12(3): 403. CrossRef
- Impact of cranial irradiation on the clinical presentation of cerebral cavernous malformations
- Evaluation of human papillomavirus (HPV) prediction using the International Endocervical Adenocarcinoma Criteria and Classification system, compared to p16 immunohistochemistry and HPV RNA in-situ hybridization
- Hezhen Ren, Jennifer Pors, Christine Chow, Monica Ta, Simona Stolnicu, Robert Soslow, David Huntsman, Lynn Hoang
- J Pathol Transl Med. 2020;54(6):480-488. Published online August 31, 2020
- DOI: https://doi.org/10.4132/jptm.2020.07.18
- 8,926 View
- 175 Download
- 11 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The International Endocervical Adenocarcinoma Criteria and Classification (IECC) separated endocervical adenocarcinomas into human papillomavirus (HPV) associated (HPVA) and non–HPV-associated (NHPVA) categories by morphology alone. Our primary objective was to assess the accuracy of HPV prediction by the IECC system compared to p16 immunohistochemistry and HPV RNA in-situ hybridization (RISH). Our secondary goal was to directly compare p16 and HPV RISH concordance.
Methods
Cases were classified by IECC and stained for p16 and HPV RISH on tissue microarray, with discordant p16/HPV RISH cases re-stained on whole tissue sections. Remaining discordant cases (p16/HPV, IECC/p16, IECC/HPV discordances) were re-reviewed by the original pathologists (n = 3) and external expert pathologists (n = 2) blinded to the p16 and HPV RISH results. Final IECC diagnosis was assigned upon independent agreement between all reviewers.
Results
One hundred and eleven endocervical adenocarcinomas were classified originally into 94 HPVA and 17 NHPVA cases. p16 and HPV RISH was concordant in 108/111 cases (97%) independent of the IECC. HPV RISH and p16 was concordant with IECC in 103/111 (93%) and 106/111 (95%), respectively. After expert review, concordance improved to 107/111 (96%) for HPV RISH. After review of the eight discordant cases, one remained as HPVA, four were reclassified to NHPVA from HPVA, two were unclassifiable, and one possibly represented a mixed usual and gastric-type adenocarcinoma.
Conclusions
p16 and HPV RISH have excellent concordance in endocervical adenocarcinomas, and IECC can predict HPV status in most cases. Focal apical mitoses and apoptotic debris on original review led to the misclassification of several NHPVA as HPVA. -
Citations
Citations to this article as recorded by- Role of human papillomavirus status in the classification, diagnosis, and prognosis of malignant cervical epithelial tumors and precursor lesions
Simona Stolnicu
Die Pathologie.2026; 47(S1): 97. CrossRef - EdgeNeXt-SEDP for cervical adenocarcinoma HPV-associated and non-HPV-associated diagnosis and decision support
Qi Chen, Hao Wang, Hao Zhang, Zhenkun Zhu, Xi Wei
Life Sciences.2025; 380: 123931. CrossRef - Cytology and histology of endocervical glandular lesions: a review with emphasis on recent developments
Natalie Banet, Karen L. Talia
Pathology.2025; 57(7): 817. CrossRef - Joint detection of multiple HPV-testing technologies and evaluation of clinicopathological characteristics discriminate between HPV-independent and low-copy HPV-associated cervical squamous cell carcinoma (CSCC) -an analysis of 3869 cases
Linghui Lu, Tianqi Liu, Shunni Wang, Jing Li, Feiran Zhang, Yan Ning, Yiqin Wang
Gynecologic Oncology.2023; 170: 59. CrossRef - Incidence and Clinicopathologic Characteristics of Human Papillomavirus–independent Invasive Squamous Cell Carcinomas of the Cervix
Simona Stolnicu, Douglas Allison, Aaron M. Praiss, Basile Tessier-Cloutier, Amir Momeni Boroujeni, Jessica Flynn, Alexia Iasonos, Rene Serrette, Lien Hoang, Andrei Patrichi, Cristina Terinte, Anna Pesci, Claudia Mateoiu, Ricardo R. Lastra, Takako Kiyokawa
American Journal of Surgical Pathology.2023; 47(12): 1376. CrossRef - Testing Algorithms for the Diagnosis of Malignant Glandular Tumors of the Uterine Cervix Histotyped per the International Endocervical Adenocarcinoma Criteria and Classification (IECC) System
Máire A. Duggan, Qiuli Duan, Ruth M. Pfeiffer, Mary Anne Brett, Sandra Lee, Mustapha Abubakar, Martin Köbel, Monica Rodriguez, Aylin Sar
Applied Immunohistochemistry & Molecular Morphology.2022; 30(2): 91. CrossRef - Local and Metastatic Relapses in a Young Woman with Papillary Squamous Cell Carcinoma of the Uterine Cervix
Ha Young Woo, Hyun-Soo Kim
Diagnostics.2022; 12(3): 599. CrossRef - Clinical correlation of lymphovascular invasion and Silva pattern of invasion in early-stage endocervical adenocarcinoma: proposed binary Silva classification system
Simona Stolnicu, Lien Hoang, Noorah Almadani, Louise De Brot, Glauco Baiocchi, Graziele Bovolim, Maria Jose Brito, Georgia Karpathiou, Antonio Ieni, Esther Guerra, Takako Kiyokawa, Pavel Dundr, Carlos Parra-Herran, Sofia Lérias, Ana Felix, Andres Roma, An
Pathology.2022; 54(5): 548. CrossRef - Reproducibility of Morphologic Parameters of the International Endocervical Adenocarcinoma Criteria and Classification System and Correlation With Clinicopathologic Parameters: A Multi-Institutional Study
Pinar Bulutay, Nihan Haberal, Özlem Özen, Özlem Erdem, Emine H. Zeren, İbrahim Kulac, Çagatay Taskiran, Dogan Vatansever, Ali Ayhan, Nilgün Kapucuoğlu
International Journal of Gynecological Pathology.2022; 41(5): 447. CrossRef - HPV-Negative Cervical Cancer: A Narrative Review
Francesca Arezzo, Gennaro Cormio, Vera Loizzi, Gerardo Cazzato, Viviana Cataldo, Claudio Lombardi, Giuseppe Ingravallo, Leonardo Resta, Ettore Cicinelli
Diagnostics.2021; 11(6): 952. CrossRef - International Endocervical Adenocarcinoma Criteria and Classification (IECC): An Independent Cohort With Clinical and Molecular Findings
Hezhen Ren, Noorah Almadani, Jennifer Pors, Samuel Leung, Julie Ho, Christine Chow, Monica Ta, Kay J. Park, Simona Stolnicu, Robert Soslow, David Huntsman, Blake C. Gilks, Lynn Hoang
International Journal of Gynecological Pathology.2021; 40(6): 533. CrossRef
- Role of human papillomavirus status in the classification, diagnosis, and prognosis of malignant cervical epithelial tumors and precursor lesions
- Prevalence of high-risk human papillomavirus and its genotype distribution in head and neck squamous cell carcinomas
- Yuil Kim, Young-Hoon Joo, Min-Sik Kim, Youn Soo Lee
- J Pathol Transl Med. 2020;54(5):411-418. Published online July 21, 2020
- DOI: https://doi.org/10.4132/jptm.2020.06.22
- 12,773 View
- 188 Download
- 23 Web of Science
- 25 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
High-risk (HR) human papillomavirus (HPV) is found in a subset of head and neck (HN) squamous cell carcinomas (SCCs). For oropharyngeal SCCs, HR HPV positivity is known to be associated with good prognosis, and a separate staging system for HPV-associated carcinomas using p16 immunohistochemistry (IHC) as a surrogate test has been adopted in the 8th American Joint Committee on Cancer staging system. We examined the HR HPV status and the genotype distribution in five HN subsites.
Methods
Formalin-fixed paraffin-embedded tissue sections were used for p16 IHC and DNA extraction. HPV DNA detection and genotyping were done employing either a DNA chip-based or real-time polymerase chain reaction–based method.
Results
During 2011–2019, a total of 466 SCCs were tested for HPV DNA with 34.1% positivity for HR HPV. Among HN subsites, the oropharynx showed the highest HR HPV prevalence (149/205, 75.1%), followed by the sinonasal tract (3/14, 21.4%), larynx (5/43, 11.6%), hypopharynx (1/38, 2.6%), and oral cavity (1/166, 0.6%). The most common HPV genotype was HPV16 (84.3%) followed by HPV35 (6.9%) and HPV33 (4.4%). Compared with HR HPV status, the sensitivity and specificity of p16 IHC were 98.6% and 94.3% for the oropharynx, and 99.2% and 93.8% for the tonsil, respectively.
Conclusions
Using a Korean dataset, we confirmed that HR HPV is most frequently detected in oropharyngeal SCCs. p16 positivity showed a good concordance with HR HPV DNA for oropharyngeal and especially tonsillar carcinomas. The use of p16 IHC may further be extended to predict HR HPV positivity in sinonasal tract SCCs. -
Citations
Citations to this article as recorded by- Impact of histopathological parameters in prognosis of oral squamous cell carcinoma
R. P. Ekanayaka, W. M. Tilakaratne
Oral Diseases.2025; 31(5): 1420. CrossRef - Prevalence of human papilloma virus in head and neck mucous squamous cell carcinoma and genotypes by location: an observational study
Emilie Uhlrich, Jerzy Klijanienko, Joey Martin, Emmanuelle Jeannot, Anne Vincent-Salomon, Paul Freneaux, Christophe Le Tourneau, Olivier Choussy, Antoine Dubray-Vautrin
European Journal of Cancer Prevention.2025; 34(5): 426. CrossRef - Risk factors for cervical lymph node metastasis in oropharyngeal cancer and its impact on prognosis
Li Zhang, Zhilin Li, Jing Wang, Chen Wang, Shuxin Wen
Brazilian Journal of Otorhinolaryngology.2025; 91(2): 101520. CrossRef - Co-infection of human papillomavirus genotypes and Epstein-Barr virus in tumors of the oral cavity and oropharynx: a retrospective study in Northeastern Mexico
Gerardo del Carmen Palacios-Saucedo, Jose Manuel Vazquez-Guillen, Alondra Yamileth Alanis-Valdez, Leticia Lizeth Valdez-Treviño, Luis Roberto Galindo-Mendez, Angel Zavala-Pompa, Lydia Guadalupe Rivera-Morales, Ana Carolina Martinez-Torres, Roberto Lopez-V
IJID Regions.2025; 14: 100555. CrossRef - Rates of p16 and p53 expression in head and neck cutaneous squamous cell carcinoma vary according to human papillomavirus status
Rachid Ait Addi
World Journal of Clinical Cases.2025;[Epub] CrossRef - The epidemiological trends and survival of HPV-related oropharyngeal cancer other than tonsils and base of tongue − a systematic review and meta-analysis
Anas Mohammad Al Fadel, Kathrine Kronberg Jakobsen, Lasse Holmgaard Jensen, Amanda-Louise Fenger Carlander, Christian Grønhøj, Christian von Buchwald
Oral Oncology.2025; 165: 107311. CrossRef - Oropharyngeal Helicobacter pylori colonization increases risk and worsens prognosis of head and neck squamous cell carcinoma
Xianyao Jiang, Yongjin Huang, Changwu Li, Hongyan Jiang
Scientific Reports.2025;[Epub] CrossRef - Characteristics of human papillomavirus infection among oropharyngeal cancer patients: A systematic review and meta-analysis
Meimei Cui, Jinling Cheng, Huijuan Cheng, Ming Zhao, Dan Zhou, Min Zhang, Jingjing Jia, Limei Luo
Archives of Oral Biology.2024; 157: 105830. CrossRef - Longitudinal Screening for Oral High-Risk Non-HPV16 and Non-HPV18 Strains of Human Papillomavirus Reveals Increasing Prevalence among Adult and Pediatric Biorepository Samples: A Pilot Study
Jordan Jacobs, Eugene Chon, Karl Kingsley
Vaccines.2024; 12(8): 895. CrossRef - Position Statement about Gender-Neutral HPV Vaccination in Korea
Kyung-Jin Min, Yung-Taek Ouh, Sangrak Bae, Yong-Bae Ji, Jae-Kwan Lee, Jae-Weon Kim, Kwang-Jae Cho, Dong-Hun Im
Vaccines.2024; 12(10): 1110. CrossRef - High-risk HPV Does not Appear to be an Important Risk Factor for Sinonasal Carcinomas in Turkish Population: A Tertiary Center Experience
Evsen Apaydin Arikan, Levent Aydemir, Murat Ulusan, Dilek Yilmazbayhan, Yasemin Ozluk
International Journal of Surgical Pathology.2023; 31(2): 124. CrossRef - Practical Application of Circulating Tumor-Related DNA of Human Papillomavirus in Liquid Biopsy to Evaluate the Molecular Response in Patients with Oropharyngeal Cancer
Agnieszka M. Mazurek, Tomasz W. Rutkowski
Cancers.2023; 15(4): 1047. CrossRef - The Prevalence of HPV in Oral Cavity Squamous Cell Carcinoma
Seyed Keybud Katirachi, Mathias Peter Grønlund, Kathrine Kronberg Jakobsen, Christian Grønhøj, Christian von Buchwald
Viruses.2023; 15(2): 451. CrossRef - The Protective Role of Cranberries and Blueberries in Oral Cancer
César Esquivel-Chirino, Mario Augusto Bolaños-Carrillo, Daniela Carmona-Ruiz, Ambar Lopéz-Macay, Fernando Hernández-Sánchez, Delina Montés-Sánchez, Montserrat Escuadra-Landeros, Luis Alberto Gaitán-Cepeda, Silvia Maldonado-Frías, Beatriz Raquel Yáñez-Ocam
Plants.2023; 12(12): 2330. CrossRef - Unusual cases of sinonasal malignancies: a letter to the editor on HPV-positive sinonasal squamous cell carcinomas
Benedicte Bitsch Lauritzen, Sannia Sjöstedt, Jakob Myllerup Jensen, Katalin Kiss, Christian von Buchwald
Acta Oncologica.2023; 62(6): 608. CrossRef - Prevalence of human Papillomavirus associated oropharyngeal and oral squamous cell carcinoma in Asian countries: A systematic review and large-scale meta-analysis
Yy Jean Tan, Ken Wong Siong Hou, Galvin Sim Siang Lin, Jasmine Lim Suk Wun, Wan Nor Amira Wan Ahmad Abdul Nasir, Lynn Wei Linn Ko
Acta Marisiensis - Seria Medica.2023; 69(2): 77. CrossRef - Top 100 most cited articles on human papillomavirus-induced head and neck squamous cell carcinoma: A bibliographic review
Rahul Mohandas, Subhashree Mohapatra, Mary Oshin, ShubhangiSambhaji Hajare
Journal of International Oral Health.2023; 15(3): 219. CrossRef - Intracellular Toll-Like Receptors Modulate Adaptive Immune Responses in Head and Neck Cancer
Sangeetha K. Nayanar, Deepak Roshan V.G., Shruthi Surendran, Göran Kjeller, Bengt Hasséus, Daniel Giglio
Viral Immunology.2023; 36(10): 659. CrossRef - Positive Rate of Human Papillomavirus and Its Trend in Head and Neck Cancer in South Korea
Hyun Woong Jun, Yong Bae Ji, Chang Myeon Song, Jae Kyung Myung, Hae Jin Park, Kyung Tae
Frontiers in Surgery.2022;[Epub] CrossRef - Transcriptionally active HPV in OPMD and OSCC: A systematic review following the CAP/ASCO guidelines
Laura Borges Kirschnick, Lauren Frenzel Schuch, Maria Eduarda Pérez‐de‐Oliveira, Ana Gabriela Costa Normando, Bruno Augusto Linhares Almeida Mariz, Eliete Neves Silva Guerra, Felipe Martins Silveira, Ana Carolina Uchoa Vasconcelos, Luciana Estevam Simonat
Oral Diseases.2022; 28(8): 2309. CrossRef - Effect of National Oral Health Screening Program on the Risk of Head and Neck Cancer: A Korean National Population-Based
Chan Woo Wee, Hyo-Jung Lee, Jae-Ryun Lee, Hyejin Lee, Min-Jeong Kwoen, Woo-Jin Jeong, Keun-Yong Eom
Cancer Research and Treatment.2022; 54(3): 709. CrossRef - Expression of p16, p53, and TLR9 in HPV-Associated Head and Neck Squamous Cell Carcinoma: Clinicopathological Correlations and Potential Prognostic Significance
Shu Wang, Xibing Zhuang, Caixia Gao, Tiankui Qiao
OncoTargets and Therapy.2021; Volume 14: 867. CrossRef - The Role of Human Papilloma Virus in Dictating Outcomes in Head and Neck Squamous Cell Carcinoma
Shane Brennan, Anne-Marie Baird, Esther O’Regan, Orla Sheils
Frontiers in Molecular Biosciences.2021;[Epub] CrossRef - A Contemporary Systematic Review on Repartition of HPV-Positivity in Oropharyngeal Cancer Worldwide
Amanda F. Carlander, Kathrine K. Jakobsen, Simone K. Bendtsen, Martin Garset-Zamani, Charlotte D. Lynggaard, Jakob Schmidt Jensen, Christian Grønhøj, Christian von Buchwald
Viruses.2021; 13(7): 1326. CrossRef - The Prevalence of High- and Low-Risk Types of HPV in Patients with Squamous Cell Carcinoma of the Head and Neck, Patients with Chronic Tonsillitis, and Healthy Individuals Living in Poland
Joanna Katarzyna Strzelczyk, Krzysztof Biernacki, Jadwiga Gaździcka, Elżbieta Chełmecka, Katarzyna Miśkiewicz-Orczyk, Natalia Zięba, Janusz Strzelczyk, Maciej Misiołek
Diagnostics.2021; 11(12): 2180. CrossRef
- Impact of histopathological parameters in prognosis of oral squamous cell carcinoma
- Gene variant profiles and tumor metabolic activity as measured by FOXM1 expression and glucose uptake in lung adenocarcinoma
- Ashley Goodman, Waqas Mahmud, Lela Buckingham
- J Pathol Transl Med. 2020;54(3):237-245. Published online March 4, 2020
- DOI: https://doi.org/10.4132/jptm.2020.02.08
- 7,535 View
- 120 Download
- 2 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Cancer cells displaying aberrant metabolism switch energy production from oxidative phosphorylation to glycolysis. Measure of glucose standardized uptake value (SUV) by positron emission tomography (PET), used for staging of adenocarcinoma in high-risk patients, can reflect cellular use of the glycolysis pathway. The transcription factor, FOXM1 plays a role in regulation of glycolytic genes. Cancer cell transformation is driven by mutations in tumor suppressor genes such as TP53 and STK11 and oncogenes such as KRAS and EGFR. In this study, SUV and FOXM1 gene expression were compared in the background of selected cancer gene mutations.
Methods
Archival tumor tissue from cases of lung adenocarcinoma were analyzed. SUV was collected from patient records. FOXM1 gene expression was assessed by quantitative reverse transcriptase polymerase chain reaction (qRT-PCR). Gene mutations were detected by allele-specific PCR and gene sequencing.
Results
SUV and FOXM1 gene expression patterns differed in the presence of single and coexisting gene mutations. Gene mutations affected SUV and FOXM1 differently. EGFR mutations were found in tumors with lower FOXM1 expression but did not affect SUV. Tumors with TP53 mutations had increased SUV (p = .029). FOXM1 expression was significantly higher in tumors with STK11 mutations alone (p < .001) and in combination with KRAS or TP53 mutations (p < .001 and p = .002, respectively).
Conclusions
Cancer gene mutations may affect tumor metabolic activity. These observations support consideration of tumor cell metabolic state in the presence of gene mutations for optimal prognosis and treatment strategy. -
Citations
Citations to this article as recorded by- Prognostic value of combining clinical factors, 18F-FDG PET-based intensity, volumetric features, and deep learning predictor in patients with EGFR-mutated lung adenocarcinoma undergoing targeted therapies: a cross-scanner and temporal validation study
Kun-Han Lue, Yu-Hung Chen, Sung-Chao Chu, Chih-Bin Lin, Tso-Fu Wang, Shu-Hsin Liu
Annals of Nuclear Medicine.2024; 38(8): 647. CrossRef
- Prognostic value of combining clinical factors, 18F-FDG PET-based intensity, volumetric features, and deep learning predictor in patients with EGFR-mutated lung adenocarcinoma undergoing targeted therapies: a cross-scanner and temporal validation study
- Morphologic variant of follicular lymphoma reminiscent of hyaline-vascular Castleman disease
- Jiwon Koh, Yoon Kyung Jeon
- J Pathol Transl Med. 2020;54(3):253-257. Published online February 5, 2020
- DOI: https://doi.org/10.4132/jptm.2019.12.17
- 8,580 View
- 240 Download
- 5 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - Follicular lymphoma (FL) with hyaline-vascular Castleman disease (FL-HVCD)-like features is a rare morphologic variant, with fewer than 20 cases in the literature. Herein, we report a case of FL-HVCD in a 37-year-old female who presented with isolated neck lymph node enlargement. The excised lymph node showed features reminiscent of HVCD, including regressed germinal centers (GCs) surrounded by onion skin-like mantle zones, lollipop lesions composed of hyalinized blood vessels penetrating into regressed GCs, and hyalinized interfollicular stroma. In addition, focal areas of abnormally conglomerated GCs composed of homogeneous, small centrocytes with strong BCL2, CD10, and BCL6 expression were observed, indicating partial involvement of the FL. Several other lymphoid follicles showed features of in situ follicular neoplasia. Based on the observations, a diagnosis of FL-HVCD was made. Although FLHVCD is very rare, the possibility of this variant should be considered in cases resembling CD. Identification of abnormal, neoplastic follicles and ancillary immunostaining are helpful for proper diagnosis.
-
Citations
Citations to this article as recorded by- Unicentric Castleman Disease: Illustration of Its Morphologic Spectrum and Review of the Differential Diagnosis
Siba El Hussein, Andrew G. Evans, Hong Fang, Wei Wang, L. Jeffrey Medeiros
Archives of Pathology & Laboratory Medicine.2024; 148(1): 99. CrossRef - Finding a Needle in the Haystack
Hung-Yu Lin, Yi-Jen Peng, Yi-Ying Wu, Ping-Ying Chang
Journal of Medical Sciences.2023; 43(6): 292. CrossRef - Analysis of immunophenotypic features in hyaline vascular type Castleman disease
Yu Chang, Yu Ma, Chen Chang, Wensheng Li
Diagnostic Pathology.2023;[Epub] CrossRef - In‐situ follicular neoplasia: a clinicopathological spectrum
Gurdip S Tamber, Myriam Chévarie‐Davis, Margaret Warner, Chantal Séguin, Carole Caron, René P Michel
Histopathology.2021; 79(6): 1072. CrossRef
- Unicentric Castleman Disease: Illustration of Its Morphologic Spectrum and Review of the Differential Diagnosis
- Colorectal epithelial neoplasm associated with gut-associated lymphoid tissue
- Yo Han Jeon, Ji Hyun Ahn, Hee Kyung Chang
- J Pathol Transl Med. 2020;54(2):135-145. Published online January 29, 2020
- DOI: https://doi.org/10.4132/jptm.2019.11.06
- 10,286 View
- 259 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Colorectal epithelial neoplasm extending into the submucosal gut-associated lymphoid tissue (GALT) can cause difficulties in the differential diagnosis. Regarding GALT-associated epithelial neoplasms, a few studies favor the term “GALT carcinoma” while other studies have mentioned the term “GALT-associated pseudoinvasion/epithelial misplacement (PEM)”.
Methods
The clinicopathologic characteristics of 11 cases of colorectal epithelial neoplasm associated with submucosal GALT diagnosed via endoscopic submucosal dissection were studied.
Results
Eight cases (72.7%) were in males. The median age was 59 years, and age ranged from 53 to 73. All cases had a submucosal tumor component more compatible with GALT-associated PEM. Eight cases (72.7%) were located in the right colon. Ten cases (90.9%) had a non-protruding endoscopic appearance. Nine cases (81.8%) showed continuity between the submucosal and surface adenomatous components. Nine cases showed (81.8%) focal defects or discontinuation of the muscularis mucosae adjacent to the submucosal GALT. No case showed hemosiderin deposits in the submucosa or desmoplastic reaction. No case showed single tumor cells or small clusters of tumor cells in the submucosal GALT. Seven cases (63.6%) showed goblet cells in the submucosa. No cases showed oncocytic columnar cells lining submucosal glands.
Conclusions
Our experience suggests that pathologists should be aware of the differential diagnosis of GALT-associated submucosal extension by colorectal adenomatous neoplasm. Further studies are needed to validate classification of GALT-associated epithelial neoplasms. -
Citations
Citations to this article as recorded by- Redefining GALT-associated carcinoma: a distinct subtype of colorectal adenocarcinoma
Jennifer Fallas, Marianna Arvanitaki, Sophie Lecomte, Jean-Yves Bonnet, Sarah De Clercq, Audrey Verrellen, Nicky D’Haene, María Gómez Galdón, Laurine Verset
Virchows Archiv.2026; 488(3): 695. CrossRef - Family adenomatous polyposis come across dome type adenocarcinoma: a case report and literature review
Ying-Ying Chang, Xiao-Long Zhang, Yao-Hui Wang, Ting-Sheng Ling
Diagnostic Pathology.2025;[Epub] CrossRef - Radiation-induced injury and the gut microbiota: insights from a microbial perspective
Qiaoli Wang, Guoqiang Xu, Ouying Yan, Shang Wang, Xin Wang
Therapeutic Advances in Gastroenterology.2025;[Epub] CrossRef
- Redefining GALT-associated carcinoma: a distinct subtype of colorectal adenocarcinoma
- Comparison of papanicolaou smear and human papillomavirus (HPV) test as cervical screening tools: can we rely on HPV test alone as a screening method? An 11-year retrospective experience at a single institution
- Myunghee Kang, Seung Yeon Ha, Hyun Yee Cho, Dong Hae Chung, Na Rae Kim, Jungsuk An, Sangho Lee, Jae Yeon Seok, Juhyeon Jeong
- J Pathol Transl Med. 2020;54(1):112-118. Published online January 15, 2020
- DOI: https://doi.org/10.4132/jptm.2019.11.29
- 14,862 View
- 269 Download
- 20 Web of Science
- 23 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The decrease in incidence of cervical dysplasia and carcinoma has not been as dramatic as expected with the development of improved research tools and test methods. The human papillomavirus (HPV) test alone has been suggested for screening in some countries. The National Cancer Screening Project in Korea has applied Papanicolaou smears (Pap smears) as the screening method for cervical dysplasia and carcinoma. We evaluated the value of Pap smear and HPV testing as diagnostic screening tools in a single institution.
Methods
Patients co-tested with HPV test and Pap smear simultaneously or within one month of each other were included in this study. Patients with only punch biopsy results were excluded because of sampling errors. A total of 999 cases were included, and the collected reports encompassed results of smear cytology, HPV subtypes, and histologic examinations.
Results
Sensitivity and specificity of detecting high-grade squamous intraepithelial lesion (HSIL) and squamous cell carcinoma (SCC) were higher for Pap smears than for HPV tests (sensitivity, 97.14%; specificity, 85.58% for Pap smears; sensitivity, 88.32%; specificity, 54.92% for HPV tests). HPV tests and Pap smears did not differ greatly in detection of low-grade squamous intraepithelial lesion (85.35% for HPV test, 80.31% for Pap smears). When atypical glandular cells were noted on Pap smears, the likelihood for histologic diagnosis of adenocarcinoma following Pap smear was higher than that of high-risk HPV test results (18.8 and 1.53, respectively).
Conclusions
Pap smears were more useful than HPV tests in the diagnosis of HSIL, SCC, and glandular lesions. -
Citations
Citations to this article as recorded by- Development of a Nano-Real-Time Polymerase Chain Reaction (RT-PCR) Kit for Detection and Genotyping of High-Risk Human Papillomavirus (HPV) Strains Using Dedicated TaqMan Probes
Mohammad Panji, Mohammad Hossein Modarresi, Zahra Azizi, Moloud Absalan, Elahe Motevaseli
Cureus.2026;[Epub] CrossRef - Detection of cervical precancerous lesions and cancer by small-scale RT-qPCR analysis of oppositely deregulated mRNAs pairs in cytological smears
Anastasia A. Artyukh, Mikhail K. Ivanov, Sergei E. Titov, Victoria V. Dzyubenko, Sergey E. Krasilnikov, Anastasia O. Shumeikina, Nikita A. Afanasev, Anastasia V. Malek, Sergei A. Glushkov, Eduard F. Agletdinov
Frontiers in Oncology.2025;[Epub] CrossRef - High burden of abnormal cervical smears in South African primary health care: health programmes implications
Olufemi B Omole, Joel M Francis, John M Musonda, Pumla P Sodo, Elizabeth Reji, Nyundu S J Phukuta, Honey L M Mabuza, Joyce S Musonda, Jimmy Akii, John V Ndimande, Olalekan A Ayo-Yusuf
Health Promotion International.2025;[Epub] CrossRef - Bibliometric analysis: a study of the microenvironment in cervical cancer (2000-2024)
Yun-Tao Zhang, Yan-Ni Wei, Chen-Chen Liu, Mai-Qing Yang
Frontiers in Oncology.2025;[Epub] CrossRef - Liquid biopsy biomarkers in cervical cancer: A systematic review and meta-analysis
Isaac Kinyua Njangiru, Bizhar Ahmed Tayeb, Hazhmat Ali, Rafl M. Kamil
The Journal of Liquid Biopsy.2025; 10: 100328. CrossRef - Diagnostic Utility of Human Papilloma Virus Testing in Comparison with Pap Cytology and Histopathology in Unvaccinated Women with Cervical High-Grade Dysplasia and Carcinoma in Botswana
Patricia Setsile Rantshabeng, Nametso Dire, Andrew Khulekani Ndlovu, Ishmael Kasvosve
Venereology.2025; 4(4): 15. CrossRef - Challenges in the diagmosis of cervical pathologies
D. Y. Chernov, O. A. Tikhonovskaya, S. V. Logvinov, I. A. Petrov, Y. S. Yuriev, A. A. Zhdankina, A. V. Gerasimov, I. V. Zingalyuk, G. A. Mikheenko
Bulletin of Siberian Medicine.2024; 22(4): 201. CrossRef - “Barriers and Advantages of Self-Sampling Tests, for HPV Diagnosis: A Qualitative Field Experience Before Implementation in a Rural Community in Ecuador”
Bernardo Vega-Crespo, Vivian Alejandra Neira, Ruth Maldonado - Rengel, Diana López, Dayanara Delgado-López, Gabriela Guerra Astudillo, Veronique Verhoeven
International Journal of Women's Health.2024; Volume 16: 947. CrossRef - Cervical Human Papillomavirus Testing
Carol N. Rizkalla, Eric C. Huang
Surgical Pathology Clinics.2024; 17(3): 431. CrossRef - Segmentation of Overlapping Cells in Cervical Cytology Images: A Survey
E Chen, Hua-Nong Ting, Joon Huang Chuah, Jun Zhao
IEEE Access.2024; 12: 114170. CrossRef - Knowledge and awareness regarding pap test and HPV typing for cervical cancer screening in Edo North, Nigeria
Amina Momodu, Johnsolomon Eghosa Ohenhen, Godfrey Innocent Iyare, Musa Abidemi Muhibi, Godwin Avwioro
Discover Public Health.2024;[Epub] CrossRef - Colposcopy Value in Young Child-bearing Women: Is New Recommendations Necessary?
Fahimeh Sabet, Avishan Aminizad, Fariba Behnamfar, Tajossadat Allameh, Seyedeh Ghazal Shahrokh, Rostami Koushan, Amirmohammad Taravati, Leila Mousavi Seresht
Advanced Biomedical Research.2024;[Epub] CrossRef - Selection of endogenous control and identification of significant microRNA deregulations in cervical cancer
T. Stverakova, I. Baranova, P. Mikyskova, B. Gajdosova, H. Vosmikova, J. Laco, V. Palicka, H. Parova
Frontiers in Oncology.2023;[Epub] CrossRef - Cytology Versus Molecular Diagnosis of HPV for Cervical Cancer Screening. Comparison of the Diagnostic Properties of Four Tests in a Rural Community of Cuenca Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, Rocío Murillo, Cristina Ochoa Avilés
ESPOCH Congresses: The Ecuadorian Journal of S.T.E.A.M..2023; 3(1): 139. CrossRef - Attitudes towards prevention of cervical cancer and early diagnosis among female academicians
Nurhan Doğan, Gamze Fışkın
Journal of Obstetrics and Gynaecology Research.2022; 48(6): 1433. CrossRef - Role of Self-Sampling for Cervical Cancer Screening: Diagnostic Test Properties of Three Tests for the Diagnosis of HPV in Rural Communities of Cuenca, Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, José Ortíz Segarra, Ruth Maldonado Rengel, Diana López, María Paz Orellana, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, Veronique Verhoeven
International Journal of Environmental Research and Public Health.2022; 19(8): 4619. CrossRef - Utility of Scoring System for Screening and Early Warning of Cervical Cancer Based on Big Data Analysis
Dan Hou, Binjie Yang, Yangdan Li, Ming Sun
Frontiers in Public Health.2022;[Epub] CrossRef - Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, José Ortíz S, Ruth Maldonado-Rengel, Diana López, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, Veronique Verhoeven
Healthcare.2022; 10(9): 1614. CrossRef - Diagnostic distribution and pitfalls of glandular abnormalities in cervical cytology: a 25-year single-center study
Jung-A Sung, Ilias P. Nikas, Haeryoung Kim, Han Suk Ryu, Cheol Lee
Journal of Pathology and Translational Medicine.2022; 56(6): 354. CrossRef - Primary screening of cervical cancer by Pap smear in women of reproductive age group
Ruchi Mishra, Dakshina Bisht, Manisha Gupta
Journal of Family Medicine and Primary Care.2022; 11(9): 5327. CrossRef - Comparison of Learning Transfer Using Simulation Problem-Based Learning and Demonstration: An Application of Papanicolaou Smear Nursing Education
Jeongim Lee, Hae Kyoung Son
International Journal of Environmental Research and Public Health.2021; 18(4): 1765. CrossRef - Investigating host-virus interaction mechanism and phylogenetic analysis of viral proteins involved in the pathogenesis
Ahmad Abu Turab Naqvi, Farah Anjum, Alaa Shafie, Sufian Badar, Abdelbaset Mohamed Elasbali, Dharmendra Kumar Yadav, Md. Imtaiyaz Hassan, Timir Tripathi
PLOS ONE.2021; 16(12): e0261497. CrossRef - Utility of Human Papillomavirus Testing for Cervical Cancer Screening in Korea
Mee-seon Kim, Eun Hee Lee, Moon-il Park, Jae Seok Lee, Kisu Kim, Mee Sook Roh, Hyoun Wook Lee
International Journal of Environmental Research and Public Health.2020; 17(5): 1726. CrossRef
- Development of a Nano-Real-Time Polymerase Chain Reaction (RT-PCR) Kit for Detection and Genotyping of High-Risk Human Papillomavirus (HPV) Strains Using Dedicated TaqMan Probes
- Analysis of the molecular subtypes of preoperative core needle biopsy and surgical specimens in invasive breast cancer
- Ye Sul Jeong, Jun Kang, Jieun Lee, Tae-Kyung Yoo, Sung Hun Kim, Ahwon Lee
- J Pathol Transl Med. 2020;54(1):87-94. Published online November 13, 2019
- DOI: https://doi.org/10.4132/jptm.2019.10.14
- 10,566 View
- 212 Download
- 20 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Accurate molecular classification of breast core needle biopsy (CNB) tissue is important for determining neoadjuvant systemic therapies for invasive breast cancer. The researchers aimed to evaluate the concordance rate (CR) of molecular subtypes between CNBs and surgical specimens.
Methods
This study was conducted with invasive breast cancer patients who underwent surgery after CNB at Seoul St. Mary’s Hospital between December 2014 and December 2017. Estrogen receptor (ER), progesterone receptor (PR), human epidermal growth factor receptor 2 (HER2), and Ki67 were analyzed using immunohistochemistry. ER and PR were evaluated by Allred score (0–8). HER2 was graded from 0 to +3, and all 2+ cases were reflex tested with silver in situ hybridization. The labeling index of Ki67 was counted by either manual scoring or digital image analysis. Molecular subtypes were classified using the above surrogate markers.
Results
In total, 629 patients were evaluated. The CRs of ER, PR, HER2, and Ki67 were 96.5% (kappa, 0.883; p<.001), 93.0% (kappa, 0.824; p<.001), 99.7% (kappa, 0.988; p<.001), and 78.7% (kappa, 0.577; p<.001), respectively. Digital image analysis of Ki67 in CNB showed better concordance with Ki67 in surgical specimens (CR, 82.3%; kappa, 0.639 for digital image analysis vs. CR, 76.2%; kappa, 0.534 for manual counting). The CRs of luminal A, luminal B, HER2, and triple negative types were 89.0%, 70.0%, 82.9%, and 77.2%, respectively.
Conclusions
CNB was reasonably accurate for determining ER, PR, HER2, Ki67, and molecular subtypes. Using digital image analysis for Ki67 in CNB produced more accurate molecular classifications. -
Citations
Citations to this article as recorded by- Predicting the Efficacy of Breast Cancer Neoadjuvant Chemotherapy Using Ultrasonography and Machine Learning
Meihong Jia, Huizhan Li, Wenli Xiao, Jiping Xue, Zhifen Wang, Xia He, Xin Wang, Dianxia Men
Ultrasound in Medicine & Biology.2026; 52(4): 834. CrossRef - Ultrasound viscosity imaging empowers BI-RADS: toward precise breast lesion diagnosis and analysis of HER2 status
Yiming Chen, Jialing Wu, Yiting Liu, Xiukun Hou
Frontiers in Oncology.2026;[Epub] CrossRef - Correlation between ultrasonography and elastography parameters and molecular subtypes of breast cancer in young women
Dian-xia Men, Hui-zhan Li, Juan Dong, Meng-hua Xue, Zhi-fen Wang, Wen-li Xiao, Ji-ping Xue, Mei-hong Jia
Annals of Medicine.2025;[Epub] CrossRef - Concordance of Oncotype DX Breast Recurrence Score Assay Results Between Paired Core Needle Biopsy and Surgical Excision Specimens in Hormone Receptor Positive, Human Epidermal Growth Factor Receptor 2 Negative, Early-Stage Breast Cancer
Aziza Nassar, Jodi Carter, Paige Innis, Andrea Pingitore Blacklock, Jennifer Racz, Matthew Petitt, Purva Singla, Helena Hanna, Abigail Lochala, Christy A. Russell, Minetta C. Liu
JCO Precision Oncology.2025;[Epub] CrossRef - Impact of immunohistochemistry staining conditions on the incidence of human epidermal growth factor receptor 2 (HER2)-low breast cancer
Min Chong Kim, Sun Young Kwon, Hye Ra Jung, Young Kyung Bae
Virchows Archiv.2024; 485(6): 1117. CrossRef - Study on Intratumoral Heterogeneity of Expression of Estrogen Receptor, Progesterone Receptor, and Human Epidermal Growth Factor Receptor 2 in Carcinoma Breast
Ragavi Uthayasuriyan, Sheba K Jacob, Saloni Naresh Shah
Apollo Medicine.2024; 21(1): 51. CrossRef - Concordance of HER2 status between core needle biopsy and surgical resection specimens of breast cancer: an analysis focusing on the HER2-low status
Sei Na, Milim Kim, Yujun Park, Hyun Jung Kwon, Hee-Chul Shin, Eun-Kyu Kim, Mijung Jang, Sun Mi Kim, So Yeon Park
Breast Cancer.2024; 31(4): 705. CrossRef - Concordance of immunohistochemistry for predictive and prognostic factors in breast cancer between biopsy and surgical excision: a single-centre experience and review of the literature
Chiara Rossi, Sara Fraticelli, Marianna Fanizza, Alberta Ferrari, Elisa Ferraris, Alessia Messina, Angelica Della Valle, Chiara Annunziata Pasqualina Anghelone, Angioletta Lasagna, Gianpiero Rizzo, Lorenzo Perrone, Maria Grazia Sommaruga, Giulia Meloni, S
Breast Cancer Research and Treatment.2023; 198(3): 573. CrossRef - Single-center study on clinicopathological and typical molecular pathologic features of metastatic brain tumor
Su Hwa Kim, Young Suk Lee, Sung Hak Lee, Yeoun Eun Sung, Ahwon Lee, Jun Kang, Jae-Sung Park, Sin Soo Jeun, Youn Soo Lee
Journal of Pathology and Translational Medicine.2023; 57(4): 217. CrossRef - The Role of Diffusion-Weighted Imaging Based on Maximum-Intensity Projection in Young Patients with Marked Background Parenchymal Enhancement on Contrast-Enhanced Breast MRI
Ga-Eun Park, Bong-Joo Kang, Sung-hun Kim, Na-Young Jung
Life.2023; 13(8): 1744. CrossRef - Concordance between core needle biopsy and surgical excision specimens for Ki‐67 in breast cancer – a systematic review of the literature
Jahnavi Kalvala, Ruth M Parks, Andrew R Green, Kwok‐Leung Cheung
Histopathology.2022; 80(3): 468. CrossRef - İnvaziv Meme Kanserinde Preoperatif Kor İğne Biyopsi ile Postoperatif Cerrahi Spesmenler Arasında ER, PR, HER2 ve Ki67 Açısından Karşılaştırma
Pınar CELEPLİ, Pelin Seher ÖZTEKİN, Salih CELEPLİ, İrem BİGAT, Sema HÜCÜMENOĞLU
Akdeniz Medical Journal.2022; : 179. CrossRef - Concordance of breast cancer biomarker testing in core needle biopsy and surgical specimens: A single institution experience
Jessica A. Slostad, Nicole K. Yun, Aimee E. Schad, Surbhi Warrior, Louis F. Fogg, Ruta Rao
Cancer Medicine.2022; 11(24): 4954. CrossRef - N-Cadherin Distinguishes Intrahepatic Cholangiocarcinoma from Liver Metastases of Ductal Adenocarcinoma of the Pancreas
Tiemo S. Gerber, Benjamin Goeppert, Anne Hausen, Hagen R. Witzel, Fabian Bartsch, Mario Schindeldecker, Lisa-Katharina Gröger, Dirk A. Ridder, Oscar Cahyadi, Irene Esposito, Matthias M. Gaida, Peter Schirmacher, Peter R. Galle, Hauke Lang, Wilfried Roth,
Cancers.2022; 14(13): 3091. CrossRef - Association of Ki-67 Change Pattern After Core Needle Biopsy and Prognosis in HR+/HER2− Early Breast Cancer Patients
Shuai Li, Xiaosong Chen, Kunwei Shen
Frontiers in Surgery.2022;[Epub] CrossRef - MRI Features for Prediction Malignant Intra-Mammary Lymph Nodes: Correlations with Mammography and Ultrasound
Meejung Kim, Bong Joo Kang, Ga Eun Park
Investigative Magnetic Resonance Imaging.2022; 26(2): 135. CrossRef - A single centre experience in Turkey for comparison between core needle biopsy and surgical specimen evaluation results for HER2, SISH, estrogen receptors and progesterone receptors in breast cancer patients
Hatice Karaman, Fatma Senel, Arzu Tasdemir, Ipek Özer, Merve Dogan
Journal of Cancer Research and Therapeutics.2022; 18(6): 1789. CrossRef - Meme kanseri trucut ve rezeksiyon materyallerinde yeni moleküler sınıflama, tanı ve hormon reseptörlerinin durumu tutarlı mı?
Yeliz ARMAN KARAKAYA, Sevda YILMAZ, Hande KARABAŞ
Pamukkale Medical Journal.2021;[Epub] CrossRef - What shear wave elastography parameter best differentiates breast cancer and predicts its histologic aggressiveness?
Hyunjin Kim, Jeongmin Lee, Bong Joo Kang, Sung Hun Kim
Ultrasonography.2021; 40(2): 265. CrossRef - Risk-based decision-making in the treatment of HER2-positive early breast cancer: Recommendations based on the current state of knowledge
Christian Jackisch, Patricia Cortazar, Charles E. Geyer, Luca Gianni, Joseph Gligorov, Zuzana Machackova, Edith A. Perez, Andreas Schneeweiss, Sara M. Tolaney, Michael Untch, Andrew Wardley, Martine Piccart
Cancer Treatment Reviews.2021; 99: 102229. CrossRef - Factors influencing agreement of breast cancer luminal molecular subtype by Ki67 labeling index between core needle biopsy and surgical resection specimens
Kristina A. Tendl-Schulz, Fabian Rössler, Philipp Wimmer, Ulrike M. Heber, Martina Mittlböck, Nicolas Kozakowski, Katja Pinker, Rupert Bartsch, Peter Dubsky, Florian Fitzal, Martin Filipits, Fanny Carolina Eckel, Eva-Maria Langthaler, Günther Steger, Mich
Virchows Archiv.2020; 477(4): 545. CrossRef
- Predicting the Efficacy of Breast Cancer Neoadjuvant Chemotherapy Using Ultrasonography and Machine Learning
- Clinical Utility of a Fully Automated Microsatellite Instability Test with Minimal Hands-on Time
- Miseon Lee, Sung-Min Chun, Chang Ohk Sung, Sun Y. Kim, Tae W. Kim, Se Jin Jang, Jihun Kim
- J Pathol Transl Med. 2019;53(6):386-392. Published online October 11, 2019
- DOI: https://doi.org/10.4132/jptm.2019.09.25
- 10,156 View
- 235 Download
- 20 Web of Science
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Microsatellite instability (MSI) analysis is becoming increasingly important in many types of tumor including colorectal cancer (CRC). The commonly used MSI tests are either time-consuming or labor-intensive. A fully automated MSI test, the Idylla MSI assay, has recently been introduced. However, its diagnostic performance has not been extensively validated in clinical CRC samples.
Methods
We evaluated 133 samples whose MSI status had been rigorously validated by standard polymerase chain reaction (PCR), clinical nextgeneration sequencing (NGS) cancer panel test, or both. We evaluated the diagnostic performance of the Idylla MSI assay in terms of sensitivity, specificity, and positive and negative predictive values, as well as various sample requirements, such as minimum tumor purity and the quality of paraffin blocks.
Results
Compared with the gold standard results confirmed through both PCR MSI test and NGS, the Idylla MSI assay showed 99.05% accuracy (104/105), 100% sensitivity (11/11), 98.94% specificity (93/94), 91.67% positive predictive value (11/12), and 100% negative predictive value (93/93). In addition, the Idylla MSI assay did not require macro-dissection in most samples and reliably detected MSI-high in samples with approximately 10% tumor purity. The total turnaround time was about 150 minutes and the hands-on time was less than 2 minutes.
Conclusions
The Idylla MSI assay shows good diagnostic performance that is sufficient for its implementation in the clinic to determine the MSI status of at least the CRC samples. In addition, the fully automated procedure requires only a few slices of formalin-fixed paraffin-embedded tissue and might greatly save time and labor. -
Citations
Citations to this article as recorded by- Leveraging Radiomics and Hybrid Quantum–Classical Convolutional Networks for Non-Invasive Detection of Microsatellite Instability in Colorectal Cancer
T. Buvaneswari, M. Ramkumar, Prabhu Venkatesan, R. Sarath Kumar
Molecular Imaging and Biology.2025; 27(2): 227. CrossRef - Molecular Profiling of H-MSI/dMMR/for Endometrial Cancer Patients: “New Challenges in Diagnostic Routine Practice”
Riccardo Adorisio, Giancarlo Troncone, Massimo Barberis, Francesco Pepe
Journal of Molecular Pathology.2024; 5(2): 187. CrossRef - Enhanced Commendable Sensitivity and Specificity for MSI in Colorectal Cancer by a New PCR‐HRM Based 8‐Loci MSI Assay
Xueping Xiang, Xiaojing Ma, Linlin Ying, Hong Zou
Journal of Clinical Laboratory Analysis.2024;[Epub] CrossRef - Endometriumkarzinom: molekulare Klassifikation in der Routinepathologie
Udo Siebolts, Birgid Schömig-Markiefka, Janna Siemanowski-Hrach, Sabine Merkelbach-Bruse
Die Pathologie.2024; 45(5): 347. CrossRef - Integration of rapid PCR testing as an adjunct to NGS in diagnostic pathology services within the UK: evidence from a case series of non-squamous, non-small cell lung cancer (NSCLC) patients with follow-up
Alison Finall, Gareth Davies, Trevor Jones, Gwion Emlyn, Pearl Huey, Anna Mullard
Journal of Clinical Pathology.2023; 76(6): 391. CrossRef - Analytical Validation and Clinical Utilization of the Oncomine Comprehensive Assay Plus Panel for Comprehensive Genomic Profiling in Solid Tumors
Catherine I. Dumur, Ramakrishnan Krishnan, Jorge A. Almenara, Kathleen E. Brown, Kailyn R. Dugan, Christiana Farni, Fatima Z. Ibrahim, Naomi A. Sanchez, Sumra Rathore, Dinesh Pradhan, Jonathan H. Hughes
Journal of Molecular Pathology.2023; 4(2): 109. CrossRef - Performance of Immunohistochemical and Molecular Methods in Detecting Microsatellite Instability in Gastric Cancer: A Multicenter Study
Diogo Sousa Marques, Irene Gullo, Luís Mascarenhas-Lemos, João Ricardo Silva, Catarina Neto do Nascimento, Patrícia Pontes, Lídia Pinho, Luis Cirnes, Xiaogang Wen, Marília Cravo, Fátima Carneiro
Pathobiology.2023; 90(6): 389. CrossRef - Diagnostic mutationnel rapide Idylla™ : applications théranostiques actuelles et futures
Amélie Bourhis, Annabelle Remoué, Laura Samaison, Arnaud Uguen
Annales de Pathologie.2022; 42(4): 329. CrossRef - Comparison of the Idylla™ MSI assay with the Promega™ MSI Analysis System and immunohistochemistry on formalin-fixed paraffin-embedded tissue of endometrial carcinoma: results from an international, multicenter study
Sonia Gatius, Ana Velasco, Mar Varela, Miriam Cuatrecasas, Pedro Jares, Lisa Setaffy, Benjamin Bonhomme, Almudena Santon, Kristina Lindemann, Sabrina Croce, Ben Davidson, Sigurd Lax, Jose Palacios, Xavier Matias-Guiu
Virchows Archiv.2022; 480(5): 1031. CrossRef - Idylla MSI test combined with immunohistochemistry is a valuable and cost effective strategy to search for microsatellite instable tumors of noncolorectal origin
Laura Samaison, Arnaud Uguen
Pathology International.2022; 72(4): 234. CrossRef - Detection of microsatellite instability in a panel of solid tumours with the Idylla MSI Test using extracted DNA
Adrien Pécriaux, Loetitia Favre, Julien Calderaro, Cécile Charpy, Jonathan Derman, Anaïs Pujals
Journal of Clinical Pathology.2021; 74(1): 36. CrossRef - Idylla microsatellite instability assay versus mismatch repair immunohistochemistry: a retrospective comparison in gastric adenocarcinoma
Luke Farmkiss, Ilona Hopkins, Mary Jones
Journal of Clinical Pathology.2021; 74(9): 604. CrossRef - Multi-center real-world comparison of the fully automated Idylla™ microsatellite instability assay with routine molecular methods and immunohistochemistry on formalin-fixed paraffin-embedded tissue of colorectal cancer
Ana Velasco, Fatma Tokat, Jesper Bonde, Nicola Trim, Elisabeth Bauer, Adam Meeney, Wendy de Leng, George Chong, Véronique Dalstein, Lorand L. Kis, Jon A. Lorentzen, Snjezana Tomić, Keeley Thwaites, Martina Putzová, Astrid Birnbaum, Romena Qazi, Vanessa Pr
Virchows Archiv.2021; 478(5): 851. CrossRef - Detection of microsatellite instability with Idylla MSI assay in colorectal and endometrial cancer
Iiris Ukkola, Pirjo Nummela, Annukka Pasanen, Mia Kero, Anna Lepistö, Soili Kytölä, Ralf Bützow, Ari Ristimäki
Virchows Archiv.2021; 479(3): 471. CrossRef - Managing Difficulties of Microsatellite Instability Testing in Endometrial Cancer-Limitations and Advantages of Four Different PCR-Based Approaches
Janna Siemanowski, Birgid Schömig-Markiefka, Theresa Buhl, Anja Haak, Udo Siebolts, Wolfgang Dietmaier, Norbert Arens, Nina Pauly, Beyhan Ataseven, Reinhard Büttner, Sabine Merkelbach-Bruse
Cancers.2021; 13(6): 1268. CrossRef - Evaluation of Micro Satellite Instability and Mismatch Repair Status in Different Solid Tumors: A Multicenter Analysis in a Real World Setting
Umberto Malapelle, Paola Parente, Francesco Pepe, Caterina De Luca, Pasquale Pisapia, Roberta Sgariglia, Mariantonia Nacchio, Gianluca Gragnano, Gianluca Russo, Floriana Conticelli, Claudio Bellevicine, Elena Vigliar, Antonino Iaccarino, Claudia Covelli,
Cells.2021; 10(8): 1878. CrossRef - Novel Biocartis Idylla™ cartridge-based assay for detection of microsatellite instability in colorectal cancer tissues
Andres E. Mindiola-RomeroMD, Donald C. GreenBS, M. Rabie Al-TurkmaniPhD, Kelley N. GodwinBS, Anna C. MackayBS, Laura J. TafeMD, Bing RenMD, Gregory J. TsongalisPhD
Experimental and Molecular Pathology.2020; 116: 104519. CrossRef - Evaluation of 3 molecular-based assays for microsatellite instability detection in formalin-fixed tissues of patients with endometrial and colorectal cancers
Pauline Gilson, Julien Levy, Marie Rouyer, Jessica Demange, Marie Husson, Céline Bonnet, Julia Salleron, Agnès Leroux, Jean-Louis Merlin, Alexandre Harlé
Scientific Reports.2020;[Epub] CrossRef
- Leveraging Radiomics and Hybrid Quantum–Classical Convolutional Networks for Non-Invasive Detection of Microsatellite Instability in Colorectal Cancer
- Current Status of and Perspectives on Cervical Cancer Screening in Korea
- Sung-Chul Lim, Chong Woo Yoo
- J Pathol Transl Med. 2019;53(4):210-216. Published online May 16, 2019
- DOI: https://doi.org/10.4132/jptm.2019.04.11
- 14,386 View
- 278 Download
- 12 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF - Since the introduction of the Papanicolaou (Pap) smear system in 1943, cervicovaginal cytology has been used as a standard screening test for cervical cancer. The dissemination of this test contributed to reductions of the incidence and mortality of cervical cancer worldwide. In Korea, regular health check-ups for industrial workers and their family members were introduced in 1988 and were performed as part of the National Cancer Screening Program in 1999. As a result, the incidence of cervical cancer in Korea has been steadily decreasing. However, about 800 cases of cervical cancer-related deaths are reported each year due to false-negative test results. Hence, new screening methods have been proposed. Liquid-based cytology (LBC) was introduced in 1996 to overcome the limitations of conventional Pap smears. Since then, other LBC methods have been developed and utilized, including the human papilloma virus test—a method with higher sensitivity that requires fewer screenings. In this study, we review current issues and future perspectives related to cervical cancer screening in Korea.
-
Citations
Citations to this article as recorded by- Practice of Cytopathology in Korea: A 40‐Year Evolution Through Standardization, Digital Transformation, and Global Partnership
Yosep Chong, Ran Hong, Hyeong Ju Kwon, Haeryoung Kim, Lucia Kim, Soon Jae Kim, Yoon Jung Choi
Diagnostic Cytopathology.2026; 54(2): 146. CrossRef - A Study on the Workload of Cytotechnologists: Focus on Commercial Laboratories
Eun-Suk PARK
Korean Journal of Clinical Laboratory Science.2025; 57(2): 228. CrossRef - Metastatic Cervical Cancer in the Asia-Pacific Region: Current Treatment Landscape and Barriers
Jeffrey Chee-Hong Goh, Chyong-Huey Lai, Efren Javier Domingo, Jae Hoon Kim, Carmel Spiteri, Danny Hsu, Soo Yeon Ihm, Peng Peng
Cancer Research Communications.2025; 5(8): 1429. CrossRef - Mathematical Assessment of the Roles of Vaccination and Pap Screening on the Burden of HPV and Related Cancers in Korea
Soyoung Park, Hyunah Lim, Abba B. Gumel
Bulletin of Mathematical Biology.2025;[Epub] CrossRef - A questionnaire study on disparity of cervical cancer prevention programs in Asia‐Oceania
Ka Yu Tse, Kimio Ushijima, Ai Ling Tan, Perapong Intasorn, Jitendra Pariyar, Chih‐Long Chang, Efren J. Domingo, Hiralal Konar, Suresh Kumarasamy, Brahmana Askandar Tjokroprawiro, Sarikapan Wilailak
Journal of Obstetrics and Gynaecology Research.2023; 49(4): 1230. CrossRef - Current state of cytopathology residency training: a Korean national survey of pathologists
Uiju Cho, Tae Jung Kim, Wan Seop Kim, Kyo Young Lee, Hye Kyoung Yoon, Hyun Joo Choi
Journal of Pathology and Translational Medicine.2023; 57(2): 95. CrossRef - Meeting the challenges of cervical cancer screening and HPV vaccination in the UK
Roxanne Westwood, Joanna Lavery
Primary Health Care.2022; 32(01): 22. CrossRef - Local and Metastatic Relapses in a Young Woman with Papillary Squamous Cell Carcinoma of the Uterine Cervix
Ha Young Woo, Hyun-Soo Kim
Diagnostics.2022; 12(3): 599. CrossRef - Serum Human Epididymis Protein 4 as a Prognostic Marker in Cervical Cancer
Woo Yeon Hwang, Dong Hoon Suh, Kidong Kim, Yong Beom Kim, Jae Hong No
Cancer Control.2022;[Epub] CrossRef - HPV detection and/or cytological diagnostics
Sanja Milenković
Glasnik javnog zdravlja.2022; 96(3): 313. CrossRef - Clinical management of abnormal Pap tests: differences between US and Korean guidelines
Seyeon Won, Mi Kyoung Kim, Seok Ju Seong
Journal of Pathology and Translational Medicine.2020; 54(3): 213. CrossRef - Current status of cytopathology practices in Korea: annual report on the Continuous Quality Improvement program of the Korean Society for Cytopathology for 2018
Yosep Chong, Haeyoen Jung, Jung-Soo Pyo, Soon Won Hong, Hoon Kyu Oh
Journal of Pathology and Translational Medicine.2020; 54(4): 318. CrossRef - Cytomorphological Features of Hyperchromatic Crowded Groups in Liquid-Based Cervicovaginal Cytology: A Single Institutional Experience
Youngeun Lee, Cheol Lee, In Ae Park, Hyoung Jin An, Haeryoung Kim
Journal of Pathology and Translational Medicine.2019; 53(6): 393. CrossRef
- Practice of Cytopathology in Korea: A 40‐Year Evolution Through Standardization, Digital Transformation, and Global Partnership
- Frozen Cytology of Meningeal Malignant Solitary Fibrous Tumor/Hemangiopericytoma
- Myunghee Kang, Na Rae Kim, Dong Hae Chung, Gie-Taek Yie
- J Pathol Transl Med. 2019;53(3):192-197. Published online April 11, 2019
- DOI: https://doi.org/10.4132/jptm.2019.03.20
- 8,230 View
- 160 Download
- 7 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF - A 51-year-old woman presented with severe dizziness. The brain magnetic resonance image revealed a 5.5 cm multiloculated mass with a thick rim in the left temporal lobe. Cytological examination of frozen diagnosis of the mass showed hypercellular sheets of round and rhabdoid cells in a hemorrhagic background, and two mitotic figures were observed. Histologically, the excised dura-based mass consisted of predominantly round cells with small foci of rhabdoid tumor cells in a pseudoalveolar pattern in a hemorrhagic background, and the cells showed nuclear positivity for signal transducer and activator of transcription 6 as well as frequent mitosis. The mass was diagnosed as a grade 3 solitary fibrous tumor (SFT)/hemangiopericytoma (HPC). The cytological diagnosis of SFT/HPC is challenging because of the heterogeneous cytological findings, such as histological heterogeneity, and because there are no standardized cytological criteria for malignant SFT/HPC. Cytological findings, such as singly scattered small cells, hypercellularity, rare ropy collagen, and round and rhabdoid cells with pseudoalveolar pattern, may assist in the diagnosis of malignant SFT/HPC.
-
Citations
Citations to this article as recorded by- A Rare Case of Cervical Solitary Fibrous Tumor in a Pediatric Patient: Case Report and Literature Review
Eleonora Becattini, Lorenzo Sgarbanti, Giuseppina Bevacqua, Valentina Grespi, Carlo Conti
NeuroSci.2025; 6(2): 49. CrossRef - Meningeal Solitary Fibrous Tumor: A Cytological Report With Emphasis on the Usefulness of Immunocytochemical Analysis for STAT6
Hiroyuki Okanishi, Mitsuaki Ishida, Naoto Kohno, Isako Kataoka, Mari Tomiuka, Mayumi Uragami, Shizuka Ono, Chihiro Deguchi, Reika Takeda, Yoshitaka Kurisu, Yoshinobu Hirose
Diagnostic Cytopathology.2025;[Epub] CrossRef - Cytologic features of mesenchymal, melanocytic and haematolymphoid tumours of the central nervous system and metastases
Carmen Bárcena, José A. Jiménez‐Heffernan
Cytopathology.2024; 35(5): 590. CrossRef - A Hemangiopericytoma in the External Auditory Canal: A Rare Clinical Presentation and Management
Vaibhavi Patil, Prasad Deshmukh, Sagar S Gaurkar , Ayushi Ghosh Moulic, Jasleen Kaur
Cureus.2024;[Epub] CrossRef - Scoring system for intraoperative diagnosis of intracranial schwannoma by squash cytology
Hirotaka Fujita, Takuma Tajiri, Tomohisa Machida, Nozomi Nomura, Suguru Toguchi, Hitoshi Itoh, Shinichiro Hiraiwa, Tomoko Sugiyama, Chie Inomoto, Masaaki Imai, Shinri Oda, Masami Shimoda, Naoya Nakamura
Cytopathology.2022; 33(2): 196. CrossRef - Occurrence of a solitary fibrous tumor adjacent to the resection bed of a high-grade meningioma: A case report
Coby Cunningham, Rocco Dabecco, Justin Davanzo
Interdisciplinary Neurosurgery.2021; 25: 101277. CrossRef - A case of solitary fibrous tumor arising in the meninge
Saori NAKANISHI, Naoto KURODA, Toshiko TAKAI, Mari KOJIMA, Misato OONOGI
The Journal of the Japanese Society of Clinical Cytology.2021; 60(4): 224. CrossRef - Intraoperative frozen cytology of intraosseous cystic meningioma in the sphenoid bone
Na Rae Kim, Gie-Taek Yie
Journal of Pathology and Translational Medicine.2020; 54(6): 508. CrossRef
- A Rare Case of Cervical Solitary Fibrous Tumor in a Pediatric Patient: Case Report and Literature Review
- Human Leukocyte Antigen Class I and Programmed Death-Ligand 1 Coexpression Is an Independent Poor Prognostic Factor in Adenocarcinoma of the Lung
- Yeon Bi Han, Hyun Jung Kwon, Soo Young Park, Eun-Sun Kim, Hyojin Kim, Jin-Haeng Chung
- J Pathol Transl Med. 2019;53(2):86-93. Published online January 14, 2019
- DOI: https://doi.org/10.4132/jptm.2018.12.26
- 8,169 View
- 136 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Both human leukocyte antigen (HLA) class I and programmed death-ligand 1 (PD-L1) molecules are known to play important roles in cancer immunity. In this study, we evaluated HLA class I expression in resected adenocarcinoma of the lung, and investigated its prognostic impact in correlation with PD-L1 expression.
Methods
HLA class I and PD-L1 expression was evaluated by immunohistochemistry in a total of 403 resected lung adenocarcinomas using tissue microarray. Correlations between the expression of HLA class I/PD-L1 and clinicopathologic features and prognostic significance were analyzed.
Results
HLA class I expression was reduced in 91.6% of adenocarcinoma, and more frequently reduced in patients with younger age, absence of vascular invasion, and low pathologic stage (p = .033, p = .007, and p = .012, respectively). Positive PD-L1 expression in tumor cells was 16.1% (1% cut-off), and associated with poor differentiation, presence of vascular invasion and nodal metastasis (p < .001, p = .002, and p = .032, respectively). On survival analysis, HLA class I or PD-L1 expression alone did not show any statistical significance. On the integrated analysis, HLA class I (+)/PD-L1 (+) subgroup showed a significantly shorter overall survival than other groups (p = .001). Multivariate analysis revealed that coexpression of HLA class I and PD-L1 was an independent poor prognostic factor of lung adenocarcinoma. (p < .001; hazard ratio, 6.106; 95% confidence interval, 2.260 to 16.501).
Conclusions
Lung adenocarcinoma with coexpression of HLA class I and PD-L1 was associated with poor prognosis. This subgroup may evade immune attack by expressing PD-L1 protein despite HLA expression. -
Citations
Citations to this article as recorded by- Assessment of cancer cell‐expressed HLA class I molecules and their immunopathological implications
Terufumi Kubo, Shiori Asano, Kenta Sasaki, Kenji Murata, Takayuki Kanaseki, Tomohide Tsukahara, Yoshihiko Hirohashi, Toshihiko Torigoe
HLA.2024;[Epub] CrossRef - Prognostic and Clinical Significance of Human Leukocyte Antigen Class I Expression in Breast Cancer: A Meta-Analysis
Weiqiang Qiao, Zhiqiang Jia, Wanying Guo, Qipeng Liu, Xiao Guo, Miao Deng
Molecular Diagnosis & Therapy.2023; 27(5): 573. CrossRef - Loss of HLA-class-I expression in non-small-cell lung cancer: Association with prognosis and anaerobic metabolism
Ioannis M. Koukourakis, Alexandra Giatromanolaki, Achilleas Mitrakas, Michael I. Koukourakis
Cellular Immunology.2022; 373: 104495. CrossRef
- Assessment of cancer cell‐expressed HLA class I molecules and their immunopathological implications
- Adrenal Cortical Neoplasm with Uncertain Malignant Potential Arising in the Heterotopic Adrenal Cortex in the Liver of a Patient with Beckwith-Wiedemann Syndrome
- Eun Na Kim, Dong Eun Song, Hee Mang Yoon, Beom Hee Lee, Chong Jai Kim
- J Pathol Transl Med. 2019;53(2):129-135. Published online November 26, 2018
- DOI: https://doi.org/10.4132/jptm.2018.11.13
- 7,981 View
- 110 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Patients with Beckwith-Wiedemann syndrome (BWS) are predisposed to developing embryonal tumors, with hepatoblastoma being the most common type. Our patient showed hemihypertrophy, macroglossia, and paternal uniparental disomy in chromosome 11 and was diagnosed with BWS. When the patient was 9 months old, a 2.5×1.5 cm oval hypoechoic exophytic mass was detected in the inferior tip of his right liver. Preoperative imaging identified it as hepatoblastoma; however, histologic, immunohistochemistry, and electron microscopic findings were compatible with adrenal cortical neoplasm with uncertain malignant potential. The origin of the adrenal tissue seemed to be heterotopic. Here, we describe for the first time an adrenal cortical neoplasm with uncertain malignant potential arising in the heterotopic adrenal cortex located in the liver of a patient with BWS.
-
Citations
Citations to this article as recorded by- Adrenocortical tumors and hereditary syndromes
Kanakamani Jeyaraman, Paola Concolino, Henrik Falhammar
Expert Review of Endocrinology & Metabolism.2025; 20(1): 1. CrossRef - Functional adrenocortical carcinoma with adrenohepatic fusion: A case report
Pastor Escárcega-Fujigaki, Guillermo Hernández-Peredo Rezk, José de Jesús Loeza- Oliva, Anallely Luna-Hernández, Bethsaida Natali Arreguín-Cortés, Rafael López-Cruz
Journal of Pediatric Surgery Case Reports.2024; 107: 102841. CrossRef - Molecular and Clinical Features of Adrenocortical Tumors in Beckwith–Wiedemann Spectrum
Diana Carli, Federico Rondot, Maria Luca, Anna Campello, Stefano Gabriele Vallero, Elisa Tirtei, Andrea Gazzin, Simona Cardaropoli, Francesca Montanari, Claudio Graziano, Paola Quarello, Abu Saadat, Angela Sparago, Giovanni Battista Ferrero, Franca Fagiol
Cancers.2024; 16(23): 3967. CrossRef - Beckwith–Wiedemann syndrome: Clinical, histopathological and molecular study of two Tunisian patients and review of literature
Hela Sassi, Yasmina Elaribi, Houweyda Jilani, Imen Rejeb, Syrine Hizem, Molka Sebai, Nadia Kasdallah, Habib Bouthour, Samia Hannachi, Jasmin Beygo, Ali Saad, Karin Buiting, Dorra H’mida Ben‐Brahim, Lamia BenJemaa
Molecular Genetics & Genomic Medicine.2021;[Epub] CrossRef - Adrenocortical Tumors in Children With Constitutive Chromosome 11p15 Paternal Uniparental Disomy: Implications for Diagnosis and Treatment
Emilia Modolo Pinto, Carlos Rodriguez-Galindo, Catherine G. Lam, Robert E. Ruiz, Gerard P. Zambetti, Raul C. Ribeiro
Frontiers in Endocrinology.2021;[Epub] CrossRef
- Adrenocortical tumors and hereditary syndromes
- Let Archived Paraffin Blocks Be Utilized for Research with Waiver of Informed Consent
- Yong-Jin Kim, Jeong Sik Park, Karam Ko, Chang Rok Jeong
- J Pathol Transl Med. 2018;52(3):141-147. Published online April 5, 2018
- DOI: https://doi.org/10.4132/jptm.2018.02.07
- 10,976 View
- 144 Download
- 3 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - Advances in biomedical and genetic research have contributed to more effective public health improvement via bench-to-bed research and the emergence of personalized medicine. This has certainly showcased the importance of archived human tissues, especially paraffin-embedded blocks in pathology. Currently in Korea, undue legislative regulations of the Bioethics and Safety Act suspend and at times discourage studies from taking place. In this paper, the authors underline the value of paraffin blocks in the era of personalized and translational medicine. We discuss detailed clauses regarding the applicability of paraffin blocks from a legal perspective and compare Korea’s regulations with those of other countries. The necessity for allowing waived consent and Institutional Review Board (IRB) approval will be argued throughout. The authors suggest that researchers declare the following to obtain IRB approval and waiver of informed consents: research could not be practically carried out without a waiver of consent; the proposed research presents no more than minimal risk of harm to subjects, and the waiver of consent will not adversely affect the rights and welfare of subjects; and research will not utilize a tissue block if only 1 is available for each subject, to allow future clinical use such as re-evaluation or further studies.
-
Citations
Citations to this article as recorded by- Investigating GILZ and SGK-1 in Oral Lesions: Biomarker Potential in Malignant Transformation
Soo Min Lee, Nur S. Ismail, Dina M. Saleh
Journal of Current Research in Oral Surgery.2025; 5(1): 70. CrossRef - NaV1.7 channels are expressed in the lower airways of the human respiratory tract
Everardo Hernández-Plata, Ana Alfaro Cruz, Carina Becerril
Respiratory Physiology & Neurobiology.2023; 311: 104034. CrossRef - Expression Profiles of GILZ and SGK-1 in Potentially Malignant and Malignant Human Oral Lesions
Mahmood S. Mozaffari, Rafik Abdelsayed
Frontiers in Oral Health.2021;[Epub] CrossRef - IRB review points for studies utilizing paraffin blocks archived in the pathology laboratory
Yong-Jin Kim, Chang Rok Jeong, Jeong Sik Park
Yeungnam University Journal of Medicine.2018; 35(1): 36. CrossRef
- Investigating GILZ and SGK-1 in Oral Lesions: Biomarker Potential in Malignant Transformation
- The Smad4/PTEN Expression Pattern Predicts Clinical Outcomes in Colorectal Adenocarcinoma
- Yumin Chung, Young Chan Wi, Yeseul Kim, Seong Sik Bang, Jung-Ho Yang, Kiseok Jang, Kyueng-Whan Min, Seung Sam Paik
- J Pathol Transl Med. 2018;52(1):37-44. Published online October 23, 2017
- DOI: https://doi.org/10.4132/jptm.2017.10.20
- 13,265 View
- 235 Download
- 13 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Smad4 and PTEN are prognostic indicators for various tumor types. Smad4 regulates tumor suppression, whereas PTEN inhibits cell proliferation. We analyzed and compared the performance of Smad4 and PTEN for predicting the prognosis of patients with colorectal adenocarcinoma.
Methods
Combined expression patterns based on Smad4+/– and PTEN+/– status were evaluated by immunostaining using a tissue microarray of colorectal adenocarcinoma. The relationships between the protein expression and clinicopathological variables were analyzed.
Results
Smad4–/PTEN– status was most frequently observed in metastatic adenocarcinoma, followed by primary adenocarcinoma and tubular adenoma (p<.001). When Smad4–/PTEN– and Smad4+/PTEN+ groups were compared, Smad4–/PTEN– status was associated with high N stage (p=.018) and defective mismatch repair proteins (p=.006). Significant differences in diseasefree survival and overall survival were observed among the three groups (Smad4+/PTEN+, Smad4–/PTEN+ or Smad4+/PTEN–, and Smad4–/PTEN–) (all p<.05).
Conclusions
Concurrent loss of Smad4 and PTEN may lead to more aggressive disease and poor prognosis in patients with colorectal adenocarcinoma compared to the loss of Smad4 or PTEN alone. -
Citations
Citations to this article as recorded by- Precision oncolytic viral therapy in colorectal cancer: Genetic targeting and immune modulation for personalized treatment (Review)
Muhammad Haris Sultan, Qi Zhan, Yigang Wang, Yulong Xia, Xiaoyuan Jia
International Journal of Molecular Medicine.2025; 56(1): 1. CrossRef - Focal Adhesion Kinase Intersects With the BRD4‐MYC Axis and YAP1 to Drive Tumor Cell Growth, Phenotypic Plasticity, Stemness, and Metastatic Potential in Colorectal Cancer
Rongbo Han, Junfeng Shi, Kai Cheng, Zian Wang, Yecang Chen, Orion Spellecy, Abu Saleh Mosa Faisal, Isha Aryal, Jinfei Chen, Rolf Craven, Olivier Thibault, Lauren Baldwin, Lawrence D. Brewer, Sonia Erfani, Chi Wang, Zhenheng Guo, Eric Chen, Burton Yang, Fr
Cancer Medicine.2025;[Epub] CrossRef - Association between the expression of epithelial–mesenchymal transition (EMT)-related markers and oncologic outcomes of colorectal cancer
Mona Hany Emile, Sameh Hany Emile, Amr Awad El-Karef, Mohamed Awad Ebrahim, Ibrahim Eldosoky Mohammed, Dina Abdallah Ibrahim
Updates in Surgery.2024; 76(6): 2181. CrossRef - The Potential Role of Genomic Signature in Stage II Relapsed Colorectal Cancer (CRC) Patients: A Mono-Institutional Study
Michela Roberto, Giulia Arrivi, Emanuela Pilozzi, Andrea Montori, Genoveffa Balducci, Paolo Mercantini, Andrea Laghi, Debora Ierinò, Martina Panebianco, Daniele Marinelli, Silverio Tomao, Paolo Marchetti, Federica Mazzuca
Cancer Management and Research.2022; Volume 14: 1353. CrossRef - Alterations of PTEN and SMAD4 methylation in diagnosis of breast cancer: implications of methyl II PCR assay
Menha Swellam, Entsar A. Saad, Shimaa Sabry, Adel Denewer, Camelia Abdel Malak, Amr Abouzid
Journal of Genetic Engineering and Biotechnology.2021; 19(1): 54. CrossRef - E3 ubiquitin ligase HECW1 promotes the metastasis of non-small cell lung cancer cells through mediating the ubiquitination of Smad4
Chen Lu, Guangyao Ning, Panpan Si, Chunsheng Zhang, Wenjian Liu, Wei Ge, Kai Cui, Renquan Zhang, Shenglin Ge
Biochemistry and Cell Biology.2021; 99(5): 675. CrossRef - Computational quantification of global effects induced by mutations and drugs in signaling networks of colorectal cancer cells
Sara Sommariva, Giacomo Caviglia, Silvia Ravera, Francesco Frassoni, Federico Benvenuto, Lorenzo Tortolina, Nicoletta Castagnino, Silvio Parodi, Michele Piana
Scientific Reports.2021;[Epub] CrossRef - Clinicopathological characterization of SMAD4-mutated intestinal adenocarcinomas: A case-control study
Xiaoyan Liao, Yansheng Hao, Xiaofei Zhang, Stephen Ward, Jane Houldsworth, Alexandros D. Polydorides, Noam Harpaz, Aldo Scarpa
PLOS ONE.2019; 14(2): e0212142. CrossRef - Clinicopathological Characterization and Prognostic Implication of SMAD4 Expression in Colorectal Carcinoma
Seung-Yeon Yoo, Ji-Ae Lee, Yunjoo Shin, Nam-Yun Cho, Jeong Mo Bae, Gyeong Hoon Kang
Journal of Pathology and Translational Medicine.2019; 53(5): 289. CrossRef - Dissecting the therapeutic implications of the complex SMAD4 regulatory network in metastatic colorectal cancer
Ion Cristóbal, Blanca Torrejón, Andrea Santos, Melani Luque, Marta Sanz-Alvarez, Federico Rojo, Jesús García-Foncillas
European Journal of Surgical Oncology.2018; 44(8): 1283. CrossRef - Reply to: Dissecting the therapeutic implications of the complex SMAD4 regulatory network in metastatic colorectal cancer
Jordan M. Cloyd, Takashi Mizuno, Jean-Nicolas Vauthey
European Journal of Surgical Oncology.2018; 44(8): 1285. CrossRef
- Precision oncolytic viral therapy in colorectal cancer: Genetic targeting and immune modulation for personalized treatment (Review)
- Implication of PHF2 Expression in Clear Cell Renal Cell Carcinoma
- Cheol Lee, Bohyun Kim, Boram Song, Kyung Chul Moon
- J Pathol Transl Med. 2017;51(4):359-364. Published online June 13, 2017
- DOI: https://doi.org/10.4132/jptm.2017.03.16
- 9,496 View
- 168 Download
- 11 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Clear cell renal cell carcinoma (CCRCC) is presumed to be associated with adipogenic differentiation. Histone modification is known to be important for adipogenesis, and the function of histone demethylase plant homeodomain finger 2 (PHF2) has been noted. In addition, PHF2 may act as a tumor suppressor via epigenetic regulation of p53 and is reported to be reduced in colon cancer and stomach cancer tissues. In this study, we examined PHF2 expression in CCRCC specimens by immunohistochemistry.
Methods
We studied 254 CCRCCs and 56 non-neoplastic renal tissues from patients who underwent radical or partial nephrectomy between 2000 and 2003 at the Seoul National University Hospital. Tissue microarray blocks were prepared, and immunohistochemical staining for PHF2 was performed.
Results
Among 254 CCRCC cases, 150 cases (59.1%) showed high expression and 104 cases (40.1%) showed low expression. High expression of PHF2 was significantly correlated with a low Fuhrman nuclear grade (p < .001), smaller tumor size (p < .001), low overall stage (p = .003), longer cancer-specific survival (p = .002), and progression-free survival (p < .001) of the patients. However, it was not an independent prognostic factor in multivariate analysis adjusted for Fuhrman nuclear grade and overall stage.
Conclusions
Our study showed that low expression of PHF2 is associated with aggressiveness and poor prognosis of CCRCC. -
Citations
Citations to this article as recorded by- The role of histone demethylase PHF2 as a tumour suppressor in hepatocellular carcinoma by regulating SRXN1
Dexter Kai Hao Thng, Lissa Hooi, Wai Khang Yong, Dennis Kappei, Tan Boon Toh, Edward Kai-Hua Chow
Oncogenesis.2026;[Epub] CrossRef - Phosphoproteomics identifies determinants of PAK inhibitor sensitivity in leukaemia cells
Pedro Casado, Santiago Marfa, Marym M. Hadi, Henry Gerdes, Sandra M. Martin-Guerrero, Farideh Miraki-Moud, Vinothini Rajeeve, Pedro R. Cutillas
Cell Communication and Signaling.2025;[Epub] CrossRef - The role of histone methylation in renal cell cancer: an update
Yanguang Hou, Yan Yuan, Yanze Li, Lei Wang, Juncheng Hu, Xiuheng Liu
Molecular Biology Reports.2023; 50(3): 2735. CrossRef - Phosphorylation of PHF2 by AMPK releases the repressive H3K9me2 and inhibits cancer metastasis
Ying Dong, Hao Hu, Xuan Zhang, Yunkai Zhang, Xin Sun, Hanlin Wang, Weijuan Kan, Min-jia Tan, Hong Shi, Yi Zang, Jia Li
Signal Transduction and Targeted Therapy.2023;[Epub] CrossRef - HIF-1α-mediated augmentation of miRNA-18b-5p facilitates proliferation and metastasis in osteosarcoma through attenuation PHF2
Peng Luo, Yan-dong Zhang, Feng He, Chang-jun Tong, Kai Liu, He Liu, Shi-zhuang Zhu, Jian-zhou Luo, Bing Yuan
Scientific Reports.2022;[Epub] CrossRef - Integration of meta-analysis and supervised machine learning for pattern recognition in breast cancer using epigenetic data
Reza Panahi, Esmaeil Ebrahimie, Ali Niazi, Alireza Afsharifar
Informatics in Medicine Unlocked.2021; 24: 100629. CrossRef - PHF2 regulates homology-directed DNA repair by controlling the resection of DNA double strand breaks
Ignacio Alonso-de Vega, Maria Cristina Paz-Cabrera, Magdalena B Rother, Wouter W Wiegant, Cintia Checa-Rodríguez, Juan Ramón Hernández-Fernaud, Pablo Huertas, Raimundo Freire, Haico van Attikum, Veronique A J Smits
Nucleic Acids Research.2020; 48(9): 4915. CrossRef - Emerging of lysine demethylases (KDMs): From pathophysiological insights to novel therapeutic opportunities
Sarder Arifuzzaman, Mst Reshma Khatun, Rabeya Khatun
Biomedicine & Pharmacotherapy.2020; 129: 110392. CrossRef - Biology and targeting of the Jumonji-domain histone demethylase family in childhood neoplasia: a preclinical overview
Tyler S. McCann, Lays M. Sobral, Chelsea Self, Joseph Hsieh, Marybeth Sechler, Paul Jedlicka
Expert Opinion on Therapeutic Targets.2019; 23(4): 267. CrossRef - MiR-221 Promotes Hepatocellular Carcinoma Cells Migration via Targeting PHF2
Yi Fu, Mingyan Liu, Fengxia Li, Li Qian, Ping Zhang, Fengwei Lv, Wenting Cheng, Ruixing Hou
BioMed Research International.2019; 2019: 1. CrossRef - PHF2 histone demethylase prevents DNA damage and genome instability by controlling cell cycle progression of neural progenitors
Stella Pappa, Natalia Padilla, Simona Iacobucci, Marta Vicioso, Elena Álvarez de la Campa, Claudia Navarro, Elia Marcos, Xavier de la Cruz, Marian A. Martínez-Balbás
Proceedings of the National Academy of Sciences.2019; 116(39): 19464. CrossRef - Plant homeodomain finger protein 2 as a novel IKAROS target in acute lymphoblastic leukemia
Zheng Ge, Yan Gu, Qi Han, Justin Sloane, Qinyu Ge, Goufeng Gao, Jinlong Ma, Huihui Song, Jiaojiao Hu, Baoan Chen, Sinisa Dovat, Chunhua Song
Epigenomics.2018; 10(1): 59. CrossRef
- The role of histone demethylase PHF2 as a tumour suppressor in hepatocellular carcinoma by regulating SRXN1
- Perivascular Epithelioid Cell Tumor in the Stomach
- Sun Ah Shin, Jiwoon Choi, Kyung Chul Moon, Woo Ho Kim
- J Pathol Transl Med. 2017;51(4):428-432. Published online April 4, 2017
- DOI: https://doi.org/10.4132/jptm.2016.09.16
- 10,083 View
- 141 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF - Perivascular epithelioid cell tumors or PEComas can arise in any location in the body. However, a limited number of cases of gastric PEComa have been reported. We present two cases of gastric PEComas. The first case involved a 62-year-old woman who presented with a 4.2 cm gastric subepithelial mass in the prepyloric antrum, and the second case involved a 67-year-old man with a 5.0 cm mass slightly below the gastroesophageal junction. Microscopic examination revealed that both tumors were composed of perivascular epithelioid cells that were immunoreactive for melanocytic and smooth muscle markers. Prior to surgery, the clinical impression of both tumors was gastrointestinal stromal tumor (GIST), and the second case was erroneously diagnosed as GIST even after microscopic examination. Although gastric PEComa is a very rare neoplasm, it should be considered in the differential diagnosis of gastric submucosal lesions.
-
Citations
Citations to this article as recorded by- Extra-uterine Endometrial Stromal Sarcoma of the Stomach Mimicking a Gastrointestinal Stromal Tumour: A Case Report
Adam Mylonakis, Eleandros Kyros, Maria Karakeke, Eleni Karakeke, Andreas Panagakis, Pagona Kastanaki, Lysandros Karydakis, Alexandros Pergaris, Stratigoula Sakellariou, Alexandros Papalampros
Cureus.2026;[Epub] CrossRef - A Perivascular Epithelioid Cell Tumor in the Ascending Colon: A Rare Case Involving a Patient With Tuberous Sclerosis
Kai Seharada, Masato Kitazawa, Satoshi Nakamura, Yuta Yamamoto, Yuji Soejima
Cureus.2025;[Epub] CrossRef - Malignant Perivascular Epithelioid Cell Tumor of Ovary: A Rare Case Report
Anuradha Sharma, Reetika Sharma, Jyoti Bala, Monika Sharma
Journal of Mid-life Health.2025; 16(1): 107. CrossRef - Unusual paediatric sigmoid perivascular epithelioid cell tumour with regional lymph node metastasis treated using gemcitabine and docetaxel: a case report and literature review
Hsiu-Chung Cheng, Chia-Yu Kuo, Ching-Wen Huang, Hsiang-Hung Shih, Chih-Hung Lin, Jaw-Yuan Wang
Journal of International Medical Research.2021;[Epub] CrossRef - Gastric Perivascular Epithelioid Cell Tumor (PEComa)
Jinghong Xu, Yu Yan, Xueping Xiang, Peter Jiang, Xiangrong Hu, Wenjun Yang
American Journal of Clinical Pathology.2019; 152(2): 221. CrossRef - Robotic wedge resection of a rare gastric perivascular epithelioid cell tumor: A case report
Alessandra Marano, Francesca Maione, Yanghee Woo, Luca Pellegrino, Paolo Geretto, Diego Sasia, Mirella Fortunato, Giulio Fraternali Orcioni, Roberto Priotto, Renato Fasoli, Felice Borghi
World Journal of Clinical Cases.2019; 7(23): 4011. CrossRef
- Extra-uterine Endometrial Stromal Sarcoma of the Stomach Mimicking a Gastrointestinal Stromal Tumour: A Case Report
- Detection of Human Papillomavirus in Korean Breast Cancer Patients by Real-Time Polymerase Chain Reaction and Meta-Analysis of Human Papillomavirus and Breast Cancer
- Jinhyuk Choi, Chungyeul Kim, Hye Seung Lee, Yoo Jin Choi, Ha Yeon Kim, Jinhwan Lee, Hyeyoon Chang, Aeree Kim
- J Pathol Transl Med. 2016;50(6):442-450. Published online October 10, 2016
- DOI: https://doi.org/10.4132/jptm.2016.07.08
- 14,496 View
- 226 Download
- 16 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) is a well-established oncogenic virus of cervical, anogenital, and oropharyngeal cancer. Various subtypes of HPV have been detected in 0% to 60% of breast cancers. The roles of HPV in the carcinogenesis of breast cancer remain controversial. This study was performed to determine the prevalence of HPV-positive breast cancer in Korean patients and to evaluate the possibility of carcinogenic effect of HPV on breast.
Methods
Meta-analysis was performed in 22 case-control studies for HPV infection in breast cancer. A total of 123 breast cancers, nine intraductal papillomas and 13 nipple tissues of patients with proven cervical HPV infection were tested by real-time polymerase chain reaction to detect 28 subtypes of HPV. Breast cancers were composed of 106 formalin-fixed and paraffin embedded (FFPE) breast cancer samples and 17 touch imprint cytology samples of breast cancers.
Results
The overall odds ratio between breast cancer and HPV infection was 5.43 (95% confidence interval, 3.24 to 9.12) with I2 = 34.5% in meta-analysis of published studies with case-control setting and it was statistically significant. HPV was detected in 22 cases of breast cancers (17.9%) and two cases of intaductal papillomas (22.2%). However, these cases had weak positivity.
Conclusions
These results failed to serve as significant evidence to support the relationship between HPV and breast cancer. Further study with larger epidemiologic population is merited to determine the relationship between HPV and breast cancer. -
Citations
Citations to this article as recorded by- HPV, APOBEC3B, and the origins of breast cancer: a narrative review and perspectives on novel mechanisms
Zhi-yong Liu, Ran Chen
Frontiers in Oncology.2026;[Epub] CrossRef - Advances in human papillomavirus detection for cervical cancer screening and diagnosis: challenges of conventional methods and opportunities for emergent tools
O. Fashedemi, Okoroike C. Ozoemena, Siwaphiwe Peteni, Aderemi B. Haruna, Leshweni J. Shai, Aicheng Chen, Frankie Rawson, Maggie E. Cruickshank, David Grant, Oluwafunmilola Ola, Kenneth I. Ozoemena
Analytical Methods.2025; 17(7): 1428. CrossRef - Bacterial-Viral Interactions in Human Orodigestive and Female Genital Tract Cancers: A Summary of Epidemiologic and Laboratory Evidence
Ikuko Kato, Jilei Zhang, Jun Sun
Cancers.2022; 14(2): 425. CrossRef - Breast cancer association with oncogenic papillomaviruses: papillomaviral DNA detection in breast cancer cells
G. M. Volgareva
Advances in Molecular Oncology.2022; 9(2): 10. CrossRef - Presence of Human Papillomavirus DNA in Malignant Neoplasia and Non-Malignant Breast Disease
Erika Maldonado-Rodríguez, Marisa Hernández-Barrales, Adrián Reyes-López, Susana Godina-González, Perla I. Gallegos-Flores, Edgar L. Esparza-Ibarra, Irma E. González-Curiel, Jesús Aguayo-Rojas, Adrián López-Saucedo, Gretel Mendoza-Almanza, Jorge L. Ayala-
Current Issues in Molecular Biology.2022; 44(8): 3648. CrossRef - Risk Role of Breast Cancer in Association with Human Papilloma Virus among Female Population in Taiwan: A Nationwide Population-Based Cohort Study
Chia-Hsin Liu, Chi-You Liao, Ming-Hsin Yeh, James Cheng-Chung Wei
Healthcare.2022; 10(11): 2235. CrossRef - HPV-Associated Breast Cancer: Myth or Fact?
Erik Kudela, Eva Kudelova, Erik Kozubík, Tomas Rokos, Terezia Pribulova, Veronika Holubekova, Kamil Biringer
Pathogens.2022; 11(12): 1510. CrossRef - Assessment of Human Papillomavirus Infection and Risk Factors in Egyptian Women With Breast Cancer
Nabila El-Sheikh, Nahla O Mousa, Amany M Tawfeik, Alaa M Saleh, Iman Elshikh, Mohamed Deyab, Faten Ragheb, Manar M Moneer, Ahmed Kawashti, Ahmed Osman, Mohamed Elrefaei
Breast Cancer: Basic and Clinical Research.2021;[Epub] CrossRef - Human Papillomavirus (HPV) Detection by Chromogenic In Situ Hybridization (CISH) and p16 Immunohistochemistry (IHC) in Breast Intraductal Papilloma and Breast Carcinoma
Hua Guo, Juan P. Idrovo, Jin Cao, Sudarshana Roychoudhury, Pooja Navale, Louis J. Auguste, Tawfiqul Bhuiya, Silvat Sheikh-Fayyaz
Clinical Breast Cancer.2021; 21(6): e638. CrossRef - Human Papillomavirus in Breast Carcinogenesis: A Passenger, a Cofactor, or a Causal Agent?
Rancés Blanco, Diego Carrillo-Beltrán, Juan P. Muñoz, Alejandro H. Corvalán, Gloria M. Calaf, Francisco Aguayo
Biology.2021; 10(8): 804. CrossRef - Systematic review and meta-analysis of the papillomavirus prevalence in breast cancer fresh tissues
Geilson Gomes de Oliveira, Ana Katherine Gonçalves, José Eleutério, Luiz Gonzaga Porto Pinheiro
Breast Disease.2021; 41(1): 123. CrossRef - Is human papillomavirus associated with breast cancer or papilloma presenting with pathologic nipple discharge?
Fatih Levent Balci, Cihan Uras, Sheldon Marc Feldman
Cancer Treatment and Research Communications.2019; 19: 100122. CrossRef - Is the HPV virus responsible for the development of breast cancer?
Erik Kudela, Marcela Nachajova, Jan Danko
The Breast Journal.2019; 25(5): 1053. CrossRef - Absence of Human Papillomavirus in Benign and Malignant Breast Tissue
Maryam Kazemi Aghdam, Seyed Alireza Nadji, Azadeh Alvandimanesh, Maliheh Khoddami, Yassaman Khademi
Iranian Journal of Pathology.2019; 14(4): 279. CrossRef - Oncogenic Viruses and Breast Cancer: Mouse Mammary Tumor Virus (MMTV), Bovine Leukemia Virus (BLV), Human Papilloma Virus (HPV), and Epstein–Barr Virus (EBV)
James S. Lawson, Brian Salmons, Wendy K. Glenn
Frontiers in Oncology.2018;[Epub] CrossRef - Viral infections and breast cancer – A current perspective
O.M. Gannon, A. Antonsson, I.C. Bennett, N.A. Saunders
Cancer Letters.2018; 420: 182. CrossRef - Prevalence of EBV, HPV and MMTV in Pakistani breast cancer patients: A possible etiological role of viruses in breast cancer
Wasifa Naushad, Orooj Surriya, Hajra Sadia
Infection, Genetics and Evolution.2017; 54: 230. CrossRef
- HPV, APOBEC3B, and the origins of breast cancer: a narrative review and perspectives on novel mechanisms
- Clinical Significance of an HPV DNA Chip Test with Emphasis on HPV-16 and/or HPV-18 Detection in Korean Gynecological Patients
- Min-Kyung Yeo, Ahwon Lee, Soo Young Hur, Jong Sup Park
- J Pathol Transl Med. 2016;50(4):294-299. Published online June 26, 2016
- DOI: https://doi.org/10.4132/jptm.2016.05.09
- 10,915 View
- 80 Download
- 3 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) is a major risk factor for cervical cancer.
Methods
We evaluated the clinical significance of the HPV DNA chip genotyping assay (MyHPV chip, Mygene Co.) compared with the Hybrid Capture 2 (HC2) chemiluminescent nucleic acid hybridization kit (Digene Corp.) in 867 patients.
Results
The concordance rate between the MyHPV chip and HC2 was 79.4% (kappa coefficient, κ = 0.55). The sensitivity and specificity of both HPV tests were very similar (approximately 85% and 50%, respectively). The addition of HPV result (either MyHPV chip or HC2) to cytology improved the sensitivity (95%, each) but reduced the specificity (approximately 30%, each) compared with the HPV test or cytology alone. Based on the MyHPV chip results, the odds ratio (OR) for ≥ high-grade squamous intraepithelial lesions (HSILs) was 9.9 in the HPV-16/18 (+) group and 3.7 in the non-16/18 high-risk (HR)-HPV (+) group. Based on the HC2 results, the OR for ≥ HSILs was 5.9 in the HR-HPV (+) group. When considering only patients with cytological diagnoses of “negative for intraepithelial lesion or malignancy” and “atypical squamous cell or atypical glandular cell,” based on the MyHPV chip results, the ORs for ≥ HSILs were 6.8 and 11.7, respectively, in the HPV-16/18 (+) group.
Conclusions
The sensitivity and specificity of the MyHPV chip test are similar to the HC2. Detecting HPV-16/18 with an HPV DNA chip test, which is commonly used in many Asian countries, is useful in assessing the risk of high-grade cervical lesions. -
Citations
Citations to this article as recorded by- Human papilloma virus identification in ocular surface squamous neoplasia by p16 immunohistochemistry and DNA chip test
Tina Shrestha, Won Choi, Ga Eon Kim, Jee Myung Yang, Kyung Chul Yoon
Medicine.2019; 98(2): e13944. CrossRef - Comparison of the PANArray HPV Genotyping Chip Test with the Cobas 4800 HPV and Hybrid Capture 2 Tests for Detection of HPV in ASCUS Women
Eun Young Ki, Yoon Kyung Lee, Ahwon Lee, Jong Sup Park
Yonsei Medical Journal.2018; 59(5): 662. CrossRef
- Human papilloma virus identification in ocular surface squamous neoplasia by p16 immunohistochemistry and DNA chip test
- Comparison of Analytical and Clinical Performance of HPV 9G DNA Chip, PANArray HPV Genotyping Chip, and Hybrid-Capture II Assay in Cervicovaginal Swabs
- Ho Young Jung, Hye Seung Han, Hyo Bin Kim, Seo Young Oh, Sun-Joo Lee, Wook Youn Kim
- J Pathol Transl Med. 2016;50(2):138-146. Published online January 13, 2016
- DOI: https://doi.org/10.4132/jptm.2015.10.21
- 10,530 View
- 68 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) infection can be detected by using several molecular methods, including Hybrid-Capture II (HC2) assay and variable HPV DNA chip tests, although each method has different sensitivities and specificities. Methods: We performed HPV 9G DNA Chip (9G) and PANArray HPV Genotyping Chip (PANArray) tests on 118 cervicovaginal swabs and compared the results with HC2, cytology, histology, and direct sequencing results. Results: The overall and high-risk HPV (HR-HPV) positivity rates were 62.7% and 44.9% using 9G, and 61.0% and 30.5% using PANArray, respectively. The positivity rates for HR-HPV with these two chips were significantly lower than 55.1% when HC2 was used. The sensitivity of overall HPV positivity in detecting histologically confirmed low-grade cervical squamous intraepithelial lesions or higher was 88.7% for all three tests. The specificity was 58.5% for 9G and 61.5% for PANArray, which was significantly lower than the 72.3% for HC2. With the HR-HPV+ genotype threshold, the sensitivity decreased to 75.5% for 9G and 52.8% for PANArray, which was significantly lower than the 88.7% for HC2. Comparison of the two chips showed concordant results in 55.1% of the samples, compatible results in 16.9%, and discordant results in 28.0%, exhibiting poor agreement in detecting certain HPV genotypes. Compared with direct sequencing, 9G yielded no discordant results, whereas PANArray yielded 31 discordant results (26.7%). Conclusions: Compared with HC2, the HPV genotyping tests showed lower sensitivity in histologic correlation. When the two chips were compared, the 9G was more sensitive and accurate for detecting HR-HPV than the PANArray. -
Citations
Citations to this article as recorded by- Concordance of Anyplex™ II HPV HR assays with reference HPV assays in cervical cancer screening: Systematic review
Habtamu Biazin
Journal of Virological Methods.2022; 301: 114435. CrossRef - The clinical performance of human papillomavirus genotyping using PANArray HPV chip: Comparison to ThinPrep cytology alone and co-testing
Jiyoung Kim, Sun-Young Jun, Lee-So Maeng
Pathology - Research and Practice.2020; 216(9): 153121. CrossRef - Analytic performance of PANArray HPV and HPV 9G DNA chip tests for genotyping of high-risk human papillomavirus in cervical ThinPrep PreservCyt samples
Jiyoung Kim, Sun-Young Jun, Magdalena Grce
PLOS ONE.2019; 14(10): e0224483. CrossRef
- Concordance of Anyplex™ II HPV HR assays with reference HPV assays in cervical cancer screening: Systematic review
- Meningeal Solitary Fibrous Tumors with Delayed Extracranial Metastasis
- Nayoung Han, Hannah Kim, Soo Kee Min, Sun-Ha Paek, Chul-Kee Park, Seung-Hong Choi, U-Ri Chae, Sung-Hye Park
- J Pathol Transl Med. 2016;50(2):113-121. Published online December 14, 2015
- DOI: https://doi.org/10.4132/jptm.2015.10.30
- 13,399 View
- 120 Download
- 26 Web of Science
- 23 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The term solitary fibrous tumor (SFT) is preferred over meningeal hemangiopericytoma (HPC), because NAB2-STAT6 gene fusion has been observed in both intracranial and extracranial HPCs. HPCs are now considered cellular variants of SFTs. Methods: This study analyzes 19 patients with STAT6-confirmed SFTs, who were followed for over 11 years in a single institution. Ten patients (10/19, 56.2%) had extracranial metastases (metastatic group), while the remainder (9/19) did not (non-metastatic group). These two groups were compared clinicopathologically. Results: In the metastatic group, the primary metastatic sites were the lungs (n = 6), bone (n = 4), and liver (n = 3). There was a mean lag time of 14.2 years between the diagnosis of the initial meningeal tumor to that of systemic metastasis. The median age at initial tumor onset was 37.1 years in the metastatic group and 52.5 in the non-metastatic group. The 10-year survival rates of the metastatic- and non-metastatic groups were 100% and 33%, respectively. The significant prognostic factors for poor outcomes on univariate analysis included advanced age (≥45 years) and large initial tumor size (≥5 cm). In contrast, the patients with higher tumor grade, high mitotic rate (≥5/10 high-power fields), high Ki-67 index (≥5%), and the presence of necrosis or CD34 positivity showed tendency of poor prognosis but these parameters were not statistically significant poor prognostic markers. Conclusions: Among patients with SFTs, younger patients (<45 years) experienced longer survival times and paradoxically had more frequent extracranial metastases after long latent periods than did older patients. Therefore, young patients with SFTs require careful surveillance and follow-up for early detection of systemic metastases. -
Citations
Citations to this article as recorded by- Single-fraction stereotactic radiosurgery for residual, recurrent, or metastatic intracranial solitary fibrous tumors: An IRRF study toward management guidance
Salem M Tos, Ahmed Shaaban, Dawood Hamdan, Georgios Mantziaris, Bardia Hajikarimloo, Mariam Ishaque, Yuki Shinya, Vanshika Lohia, Zhishuo Wei, Orbay Askeroglu, Christian Amezquita-Contreras, Andrea Becerril-Gaitan, Onam Verma, Keiss Douri, Nathalia Lora,
Neuro-Oncology.2026;[Epub] CrossRef - High-grade, metastatic disease, and adjuvant radiotherapy are independent prognostic factors for progression-free survival in patients with solitary fibrous tumors
Jan Paul Alker, Ramin Rahmanzade, Thomas Held, Christel Herold-Mende, Andreas Unterberg, Felix Sahm, Sandro Manuel Krieg, Gerhard Jungwirth
Neuro-Oncology Advances.2025;[Epub] CrossRef - Meningeal malignant solitary fibrous tumor with multiple recurrence, extracranial extension, cervical lymph node metastases: case report and review of the literature
Rong He, Peng Zhong, Juntao Hu, Guangkuo Guo, He Xiao, Lin Lei, Yun Liu, Mingying Geng, Jungang Ma
Discover Oncology.2025;[Epub] CrossRef - A Case of Intracranial Solitary Fibrous Tumor Followed by Distant Metastasis without Local Recurrence
Masafumi YOSHIDA, Koki MORIYOSHI, Kento DOI, Yukihiro YAMAO, Natsue KISHIDA, Hiroya UEMURA, Shunichi FUKUDA
NMC Case Report Journal.2025; 12: 181. CrossRef - The association between WHO grading and the long-term outcomes and radiotherapy efficacy of intracranial solitary fibrous tumors
Leihao Ren, Lingyang Hua, AO Feng, Jiaojiao Deng, Hiroaki Wakimoto, Tareq Juratli, Qing Xie, Ye Gong
Acta Neuropathologica Communications.2025;[Epub] CrossRef - Meningeal Solitary Fibrous Tumor: A Single-Center Retrospective Cohort Study
Siyer Roohani, Yasemin Alberti, Maximilian Mirwald, Felix Ehret, Carmen Stromberger, Soleiman Fabris Roohani, Katja Bender, Anne Flörcken, Sven Märdian, Daniel Zips, David Kaul, Manish Charan
Sarcoma.2024; 2024: 1. CrossRef - De-differentiation associated with drop metastasis of a recurrent intracranial solitary fibrous tumor: a case report and literature review
Chenhui Zhao, Xiran Fan, Wanwan Gao, Fan Zhang, Haijun Lv, Xiaochun Jiang, Guangfu Di
International Journal of Neuroscience.2022; 132(8): 843. CrossRef - Long-term extracranial metastatic relapse of an intraventricular solitary fibrous tumor: a case report
Tarek Assi, Elie Samaha, Hussein Nassereddine
Anti-Cancer Drugs.2022; 33(1): e764. CrossRef - Multidisciplinary Treatment of Liver Metastases from Intracranial SFTs/HPCs: A Report of Three Consecutive Cases
Felix J. Krendl, Franka Messner, Gregor Laimer, Angela Djanani, Andreas Seeber, Georg Oberhuber, Dietmar Öfner, Dominik Wolf, Stefan Schneeberger, Reto Bale, Christian Margreiter
Current Oncology.2022; 29(11): 8720. CrossRef - A review of solitary fibrous tumor/hemangiopericytoma tumor and a comparison of risk factors for recurrence, metastases, and death among patients with spinal and intracranial tumors.
Enrico Giordan, Elisabetta Marton, Alexandra M. Wennberg, Angela Guerriero, Giuseppe Canova
Neurosurgical Review.2021; 44(3): 1299. CrossRef - Intracranial Solitary Fibrous Tumor of the Skull Base: 2 Cases and Systematic Review of the Literature
Sricharan Gopakumar, Visish M. Srinivasan, Caroline C. Hadley, Adrish Anand, Marc Daou, Patrick J. Karas, Jacob Mandel, Shankar P. Gopinath, Akash J. Patel
World Neurosurgery.2021; 149: e345. CrossRef - Hemangiopericytoma/Solitary Fibrous Tumor in the central nervous system. Experience with surgery and radiotherapy as a complementary treatment: A 10-year analysis of a heterogeneous series in a single tertiary center
Pedro Miguel González-Vargas, José Luis Thenier-Villa, Pablo Sanromán Álvarez, Alexandre Serantes Combo, Lourdes Calero Félix, Raúl Alejandro Galárraga Campoverde, Eva Azevedo González, Álvaro Martín-Gallego, Rosa Martínez-Rolan, Adolfo de la Lama Zaragoz
Neurocirugía.2020; 31(1): 14. CrossRef - Hemangiopericytoma/Solitary Fibrous Tumor in the central nervous system. Experience with surgery and radiotherapy as a complementary treatment: A 10-year analysis of a heterogeneous series in a single tertiary center
Pedro Miguel González-Vargas, José Luis Thenier-Villa, Pablo Sanromán Álvarez, Alexandre Serantes Combo, Lourdes Calero Félix, Raúl Alejandro Galárraga Campoverde, Eva Azevedo González, Álvaro Martín-Gallego, Rosa Martínez-Rolan, Adolfo de la Lama Zaragoz
Neurocirugía (English Edition).2020; 31(1): 14. CrossRef - Solitary fibrous tumor/hemangiopericytoma: treatment results based on the 2016 WHO classification
Kyoung Su Sung, Ju Hyung Moon, Eui Hyun Kim, Seok-Gu Kang, Se Hoon Kim, Chang-Ok Suh, Sun Ho Kim, Kyu-Sung Lee, Won Seok Chang, Jong Hee Chang
Journal of Neurosurgery.2019; 130(2): 418. CrossRef - Grading of meningeal solitary fibrous tumors/hemangiopericytomas: analysis of the prognostic value of the Marseille Grading System in a cohort of 132 patients
Nicolas Macagno, Rob Vogels, Romain Appay, Carole Colin, Karima Mokhtari, Benno Küsters, Pieter Wesseling, Dominique Figarella‐Branger, Uta Flucke, Corinne Bouvier
Brain Pathology.2019; 29(1): 18. CrossRef - Solitary fibrous tumor of the pineal region with delayed ectopic intracranial metastasis: A case report and review of the literature
Yongjie Wang, Jingying Zhang, Qichang Liu, Fuyi Liu, Xiangdong Zhu, Jianmin Zhang
Medicine.2019; 98(21): e15737. CrossRef - Case report: neonatal giant forehead hemangiopericytoma with a 5-year follow-up
AiJun Peng, LiBing Zhang, Hai Zhao, LiangXue Zhou
Medicine.2019; 98(47): e17888. CrossRef - Liquid Biopsy in Rare Cancers: Lessons from Hemangiopericytoma
Chiara Nicolazzo, Luciano Colangelo, Alessandro Corsi, Guido Carpino, Angela Gradilone, Chiara Sonato, Cristina Raimondi, Eugenio Gaudio, Paola Gazzaniga, Walter Gianni
Analytical Cellular Pathology.2018; 2018: 1. CrossRef - Surveillance for metastatic hemangiopericytoma-solitary fibrous tumors-systematic literature review on incidence, predictors and diagnosis of extra-cranial disease
Tarini Ratneswaren, Florence Rosie Avila Hogg, Mathew Joseph Gallagher, Keyoumars Ashkan
Journal of Neuro-Oncology.2018; 138(3): 447. CrossRef - Intracranial Solitary Fibrous Tumor
Eveline Claus, Patrick Seynaeve, Jeroen Ceuppens, Alain Vanneste, Koenraad Verstraete
Journal of the Belgian Society of Radiology.2017;[Epub] CrossRef - Comparison and evaluation of risk factors for meningeal, pleural, and extrapleural solitary fibrous tumors: A clinicopathological study of 92 cases confirmed by STAT6 immunohistochemical staining
Ji Min Kim, Yoon-La Choi, Yu Jin Kim, Hyung Kyu Park
Pathology - Research and Practice.2017; 213(6): 619. CrossRef - Molecular Testing of Brain Tumor
Sung-Hye Park, Jaekyung Won, Seong-Ik Kim, Yujin Lee, Chul-Kee Park, Seung-Ki Kim, Seung-Hong Choi
Journal of Pathology and Translational Medicine.2017; 51(3): 205. CrossRef - Solitary fibrous tumour presenting with a single bone metastasis: report of six cases and literature review
Vittoria Colia, Salvatore Provenzano, Carlo Morosi, Paola Collini, Salvatore Lorenzo Renne, Paolo G. Dagrada, Claudia Sangalli, Angelo Paolo Dei Tos, Andrea Marrari, Paolo G. Casali, Silvia Stacchiotti
Clinical Sarcoma Research.2016;[Epub] CrossRef
- Single-fraction stereotactic radiosurgery for residual, recurrent, or metastatic intracranial solitary fibrous tumors: An IRRF study toward management guidance
- Tongue Growth during Prenatal Development in Korean Fetuses and Embryos
- Soo Jeong Hong, Bong Geun Cha, Yeon Sook Kim, Suk Keun Lee, Je Geun Chi
- J Pathol Transl Med. 2015;49(6):497-510. Published online October 16, 2015
- DOI: https://doi.org/10.4132/jptm.2015.09.17
- 15,593 View
- 158 Download
- 9 Web of Science
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Prenatal tongue development may affect oral-craniofacial structures, but this muscular organ has rarely been investigated. Methods: In order to document the physiology of prenatal tongue growth, we histologically examined the facial and cranial base structures of 56 embryos and 106 fetuses. Results: In Streeter’s stages 13–14 (fertilization age [FA], 28 to 32 days), the tongue protruded into the stomodeal cavity from the retrohyoid space to the cartilaginous mesenchyme of the primitive cranial base, and in Streeter’s stage 15 (FA, 33 to 36 days), the tongue rapidly swelled and compressed the cranial base to initiate spheno-occipital synchondrosis and continued to swell laterally to occupy most of the stomodeal cavity in Streeter’s stage 16–17 (FA, 37 to 43 days). In Streeter’s stage 18–20 (FA, 44 to 51 days), the tongue was vertically positioned and filled the posterior nasopharyngeal space. As the growth of the mandible and maxilla advanced, the tongue was pulled down and protruded anteriorly to form the linguomandibular complex. Angulation between the anterior cranial base (ACB) and the posterior cranial base (PCB) was formed by the emerging tongue at FA 4 weeks and became constant at approximately 124°–126° from FA 6 weeks until birth, which was consistent with angulations measured on adult cephalograms. Conclusions: The early clockwise growth of the ACB to the maxillary plane became harmonious with the counter-clockwise growth of the PCB to the tongue axis during the early prenatal period. These observations suggest that human embryonic tongue growth affects ACB and PCB angulation, stimulates maxillary growth, and induces mandibular movement to achieve the essential functions of oral and maxillofacial structures. -
Citations
Citations to this article as recorded by- Detection of Muscle Fiber Orientation During Human Tongue Development: Analysis Using Diffusion Tensor Imaging
Saho Suto, Toru Kanahashi, Sena Fujii, Hirohiko Imai, Hiroki Otani, Shigehito Yamada, Tetsuya Takakuwa
NMR in Biomedicine.2026;[Epub] CrossRef - On the issue of the influence of craniometric parameters of the skull on the development of the tongue in the intermediate fetal period of human ontogenesis
Tatiana A. Alekseeva, Elena D. Lutsai
Volgograd Journal of Medical Research.2025; 22(1): 81. CrossRef - Associations of tongue and hyoid position, tongue volume, and pharyngeal airway dimensions with various dentoskeletal growth patterns
Jin Hye Kang, Jeong-Yun Kim, Nayansi Jha, Seok-Ki Jung, You-Sun Lee, Yoon-Ji Kim, Claudia Trindade Mattos
PLOS One.2025; 20(6): e0326092. CrossRef - Anquiloglosia y macroglosia: impacto en el crecimiento mandibular y la estabilidad del tratamiento ortodóncico: revisión de la literatura
Rocío del Pilar Sandoval Gálvez, Benjamín Alberto Alfero Ricci
South Florida Journal of Development.2025; 6(9): e5837. CrossRef - 3D Genial Tubercle Anatomic Considerations in Genioglossus Advancement Surgery
Nihal Punjabi, Alexandra Vacaru, Jared C. Inman
Otolaryngology–Head and Neck Surgery.2024; 171(5): 1572. CrossRef - Anatomical investigation of the common minke whale fetal tongue reveals papillae marginales and glands
Haruto Watanabe, Ayumi Hirose, Hiroto Murase, Gen Nakamura
Fisheries Science.2024; 90(6): 953. CrossRef - Fetal Micro and Macroglossia
Natalie Koren, Shir Shust‐Barequet, Tal Weissbach, Oshrat Raviv, Samar Abu Snenh, Efrat Abraham, Tal Cahan, Vered Eisenberg, Vered Yulzari, Efrat Hadi, Laura Adamo, Shali Mazaki Tovi, Reuven Achiron, Zvi Kivilevitch, Boaz Weisz, Eran Kassif
Journal of Ultrasound in Medicine.2023; 42(1): 59. CrossRef - Current data on the development of tongue in prenatal period of human ontogenesis
Tatyana A. Alekseeva, Elena D. Lutsay
Science and Innovations in Medicine.2022; 7(3): 148. CrossRef - Morphometric development of the tongue in fetal cadavers
Ahmet Dursun, Yadigar Kastamonı, Demet Kacaroglu, Neslihan Yuzbasıoglu, Tolga Ertekın
Surgical and Radiologic Anatomy.2020; 42(1): 3. CrossRef - Pigmented Fungiform Papillae of the Tongue and Lingual Fimbriae as Single Presentation in Adult: A Case Report and Literature Review
Meircurius Dwi Condro Surboyo, Diah Savitri Ernawati, Adiastuti Endah Parmadiati, Riyan Iman Marsetyo
European Journal of Dentistry.2020; 14(04): 702. CrossRef - Tongue development in stillborns autopsied at different gestational ages
Laura S. Aguiar, Guilherme R. Juliano, Luciano A.M. Silveira, Mariana S. Oliveira, Bianca G.S. Torquato, Gabriela R. Juliano, Márcia F. Araújo, Sanivia Aparecida L. Pereira, Vicente de Paula A. Teixeira, Mara Lúcia F. Ferraz
Jornal de Pediatria.2018; 94(6): 616. CrossRef - In Utero Glossoptosis in Fetuses With Robin Sequence
Cory M. Resnick, Tessa D. Kooiman, Carly E. Calabrese, Ryne Didier, Bonnie L. Padwa, Judy A. Estroff, Maarten J. Koudstaal
The Cleft Palate Craniofacial Journal.2018; 55(4): 562. CrossRef - Tongue development in stillborns autopsied at different gestational ages
Laura S. Aguiar, Guilherme R. Juliano, Luciano A.M. Silveira, Mariana S. Oliveira, Bianca G.S. Torquato, Gabriela R. Juliano, Márcia F. Araújo, Sanivia Aparecida L. Pereira, Vicente de Paula A. Teixeira, Mara Lúcia F. Ferraz
Jornal de Pediatria (Versão em Português).2018; 94(6): 616. CrossRef - Coexisting Congenital Subglosso-palatal Membrane and Tongue Dermoid in a Neonate
Preeti Tiwari, Vaibhav Pandey, Jayanto Tapadar
Indian Pediatrics.2018; 55(12): 1087. CrossRef - Tongue harmatoma in association with cleft palate: Case report
UwakweCosmas Mba, IfeanyiIgwilo Onah
Journal of Cleft Lip Palate and Craniofacial Anomalies.2017; 4(2): 168. CrossRef
- Detection of Muscle Fiber Orientation During Human Tongue Development: Analysis Using Diffusion Tensor Imaging
- Human Herpesvirus 8-Negative and Epstein-Barr Virus-Positive Effusion-Based Lymphoma in a Patient with Human Immunodeficiency Virus
- Jung-Woo Choi, Younghye Kim, Ju-Han Lee, Young-Sik Kim
- J Pathol Transl Med. 2015;49(5):409-412. Published online June 17, 2015
- DOI: https://doi.org/10.4132/jptm.2015.06.03
- 10,017 View
- 65 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - A 39-year-old man infected with human immunodeficiency virus (HIV) was admitted to our hospital because of sudden onset of chest pain. Chest radiography revealed pneumothorax of the right lung. Computed tomographic scans disclosed a 5.8-cm-sized emphysematous bulla in the right middle lobe of the lung. Histologically, the wedge-resected lung showed medium to large atypical cells within the bullous cavity of the Pneumocystis jirovecii pneumonia, without solid mass formation. These atypical cells were confirmed to be large B-cell lymphoma, Epstein-Barr virus–positive and human herpesvirus 8–negative. Therefore, this case was not diagnosed as primary effusion lymphoma, but effusion-based lymphoma arising in an emphysematous cavity of an HIV-infected patient. This type of effusion-based lymphoma has never been reported, and, although rare, it should be noted in order to clinically diagnose this lymphoma.
-
Citations
Citations to this article as recorded by- Primary Effusion Lymphoma: A Timely Review on the Association with HIV, HHV8, and EBV
Chih-Yi Liu, Bo-Jung Chen, Shih-Sung Chuang
Diagnostics.2022; 12(3): 713. CrossRef - Human herpesvirus 8-negative effusion-based large B-cell lymphoma: a distinct entity with unique clinicopathologic characteristics
Savanah D. Gisriel, Ji Yuan, Ryan C. Braunberger, Danielle L.V. Maracaja, Xueyan Chen, Xiaojun Wu, Jenna McCracken, Mingyi Chen, Yi Xie, Laura E. Brown, Peng Li, Yi Zhou, Tarsheen Sethi, Austin McHenry, Ronald G. Hauser, Nathan Paulson, Haiming Tang, Eric
Modern Pathology.2022; 35(10): 1411. CrossRef - Age and CD20 Expression Are Significant Prognostic Factors in Human Herpes Virus-8-negative Effusion-based Lymphoma
Tomomi Kubota, Yosuke Sasaki, Eisuke Shiozawa, Masafumi Takimoto, Tsunekazu Hishima, Ja-Mun Chong
American Journal of Surgical Pathology.2018; 42(12): 1607. CrossRef
- Primary Effusion Lymphoma: A Timely Review on the Association with HIV, HHV8, and EBV
- Accuracy of Core Needle Biopsy Versus Fine Needle Aspiration Cytology for Diagnosing Salivary Gland Tumors
- In Hye Song, Joon Seon Song, Chang Ohk Sung, Jong-Lyel Roh, Seung-Ho Choi, Soon Yuhl Nam, Sang Yoon Kim, Jeong Hyun Lee, Jung Hwan Baek, Kyung-Ja Cho
- J Pathol Transl Med. 2015;49(2):136-143. Published online March 12, 2015
- DOI: https://doi.org/10.4132/jptm.2015.01.03
- 18,090 View
- 239 Download
- 79 Web of Science
- 82 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Core needle biopsy is a relatively new technique used to diagnose salivary gland lesions, and its role in comparison with fine needle aspiration cytology needs to be refined. Methods: We compared the results of 228 ultrasound-guided core needle biopsy and 371 fine needle aspiration procedures performed on major salivary gland tumors with their postoperative histological diagnoses. Results: Core needle biopsy resulted in significantly higher sensitivity and more accurate tumor subtyping, especially for malignant tumors, than fine needle aspiration. No patient developed major complications after core needle biopsy. Conclusions: We recommend ultrasoundguided core needle biopsy as the primary diagnostic tool for the preoperative evaluation of patients with salivary gland lesions, especially when malignancy is suspected. -
Citations
Citations to this article as recorded by- Parotid Secretory Carcinoma: A Distinct Entity from Acinic Cell Carcinoma
Muhammad Adzha Musa, Muhamad Arif Ahmad Radzi, Moharzudi Mohamed, Ikram Hakim
Indian Journal of Otolaryngology and Head & Neck Surgery.2026; 78(2): 1209. CrossRef - Fine-needle aspiration or core needle biopsy? A meta-analysis of diagnostic accuracy and procedural outcomes in salivary gland tumors
Kenan Kassem, Alaa Safia, Uday Abd Elhadi, Shlomo Merchavy
European Journal of Radiology.2026; 194: 112532. CrossRef - Controversial issues in core needle biopsy for diagnosing parotid neoplasms
N. V. Vishneva, P. A. Demenchuk, O. Yu. Petropavlovskaya, E. I. Selifanova, A. N. Lanina, N. V. Kalakutsky, A. I. Yaremenko
Parodontologiya.2026; 30(4): 407. CrossRef - Frozen Section Analysis in Submandibular Gland Tumors: Optimizing Intraoperative Decision-Making
Amir Bolooki, Felix Johnson, Anna Stenzl, Zhaojun Zhu, Benedikt Gabriel Hofauer
Cancers.2025; 17(5): 895. CrossRef - The Myriad Spectrum of Salivary Gland Lesions: Cytohistological Correlation on Fine Needle Aspiration Cytology, Core Needle Biopsy, and Resections in a 5‐Year Single Institutional Experience of North India
Zachariah Chowdhury, Pallavi Majumdar, Sumeet Narain, Komal Lamba
Diagnostic Cytopathology.2025; 53(8): 391. CrossRef - Salivary Duct Carcinoma: A 12-Year Single Center Experience
Hyowon Ahn, Dongbin Ahn, Ji Hye Kwak
Korean Journal of Otorhinolaryngology-Head and Neck Surgery.2025; 68(6): 232. CrossRef - Cytological Spectrum of Salivary Gland Lesions Using the Milan System and their Histopathological Correlation: Retrospective Study in a Peripheral Medical College of Eastern India
Ujjwal Bandyopadhyay, Sarmila Guha Banerjee, Sirshak Dutta
Indian Journal of Otolaryngology and Head & Neck Surgery.2025; 77(11): 4887. CrossRef - Diagnostic performance of ultrasound guided salivary gland core needle biopsy and fine needle aspiration in children
Vicente Oliveira, Anthea Lafrenière, Nikolaus Wolter, Joao Amaral, Alessandro Gasparetto, Dimitri Parra Rojas
Pediatric Radiology.2025; 56(2): 393. CrossRef - Giant Pleomorphic Adenoma of Submandibular Gland
Harendra Kumar, Qazi Saquib Rizwan, Mayank Gupta, Tarun Kumar
Indian Journal of Otolaryngology and Head & Neck Surgery.2024; 76(1): 1361. CrossRef - CT-guided core needle biopsies of head and neck tumors: a comprehensive monocenter analysis of safety and outcomes
Thomas Joseph Vogl, Heinrich Johannes Ketelsen, Scherwin Mahmoudi, Jan-Erik Scholtz, Vitali Koch, Leon David Grünewald, Peter Wild, Timo Stoever, Simon Bernatz
European Radiology.2024; 34(8): 5370. CrossRef - Indications for Submandibulectomy Within a 20-Year Period
Amir Bolooki, Anna Stenzl, Christopher Weusthof, Benedikt Hofauer
Ear, Nose & Throat Journal.2024;[Epub] CrossRef - Treatment of Warthin’s Tumors of the Parotid Gland With Radiofrequency Ablation: A Systematic Review of the Current Literature
Kenny Do, Eric Kawana, Sisi Tian, Jo-Lawrence Bigcas
Ear, Nose & Throat Journal.2024;[Epub] CrossRef - Evaluation of the anterior processes of the parotid gland: an ultrasonographic study
Tarık Ali Uğur, Hümeyra Tercanlı
Surgical and Radiologic Anatomy.2024; 46(6): 915. CrossRef - Salivary Gland Fine-Needle Aspiration
Federica Policardo, Antonino Mule’, Esther Diana Rossi
Surgical Pathology Clinics.2024; 17(3): 347. CrossRef - Implementation of the Milan System for Reporting Salivary Gland Cytology: A Two-Year Outcome Cytopathology Data of a Tertiary Care Center
Soudamini Mahapatra, Chinmaya Sundar Ray, Aparajita Mishra, Dileswari Pradhan
Cureus.2024;[Epub] CrossRef - Preoperative cytopathological investigatory aids in the diagnosis of salivary gland lesions
S Vidyalakshmi, K Shanmugasamy
Journal of Oral and Maxillofacial Pathology.2024; 28(2): 172. CrossRef - Machine Learning on Ultrasound Texture Analysis Data for Characterizing of Salivary Glandular Tumors: A Feasibility Study
Li-Jen Liao, Ping-Chia Cheng, Feng-Tsan Chan
Diagnostics.2024; 14(16): 1761. CrossRef - Association of Membranous Basal Cell Adenoma and Basal Cell Adenocarcinoma With Brooke-Spiegler Syndrome
Lexi Goehring, Debby Rampisela, Jordan L Pleitz
Cureus.2024;[Epub] CrossRef - A Retrospective 8‐Year Single Institutional Study in Germany Regarding Diagnosis, Treatment, and Outcome of Malignant Parotid Tumors
S. Andrianopoulou, L. S. Fiedler, B. M. Lippert, O. C. Bulut, Mohamed Rahouma
International Journal of Surgical Oncology.2024;[Epub] CrossRef - High Field MRI in Parotid Gland Tumors: A Diagnostic Algorithm
Chiara Gaudino, Andrea Cassoni, Martina Lucia Pisciotti, Resi Pucci, Chiara Veneroso, Cira Rosaria Tiziana Di Gioia, Francesca De Felice, Patrizia Pantano, Valentino Valentini
Cancers.2024; 17(1): 71. CrossRef - Nationwide Incidence Trends of Pediatric Parotid Malignancy in Korea and a Retrospective Analysis of Single-Institution Surgical Experience of Parotidectomy
Hyun Seong Kim, Seo Young Kim, Eun-Jae Chung, Seong Keun Kwon, Soon-Hyun Ahn, Yuh-Seog Jung, Jungirl Seok
Korean Society of Head and Neck Oncology.2024; 40(2): 7. CrossRef - The Usefulness of Ultrasound-Guided Core Needle Biopsy Compared to Fine Needle Aspiration in Pre-Operative Diagnosis of Cystic-Predominant Parotid Tumors
Youn Jin Cho, Young Rok Jo, Hyun Jun Hong, Hye Ran Lee
Korean Journal of Otorhinolaryngology-Head and Neck Surgery.2023; 66(8): 532. CrossRef - The Value of Ultrasound-guided Core Needle Biopsy in Differentiating Benign from Malignant Salivary Gland Lesions
Mohammad Ali Kazemi, Farzaneh Amini, Bita Kargar, Maryam Lotfi, Keyvan Aghazadeh, Hashem Sharifian, Behnaz Moradi, Javid Azadbakht
Indian Journal of Otolaryngology and Head & Neck Surgery.2023; 75(2): 266. CrossRef - Schnellschnittdiagnostik bei Tumoren des Trigonum submandibulare
S. Riemann, A. Knopf
HNO.2023; 71(3): 164. CrossRef - Myoepithelial Carcinoma Ex Pleomorphic Adenoma of the Submandibular Gland: A Case Report
Georgia Syrnioti, Antonia Syrnioti, Alharith Abdullah, Xuehui Lui, Ernesto Mendoza
Cureus.2023;[Epub] CrossRef - Intraductal Carcinoma: The Carcinoma In Situ of the Salivary Gland
Rhema Thomas, Tijjani Umar, Farzad Borumandi
Journal of Craniofacial Surgery.2023; 34(5): e432. CrossRef - Fine-Needle Aspiration Cytology for Parotid Tumors
Masataka Taniuchi, Tetsuya Terada, Ryo Kawata
Life.2022; 12(11): 1897. CrossRef - Utility of the Milan System for Reporting Salivary Gland Cytology, with focus on the incidence and histologic correlates of atypia of undetermined significance (AUS) and salivary gland neoplasm of uncertain malignant potential (SUMP): A 3‐year institution
Christopher M. Cormier, Shweta Agarwal
Cancer Cytopathology.2022; 130(4): 303. CrossRef - Percutaneous CT-Guided Core Needle Biopsies of Head and Neck Masses: Review of 184 Cases at a Single Academic Institution, Common and Special Techniques, Diagnostic Yield, and Safety
R.W. Jordan, D.P. Shlapak, J.C. Benson, F.E. Diehn, D.K. Kim, V.T. Lehman, G.B. Liebo, A.A. Madhavan, J.M. Morris, P.P. Morris, J.T. Verdoorn, C.M. Carr
American Journal of Neuroradiology.2022; 43(1): 117. CrossRef - Nodular fasciitis of the submandibular gland
Ting Suen Wong, Richard Wei Chern Gan, Laszlo Karsai, Bun Yin Winson Wong
BMJ Case Reports.2022; 15(4): e245584. CrossRef - Validation of the Milan system for reporting salivary gland cytopathology: a single institution’s 10-year experience
Christopher Felicelli, Joseph Reznicek, Yevgen Chornenkyy, Lucy Jager, Daniel Johnson
Journal of the American Society of Cytopathology.2022; 11(5): 264. CrossRef - Application of the Milan system for reporting salivary gland cytopathology using cell blocks
Grégoire B. Morand, Raihanah Alsayegh, Alex M. Mlynarek, Marianne Plourde, Tiffany Mach, Marco A. Mascarella, Michael P. Hier, Livia Florianova, Marc P. Pusztaszeri
Virchows Archiv.2022; 481(4): 575. CrossRef - Comparisons among the Ultrasonography Prediction Model, Real-Time and Shear Wave Elastography in the Evaluation of Major Salivary Gland Tumors
Ping-Chia Cheng, Wu-Chia Lo, Chih-Ming Chang, Ming-Hsun Wen, Po-Wen Cheng, Li-Jen Liao
Diagnostics.2022; 12(10): 2488. CrossRef - A Novel Sonographic Scoring Model in the Prediction of Major Salivary Gland Tumors
Wu‐Chia Lo, Chih‐Ming Chang, Chi‐Te Wang, Po‐Wen Cheng, Li‐Jen Liao
The Laryngoscope.2021;[Epub] CrossRef - Assessing the diagnostic accuracy for pleomorphic adenoma and Warthin tumor by employing the Milan System for Reporting Salivary Gland Cytopathology: An international, multi‐institutional study
Derek B. Allison, Alexander P. Smith, Daniel An, James Adam Miller, Khurram Shafique, Sharon Song, Kartik Viswanathan, Elizabeth Eykman, Rema A. Rao, Austin Wiles, Güliz A. Barkan, Ritu Nayar, Guido Fadda, Celeste N. Powers, Esther Diana Rossi, Momin T. S
Cancer Cytopathology.2021; 129(1): 43. CrossRef - Magnetic resonance imaging of salivary gland tumours: Key findings for imaging characterisation
Davide Maraghelli, Michele Pietragalla, Cesare Cordopatri, Cosimo Nardi, Anna Julie Peired, Giandomenico Maggiore, Stefano Colagrande
European Journal of Radiology.2021; 139: 109716. CrossRef - The Milan System, from Its Introduction to Its Current Adoption in the Diagnosis of Salivary Gland Cytology
Esther Diana Rossi
Journal of Molecular Pathology.2021; 2(2): 114. CrossRef - Utility of the Milan system for reporting salivary gland cytopathology during rapid on‐site evaluation (ROSE) of salivary gland aspirates
Aanchal Kakkar, Mukin Kumar, Priyadarsani Subramanian, Arshad Zubair, Rajeev Kumar, Alok Thakar, Deepali Jain, Sandeep R. Mathur, Venkateswaran K. Iyer
Cytopathology.2021; 32(6): 779. CrossRef - Contribution of small tissue biopsy and flow cytometry to preoperative cytological categorization of salivary gland fine needle aspirates according to the Milan System: Single center experience on 287 cases
Tolga Bağlan, Serpil Dizbay Sak, Cevriye Cansız Ersöz, Koray Ceyhan
Diagnostic Cytopathology.2021; 49(4): 509. CrossRef - Is Milan for kids?: The Milan System for Reporting Salivary Gland Cytology in pediatric patients at an academic children's hospital with cytologic‐histologic correlation
Swati P. Satturwar, Maren Y. Fuller, Sara E. Monaco
Cancer Cytopathology.2021; 129(11): 884. CrossRef - Radiographic Interpretation in Oral Medicine and Hospital Dental Practice
Katherine France, Anwar A.A.Y. AlMuzaini, Mel Mupparapu
Dental Clinics of North America.2021; 65(3): 509. CrossRef - Carcinoma ex pleomorphic adenoma of major salivary glands: CT and MR imaging findings
Can Wang, Qiang Yu, Siyi Li, Jingjing Sun, Ling Zhu, Pingzhong Wang
Dentomaxillofacial Radiology.2021; 50(7): 20200485. CrossRef - Salivary gland carcinoma in children and adolescents: The EXPeRT/PARTNER diagnosis and treatment recommendations
Aurore Surun, Dominik T. Schneider, Andrea Ferrari, Teresa Stachowicz‐Stencel, Jelena Rascon, Anna Synakiewicz, Abbas Agaimy, Kata Martinova, Denis Kachanov, Jelena Roganovic, Ewa Bien, Gianni Bisogno, Ines B. Brecht, Frédéric Kolb, Juliette Thariat, Anto
Pediatric Blood & Cancer.2021;[Epub] CrossRef - A Call for Universal Acceptance of the Milan System for Reporting Salivary Gland Cytopathology
Eric Barbarite, Sidharth V. Puram, Adeeb Derakhshan, Esther D. Rossi, William C. Faquin, Mark A. Varvares
The Laryngoscope.2020; 130(1): 80. CrossRef - Preoperative biopsy in parotid malignancies: Variation in use and impact on surgical margins
Liliya Benchetrit, Sina J. Torabi, Elliot Morse, Saral Mehra, Rahmatullah Rahmati, Heather A. Osborn, Benjamin L. Judson
The Laryngoscope.2020; 130(6): 1450. CrossRef - α‐Synuclein Real‐Time Quaking‐Induced Conversion in the Submandibular Glands of Parkinson's Disease Patients
Sireesha Manne, Naveen Kondru, Huajun Jin, Vellareddy Anantharam, Xuemei Huang, Arthi Kanthasamy, Anumantha G. Kanthasamy
Movement Disorders.2020; 35(2): 268. CrossRef - The Accessory Parotid Gland and its Clinical Significance
Mateusz A. Rosa, Dominik P. Łazarz, Jakub R. Pękala, Bendik Skinningsrud, Sigurd S. Lauritzen, Bernard Solewski, Przemysław A. Pękala, Jerzy A. Walocha, Krzysztof A. Tomaszewski
Journal of Craniofacial Surgery.2020; 31(3): 856. CrossRef - Comparison of core needle biopsy and fine‐needle aspiration in diagnosis of ma lignant salivary gland neoplasm: Systematic review and meta‐analysis
Jungheum Cho, Junghoon Kim, Ji Sung Lee, Choong Guen Chee, Youngjune Kim, Sang Il Choi
Head & Neck.2020; 42(10): 3041. CrossRef - The Milan system for reporting salivary gland cytopathology: The clinical impact so far. Considerations from theory to practice
Esther Diana Rossi, William C. Faquin
Cytopathology.2020; 31(3): 181. CrossRef - The role of core needle biopsy in parotid glands lesions with inconclusive fine needle aspiration
Farrokh Heidari, Firouzeh Heidari, Benyamin Rahmaty, Neda Jafari, Kayvan Aghazadeh, Saeed Sohrabpour, Ebrahim Karimi
American Journal of Otolaryngology.2020; 41(6): 102718. CrossRef - Role of Fine Needle Aspiration Cytology in the Diagnosis of Parotid Gland Tumors: Analysis of 193 Cases
Rahim Dhanani, Haissan Iftikhar, Muhammad Sohail Awan, Nida Zahid, Sehrish Nizar Ali Momin
International Archives of Otorhinolaryngology.2020; 24(04): e508. CrossRef - Cytohistological correlation of salivary gland tumours with emphasis on Milan system for reporting: A novel step towards internal quality assurance
Anandraj Vaithy.K, ATM Venkat Raghava, E S Keerthika Sri, K R Umadevi
IP Archives of Cytology and Histopathology Research.2020; 5(4): 283. CrossRef - Diagnosing Recently Defined and Uncommon Salivary Gland Lesions in Limited Cellularity Specimens: Cytomorphology and Ancillary Studies
Esther Diana Rossi, Zubair Baloch, William Faquin, Liron Pantanowitz
AJSP: Reviews and Reports.2020; 25(5): 210. CrossRef - Peripheral T Cell Lymphoma of Parotid Gland: A Diagnostic Challenge
J. G. Aishwarya, Satish Nair, C. N. Patil, Swarna Shivakumar, N. Shrivalli, Ashish Shah
Indian Journal of Otolaryngology and Head & Neck Surgery.2019; 71(S1): 533. CrossRef - Potential utility of core needle biopsy in the diagnosis of IgG4-related dacryoadenitis and sialadenitis
Kenichi Takano, Tsuyoshi Okuni, Keisuke Yamamoto, Ryuta Kamekura, Ryoto Yajima, Motohisa Yamamoto, Hiroki Takahashi, Tetsuo Himi
Modern Rheumatology.2019; 29(2): 393. CrossRef - Retrospective assessment of the effectiveness of the Milan system for reporting salivary gland cytology: A systematic review and meta‐analysis of published literature
Sahar J Farahani, Zubair Baloch
Diagnostic Cytopathology.2019; 47(2): 67. CrossRef - Values of fine‐needle aspiration cytology of parotid gland tumors: A review of 996 cases at a single institution
Manabu Suzuki, Ryo Kawata, Masaaki Higashino, Shuji Nishikawa, Tetsuya Terada, Shin‐Ichi Haginomori, Yoshitaka Kurisu, Yoshinobu Hirose
Head & Neck.2019; 41(2): 358. CrossRef - Positive Surgical Margins in Submandibular Malignancies: Facility and Practice Variation
Liliya Benchetrit, Elliot Morse, Benjamin L. Judson, Saral Mehra
Otolaryngology–Head and Neck Surgery.2019; 161(4): 620. CrossRef - The growth rate and the positive prediction of needle biopsy of clinically diagnosed Warthin’s tumor
Jungirl Seok, Woo-Jin Jeong, Soon-Hyun Ahn, Young Ho Jung
European Archives of Oto-Rhino-Laryngology.2019; 276(7): 2091. CrossRef - The Difference in the Clinical Features Between Carcinoma ex Pleomorphic Adenoma and Pleomorphic Adenoma
Jungirl Seok, Se Jin Hyun, Woo-Jin Jeong, Soon-Hyun Ahn, Hyojin Kim, Young Ho Jung
Ear, Nose & Throat Journal.2019; 98(8): 504. CrossRef - Fine‐needle aspiration cytology and radiological imaging in parotid gland tumours: Our experience in 103 patients
Clare Perkins, Edward Toll, Philip Reece
Clinical Otolaryngology.2019; 44(6): 1124. CrossRef - Application of the Milan system of reporting salivary cytopathology – A retrospective cytohistological correlation study
Ramya Katta, Devi Padmavathi Chaganti
Journal of Dr. NTR University of Health Sciences.2019; 8(1): 11. CrossRef - Ultrasound‐guided core needle biopsy in salivary glands: A meta‐analysis
Hee Joon Kim, Jong Seung Kim
The Laryngoscope.2018; 128(1): 118. CrossRef - Accuracy and effectiveness of ultrasound-guided core-needle biopsy in the diagnosis of focal lesions in the salivary glands
Jose Luis del Cura, Gloria Coronado, Rosa Zabala, Igone Korta, Ignacio López
European Radiology.2018; 28(7): 2934. CrossRef - The Milan System for Reporting Salivary Gland Cytopathology (MSRSGC): an ASC-IAC–sponsored system for reporting salivary gland fine-needle aspiration
Esther Diana Rossi, Zubair Baloch, Marc Pusztaszeri, William C. Faquin
Journal of the American Society of Cytopathology.2018; 7(3): 111. CrossRef - Routine and Advanced Ultrasound of Major Salivary Glands
Kunwar Suryaveer Singh Bhatia, Yuk-Ling Dai
Neuroimaging Clinics of North America.2018; 28(2): 273. CrossRef - The Milan System for Reporting Salivary Gland Cytopathology (MSRSGC): An ASC-IAC-Sponsored System for Reporting Salivary Gland Fine-Needle Aspiration
Esther Diana Rossi, Zubair W. Baloch, Marc Pusztaszeri, William C. Faquin
Acta Cytologica.2018; 62(3): 157. CrossRef - Evaluation and diagnosis of salivary gland neoplasms
Erica Jackson Mayland, Anna M. Pou
Operative Techniques in Otolaryngology-Head and Neck Surgery.2018; 29(3): 129. CrossRef - Feasibility and Safety of Multicenter Tissue and Biofluid Sampling for α-Synuclein in Parkinson’s Disease: The Systemic Synuclein Sampling Study (S4)
Lana M. Chahine, Thomas G. Beach, Nicholas Seedorff, Chelsea Caspell-Garcia, Christopher S. Coffey, Michael Brumm, Charles H. Adler, Geidy E. Serrano, Carly Linder, Sherri Mosovsky, Tatiana Foroud, Holly Riss, Dixie Ecklund, John Seibyl, Danna Jennings, V
Journal of Parkinson’s Disease.2018; 8(4): 517. CrossRef - Preoperative diagnostic of parotid gland neoplasms: fine-needle aspiration cytology or core needle biopsy?
Peter Zbären, Asterios Triantafyllou, Kenneth O. Devaney, Vincent Vander Poorten, Henrik Hellquist, Alessandra Rinaldo, Alfio Ferlito
European Archives of Oto-Rhino-Laryngology.2018; 275(11): 2609. CrossRef - A comparison study of the reporting systems for salivary gland fine needle aspirations: Are they really different?
Diana Montezuma, Sule Canberk, Ozlem Aydın, Mehmet Polat Dermirhas, André F. Vieira, Süha Goksel, Ümit İnce, Fernando Schmitt
Diagnostic Cytopathology.2018; 46(10): 859. CrossRef - Pediatric salivary gland carcinomas: Diagnostic and therapeutic management
Céleste Rebours, Vincent Couloigner, Louise Galmiche, Odile Casiraghi, Cécile Badoual, Sabah Boudjemaa, Anthony Chauvin, Monique Elmaleh, Brice Fresneau, Sylvie Fasola, Erea‐Noël Garabédian, Thierry Van Den Abeele, Daniel Orbach
The Laryngoscope.2017; 127(1): 140. CrossRef - Agreement between rapid on‐site evaluation and the final cytological diagnosis of salivary gland specimens
S. Wangsiricharoen, S. Lekawanvijit, S. Rangdaeng
Cytopathology.2017; 28(4): 321. CrossRef - Mesenchymal neoplasms of the head and neck: a cytopathologic analysis on fine needle aspiration
James Lee, Samia Kazmi, Christopher J. VandenBussche, Syed Z. Ali
Journal of the American Society of Cytopathology.2017; 6(3): 105. CrossRef - Clinical Results of Surgical Treatment in Parotid Tumors
Ahmet Kara
Journal of Otolaryngology-ENT Research.2017;[Epub] CrossRef - Parotid gland metastases of distant primary tumours: A diagnostic challenge
Achim M. Franzen, Thomas Günzel, Anja Lieder
Auris Nasus Larynx.2016; 43(2): 187. CrossRef - Modern Radiology in the Management of Head and Neck Cancer
G.J.C. Burkill, R.M. Evans, V.V. Raman, S.E.J. Connor
Clinical Oncology.2016; 28(7): 440. CrossRef - Fine‐needle aspiration and core needle biopsy: An update on 2 common minimally invasive tissue sampling modalities
Paul A. VanderLaan
Cancer Cytopathology.2016; 124(12): 862. CrossRef - Staging and follow-up of high-grade malignant salivary gland tumours: The role of traditional versus functional imaging approaches – A review
Nicole Freling, Flavio Crippa, Roberto Maroldi
Oral Oncology.2016; 60: 157. CrossRef - Biopsy of parotid masses: Review of current techniques
Sananda Haldar, Joseph D Sinnott, Kemal M Tekeli, Samuel S Turner, David C Howlett
World Journal of Radiology.2016; 8(5): 501. CrossRef - Review on the applications of ultrasonography in dentomaxillofacial region
Şehrazat Evirgen
World Journal of Radiology.2016; 8(1): 50. CrossRef - Comprehensive Cytomorphologic Analysis of Pulmonary Adenoid Cystic Carcinoma: Comparison to Small Cell Carcinoma and Non-pulmonary Adenoid Cystic Carcinoma
Seokhwi Kim, Jinah Chu, Hojoong Kim, Joungho Han
Journal of Pathology and Translational Medicine.2015; 49(6): 511. CrossRef
- Parotid Secretory Carcinoma: A Distinct Entity from Acinic Cell Carcinoma
- Supratentorial Hemangioblastoma with Unusual Features
- Yooju Shin, Seokhwi Kim, Hyun-Woo Lee, Heejin Bang, Yeon-Lim Suh
- Korean J Pathol. 2014;48(6):462-465. Published online December 31, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.6.462
- 12,523 View
- 79 Download
- 6 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Supratentorial Hemangioblastoma in Adults: A Systematic Review and Comparison of Infratentorial and Spinal Cord Locations
Dragan Jankovic, Kyna Vuong, Bruno Splavski, Kresimir Rotim, Kenan I. Arnautovic
World Neurosurgery.2023; 173: 48. CrossRef - Supratentorial hemangioblastoma: correlation between phenotype, gender and vascular territory affected
Yosef Laviv, David Saraf, Liat Oxman, Ido Ben Zvi
Neurosurgical Review.2023;[Epub] CrossRef - Neuropathologic features of central nervous system hemangioblastoma
Rebecca A. Yoda, Patrick J. Cimino
Journal of Pathology and Translational Medicine.2022; 56(3): 115. CrossRef - The loss of succinate dehydrogenase B expression is frequently identified in hemangioblastoma of the central nervous system
Tae Hoon Roh, Hyunee Yim, Jin Roh, Kyi Beom Lee, So Hyun Park, Seon-Yong Jeong, Se-Hyuk Kim, Jang-Hee Kim
Scientific Reports.2019;[Epub] CrossRef - Supratentorial hemangioblastomas in von Hippel–Lindau wild-type patients – case series and literature review
Luís Rocha, Carolina Noronha, Ricardo Taipa, Joaquim Reis, Mário Gomes, Ernesto Carvalho
International Journal of Neuroscience.2018; 128(3): 295. CrossRef - MR Imaging Findings of Supratentorial Meningeal Hemangioblastoma: A Case Report
Gi Hong Kim, Ho Kyu Lee, Myeong Ju Koh, Young Hee Maeng
Journal of the Korean Society of Radiology.2016; 75(1): 26. CrossRef
- Supratentorial Hemangioblastoma in Adults: A Systematic Review and Comparison of Infratentorial and Spinal Cord Locations
- A Case of Metastatic Angiosarcoma Diagnosed by Liquid-Based Preparation: Peculiar Cytoplasmic Changes
- Min Jung Jung, Young Ok Kim
- Korean J Pathol. 2014;48(3):241-247. Published online June 26, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.3.241
- 9,102 View
- 54 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Angiosarcoma with predominantly epithelioid features is a rare soft tissue neoplasm and the interpretation of its cytopathologic findings may be difficult. We report a case of metastatic angiosarcoma with predominantly epithelioid features diagnosed by liquid-based cytology. The cytopathologic findings in this case differed from those of the conventional preparation and we found a clean background, no hyperchromatic nuclei and several cytoplasmic changes, including intracytoplasmic vacuoles with peculiar shapes, juxtanuclear condensation and perinuclear clearing. Identification of these changes using liquid-based cytology supplemented with immunochemistry may be helpful in reaching a correct cytopathologic diagnosis.
-
Citations
Citations to this article as recorded by- Cytological Features of a Metastatic Angiosarcoma in the Lymph Node Diagnosed via Liquid-Based Cytology
Jie-Yang Jhuang, Chih-Yi Liu, Min-Hui Tseng, Shih-Sung Chuang
Diagnostics.2023; 13(12): 2124. CrossRef - Radiation-associated Angiosarcoma Presenting as Massive Pleural Effusion
Hirokazu Ogino, Makoto Tobiume, Kozo Kagawa, Hiroshi Kawano, Satoshi Sakaguchi, Atsuro Saijo, Daisuke Matsumoto, Hiromitsu Takizawa, Yuriko Morikawa, Yoshimi Bando, Hisatsugu Goto, Hiroshi Nokihara, Yasuhiko Nishioka
Internal Medicine.2022; 61(9): 1393. CrossRef - Delayed diagnosis of angiosarcoma of the spleen: clinically presenting as recurrent haemoperitoneum following embolisation
Verena Kornmann, Philip van Rijn, Dries Mulder, Koen Reijnders
BMJ Case Reports.2015; 2015: bcr2014208956. CrossRef - A Case of Angiosarcoma of the Scalp with Invasion to the Pleural Effusion
Yusuke Amano, Yukari Obana, Yoko Nakanishi, Ryusuke Tsujimura, Kayomi Wakamatsu, Fumiko Uemura, Yoshihisa Katsura, Masahiko Sugitani, Norimichi Nemoto
Journal of Nihon University Medical Association.2015; 74(3): 113. CrossRef
- Cytological Features of a Metastatic Angiosarcoma in the Lymph Node Diagnosed via Liquid-Based Cytology
- Current Concepts in Primary Effusion Lymphoma and Other Effusion-Based Lymphomas
- Yoonjung Kim, Chan Jeong Park, Jin Roh, Jooryung Huh
- Korean J Pathol. 2014;48(2):81-90. Published online April 28, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.2.81
- 16,356 View
- 176 Download
- 30 Crossref
-
 Abstract
Abstract
 PDF
PDF Primary effusion lymphoma (PEL) is a human herpes virus 8 (HHV8)-positive large B-cell neoplasm that presents as an effusion with no detectable tumor in individuals with human immunodeficiency virus infection or other immune deficiencies. PEL is an aggressive neoplasm with a poor prognosis. PEL cells show diverse morphologies, ranging from immunoblastic or plasmablastic to anaplastic. The immunophenotype of PEL is distinct, but its lineage can be misdiagnosed if not assessed thoroughly. PEL cells usually express CD45, lack B- and T-cell-associated antigens, and characteristically express lymphocyte activation antigens and plasma cell-associated antigens. Diagnosis of PEL often requires the demonstration of a B-cell genotype. HHV8 must be detected in cells to diagnose PEL. In most cases, PEL cells also harbor the Epstein-Barr virus (EBV) genome. Similar conditions associated with HHV8 but not effusion-based are called "extracavitary PELs." PELs should be differentiated from HHV8-negative, EBV-positive, body cavity-based lymphomas in patients with long-standing chronic inflammation; the latter can occur in tuberculous pleuritis, artificial pneumothorax, chronic liver disease and various other conditions. Despite their morphological similarity, these various lymphomas require different therapeutic strategies and have different prognostic implications. Correct diagnosis is essential to manage and predict the outcome of patients with PEL and related disorders.
-
Citations
Citations to this article as recorded by- Imaging Findings of Thoracic Extranodal Lymphoma: A Pictorial Essay
Songa Seo, Soo-yeon Jeong, Mi Sook Lee
Journal of the Korean Society of Radiology.2025; 86(6): 1011. CrossRef - Update: The molecular spectrum of virus-associated high-grade B-cell non-Hodgkin lymphomas
H. Witte, A. Künstner, N. Gebauer
Blood Reviews.2024; 65: 101172. CrossRef - Oncolytic strategy using new bifunctional HDACs/BRD4 inhibitors against virus-associated lymphomas
Jungang Chen, Zhengyu Wang, Tran Phuc, Zhigang Xu, Donglin Yang, Zhengzhu Chen, Zhen Lin, Samantha Kendrick, Lu Dai, Hong-yu Li, Zhiqiang Qin, Michael Lagunoff
PLOS Pathogens.2023; 19(1): e1011089. CrossRef - Primary Effusion Lymphoma: A Timely Review on the Association with HIV, HHV8, and EBV
Chih-Yi Liu, Bo-Jung Chen, Shih-Sung Chuang
Diagnostics.2022; 12(3): 713. CrossRef - Lymphoproliferative disorder involving body fluid: diagnostic approaches and roles of ancillary studies
Jiwon Koh, Sun Ah Shin, Ji Ae Lee, Yoon Kyung Jeon
Journal of Pathology and Translational Medicine.2022; 56(4): 173. CrossRef - Clinical Characteristics and Management of Patients With Concomitant Liver Cirrhosis and Lymphoma: A Systematic Review
Jelena Jelicic, Thomas Stauffer Larsen, Annette Dam Fialla, Zoran Bukumiric, Bosko Andjelic
Clinical Lymphoma Myeloma and Leukemia.2022; 22(11): e981. CrossRef - HHV8-unrelated primary effusion lymphoma: Two case reports and a review of literature
Ryan W. Kendall, Ricky A. Thompson, Christopher P. Garwacki, Alan Z. Skarbnik
Current Problems in Cancer: Case Reports.2021; 4: 100087. CrossRef - Targeting Host Cellular Factors as a Strategy of Therapeutic Intervention for Herpesvirus Infections
Kumari Asha, Neelam Sharma-Walia
Frontiers in Cellular and Infection Microbiology.2021;[Epub] CrossRef - A Rare Case of Extracavitary Primary Effusion Lymphoma in the Bladder and Ureter
Jiankun Tong, Sana Jadallah, William H. Rodgers, Gabriel Jung, Malvina Fulman, Abhisek Swaika
Case Reports in Hematology.2020; 2020: 1. CrossRef - KSHV: Immune Modulation and Immunotherapy
Grant Broussard, Blossom Damania
Frontiers in Immunology.2020;[Epub] CrossRef - Role of Ki 67 Labelling Index as an Adjunct to Histopathological Diagnosis for Grading of CNS Tumours
Priyanka Rai, Chandni Krishnani, Goswami S. S.
Journal of Evolution of Medical and Dental Sciences.2020; 9(16): 1331. CrossRef - Brentuximab vedotin as frontline treatment for HIV-related extracavitary primary effusion lymphoma
Jose D. Sandoval-Sus, Amanda Brahim, Alina Khan, Barbara Raphael, Ali Ansari-Lari, Marco Ruiz
International Journal of Hematology.2019; 109(5): 622. CrossRef - High-dose Therapy and Autologous Hematopoietic Cell Transplantation as Consolidation Treatment for Primary Effusion Lymphoma
Abu-Sayeef Mirza, Bhagirathbhai R. Dholaria, Mohammad Hussaini, Sarah Mushtaq, Pedro Horna, Adharsh Ravindran, Ambuj Kumar, Ernesto Ayala, Mohamed A. Kharfan-Dabaja, Celeste Bello, Julio C. Chavez, Lubomir Sokol
Clinical Lymphoma Myeloma and Leukemia.2019; 19(9): e513. CrossRef - Remission of an HHV8-related extracavitary primary effusion lymphoma in an HIV-positive patient during antiretroviral treatment containing dolutegravir
Laura Campogiani, Carlotta Cerva, Gaetano Maffongelli, Elisabetta Teti, Livio Pupo, Sara Vaccarini, Maria Cantonetti, Alfredo Pennica, Massimo Andreoni, Loredana Sarmati
AIDS Research and Therapy.2019;[Epub] CrossRef - Primary Effusion Lymphoma in a Non-Human Immunodeficiency Virus Patient: A Case Report
Beum Jin Kim, Mi Sook Lee
Journal of the Korean Society of Radiology.2019; 80(4): 810. CrossRef - Pleural effusion in a human immunodeficiency virus‐infected patient
Rafael Martínez‐Girón, Santiago Martínez‐Torre
Cytopathology.2019; 30(6): 673. CrossRef - Case report of a primary effusion lymphoma successfully treated with oral valganciclovir after failing chemotherapy
Juan Marquet, Kyra Velazquez‐Kennedy, Sandra López, Amparo Benito, María‐Jesús Blanchard, Jose Antonio Garcia‐Vela
Hematological Oncology.2018; 36(1): 316. CrossRef - Primary effusion lymphoma in Taiwan shows two distinctive clinicopathological subtypes with rare human immunodeficiency virus association
Bo‐Jung Chen, Ran‐Ching Wang, Chung‐Han Ho, Chang‐Tsu Yuan, Wan‐Ting Huang, Sheau‐Fang Yang, Pin‐Pen Hsieh, Yun‐Chih Yung, Shih‐Yao Lin, Chen‐Fang Hsu, Ying‐Zhen Su, Chun‐Chi Kuo, Shih‐Sung Chuang
Histopathology.2018; 72(6): 930. CrossRef - Effusion‐based lymphoma with morphological regression but with clonal genetic features after aspiration
Meng‐Chen Tsai, Chun‐Chi Kuo, Ying‐Zhen Su, Yen‐Chuan Hsieh, Shih‐Sung Chuang
Diagnostic Cytopathology.2018; 46(8): 685. CrossRef - Biology and management of primary effusion lymphoma
Kazuyuki Shimada, Fumihiko Hayakawa, Hitoshi Kiyoi
Blood.2018; 132(18): 1879. CrossRef - EBV‐associated but HHV8‐unrelated double‐hit effusion‐based lymphoma
Bo‐Jung Chen, David Yen‐Ting Chen, Chun‐Chi Kuo, Shih‐Sung Chuang
Diagnostic Cytopathology.2017; 45(3): 257. CrossRef - HHV8/KSHV-Positive Lymphoproliferative Disorders and the Spectrum of Plasmablastic and Plasma Cell Neoplasms
Amy Chadburn, Jonathan Said, Dita Gratzinger, John K. C. Chan, Daphne de Jong, Elaine S. Jaffe, Yasodha Natkunam, John R. Goodlad
American Journal of Clinical Pathology.2017; 147(2): 171. CrossRef - Human immunodeficiency virus (HIV) and Epstein-Barr virus (EBV) related lymphomas, pathology view point
Ebru Linke-Serinsöz, Falko Fend, Leticia Quintanilla-Martinez
Seminars in Diagnostic Pathology.2017; 34(4): 352. CrossRef - Anticancer drug-loaded quantum dots engineered polymeric nanoparticles: Diagnosis/therapy combined approach
D. Belletti, G. Riva, M. Luppi, G. Tosi, F. Forni, M.A. Vandelli, B. Ruozi, F. Pederzoli
European Journal of Pharmaceutical Sciences.2017; 107: 230. CrossRef - CD20-negative diffuse large B cell lymphoma: a comprehensive analysis of 695 cases
Jing Li, Shu Zhao, Jingxuan Wang, Jingyu Chen, Wen Wen, Qingyuan Zhang
Tumor Biology.2016; 37(3): 3619. CrossRef - Co-infections and Pathogenesis of KSHV-Associated Malignancies
Suhani Thakker, Subhash C. Verma
Frontiers in Microbiology.2016;[Epub] CrossRef - Pathology of Extranodal Lymphoma
Emily Heckendorn, Aaron Auerbach
Radiologic Clinics of North America.2016; 54(4): 639. CrossRef - 2015 update on the diagnosis and management of neoplastic pericardial disease
Chiara Lestuzzi, Massimiliano Berretta, Witold Tomkowski
Expert Review of Cardiovascular Therapy.2015; 13(4): 377. CrossRef - CD20-negative diffuse large B-cell lymphomas: biology and emerging therapeutic options
Jorge J Castillo, Julio C Chavez, Francisco J Hernandez-Ilizaliturri, Santiago Montes-Moreno
Expert Review of Hematology.2015; 8(3): 343. CrossRef - Primary Effusion Lymphoma: Cytological Diagnosis of a Rare Entity - Report of Two Cases in HIV-Uninfected Patients from a Single Institution
Marta Nicola, Monica Onorati, Chiara Luisa Bianchi, Giuseppe Pepe, Stefano Bellone, Franca Di Nuovo
Acta Cytologica.2015; 59(5): 425. CrossRef
- Imaging Findings of Thoracic Extranodal Lymphoma: A Pictorial Essay
- Uncommon and Rare Human Papillomavirus Genotypes Relating to Cervical Carcinomas
- Na Rae Kim, Myunghee Kang, Soon Pyo Lee, Hyunchul Kim, Jungsuk An, Dong Hae Chung, Seung Yeon Ha, Hyun Yee Cho
- Korean J Pathol. 2014;48(1):43-49. Published online February 25, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.1.43
- 10,888 View
- 56 Download
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Human papillomavirus (HPV) is an oncogenic virus in cervical cancer and most invasive carcinomas (ICs) are caused by HPV16 and 18. However, the roles and contributions of other uncommon and rare genotypes remain uncertain.
Methods HPV genotypes were retrospectively assessed using an HPV DNA chip that can specify up to 32 HPV genotypes. We arbitrarily regarded genotypes accounting for less than 6% of the total as uncommon and rare genotypes.
Results A total of 3,164 HPV-positive cases were enrolled. In groups 2A, 2B, 3, and unclassified HPV genotypes, 2.4% of cases with uncommon HPV genotypes (68, 26, 34, 53, 66, 69, 70, 73, 40, 42, 43, 44, 54, 55, 61, 62, 6, and 11) showed high grade squamous intraepithelial lesions and ICs. There were no HPV32- and 57-infected cases.
Conclusions We found that the uncommon and rare HPV genotypes may provide incremental etiologic contributions in cervical carcinogenesis, especially HPV68, 70, and 53. Further studies on these uncommon and rare HPV genotypes will be of importance in establishing the significance of genotypes in different regions, especially in planning a strategy for further vaccine development as well as follow-up on the effectiveness of the currently used vaccines.
-
Citations
Citations to this article as recorded by- High-risk human papillomavirus diversity among indigenous women of western Botswana with normal cervical cytology and dysplasia
Patricia S. Rantshabeng, Billy M. Tsima, Andrew K. Ndlovu, Keneilwe Motlhatlhedi, Kirthana Sharma, Carol B. Masole, Natasha O. Moraka, Kesego Motsumi, Angela K. T. Maoto-Mokote, Alemayehu B. Eshetu, Leabaneng Tawe, Tendani Gaolathe, Sikhulile Moyo, Lynnet
BMC Infectious Diseases.2024;[Epub] CrossRef - Human Papillomavirus (HPV69/HPV73) Coinfection associated with Simultaneous Squamous Cell Carcinoma of the Anus and Presumed Lung Metastasis
Stephanie Shea, Marina Muñoz, Stephen C. Ward, Mary B. Beasley, Melissa R Gitman, Michael D Nowak, Jane Houldsworth, Emilia Mia Sordillo, Juan David Ramirez, Alberto E. Paniz Mondolfi
Viruses.2020; 12(3): 349. CrossRef - Human Papillomavirus Selected Properties and Related Cervical Cancer Prevention Issues
Saule Balmagambetova, Andrea Tinelli, Ospan A. Mynbaev, Arip Koyshybaev, Olzhas Urazayev, Nurgul Kereyeva, Elnara Ismagulova
Current Pharmaceutical Design.2020; 26(18): 2073. CrossRef - Periungual Bowen's disease with a narrow longitudinal melanonychia mimicking periungual warts
Taiyo HITAKA, Michiko HASEGAWA, Akira SHIMIZU, Yuko KURIYAMA, Atsushi TAMURA
Skin Cancer.2019; 33(3): 211. CrossRef - Detection of HPV RNA molecules in stratified mucin-producing intraepithelial lesion (SMILE) with concurrent cervical intraepithelial lesion: a case report
Shiho Fukui, Kazunori Nagasaka, Naoko Iimura, Ranka Kanda, Takayuki Ichinose, Takeru Sugihara, Haruko Hiraike, Shunsuke Nakagawa, Yuko Sasajima, Takuya Ayabe
Virology Journal.2019;[Epub] CrossRef - Pitfalls of commercially available HPV tests in HPV68a detection
Hana Jaworek, Katerina Kubanova, Vladimira Koudelakova, Rastislav Slavkovsky, Jiri Drabek, Marian Hajduch, Craig Meyers
PLOS ONE.2019; 14(8): e0220373. CrossRef - Overall accuracy of cervical cytology and clinicopathological significance of LSIL cells in ASC‐H cytology
S. H. Kim, J. M. Lee, H. G. Yun, U. S. Park, S. U. Hwang, J.‐S. Pyo, J. H. Sohn
Cytopathology.2017; 28(1): 16. CrossRef - Human papillomavirus genotyping by Linear Array and Next-Generation Sequencing in cervical samples from Western Mexico
María Guadalupe Flores-Miramontes, Luis Alberto Torres-Reyes, Liliana Alvarado-Ruíz, Salvador Angel Romero-Martínez, Verenice Ramírez-Rodríguez, Luz María Adriana Balderas-Peña, Verónica Vallejo-Ruíz, Patricia Piña-Sánchez, Elva Irene Cortés-Gutiérrez, Lu
Virology Journal.2015;[Epub] CrossRef - Impact of human papillomavirus coinfections on the risk of high-grade squamous intraepithelial lesion and cervical cancer
Adela Carrillo-García, Sergio Ponce-de-León-Rosales, David Cantú-de-León, Verónica Fragoso-Ontiveros, Imelda Martínez-Ramírez, Asunción Orozco-Colín, Alejandro Mohar, Marcela Lizano
Gynecologic Oncology.2014; 134(3): 534. CrossRef - Human papillomavirus 66‐associated subungual squamous cell carcinoma
Jin Hee Kang, Hwa young Ahn, Miri Kim, Shin Taek Oh, Baik Kee Cho, Hyun Jeong Park
The Journal of Dermatology.2014; 41(12): 1119. CrossRef
- High-risk human papillomavirus diversity among indigenous women of western Botswana with normal cervical cytology and dysplasia
- Altered Expression of PTEN and Its Major Regulator MicroRNA-21 in Pulmonary Neuroendocrine Tumors
- Hyoun Wook Lee, Seung Yeon Ha, Mee Sook Roh
- Korean J Pathol. 2014;48(1):17-23. Published online February 25, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.1.17
- 9,286 View
- 46 Download
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Phosphatase and tensin homolog on chromosome ten (PTEN) is one of the most frequently inactivated tumor suppressors in various tumor types. MicroRNA-21 (miR-21) may affect tumor progression by post-transcriptional repression of expression of tumor suppressors, such as PTEN. This study was conducted to evaluate the significance of PTEN expression in pulmonary neuroendocrine (NE) tumors and to analyze the relationship between PTEN and miR-21 expressions.
Methods Expressions of PTEN and miR-21 were investigated by immunohistochemistry and real time reverse transcription-polymerase chain reaction, respectively, in 75 resected pulmonary NE tumors (23 typical carcinoids [TCs], nine atypical carcinoids [ACs], 22 large cell NE carcinomas [LCNECs], and 21 small cell lung carcinomas [SCLCs]).
Results Loss of PTEN expression was observed in four of 23 TCs (17.4%), four of nine ACs (44.4%), 16 of 22 LCNECs (72.7%) and nine of 21 SCLCs (42.9%) (p=.025). The expression level of miR-21 was significantly higher in high-grade NE carcinomas than in carcinoid tumors (p<.001). PTEN expression was inversely correlated with miR-21 expression (p<.001).
Conclusions This study suggests that aberrant expression of PTEN in relation to miR-21 may represent an important step in the development and progression of pulmonary NE tumors.
-
Citations
Citations to this article as recorded by- Mechanisms of skin wound healing regulated by fibroblast-derived exosomes
Ye Qiu, Xingying Zhu, Xiaoqian Yang, Jiaming Wan
Biochemistry and Biophysics Reports.2025; 44: 102371. CrossRef - Role of microRNAs in regulating cell proliferation, metastasis and chemoresistance and their applications as cancer biomarkers in small cell lung cancer
Monu Pandey, Abhirup Mukhopadhyay, Surender K. Sharawat, Sachin Kumar
Biochimica et Biophysica Acta (BBA) - Reviews on Cancer.2021; 1876(1): 188552. CrossRef - Neuroendocrine Tumors Are Enriched in Cowden Syndrome
Alison Greidinger, Susan Miller-Samuel, Veda N. Giri, Michele Sue-Ann Woo, Saranya Akumalla, Charnita Zeigler-Johnson, Scott W. Keith, Daniel P. Silver
JCO Precision Oncology.2020; (4): 551. CrossRef - Prognostic and predictive role of the PI3K–AKT–mTOR pathway in neuroendocrine neoplasms
P. Gajate, T. Alonso-Gordoa, O. Martínez-Sáez, J. Molina-Cerrillo, E. Grande
Clinical and Translational Oncology.2018; 20(5): 561. CrossRef - Genetic and epigenetic drivers of neuroendocrine tumours (NET)
Annunziata Di Domenico, Tabea Wiedmer, Ilaria Marinoni, Aurel Perren
Endocrine-Related Cancer.2017; 24(9): R315. CrossRef - Expression of hsa-let-7b-5p, hsa-let-7f-5p, and hsa-miR-222-3p and their putative targets HMGA2 and CDKN1B in typical and atypical carcinoid tumors of the lung
Pietro Di Fazio, Moritz Maass, Silvia Roth, Christian Meyer, Joana Grups, Peter Rexin, Detlef K Bartsch, Andreas Kirschbaum
Tumor Biology.2017; 39(10): 101042831772841. CrossRef - The regulatory role of aberrant Phosphatase and Tensin Homologue and Liver Kinase B1 on AKT/mTOR/c-Myc axis in pancreatic neuroendocrine tumors
Tsung-Ming Chang, Yan-Shen Shan, Pei-Yi Chu, Shih Sheng Jiang, Wen-Chun Hung, Yu-Lin Chen, Hsiu-Chi Tu, Hui-You Lin, Hui-Jen Tsai, Li-Tzong Chen
Oncotarget.2017; 8(58): 98068. CrossRef - Pulmonary atypical carcinoid in a patient with Cowden syndrome
Hiroaki Tsunezuka, Kaori Abe, Junichi Shimada, Masayoshi Inoue
Interactive CardioVascular and Thoracic Surgery.2016; 22(6): 860. CrossRef - Differential miRNA-Expression as an Adjunctive Diagnostic Tool in Neuroendocrine Tumors of the Lung
Melanie Demes, Christoph Aszyk, Holger Bartsch, Joachim Schirren, Annette Fisseler-Eckhoff
Cancers.2016; 8(4): 38. CrossRef - microRNA-21 promotes osteogenic differentiation of mesenchymal stem cells by the PI3K/β-catenin pathway
Yu-Bin Meng, Xue Li, Zhao-Yang Li, Jin Zhao, Xu-Bo Yuan, Yu Ren, Zhen-Duo Cui, Yun-De Liu, Xian-Jin Yang
Journal of Orthopaedic Research.2015; 33(7): 957. CrossRef - Inhibition of NADPH oxidase protects against metastasis of human lung cancer by decreasing microRNA-21
Song Yan, Gang Liu, Changyan Pei, Wenqing Chen, Pei Li, Qiang Wang, Xintian Jin, Jiajia Zhu, Mengzhu Wang, Xiyu Liu
Anti-Cancer Drugs.2015; 26(4): 388. CrossRef
- Mechanisms of skin wound healing regulated by fibroblast-derived exosomes
- Immunohistochemical Classification of Primary and Secondary Glioblastomas
- Kyu Sang Lee, Gheeyoung Choe, Kyung Han Nam, An Na Seo, Sumi Yun, Kyung Ju Kim, Hwa Jin Cho, Sung Hye Park
- Korean J Pathol. 2013;47(6):541-548. Published online December 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.6.541
- 10,501 View
- 69 Download
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Glioblastomas may develop
de novo (primary glioblastomas, P-GBLs) or through progression from lower-grade astrocytomas (secondary glioblastomas, S-GBLs). The aim of this study was to compare the immunohistochemical classification of glioblastomas with clinically determined P-GBLs and S-GBLs to identify the best combination of antibodies for immunohistochemical classification.Methods We evaluated the immunohistochemical expression of epidermal growth factor receptor (EGFR), p53, and isocitrate dehydrogenase 1 (IDH-1) in 150 glioblastoma cases.
Results According to clinical history, the glioblastomas analyzed in this study consisted of 146 P-GBLs and 4 S-GBLs. Immunohistochemical expression of EGFR, p53, and IDH-1 was observed in 62.6%, 49.3%, and 11.1%, respectively. Immunohistochemical profiles of EGFR(+)/p53(-), IDH-1(-)/EGFR(+)/p53(-), and EGFR(-)/p53(+) were noted in 41.3%, 40.2%, and 28.7%, respectively. Expression of IDH-1 and EGFR(-)/p53(+) was positively correlated with young age. The typical immunohistochemical features of S-GBLs comprised IDH-1(+)/EGFR(-)/p53(+), and were noted in 3.6% of clinically P-GBLs. The combination of IDH-1(-) or EGFR(+) was the best set of immunohistochemical stains for identifying P-GBLs, whereas the combination of IDH-1(+) and EGFR(-) was best for identifying S-GBLs.
Conclusions We recommend a combination of IDH-1 and EGFR for immunohistochemical classification of glioblastomas. We expect our results to be useful for determining treatment strategies for glioblastoma patients.
-
Citations
Citations to this article as recorded by- The Co-Expression and Cellular Location of HER Family Members, EGFRvIII, Putative Cancer Stem Cell Biomarkers CD44 and CD109 in Patients with Glioblastoma, and Their Impacts on Prognosis
Ermira Mulliqi, Said Khelwatty, Izhar Bagwan, Ahmad Kamaludin, Anna Morgan, Natalie Long, Keyoumars Ashkan, Helmout Modjtahedi
Cancers.2025; 17(7): 1221. CrossRef - Predicting p53 Status in IDH‐Mutant Gliomas Using MRI‐Based Radiomic Model
Jiamin Li, Zhihong Lan, Xiao Zhang, Xiaoyun Liang, Hanwei Chen, Xiangrong Yu
Cancer Medicine.2025;[Epub] CrossRef - Classification of Glioblastoma Based on Immunohistochemical Expression of IDH-1, p53, and ATRX: A Study from a Tertiary Care Center in South India
Hiba Thankayathil, Aparna Govindan, Supriya Nilambur Kovilakam, Rajeev Mandaka Parambil
Indian Journal of Neurosurgery.2025; 14(S 01): S48. CrossRef - Endothelial transdifferentiation of glioma stem cells: a literature review
Andrei Buruiana, Stefan Ioan Florian, Alexandru Ioan Florian, Olga Soritau, Sergiu Susman
Acta Neuropathologica Communications.2025;[Epub] CrossRef - Cutaneous Melanoma and Glioblastoma Multiforme Association—Case Presentation and Literature Review
Olguța Anca Orzan, Călin Giurcăneanu, Bogdan Dima, Monica Beatrice Dima, Ana Ion, Beatrice Bălăceanu, Cornelia Nițipir, Irina Tudose, Cătălina Andreea Nicolae, Alexandra Maria Dorobanțu
Diagnostics.2023; 13(6): 1046. CrossRef - Primary Extra-axial Glioblastoma: Case Report and Literature Review
Baraa Dabboucy, Philippe Younes, Abdallah Rahbani, Elie Fahed, Gérard Abadjian
Arquivos Brasileiros de Neurocirurgia: Brazilian Neurosurgery.2021; 40(04): e368. CrossRef - TERT Promoter Mutation in Adult Glioblastomas: It's Correlation with Other Relevant Molecular Markers
Mukesh Barange, Sridhar Epari, Mamta Gurav, Omshree Shetty, Ayushi Sahay, Prakash Shetty, Jayantsastri Goda, Aliasagar Moyiadi, Tejpal Gupta, Rakesh Jalali
Neurology India.2021; 69(1): 126. CrossRef - Immunohistochemical characterisation and histopathology of astrocytic neoplasms at a tertiary Nigerian hospital
Michael Nweke, Gabriel Ogun, Amos Adeleye, Clement A. Okolo, Adekunle Adesina
International Journal of Clinical Practice.2021;[Epub] CrossRef - Cytotoxic Effects of Blue Scorpion Venom (Rhopalurus junceus) in a Glioblastoma Cell Line Model
Laura A. Lozano-Trujillo, Diana K. Garzón-Perdomo, Andrea C.R. Vargas, Lina M. de los Reyes, Marco F. Avila-Rodriguez, Olivia T.G. Gay, Liliana F. Turner
Current Pharmaceutical Biotechnology.2021; 22(5): 636. CrossRef - Molecular Subgroups of Glioblastoma– an Assessment by Immunohistochemical Markers
Ádám Nagy, Ferenc Garzuly, Gergely Padányi, Iván Szűcs, Ádám Feldmann, Balázs Murnyák, Tibor Hortobágyi, Bernadette Kálmán
Pathology & Oncology Research.2019; 25(1): 21. CrossRef - Proteomic Advances in Glial Tumors through Mass Spectrometry Approaches
Radu Pirlog, Sergiu Susman, Cristina Adela Iuga, Stefan Ioan Florian
Medicina.2019; 55(8): 412. CrossRef - Isocitrate dehydrogenase 1 mutant glioblastomas demonstrate a decreased rate of pseudoprogression: a multi-institutional experience
Homan Mohammadi, Kevin Shiue, G Daniel Grass, Vivek Verma, Kay Engellandt, Dirk Daubner, Gabriele Schackert, Mercia J Gondim, Dibson Gondim, Alexander O Vortmeyer, Aaron P Kamer, William Jin, Timothy J Robinson, Gordon Watson, Hsiang-Hsuan M Yu, Tim Laute
Neuro-Oncology Practice.2019;[Epub] CrossRef - Calvarium mass as the first presentation of glioblastoma multiforme: A very rare manifestation of high-grade glioma
S. Taghipour Zahir, M. Mortaz, M. Baghi Yazdi, N. Sefidrokh Sharahjin, M. Shabani
Neurochirurgie.2018; 64(1): 76. CrossRef - Malignant Gliomas as Second Neoplasms in Pediatric Cancer Survivors: Neuropathological Study
Ewa Izycka-Swieszewska, Ewa Bien, Joanna Stefanowicz, Edyta Szurowska, Ewa Szutowicz-Zielinska, Magdalena Koczkowska, Dawid Sigorski, Wojciech Kloc, Wojciech Rogowski, Elzbieta Adamkiewicz-Drozynska
BioMed Research International.2018; 2018: 1. CrossRef - Prognostic significance of mutant IDH1, CD133, and β-catenin immunohistochemical expression in glioblastoma multiforme
Azza Abdel-Aziz, Mie A. Mohamed, Dina Abdallah, Fatma M.F. Akl, Ghada E. Eladawy, Ahmed N. Taha, Hossam Shata
Egyptian Journal of Pathology.2018; 38(1): 27. CrossRef - On glioblastoma and the search for a cure: where do we stand?
John Bianco, Chiara Bastiancich, Aleksander Jankovski, Anne des Rieux, Véronique Préat, Fabienne Danhier
Cellular and Molecular Life Sciences.2017; 74(13): 2451. CrossRef - Expression of p53 & epidermal growth factor receptor in glioblastoma
Sameera Karnam, Radhika Kottu, Amit Kumar Chowhan, Prasad Chandramouleswara Bodepati
Indian Journal of Medical Research.2017; 146(6): 738. CrossRef - Development of Glioblastoma after Treatment of Brain Abscess
Hiroaki Matsumoto, Hiroaki Minami, Shogo Tominaga, Yasuhisa Yoshida
World Neurosurgery.2016; 88: 686.e19. CrossRef - Clinical, immunohistochemical, and molecular genetic prognostic factors in adult patients with glioblastoma
N. V. Lobanova, L. V. Shishkina, M. V. Ryzhova, G. L. Kobyakov, R. V. Sycheva, S. A. Burov, A. V. Lukyanov, Zh. R. Omarova
Arkhiv patologii.2016; 78(4): 10. CrossRef - Concordance analysis and diagnostic test accuracy review of IDH1 immunohistochemistry in glioblastoma
Jung-Soo Pyo, Nae Yu Kim, Roy Hyun Jai Kim, Guhyun Kang
Brain Tumor Pathology.2016; 33(4): 248. CrossRef - Methyl Guanine Methyl Transferase Methylation Status and Epidermal Growth Factor Receptor expression in a cohort of Egyptian glioblastoma patients
Soheir M. Hamam, Bassma M. El Sabaa, Iman M. Talaat, Rasha A. Nassra, Doaa A. Abdelmonsif
Egyptian Journal of Pathology.2016; 36(2): 282. CrossRef
- The Co-Expression and Cellular Location of HER Family Members, EGFRvIII, Putative Cancer Stem Cell Biomarkers CD44 and CD109 in Patients with Glioblastoma, and Their Impacts on Prognosis
- MAD2 Expression in Ovarian Carcinoma: Different Expression Patterns and Levels among Various Types of Ovarian Carcinoma and Its Prognostic Significance in High-Grade Serous Carcinoma
- Po Eun Park, Ji Yun Jeong, Sun Zoo Kim, Ji Young Park
- Korean J Pathol. 2013;47(5):418-425. Published online October 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.5.418
- 8,438 View
- 40 Download
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Mitotic arrest deficiency protein 2 (MAD2) is a key component of spindle assembly checkpoint function, which mediates cell apoptosis through microtubule kinetics. Aberrant expression of MAD2 is believed to be associated with the development of chromosome instability. MAD2 also has a signihicant role in cellular drug resistance to taxane chemotherapeutic agents.
Methods Expression of MAD2 and p53 was investigated using immunohistochemistry in 85 cases of ovarian carcinomas. Clinicopathological data including progression-free survival were analyzed.
Results A significant (p=.035) association was observed between the grade of serous carcinoma and the expression level of MAD2. While low-grade serous carcinoma showed a low-level expression of MAD2, high-grade serous carcinoma showed a high-level expression of MAD2. We also determined that low-level expression of MAD2 was associated with reduced progression-free survival (PFS) (p=.016) in high-grade serous carcinoma.
Conclusions MAD2 expression in ovarian carcinoma is related to the grade of serous carcinoma and PFS of high-grade serous carcinoma. Expression level of MAD2 detected by immunohistochemistry may serve as an indicator in predicting the response of microtubule-interfering chemotherapeutic agents.
-
Citations
Citations to this article as recorded by- MAD2L1 supports MYC-driven liver carcinogenesis in mice and predicts poor prognosis in human hepatocarcinoma
Xinjun Lu, Ya Zhang, Jiahao Xue, Matthias Evert, Diego Calvisi, Xin Chen, Xue Wang
Toxicological Sciences.2025; 203(1): 41. CrossRef - Checkpoint Genes in Check: Impact of BUB1, BUB1B, and MAD2 Alterations on the Treatment Outcomes of Advanced Ovarian Cancer
Sinjini Sarkar, Ranita Pal, Trisha Choudhury, Manisha Vernekar, Puja Chatterjee, Kalyan Kusum Mukherjee, Partha Nath, Santosh Kumar Behera, Sunil Kumar, Vilas D. Nasare
Journal of Current Oncological Trends.2025; 2(1): 72. CrossRef - Biomarkers in high grade serous ovarian cancer
Mark Bates, Bashir M. Mohamed, Faye Lewis, Sharon O’Toole, John J. O’Leary
Biochimica et Biophysica Acta (BBA) - Reviews on Cancer.2024; 1879(6): 189224. CrossRef - The role of the MAD2-TLR4-MyD88 axis in paclitaxel resistance in ovarian cancer
Mark Bates, Cathy D. Spillane, Michael F. Gallagher, Amanda McCann, Cara Martin, Gordon Blackshields, Helen Keegan, Luke Gubbins, Robert Brooks, Doug Brooks, Stavros Selemidis, Sharon O’Toole, John J. O’Leary, David Wai Chan
PLOS ONE.2020; 15(12): e0243715. CrossRef - Aneuploidy: Cancer strength or vulnerability?
Giorgia Simonetti, Samantha Bruno, Antonella Padella, Elena Tenti, Giovanni Martinelli
International Journal of Cancer.2019; 144(1): 8. CrossRef - The association between MAD2 and prognosis in cancer: a systematic review and meta-analyses
Tara Byrne, Helen G. Coleman, Janine A. Cooper, W. Glenn McCluggage, Amanda McCann, Fiona Furlong
Oncotarget.2017; 8(60): 102223. CrossRef - Identification of transcription factors (TFs) and targets involved in the cholangiocarcinoma (CCA) by integrated analysis
L Yang, S Feng, Y Yang
Cancer Gene Therapy.2016; 23(12): 439. CrossRef - Proteins of the mitotic checkpoint and spindle are related to chromosomal instability and unfavourable prognosis in patients with myelodysplastic syndrome
Kelly Roveran Genga, Francisco Dário Rocha Filho, Francisco Valdeci de Almeida Ferreira, Juliana Cordeiro de Sousa, Fernando Sergio Studart, Silvia Maria Meira Magalhães, Fabíola Fernandes Heredia, Ronald Feitosa Pinheiro
Journal of Clinical Pathology.2015; 68(5): 381. CrossRef
- MAD2L1 supports MYC-driven liver carcinogenesis in mice and predicts poor prognosis in human hepatocarcinoma
- Heterotopic Intestinal Cyst of the Submandibular Gland: A Case Study
- Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Soo Kee Min, Jinwon Seo, Eun Soo Kim, Si Whan Kim, Bumjung Park
- Korean J Pathol. 2013;47(3):279-283. Published online June 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.3.279
- 9,375 View
- 42 Download
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF Heterotopic gastrointestinal cysts are rarely found in the oral cavity. Most of these cysts are lined with gastric mucosa and involve the tongue. There have been no reported heterotopic intestinal cysts of the submandibular gland that are completely lined with colonic mucosa. An 8-year-old girl presented with an enlarging swelling in the left submandibular area, and a 4-cm unilocular cyst was fully excised. The cyst was completely lined with colonic mucosa that was surrounded by smooth muscle layer, and the lining cells were positive for CDX-2, an intestinal marker, indicating a high degree of differentiation. The pathogenesis remains unclear, but it may be related to the misplacement of embryonic rests within the oral cavity during early fetal development. Although heterotopic intestinal cysts rarely occur in the submandibular gland, they should be considered in the differential diagnosis of facial swellings in the pediatric population.
-
Citations
Citations to this article as recorded by- Large oral heterotopic gastrointestinal cyst in a child: A case report and update
Débora Frota Colares, Julliany Taverny Sousa, André Luis Alves Borges, Bárbara de Assis Araújo, José Sandro Pereira da Silva, Lélia Batista de Souza
Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology.2025; 37(5): 1137. CrossRef - Heterotopic gastrointestinal cyst of the oral cavity: A rare clinical report and literature review
Andrea Maldonado, Rubén Muñoz, Jesús Cabrera, José Alcides Almeida de Arruda, Bruno Augusto Benevenuto de Andrade, Mariana Villarroel-Dorrego, Isabella Bittencourt do Valle
Journal of Stomatology Oral and Maxillofacial Surgery.2025; 126(5): 102406. CrossRef - Atypical Extraoral Presentation of a Heterotopic Gastrointestinal Cyst on the Face: A Case Report
Anita Dhupar, Anupama Mukherjee, Anita E Spadigam, Praveen S Kumar
Cureus.2024;[Epub] CrossRef - Heterotopic gastrointestinal cyst in the floor of mouth: a case report
Naoaki SAITO, Satoshi MARUYAMA, Yusuke KATO, Ryoko TAKEUCHI, Jun-ichi TANUMA, Tadaharu KOBAYASHI
Japanese Journal of Oral and Maxillofacial Surgery.2023; 69(1): 27. CrossRef - A case report of oral heterotopic gastrointestinal cysts (HGIC) and review of the literature
Gursimran Kaur Bains, Richard Pilkington, Joanna Stafford, Sunil Bhatia
Oral Surgery.2022; 15(1): 71. CrossRef - A Rare Case of Ectopic Colonic Mucosa Presenting With Airway Compromise in a Neonate
Justin Hall, Fatima Z Aly, Julia Comer, Michael P Gebhard, Thomas Schrepfer
Cureus.2022;[Epub] CrossRef - Ultrasonic Features of Uncommon Congenital Heterotopic Colon and Pancreas in the Neck: An Extremely Rare Case Report
Yingli Wei, Zhihao Pan, Xiaoling Kang, Cuiqing Huang, Dan Chen
Frontiers in Pediatrics.2021;[Epub] CrossRef - Quiste gastrointestinal heterotópico en la cavidad oral
Beatriz Arango de Samper, Eliana Elisa Muñoz López, Estefanía Morales González
Latin American Journal of Oral and Maxillofacial Surgery.2021; 1(1): 40. CrossRef
- Large oral heterotopic gastrointestinal cyst in a child: A case report and update
- Cytological Evaluation and REBA HPV-ID HPV Testing of Newly Developed Liquid-Based Cytology, EASYPREP: Comparison with SurePath
- Youn Soo Lee, Gyungyub Gong, Jin Hee Sohn, Ki Sung Ryu, Jung Hun Lee, Shin Kwang Khang, Kyung-Ja Cho, Yong-Man Kim, Chang Suk Kang
- Korean J Pathol. 2013;47(3):265-274. Published online June 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.3.265
- 12,217 View
- 98 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Background The objective of this study was to evaluate a newly-developed EASYPREP liquid-based cytology method in cervicovaginal specimens and compare it with SurePath.
Methods Cervicovaginal specimens were prospectively collected from 1,000 patients with EASYPREP and SurePath. The specimens were first collected by brushing for SurePath and second for EASYPREP. The specimens of both methods were diagnosed according to the Bethesda System. Additionally, we performed to REBA HPV-ID genotyping and sequencing analysis for human papillomavirus (HPV) on 249 specimens.
Results EASYPREP and SurePath showed even distribution of cells and were equal in cellularity and staining quality. The diagnostic agreement between the two methods was 96.5%. Based on the standard of SurePath, the sensitivity, specificity, positive predictive value, and negative predictive value of EASYPREP were 90.7%, 99.2%, 94.8%, and 98.5%, respectively. The positivity of REBA HPV-ID was 49.4% and 95.1% in normal and abnormal cytological samples, respectively. The result of REBA HPV-ID had high concordance with sequencing analysis.
Conclusions EASYPREP provided comparable results to SurePath in the diagnosis and staining quality of cytology examinations and in HPV testing with REBA HPV-ID. EASYPREP could be another LBC method choice for the cervicovaginal specimens. Additionally, REBA HPV-ID may be a useful method for HPV genotyping.
-
Citations
Citations to this article as recorded by- Virome capture sequencing for comprehensive HPV genotyping in cervical samples
Thanayod Sasivimolrattana, Sasiprapa Liewchalermwong, Wasun Chantratita, Insee Sensorn, Arkom Chaiwongkot, Parvapan Bhattarakosol
Science Progress.2025;[Epub] CrossRef - High-Risk Human Papillomavirus Detection via Cobas® 4800 and REBA HPV-ID® Assays
Sasiprapa Liewchalermwong, Shina Oranratanaphan, Wichai Termrungruanglert, Surang Triratanachat, Patou Tantbirojn, Nakarin Kitkumthorn, Parvapan Bhattarakosol, Arkom Chaiwongkot
Viruses.2022; 14(12): 2713. CrossRef - Evaluation of nuclear chromatin using grayscale intensity and thresholded percentage area in liquid‐based cervical cytology
Hyekyung Lee, Myungein Han, Taejo Yoo, Chanho Jung, Hyun‐Jin Son, Migyung Cho
Diagnostic Cytopathology.2018; 46(5): 384. CrossRef - Comparison of EASYPREP® and SurePath® in thyroid fine‐needle aspiration
Yosep Chong, Ki Hyun Baek, Jee Young Kim, Tae‐Jung Kim, Eun Jung Lee, Chang Suk Kang
Diagnostic Cytopathology.2016; 44(4): 283. CrossRef
- Virome capture sequencing for comprehensive HPV genotyping in cervical samples
- Human Papillomavirus Prevalence and Cell Cycle Related Protein Expression in Tonsillar Squamous Cell Carcinomas of Korean Patients with Clinicopathologic Analysis
- Miji Lee, Sung Bae Kim, Sang-wook Lee, Jong-Lyel Roh, Seung-Ho Choi, Soon Yuhl Nam, Sang Yoon Kim, Kyung-Ja Cho
- Korean J Pathol. 2013;47(2):148-157. Published online April 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.2.148
- 9,393 View
- 52 Download
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Human papillomavirus (HPV)-related tonsillar squamous cell carcinoma (TSCC) has recently been characterized as a distinct subset with a favorable prognosis. The prevalence and clinicopathologic significance of HPV-related TSCC in Koreans are not well known.
Methods HPV
in situ hybridization (ISH) accompanied by p53, p16, pRb, and cyclin D1 immunohistochemical staining were performed on 89 resection cases of TSCC from 2000 through 2010.Results HPV was detected by ISH in 59 of 89 cases (66.3%). HPV-positive TSCCs were more common in younger ages (p=0.005), and tumor sizes were smaller in the HPV-positive compared to the HPV-negative group (p=0.040). Positive HPV staining was significantly correlated with p16 expression (p<0.001), pRb inactivation (p=0.003), and cyclin D1 down-regulation (p<0.001) but not with p53 expression (p=0.334). Seventeen cases that showed p16-immunopositivity with HPV-negativity by ISH were retested by HPV typing; HPV DNA was not detected in all cases. There was no significant difference between HPV-positive and HPV-negative patients either in the disease-specific survival (DSS, p=0.857) or overall survival (p=0.910). Furthermore, pRb-inactivated cases showed better DSS (p=0.023), and p53-positive cases showed worse DSS (p=0.001).
Conclusions Although high HPV prevalence was noted, it was not correlated with histopathologic findings or survival benefit. In addition to p53 expression, pRb inactivation along with p16 overexpression and down-regulation of cyclin D1 are thought to be important pathogenetic steps for developing TSCCs.
-
Citations
Citations to this article as recorded by- Assessment of the Mutation Profile of Tonsillar Squamous Cell Carcinomas Using Targeted Next-Generation Sequencing
Ha Young Park, Joong Seob Lee, Jee Hye Wee, Jeong Wook Kang, Eun Soo Kim, Taeryool Koo, Hee Sung Hwang, Hyo Jung Kim, Ho Suk Kang, Hyun Lim, Nan Young Kim, Eun Sook Nam, Seong Jin Cho, Mi Jung Kwon
Biomedicines.2023; 11(3): 851. CrossRef - Clinicopathologic characterization of cervical metastasis from an unknown primary tumor: a multicenter study in Korea
Miseon Lee, Uiree Jo, Joon Seon Song, Youn Soo Lee, Chang Gok Woo, Dong-Hoon Kim, Jung Yeon Kim, Sun Och Yoon, Kyung-Ja Cho
Journal of Pathology and Translational Medicine.2023; 57(3): 166. CrossRef - Negative Prognostic Implication of TERT Promoter Mutations in Human Papillomavirus–Negative Tonsillar Squamous Cell Carcinoma Under the New 8th AJCC Staging System
Hyunchul Kim, Mi Jung Kwon, Bumjung Park, Hyo Geun Choi, Eun Sook Nam, Seong Jin Cho, Kyueng-Whan Min, Eun Soo Kim, Hee Sung Hwang, Mineui Hong, Taeryool Koo, Hyo Jung Kim
Indian Journal of Surgical Oncology.2021; 12(S1): 134. CrossRef - Prevalence of high-risk human papillomavirus and its genotype distribution in head and neck squamous cell carcinomas
Yuil Kim, Young-Hoon Joo, Min-Sik Kim, Youn Soo Lee
Journal of Pathology and Translational Medicine.2020; 54(5): 411. CrossRef - Frequent hepatocyte growth factor overexpression and low frequency of c-Met gene amplification in human papillomavirus–negative tonsillar squamous cell carcinoma and their prognostic significances
Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Hyung Sik Shin, Ji Hyun Kwon, Dong Jin Lee, Jin Hwan Kim, Seong Jin Cho, Eun Sook Nam
Human Pathology.2014; 45(7): 1327. CrossRef
- Assessment of the Mutation Profile of Tonsillar Squamous Cell Carcinomas Using Targeted Next-Generation Sequencing
- Finding and Characterizing Mammary Analogue Secretory Carcinoma of the Salivary Gland
- Min Jung Jung, Joon Seon Song, Sang Yoon Kim, Soon Yuhl Nam, Jong-Lyel Roh, Seung-Ho Choi, Sung-Bae Kim, Kyung-Ja Cho
- Korean J Pathol. 2013;47(1):36-43. Published online February 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.1.36
- 15,166 View
- 117 Download
- 74 Crossref
-
 Abstract
Abstract
 PDF
PDF Background A new tumor entity of the salivary glands, mammary analogue secretory carcinoma (MASC) with
ETV6-NTRK3 translocation, has recently been proposed. MASC was originally diagnosed as adenocarcinoma, not otherwise specified (ANOS), or acinic cell carcinoma (AciCC) by the current World Health Organization classification. We aimed to identify MASC cases by molecular tests, and to characterize their clinical, histological, and immunohistochemical features.Methods Thirty cases of MASC candidates were selected after review of 196 salivary gland tumors, and subjected to break-apart
ETV6 fluorescencein situ hybridization (FISH), and immunohistochemical study for S100 protein, gross cystic disease fluid protein 15, DOG1, estrogen receptor, and progesterone receptor.Results Valid FISH results were obtained in 23 cases, and 13 positive cases were retrieved. MASCs were histologically varied, and the most frequent features observed in 10 cases were low-grade papillary/cystic/glandular patterns, intraluminal secretory materials, ovoid/wrinkled nuclei, and relatively abundant granular eosinophilic cytoplasms, corresponding to papillary-cystic or follicular types of AciCC. All cases showed diffuse immunopositivity for S100 protein. Three cases developed recurrences, but all patients remained alive.
Conclusions MASC could be a molecularly well-defined salivary gland neoplasm, encompassing some portions of AciCC and ANOS, but its histological spectrum and clinical implication require further investigation.
-
Citations
Citations to this article as recorded by- Rare Tumors of Oral Cavity: A Case Report and Literature Review on Secretory Carcinoma of Minor Salivary Glands
Emilio Salerno, Silvio Abati, Gianluigi Arrigoni, Daniela Finocchiaro, Giorgio Gastaldi, Alessandra Lissoni, Andrea Galli, Matteo Trimarchi
Clinical and Experimental Dental Research.2025;[Epub] CrossRef - Salivary Gland Secretory Carcinoma; Review of 13 Years World‐Wide Experience and Meta‐Analysis
Eyal Yosefof, Tomer Boldes, Daniel Dan, Eyal Robenshtok, Yulia Strenov, Gideon Bachar, Thomas Shpitzer, Aviram Mizrachi
The Laryngoscope.2024; 134(4): 1716. CrossRef - Salivary gland secretory carcinoma presenting as a cervical soft tissue mass: a case report
Parisa Mokhles, Alireza Sadeghipour, Pegah Babaheidarian, Saleh Mohebbi, Zahra Keshtpour Amlashi, Mohammad Hadi Gharib, Mohammad Saeid Ahmadi, Zeinab Khastkhodaei
Journal of Medical Case Reports.2024;[Epub] CrossRef - Mammary analogue secretory carcinoma of the head and neck — Clinicopathological, imaging features and prognosis analysis
Runjia Liu, Chuanzheng Sun, Likang Zhao, Shiyu Zhou, Tao Xie, Ji Zhang, Dengpeng Tang, Lei Li, Yan Xi
Journal of Radiation Research and Applied Sciences.2024; 17(2): 100914. CrossRef - Mammary analogue secretory carcinoma involving submandibular gland: Diagnostic pitfall with review of literature
Nimisha Dhankar, Nidhi Verma, Abhinav Agarwal, Ravi Mehar, Sunil Pasricha
Journal of Cancer Research and Therapeutics.2024; 20(5): 1658. CrossRef - Metastatic salivary gland mammary analogue secretory carcinoma (MASC) of parotid gland – A rare case report in the literature review
Aynur Aliyeva, Ziya Karimov, Togay Muderris
Acta Oto-Laryngologica Case Reports.2023; 8(1): 38. CrossRef - Secretory carcinoma of minor salivary glands of buccal mucosa
Noshad Ali Langah, Abdul Ahad, Shayan Khalid Ghaloo, Muhammad Faisal, Raza Tasawar Hussain, Fareed Akbar Shah
International Journal of Surgery Case Reports.2023;[Epub] CrossRef - An Underappreciated Cytomorphological Feature of Secretory Carcinoma of Salivary Gland on Fine Needle Aspiration Biopsy: Case Report with Literature Review
Yinan Hua, Bing Leng, Kenneth E. Youens, Lina Liu
Head and Neck Pathology.2022; 16(2): 567. CrossRef - Clinicopathological investigation of secretory carcinoma cases including a successful treatment outcome using entrectinib for high-grade transformation: a case report
Kensuke Suzuki, Hiroshi Harada, Masayuki Takeda, Chisato Ohe, Yoshiko Uemura, Akihiko Kawahara, Shunsuke Sawada, Akira Kanda, Bhaswati Sengupta, Hiroshi Iwai
BMC Medical Genomics.2022;[Epub] CrossRef - DOG1 as an Immunohistochemical Marker of Acinic Cell Carcinoma: A Systematic Review and Meta-Analysis
Vincenzo Fiorentino, Patrizia Straccia, Pietro Tralongo, Teresa Musarra, Francesco Pierconti, Maurizio Martini, Guido Fadda, Esther Diana Rossi, Luigi Maria Larocca
International Journal of Molecular Sciences.2022; 23(17): 9711. CrossRef - Secretory carcinoma of the sinonasal cavity and pharynx: A retrospective analysis of four cases and literature review
Changli Yue, Xiaoli Zhao, Donglin Ma, Yingshi Piao
Annals of Diagnostic Pathology.2022; 61: 152052. CrossRef - Secretory carcinoma of the salivary gland: a multi‐institutional clinicopathologic study of 90 cases with emphasis on grading and prognostic factors
Bin Xu, Kartik Viswanathan, Kavita Umrau, Thair A. D. Al‐Ameri, Snjezana Dogan, Kelly Magliocca, Ronald A. Ghossein, Nicole A. Cipriani, Nora Katabi
Histopathology.2022; 81(5): 670. CrossRef - A systematic review of secretory carcinoma of the salivary gland: where are we?
Lísia Daltro Borges Alves, Andreia Cristina de Melo, Thayana Alves Farinha, Luiz Henrique de Lima Araujo, Leandro de Souza Thiago, Fernando Luiz Dias, Héliton Spíndola Antunes, Ana Lucia Amaral Eisenberg, Luiz Claudio Santos Thuler, Daniel Cohen Goldember
Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.2021; 132(4): e143. CrossRef - A case report of surgical resection of secretory carcinoma in the maxillary and ethmoid sinus
Kurt Willis, Martin Bullock, Matthew H. Rigby
International Journal of Surgery Case Reports.2021; 81(C): 105750. CrossRef - High‐grade salivary gland carcinoma with the ETV6‐NTRK3 gene fusion: A case report and literature review of secretory carcinoma with high‐grade transformation
Satsuki Asai, Shinji Sumiyoshi, Yosuke Yamada, Ichiro Tateya, Toshitaka Nagao, Sachiko Minamiguchi, Hironori Haga
Pathology International.2021; 71(6): 427. CrossRef - High-grade Transformation/Dedifferentiation in Salivary Gland Carcinomas: Occurrence Across Subtypes and Clinical Significance
Alena Skalova, Ilmo Leivo, Henrik Hellquist, Abbas Agaimy, Roderick H.W. Simpson, Göran Stenman, Vincent Vander Poorten, Justin A. Bishop, Alessandro Franchi, Juan C. Hernandez-Prera, David Slouka, Stefan M. Willems, Kerry D. Olsen, Alfio Ferlito
Advances in Anatomic Pathology.2021; 28(3): 107. CrossRef - Radiological features of head and neck mammary analogue secretory carcinoma: 11 new cases with a systematic review of 29 cases reported in 28 publications
Ryo Kurokawa, Mariko Kurokawa, Akira Baba, Yoshiaki Ota, Toshio Moritani, Ashok Srinivasan
Neuroradiology.2021; 63(11): 1901. CrossRef - A case of secretory carcinoma of the salivary glands in the lower lip
Reiko OHARA, Haruki SATO, Kensuke NAGANAWA, Taihei HAYAKAWA, Tatsuya KATAOKA, Ichiro OH-IWA
Japanese Journal of Oral and Maxillofacial Surgery.2021; 67(2): 83. CrossRef - Undifferentiated and dedifferentiated head and neck carcinomas
Alessandro Franchi, Alena Skalova
Seminars in Diagnostic Pathology.2021; 38(6): 127. CrossRef - Cytopathological Findings of Secretory Carcinoma of the Salivary Gland and the Diagnostic Utility of Giemsa Staining
Yuria Egusa, Midori Filiz Nishimura, Satoko Baba, Kengo Takeuchi, Takuma Makino, Tomoyasu Tachibana, Asami Nishikori, Azusa Fujita, Hiroyuki Yanai, Yasuharu Sato
Diagnostics.2021; 11(12): 2284. CrossRef - Diagnosis and treatment of secretory carcinoma arising from the oral minor salivary gland
Masaru Ogawa, Satoshi Yokoo, Takahiro Yamaguchi, Keisuke Suzuki, Mai Seki-Soda, Takahiro Shimizu, Jun Kurihara, Takaya Makiguchi
Medicine.2021; 100(51): e28390. CrossRef - A biphasic sessile mass of the buccal mucosa
Tiffany M. Peters, James A. Phero, Brent A. Golden, Alice E. Curran
Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.2020; 130(6): 612. CrossRef - Don't stop the champions of research now: a brief history of head and neck pathology developments
Lester D.R. Thompson, James S. Lewis, Alena Skálová, Justin A. Bishop
Human Pathology.2020; 95: 1. CrossRef - High Grade Transformation in Mucoepidermoid Carcinoma of the Minor Salivary Gland with Polyploidy of the Rearranged MAML2 Gene
Hyun Lee, Jong-Lyel Roh, Young-Jun Choi, Jene Choi, Kyung-Ja Cho
Head and Neck Pathology.2020; 14(3): 822. CrossRef - Pan‐Trk immunohistochemistry is a sensitive and specific ancillary tool for diagnosing secretory carcinoma of the salivary gland and detecting ETV6–NTRK3 fusion
Bin Xu, Mohamed R Haroon Al Rasheed, Cristina R Antonescu, Deepu Alex, Denise Frosina, Ronald Ghossein, Achim A Jungbluth, Nora Katabi
Histopathology.2020; 76(3): 375. CrossRef - Characterization of novel genetic alterations in salivary gland secretory carcinoma
Kiyong Na, Juan C. Hernandez-Prera, Jae-Yol Lim, Ha Young Woo, Sun Och Yoon
Modern Pathology.2020; 33(4): 541. CrossRef - Mammary analogue secretory carcinoma: An Indian experience of a novel entity
Zeba Nisar, JaydeepN Pol, RakhiV Jagdale, MadhuraD Phadke, GirishA Kadkol
Indian Journal of Pathology and Microbiology.2020; 63(5): 134. CrossRef - Secretory Carcinoma of Salivary Gland with High-Grade Histology Arising in Hard Palate: A Case Report
Kiyofumi Takabatake, Keisuke Nakano, Hotaka Kawai, Saori Yoshida, Haruka Omori, May Wathone Oo, Shan Qiusheng, Kenichiro Uchida, Katsuaki Mishima, Hitoshi Nagatsuka
Reports.2020; 3(2): 6. CrossRef - Secretory carcinoma of the salivary gland (mammary analogue secretory carcinoma) in children
I. V. Sidorov, I. S. Kletskaya, D. M. Konovalov
Arkhiv patologii.2020; 82(2): 43. CrossRef - Secretory carcinoma of the major salivary gland: Provincial population‐based analysis of clinical behavior and outcomes
Gareth Ayre, Martin Hyrcza, Jonn Wu, Eric Berthelet, Alena Skálová, Tom Thomson
Head & Neck.2019; 41(5): 1227. CrossRef - Higher Ki67 Index, Nodal Involvement, and Invasive Growth Were High Risk Factors for Worse Prognosis in Conventional Mammary Analogue Secretory Carcinoma
Jingjing Sun, Lizhen Wang, Zhen Tian, Yuhua Hu, Ronghui Xia, Jiang Li
Journal of Oral and Maxillofacial Surgery.2019; 77(6): 1187. CrossRef - Mammary analogue secretory carcinoma of salivary gland diagnosed on submandibular gland cytology: A case report and review of the literature
Ethar Al‐Husseinawi, Soheila Hamidpour, Evanthia Omoscharka
Cytopathology.2019; 30(3): 318. CrossRef - Secretory Carcinoma of Minor Salivary Gland in Buccal Mucosa: A Case Report and Review of the Literature
Durga Paudel, Michiko Nishimura, Bhoj Raj Adhikari, Daichi Hiraki, Aya Onishi, Tetsuro Morikawa, Puja Neopane, Sarita Giri, Koki Yoshida, Jun Sato, Masayuki Ono, Yoshitaka Kamino, Hiroki Nagayasu, Yoshihiro Abiko
Case Reports in Pathology.2019; 2019: 1. CrossRef - Estrogen Receptor, Progesterone Receptor, and HER-2 Expression in Recurrent Pleomorphic Adenoma
Ana Amélia de Souza, Albina Altemani, Ney Soares de Araujo, Lucas Novaes Texeira, Vera Cavalcanti de Araújo, Andresa Borges Soares
Clinical Pathology.2019;[Epub] CrossRef - A Case of Secretory Carcinoma That Occurred in the Buccal Submucosa
Saito Yoshiro, Kurasawa Yuya, Moriya Takashi, Ikeda Kenitiro, Kushihashi Yukiomi, Egawa Shunya, Katsuta Hideyuki, Shimane Toshikazu
International Journal of Otolaryngology and Head & Neck Surgery.2019; 08(06): 191. CrossRef - Sinonasal Secretory Carcinoma of Salivary Gland with High Grade Transformation: A Case Report of this Under-Recognized Diagnostic Entity with Prognostic and Therapeutic Implications
Bin Xu, Ruth Aryeequaye, Lu Wang, Nora Katabi
Head and Neck Pathology.2018; 12(2): 274. CrossRef - Primary mammary analogue secretory carcinoma of the lung: a case report
Tao Huang, Jonathan B. McHugh, Gerald J. Berry, Jeffrey L. Myers
Human Pathology.2018; 74: 109. CrossRef - Salivary Secretory Carcinoma With a Novel ETV6-MET Fusion
Lisa M. Rooper, Theodoros Karantanos, Yi Ning, Justin A. Bishop, Sarah W. Gordon, Hyunseok Kang
American Journal of Surgical Pathology.2018; 42(8): 1121. CrossRef - Secretory carcinoma: The eastern Canadian experience and literature review
David Forner, Martin Bullock, Daniel Manders, Timothy Wallace, Christopher J. Chin, Liane B. Johnson, Matthew H. Rigby, Jonathan R. Trites, Mark S. Taylor, Robert D. Hart
Journal of Otolaryngology - Head & Neck Surgery.2018;[Epub] CrossRef - Newly described salivary gland tumors
Alena Skalova, Michal Michal, Roderick HW Simpson
Modern Pathology.2017; 30: S27. CrossRef - Diagnóstico, tratamiento y seguimiento de un tumor de reciente descripción: el carcinoma análogo secretor de mama (MASC) de glándula salival. A propósito de 2 nuevos casos
Marina Alexandra Gavín-Clavero, M. Victoria Simón-Sanz, Ana M. López-López, Alberto Valero-Torres, Esther Saura-Fillat
Revista Española de Cirugía Oral y Maxilofacial.2017; 39(4): 221. CrossRef - Systematic review of mammary analog secretory carcinoma of salivary glands at 7 years after description
Bacem A. Khalele
Head & Neck.2017; 39(6): 1243. CrossRef - Salivary Gland Secretory Carcinoma With High-Grade Transformation, CDKN2A/B Loss, Distant Metastasis, and Lack of Sustained Response to Crizotinib
Nicole A. Cipriani, Elizabeth A. Blair, Joshua Finkle, Jennifer L. Kraninger, Christopher M. Straus, Victoria M. Villaflor, Daniel Thomas Ginat
International Journal of Surgical Pathology.2017; 25(7): 613. CrossRef - A systematic review including an additional pediatric case report: Pediatric cases of mammary analogue secretory carcinoma
Amanda L. Ngouajio, Sarah M. Drejet, D. Ryan Phillips, Don-John Summerlin, John P. Dahl
International Journal of Pediatric Otorhinolaryngology.2017; 100: 187. CrossRef - Newly Described Entities in Salivary Gland Pathology
Alena Skálová, Douglas R. Gnepp, James S. Lewis, Jennifer L. Hunt, Justin A. Bishop, Henrik Hellquist, Alessandra Rinaldo, Vincent Vander Poorten, Alfio Ferlito
American Journal of Surgical Pathology.2017; 41(8): e33. CrossRef - Mammary Analogue Secretory Carcinoma of Salivary Glands: Diagnostic Pitfall with Distinct Immunohistochemical Profile and Molecular Features
Oliver Bissinger, Carolin Götz, Andreas Kolk, Henning A. Bier, Abbas Agaimy, Henning Frenzel, Sven Perner, Julika Ribbat-Idel, Klaus Dietrich Wolff, Wilko Weichert, Caroline Mogler
Rare Tumors.2017; 9(3): 89. CrossRef - Mammary Analogue Secretory Carcinoma of Salivary Gland. A Case Report Emphasizing its Diagnostic Histological, Immunohistochemistry and Molecular Findings
Monalisa Hui, Shantveer G Uppin, Vamshi Krishna Thamtam, Abhiram Kalle
International Journal of Head and Neck Surgery.2017; 8(4): 160. CrossRef - A case of mammary analog secretory carcinoma of the lower lip
Takako Aizawa, Taro Okui, Ken Kitagawa, Yoshikazu Kobayashi, Koji Satoh, Hideki Mizutani
Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology.2016; 28(3): 277. CrossRef - Mammary analogue secretory carcinoma of parotid: Is preoperative cytological diagnosis possible?
Nikita Oza, Kintan Sanghvi, Tanuja Shet, Asawari Patil, Santosh Menon, Mukta Ramadwar, Shubhada Kane
Diagnostic Cytopathology.2016; 44(6): 519. CrossRef - Lysozyme Expression Can be Useful to Distinguish Mammary Analog Secretory Carcinoma from Acinic Cell Carcinoma of Salivary Glands
Fernanda Viviane Mariano, Camila Andrea Concha Gómez, Juliana de Souza do Nascimento, Harim Tavares dos Santos, Erika Said Egal, Victor Angelo Martins Montalli, Pablo Agustin Vargas, Oslei Paes de Almeida, Albina Altemani
Head and Neck Pathology.2016; 10(4): 429. CrossRef - Cytogenetic and immunohistochemical characterization of mammary analogue secretory carcinoma of salivary glands
Syed A. Khurram, Jemel Sultan-Khan, Neil Atkey, Paul M. Speight
Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.2016; 122(6): 731. CrossRef - The role of DOG1 immunohistochemistry in dermatopathology
Keisuke Goto
Journal of Cutaneous Pathology.2016; 43(11): 974. CrossRef - Extended immunologic and genetic lineage of mammary analogue secretory carcinoma of salivary glands
Hao Ni, Xue-ping Zhang, Xiao-tong Wang, Qiu-yuan Xia, Jing-huan Lv, Xuan Wang, Shan-shan Shi, Rui Li, Xiao-jun Zhou, Qiu Rao
Human Pathology.2016; 58: 97. CrossRef - A New Hitherto Unreported Histopathologic Manifestation of Mammary Analogue Secretory Carcinoma: “Masked MASC” Associated With Low-grade Mucinous Adenocarcinoma and Low-grade In Situ Carcinoma Components
Fredrik Petersson, Michael Michal, Dmitry V. Kazakov, Petr Grossmann, Michal Michal
Applied Immunohistochemistry & Molecular Morphology.2016; 24(9): e80. CrossRef - Papillary-cystic pattern is characteristic in mammary analogue secretory carcinomas but is rarely observed in acinic cell carcinomas of the salivary gland
Min-Shu Hsieh, Yueh-Hung Chou, Shin-Joe Yeh, Yih-Leong Chang
Virchows Archiv.2015; 467(2): 145. CrossRef - Mammary analog secretory carcinoma, low-grade salivary duct carcinoma, and mimickers: a comparative study
Todd M Stevens, Andra O Kovalovsky, Claudia Velosa, Qiuying Shi, Qian Dai, Randall P Owen, Walter C Bell, Shi Wei, Pamela A Althof, Jennifer N Sanmann, Larissa Sweeny, William R Carroll, Gene P Siegal, Martin J Bullock, Margaret Brandwein-Gensler
Modern Pathology.2015; 28(8): 1084. CrossRef - Aspiration cytology of mammary analogue secretory carcinoma of the salivary gland
Min Jung Jung, Sang Yoon Kim, Soon Yuhl Nam, Jong‐Lyel Roh, Seung‐Ho Choi, Jeong Hyun Lee, Jung Hwan Baek, Kyung‐Ja Cho
Diagnostic Cytopathology.2015; 43(4): 287. CrossRef - A Unique Case of a Cutaneous Lesion Resembling Mammary Analog Secretory Carcinoma
Jennifer Albus, Jacqueline Batanian, Bruce M. Wenig, Claudia I. Vidal
The American Journal of Dermatopathology.2015; 37(4): e41. CrossRef - Mammary analogue secretory carcinoma of salivary glands: a new entity associated with ETV6 gene rearrangement
Hanna Majewska, Alena Skálová, Dominik Stodulski, Adéla Klimková, Petr Steiner, Czesław Stankiewicz, Wojciech Biernat
Virchows Archiv.2015; 466(3): 245. CrossRef - A comparative immunohistochemistry study of diagnostic tools in salivary gland tumors: usefulness of mammaglobin, gross cystic disease fluid protein 15, and p63 cytoplasmic staining for the diagnosis of mammary analog secretory carcinoma?
Fabrice Projetti, Magali Lacroix‐Triki, Elie Serrano, Sebastien Vergez, Béatrice Herbault Barres, Julie Meilleroux, Marie‐Bernadette Delisle, Emmanuelle Uro‐Coste
Journal of Oral Pathology & Medicine.2015; 44(4): 244. CrossRef - Mammary Analogue Secretory Carcinoma of Salivary Glands
Yohei Ito, Kenichiro Ishibashi, Ayako Masaki, Kana Fujii, Yukio Fujiyoshi, Hideo Hattori, Daisuke Kawakita, Manabu Matsumoto, Satoru Miyabe, Kazuo Shimozato, Toshitaka Nagao, Hiroshi Inagaki
American Journal of Surgical Pathology.2015; 39(5): 602. CrossRef - Cytopathological features of mammary analogue secretory carcinoma—Review of literature
Maiko Takeda, Takahiko Kasai, Kohei Morita, Mao Takeuchi, Takeshi Nishikawa, Akinori Yamashita, Shinji Mikami, Hiroshi Hosoi, Chiho Ohbayashi
Diagnostic Cytopathology.2015; 43(2): 131. CrossRef - Mammary Analog Secretory Carcinoma of Salivary Glands
Justin A. Bishop
Pathology Case Reviews.2015; 20(1): 7. CrossRef - Diagnostic utility of phosphorylated signal transducer and activator of transcription 5 immunostaining in the diagnosis of mammary analogue secretory carcinoma of the salivary gland: A comparative study of salivary gland cancers
Akihiko Kawahara, Tomoki Taira, Hideyuki Abe, Yorihiko Takase, Takashi Kurita, Eiji Sadashima, Satoshi Hattori, Ichio Imamura, Shinji Matsumoto, Hitomi Fujisaki, Kazunobu Sueyoshi, Jun Akiba, Masayoshi Kage
Cancer Cytopathology.2015; 123(10): 603. CrossRef - A Case of Mammary Analogue Secretory Carcinoma Arising from Parotid Gland
Hee Tae Kim, Cha Hee Lee, Han Su Kim, Hae Sang Park
Korean Journal of Otorhinolaryngology-Head and Neck Surgery.2015; 58(8): 563. CrossRef - WITHDRAWN: A biphasic sessile mass of the buccal mucosa
Tiffany M. Peters, Jose P. Zevallos, Brent A. Golden, Alice E. Curran
Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.2015;[Epub] CrossRef - Mammary analogue secretory carcinoma: an evaluation of its clinicopathological and genetic characteristics
Peter P. Luk, Christina I. Selinger, Timothy J. Eviston, Trina Lum, Bing Yu, Sandra A. O’Toole, Jonathan R. Clark, Ruta Gupta
Pathology.2015; 47(7): 659. CrossRef - A case of mammary analogue secretory carcinoma arising in the submandibular region
Kotaro ISHII, Koji NAKAMATSU, Koji SATO, Chikashi MINEMURA, Wataru KUMAMARU, Hiroyo YOSHIKAWA
Japanese Journal of Oral and Maxillofacial Surgery.2015; 61(11): 564. CrossRef - DOG1, p63, and S100 protein: a novel immunohistochemical panel in the differential diagnosis of oncocytic salivary gland neoplasms in fine-needle aspiration cell blocks
Alessandra C. Schmitt, Ryan McCormick, Cynthia Cohen, Momin T. Siddiqui
Journal of the American Society of Cytopathology.2014; 3(6): 303. CrossRef - Salivary Gland Tumor “Wishes” to Add to the Next WHO Tumor Classification: Sclerosing Polycystic Adenosis, Mammary Analogue Secretory Carcinoma, Cribriform Adenocarcinoma of the Tongue and Other Sites, and Mucinous Variant of Myoepithelioma
Douglas R. Gnepp
Head and Neck Pathology.2014; 8(1): 42. CrossRef - Hepatoid differentiation in renal cell carcinoma: a rare histologic pattern with clinical significance
Jungweon Shim, Heounjeong Go, Young-Suk Lim, Kyung Chul Moon, Jae Y. Ro, Yong Mee Cho
Annals of Diagnostic Pathology.2014; 18(6): 363. CrossRef - Mammary analogue secretory carcinoma: Update on a new diagnosis of salivary gland malignancy
Roshan Sethi, Elliott Kozin, Aaron Remenschneider, Josh Meier, Paul VanderLaan, William Faquin, Daniel Deschler, Robert Frankenthaler
The Laryngoscope.2014; 124(1): 188. CrossRef - Mammary analog secretory carcinoma of salivary gland in a 5 year old: Case report
Matthew Keisling, Michael Bianchi, Judy Mae Pascasio
International Journal of Pediatric Otorhinolaryngology Extra.2014; 9(4): 163. CrossRef - Fine-Needle Aspiration Cytology of Mammary Analog Secretory Carcinoma Masquerading as Low-Grade Mucoepidermoid Carcinoma: Case Report with a Review of the Literature
Jaya Bajaj, Cecilia Gimenez, Farah Slim, Mohamed Aziz, Kasturi Das
Acta Cytologica.2014; 58(5): 501. CrossRef
- Rare Tumors of Oral Cavity: A Case Report and Literature Review on Secretory Carcinoma of Minor Salivary Glands
- Rosai-Dorfman Disease: Report of a Case Associated with IgG4-Related Sclerotic Lesions
- Bong-Hee Park, Da Hye Son, Myung-Hwan Kim, Tae Sun Shim, Hee Jin Lee, Jooryung Huh
- Korean J Pathol. 2012;46(6):583-586. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.583
- 8,988 View
- 53 Download
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF We describe a rare case of sinus histiocytosis with massive lymphadenopathy (Rosai-Dorfman disease) associated with a six-year history of autoimmune pancreatitis, which was controlled by steroid treatment. The patient presented with multiple, cervical and thoracic lymphadenopathy and abnormal, nodular opacities in the lung. Histologically, Rosai-Dorfman disease with numerous IgG4-positive cells was identified in a subcutaneous lymph node in the patient's left forearm. The patient recovered uneventfully with steroid treatment.
-
Citations
Citations to this article as recorded by- Lung Involvement in Destombes-Rosai-Dorfman Disease
Quentin Moyon, Samia Boussouar, Philippe Maksud, Jean-François Emile, Frédéric Charlotte, Nathalie Aladjidi, Grégoire Prévot, Jean Donadieu, Zahir Amoura, Philippe Grenier, Julien Haroche, Fleur Cohen Aubart
Chest.2020; 157(2): 323. CrossRef - Rosai-Dorfman Disease: Rare Pulmonary Involvement Mimicking Pulmonary Langerhans Cell Histiocytosis and Review of the Literature
Rashid AL Umairi, Danielle Blunt, Wedad Hana, Matthew Cheung, Anastasia Oikonomou
Case Reports in Radiology.2018; 2018: 1. CrossRef - IgG4‐related skin disease may have distinct systemic manifestations: a systematic review
Adam E. Bennett, Neil A. Fenske, Paul Rodriguez‐Waitkus, Jane L. Messina
International Journal of Dermatology.2016; 55(11): 1184. CrossRef - Nosology and Pathology of Langerhans Cell Histiocytosis
Jennifer Picarsic, Ronald Jaffe
Hematology/Oncology Clinics of North America.2015; 29(5): 799. CrossRef - A subset of Rosai–Dorfman disease cases show increased IgG4‐positive plasma cells: another red herring or a true association with IgG4‐related disease?
Madhu P Menon, Moses O Evbuomwan, Juan Rosai, Elaine S Jaffe, Stefania Pittaluga
Histopathology.2014; 64(3): 455. CrossRef - Pulmonary IgG4+ Rosai-Dorfman disease
Karim El-Kersh, Rafael L Perez, Juan Guardiola
BMJ Case Reports.2013; 2013: bcr2012008324. CrossRef
- Lung Involvement in Destombes-Rosai-Dorfman Disease
- Expression of SIRT1 and DBC1 in Gastric Adenocarcinoma
- Youngran Kang, Woon Yong Jung, Hyunjoo Lee, Eunjung Lee, Aeree Kim, Baek-hui Kim
- Korean J Pathol. 2012;46(6):523-531. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.523
- 10,616 View
- 50 Download
- 31 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Sirtuin 1 (SIRT1) and deleted in breast cancer 1 (DBC1) are known as tumor suppressor or promoter genes. This may be due to their diverse functions and interaction with other proteins. Gastric adenocarcinoma is one of the most common malignancies, but little is known about its carcinogenesis. Therefore, we investigated the association of immunohistochemical expression of SIRT1, DBC1, p53, and β-catenin and their variable clinicopathological characteristics.
Methods We obtained samples from 452 patients who underwent gastrectomy. Tissue microarray blocks were constructed and immonohistochemical staining was performed.
Results Expression of DBC1 and SIRT1 was associated with lower histologic grade, intestinal type of Lauren classification, and lower pT (p<0.001) and pN stage (DBC1, p=0.002; SIRT1, p<0.001). Association between absence of lymphatic invasion, and SIRT1 (p=0.001) and DBC1 (p=0.004) was observed. Cytoplasmic β-catenin expression was associated with lower histologic grade, pT, pN, tumor-node-metastasis (TNM) stage, DBC1 (p<0.001), and SIRT1 (p=0.001). Expression of SIRT1 and DBC1 was not associated with p53 (p=0.063 and p=0.060). DBC1 was an independent good prognostic factor in multivariate analysis (p=0.012).
Conclusions SIRC1 and DBC1 can be considered to be good prognostic factors in gastric adenocarcinoma.
-
Citations
Citations to this article as recorded by- Regulatory role of DBC1 in inflammation and autoimmune diseases
Jinzhi Wu, Fan Yang, Guanhua Xu, Xinlei Ma, Jin Lin, Weiqian Chen
Rheumatology & Autoimmunity.2025; 5(1): 15. CrossRef - Prognostic and clinicopathological value of dbc1 expression in human cancers: a systematic review and meta-analysis
Haojia Wang, Xinhong Cheng, Bruce Xianzhuo Zhang, Yong Wang, Shuo Gao, Fanghui Ding, Xiaojing Song, Dandan Li, Haixu Ni, Yang Luo, Xun Li
Frontiers in Oncology.2025;[Epub] CrossRef - Mechanistic insights into the dual role of CCAR2/DBC1 in cancer
Hwa Jin Kim, Sue Jin Moon, Jeong Hoon Kim
Experimental & Molecular Medicine.2023; 55(8): 1691. CrossRef - Sirtuins (SIRTs) As a Novel Target in Gastric Cancer
Agata Poniewierska-Baran, Paulina Warias, Katarzyna Zgutka
International Journal of Molecular Sciences.2022; 23(23): 15119. CrossRef - Histone Deacetylase Functions in Gastric Cancer: Therapeutic Target?
Amandine Badie, Christian Gaiddon, Georg Mellitzer
Cancers.2022; 14(21): 5472. CrossRef - Advances on the role of the deleted in breast cancer (DBC1) in cancer and autoimmune diseases
Qiannan Fang, Joseph A Bellanti, Song Guo Zheng
Journal of Leukocyte Biology.2021; 109(2): 449. CrossRef - miR-1301-3p Promotes Cell Proliferation and Facilitates Cell Cycle Progression via Targeting SIRT1 in Gastric Cancer
Dakui Luo, Hao Fan, Xiang Ma, Chao Yang, Yu He, Yugang Ge, Mingkun Jiang, Zekuan Xu, Li Yang
Frontiers in Oncology.2021;[Epub] CrossRef - CCAR1 and CCAR2 as gene chameleons with antagonistic duality: Preclinical, human translational, and mechanistic basis
Gavin S. Johnson, Praveen Rajendran, Roderick H. Dashwood
Cancer Science.2020; 111(10): 3416. CrossRef - Role of Histone Acetylation in Gastric Cancer: Implications of Dietetic Compounds and Clinical Perspectives
Danielle Q Calcagno, Fernanda Wisnieski, Elizangela R da Silva Mota, Stefanie B Maia de Sousa, Jéssica M Costa da Silva, Mariana F Leal, Carolina O Gigek, Leonardo C Santos, Lucas T Rasmussen, Paulo P Assumpção, Rommel R Burbano, Marília AC Smith
Epigenomics.2019; 11(3): 349. CrossRef - Survival and Clinicopathological Significance of SIRT1 Expression in Cancers: A Meta-Analysis
Min Sun, Mengyu Du, Wenhua Zhang, Sisi Xiong, Xingrui Gong, Peijie Lei, Jin Zha, Hongrui Zhu, Heng Li, Dong Huang, Xinsheng Gu
Frontiers in Endocrinology.2019;[Epub] CrossRef - Cell cycle and apoptosis regulator 2 at the interface between DNA damage response and cell physiology
Martina Magni, Giacomo Buscemi, Laura Zannini
Mutation Research/Reviews in Mutation Research.2018; 776: 1. CrossRef - NANOGP8 expression regulates gastric cancer cell progression by transactivating DBC1 in gastric cancer MKN‑45 cells
Li Li, Ru Feng, Sujuan Fei, Jiang Cao, Qinqin Zhu, Guozhong Ji, Jianwei Zhou
Oncology Letters.2018;[Epub] CrossRef - Overexpression of DBC1, correlated with poor prognosis, is a potential therapeutic target for hepatocellular carcinoma
Changcan Li, Jianhua Liao, Shaohan Wu, Junwei Fan, Zhihai Peng, Zhaowen Wang
Biochemical and Biophysical Research Communications.2017; 494(3-4): 511. CrossRef - Association of sirtuins with clinicopathological parameters and overall survival in gastric cancer
Xiaobing Shen, Pengfei Li, Yuchao Xu, Xiaowei Chen, Haixiang Sun, Ying Zhao, Mengqi Liu, Wenwen Zhang
Oncotarget.2017; 8(43): 74359. CrossRef - Co-ordinated overexpression of SIRT1 and STAT3 is associated with poor survival outcome in gastric cancer patients
Shu Zhang, Shuling Huang, Chao Deng, Yu Cao, Jun Yang, Guangxia Chen, Bin Zhang, Chaoqin Duan, Jiong Shi, Bo Kong, Helmut Friess, Nanyi Zhao, Chen Huang, Xiaoli Huang, Lei Wang, Xiaoping Zou
Oncotarget.2017; 8(12): 18848. CrossRef - The prognostic role of Sirt1 expression in solid malignancies: a meta-analysis
Changwen Wang, Wen Yang, Fang Dong, Yawen Guo, Jie Tan, Shengnan Ruan, Tao Huang
Oncotarget.2017; 8(39): 66343. CrossRef - SIRT1 induces tumor invasion by targeting epithelial mesenchymal transition-related pathway and is a prognostic marker in triple negative breast cancer
Min-Sun Jin, Chang Lim Hyun, In Ae Park, Ji Young Kim, Yul Ri Chung, Seock-Ah Im, Kyung-Hun Lee, Hyeong-Gon Moon, Han Suk Ryu
Tumor Biology.2016; 37(4): 4743. CrossRef - Prognostic and clinical value of Sirt1 expression in gastric cancer: A systematic meta-analysis
Bin Jiang, Jin-huang Chen, Wen-zheng Yuan, Jin-tong Ji, Zheng-yi Liu, Liang Wu, Qiang Tang, Xiao-gang Shu
Journal of Huazhong University of Science and Technology [Medical Sciences].2016; 36(2): 278. CrossRef - Significance of silent mating type information regulation 2 homolog 1 and claudin 4 expression in gastric carcinoma and precursor lesions
Nashwa M. Emara, Ranih Z. Amer, Khaled M. Elsadek Attia, Heba M. Rashad, Adel Z. Elseady, Abd El-Latif M. Elbalshy
Egyptian Journal of Pathology.2016; 36(2): 158. CrossRef - Distinctive role of SIRT1 expression on tumor invasion and metastasis in breast cancer by molecular subtype
Yul Ri Chung, Hyojin Kim, Soo Young Park, In Ae Park, Ja June Jang, Ji-Young Choe, Yoon Yang Jung, Seock-Ah Im, Hyeong-Gon Moon, Kyung-Hun Lee, Koung Jin Suh, Tae-Yong Kim, Dong-Young Noh, Wonshik Han, Han Suk Ryu
Human Pathology.2015; 46(7): 1027. CrossRef - SIRT1 is a regulator of autophagy: Implications in gastric cancer progression and treatment
Guanglin Qiu, Xuqi Li, Xiangming Che, Chao Wei, Shicai He, Jing Lu, Zongliang Jia, Ke Pang, Lin Fan
FEBS Letters.2015; 589(16): 2034. CrossRef - DBC1 Functions as a Tumor Suppressor by Regulating p53 Stability
Bo Qin, Katherine Minter-Dykhouse, Jia Yu, Jun Zhang, Tongzheng Liu, Haoxing Zhang, SeungBaek Lee, JungJin Kim, Liewei Wang, Zhenkun Lou
Cell Reports.2015; 10(8): 1324. CrossRef - DBC1 promotes anoikis resistance of gastric cancer cells by regulating NF-κB activity
YONGWEI HUAN, DEPING WU, DAYONG ZHOU, BO SUN, GUOXIN LI
Oncology Reports.2015; 34(2): 843. CrossRef - Resveratrol relieves ischemia‑induced oxidative stress in the hippocampus by activating SIRT1
Zhuangzhi Meng, Jianguo Li, Honglin Zhao, Haiying Liu, Guowei Zhang, Lingzhan Wang, He Hu, Di Li, Mingjing Liu, Fulong Bi, Xiaoping Wang, Geng Tian, Qiang Liu, Batu Buren
Experimental and Therapeutic Medicine.2015;[Epub] CrossRef - CCAR2 deficiency augments genotoxic stress-induced apoptosis in the presence of melatonin in non-small cell lung cancer cells
Wootae Kim, Joo-Won Jeong, Ja-Eun Kim
Tumor Biology.2014; 35(11): 10919. CrossRef - Radioprotective and Antioxidant Effect of Resveratrol in Hippocampus by Activating Sirt1
Jianguo Li, Li Feng, Yonghua Xing, Yan Wang, Liqing Du, Chang Xu, Jia Cao, Qin Wang, Saijun Fan, Qiang Liu, Feiyue Fan
International Journal of Molecular Sciences.2014; 15(4): 5928. CrossRef - SIRT1 expression is associated with a poor prognosis, whereas DBC1 is associated with favorable outcomes in gastric cancer
Akira Noguchi, Keiji Kikuchi, Huachuan Zheng, Hiroyuki Takahashi, Yohei Miyagi, Ichiro Aoki, Yasuo Takano
Cancer Medicine.2014; 3(6): 1553. CrossRef - Sirtuins and Cancer: New Insights and Cell Signaling
Marcos Vinícius Macedo de Oliveira, João Marcus Oliveira Andrade, Alanna Fernandes Paraíso, Sérgio Henrique Sousa Santos
Cancer Investigation.2013; 31(10): 645. CrossRef - Deleted in breast cancer-1 (DBC-1) in the interface between metabolism, aging and cancer
Eduardo Nunes Chini, Claudia C. S. Chini, Veronica Nin, Carlos Escande
Bioscience Reports.2013;[Epub] CrossRef - SIRT1 Expression Is Associated with Good Prognosis in Colorectal Cancer
Wonkyung Jung, Kwang Dae Hong, Woon Yong Jung, Eunjung Lee, Bong Kyung Shin, Han Kyeom Kim, Aeree Kim, Baek-hui Kim
Korean Journal of Pathology.2013; 47(4): 332. CrossRef - Clinicopathological significance of SIRT1 and p300/CBP expression in gastroesophageal junction (GEJ) cancer and the correlation with E-cadherin and MLH1
Li-Hua Zhang, Qin Huang, Xiang-Shan Fan, Hong-Yan Wu, Jun Yang, An-Ning Feng
Pathology - Research and Practice.2013; 209(10): 611. CrossRef
- Regulatory role of DBC1 in inflammation and autoimmune diseases
- Expression of c-Met Is Different along the Location and Associated with Lymph Node Metastasis of Head and Neck Carcinoma
- Ji-Young Choe, Ji Yun Yun, Soo-Jeong Nam, Ji Eun Kim
- Korean J Pathol. 2012;46(6):515-522. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.515
- 9,428 View
- 52 Download
- 19 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Activation of the c-Met pathway is involved in cancer progression and the prognosis. We aimed to identify any association of c-Met protein expression with a number of clinicopathologic variables including infection of human papillomavirus and Epstein-Barr virus (EBV) in head and neck carcinomas (HNCa).
Methods Eighty-two cases were enrolled in this study. Expression of c-Met and p16 was investigated immunohistochemically. EBV was detected by
in situ hybridization and amplification of thec-Met gene by fluorescencein situ hybridization.Results The c-Met protein was expressed in 41.5% (34/82), and gene amplification was found in 1.4% (1/71). High expression of c-Met was associated with the primary location of the tumor; the hypopharynx showed the highest expression, followed by the oral cavity, larynx, and nasal cavity. Squamous cell carcinoma expressed c-Met more frequently than undifferentiated carcinoma. Also, p16 immunoreactivity or EBV infection was associated with the tumor location and well-differentiated histologic type, but were not linked to c-Met expression. The patients with positive c-Met expression showed frequent lymph node metastasis.
Conclusions Activation of the c-Met pathway might be involved in a subset of HNCa. Cases showing positive c-Met expression should be carefully monitored because of the high probability of lymph node metastasis.
-
Citations
Citations to this article as recorded by- Case Report: A rare case of MET-amplified gastric cancer with systemic metastasis: remarkable efficacy of crizotinib and the role of precision medicine
Yan Shen, Yaxin Xu, Jing Sun
Frontiers in Oncology.2025;[Epub] CrossRef - c-MET pathway in human malignancies and its targeting by natural compounds for cancer therapy
Chakrabhavi Dhananjaya Mohan, Muthu K Shanmugam, Siddegowda Gopalapura Shivanne Gowda, Arunachalam Chinnathambi, Kanchugarakoppal S. Rangappa, Gautam Sethi
Phytomedicine.2024; 128: 155379. CrossRef - Nadir paranazal sinüs kanserlerinde yeni tanımlanan reseptör tirozin kinaz mutasyonları ve potansiyel fonksiyonel etkileri
Bakiye GÖKER BAGCA, Sercan GÖDE, Göksel TURHAL, Neslihan Pınar ÖZATEŞ, Ali VERAL, Cumhur GÜNDÜZ, Çığır Biray AVCI
Ege Tıp Dergisi.2023; 62(1): 139. CrossRef - The Emerging Role of c-Met in Carcinogenesis and Clinical Implications as a Possible Therapeutic Target
Antonio Faiella, Ferdinando Riccardi, Giacomo Cartenì, Martina Chiurazzi, Livia Onofrio, Rengyun Liu
Journal of Oncology.2022; 2022: 1. CrossRef - NK4 Regulates Laryngeal Squamous Cell Carcinoma Cell Properties and Inhibits Tumorigenicity by Modulating the DKK1/Wnt/β-Catenin Axis
Shoukai Zhang, Hulai Wei, Xiaoqin Ha, Yueyu Zhang, Yufen Guo
Frontiers in Oncology.2021;[Epub] CrossRef - Epstein-Barr Virus-Associated Carcinoma of the Larynx: A Systematic Review with Meta-Analysis
Marcos Antonio Pereira de Lima, Álife Diêgo Lima Silva, Antônio Carlos Silva do Nascimento Filho, Thiago Lima Cordeiro, João Pedro de Souza Bezerra, Maria Aline Barroso Rocha, Sally de França Lacerda Pinheiro, Roberto Flávio Fontenelle Pinheiro Junior, Ma
Pathogens.2021; 10(11): 1429. CrossRef - The roles of PTEN, cMET, and p16 in resistance to cetuximab in head and neck squamous cell carcinoma
Alexandre A. B. A. da Costa, Felipe D’Almeida Costa, Daniel Vilarim Araújo, Marcos Pedro Guedes Camandaroba, Victor Hugo Fonseca de Jesus, Audrey Oliveira, Ana Caroline Fonseca Alves, Carlos Stecca, Larissa Machado, Andrea Cruz Feraz de Oliveira, Thiago B
Medical Oncology.2019;[Epub] CrossRef - Role of c‐Met expression on prognosis of head and neck cancer: A literature review and meta‐analysis
Lei Li, Zhijun Sun, Xin Huang, Xiao Li, Lihua Sun, Lei Zhang, Xiaodan Zhang, Longwei Ye, Jie Yuan, Limin Mao, Guolin Li
Head & Neck.2019; 41(6): 1999. CrossRef - MET Genomic Alterations in Head and Neck Squamous Cell Carcinoma (HNSCC): Rapid Response to Crizotinib in a Patient with HNSCC with a Novel MET R1004G Mutation
Lisa Pei Chu, Debra Franck, Christine A. Parachoniak, Jeffrey P. Gregg, Michael G. Moore, D. Gregory Farwell, Shyam Rao, Andreas M. Heilmann, Rachel L. Erlich, Jeffrey S. Ross, Vincent A. Miller, Siraj Ali, Jonathan W. Riess
The Oncologist.2019; 24(10): 1305. CrossRef - Understanding c-MET signalling in squamous cell carcinoma of the head & neck
P. Szturz, E. Raymond, C. Abitbol, S. Albert, A. de Gramont, S. Faivre
Critical Reviews in Oncology/Hematology.2017; 111: 39. CrossRef - Prognostic value of c-MET in head and neck cancer: A systematic review and meta-analysis of aggregate data
Petr Szturz, Marie Budíková, Jan B. Vermorken, Ivana Horová, Břetislav Gál, Eric Raymond, Armand de Gramont, Sandrine Faivre
Oral Oncology.2017; 74: 68. CrossRef - Activated HGF-c-Met Axis in Head and Neck Cancer
Levi Arnold, Jonathan Enders, Sufi Thomas
Cancers.2017; 9(12): 169. CrossRef - Clinicopathological impacts of high c-Met expression in head and neck squamous cell carcinoma: a meta-analysis and review
Jung Han Kim, Bum Jun Kim, Hyeong Su Kim
Oncotarget.2017; 8(68): 113120. CrossRef - High expression of c‑Met and EGFR is associated with poor survival of patients with glottic laryngeal squamous cell carcinoma
Mei Jiang, Hui Zhang, He Xiao, Zhimin Zhang, Dan Que, Jia Luo, Jian Li, Bijing Mao, Yuanyuan Chen, Meilin Lan, Ge Wang, Hualiang Xiao
Oncology Letters.2017;[Epub] CrossRef - Profiling of cMET and HER Family Receptor Expression in Pancreatic Ductal Adenocarcinomas and Corresponding Lymph Node Metastasis to Assess Relevant Pathways for Targeted Therapies
Alexander Muckenhuber, Galina Babitzki, Marlene Thomas, Gabriele Hölzlwimmer, Magdalena Zajac, Moritz Jesinghaus, Frank Bergmann, Jens Werner, Albrecht Stenzinger, Wilko Weichert
Pancreas.2016; 45(8): 1167. CrossRef - Absent and abundant MET immunoreactivity is associated with poor prognosis of patients with oral and oropharyngeal squamous cell carcinoma
Maria J. De Herdt, Stefan M. Willems, Berdine van der Steen, Rob Noorlag, Esther I. Verhoef, Geert J.L.H. van Leenders, Robert J.J. van Es, Senada Koljenović, Robert J. Baatenburg de Jong, Leendert H.J. Looijenga
Oncotarget.2016; 7(11): 13167. CrossRef - Biological, diagnostic and therapeutic relevance of the MET receptor signaling in head and neck cancer
Lluís Nisa, Daniel Matthias Aebersold, Roland Giger, Yitzhak Zimmer, Michaela Medová
Pharmacology & Therapeutics.2014; 143(3): 337. CrossRef - Frequent hepatocyte growth factor overexpression and low frequency of c-Met gene amplification in human papillomavirus–negative tonsillar squamous cell carcinoma and their prognostic significances
Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Hyung Sik Shin, Ji Hyun Kwon, Dong Jin Lee, Jin Hwan Kim, Seong Jin Cho, Eun Sook Nam
Human Pathology.2014; 45(7): 1327. CrossRef - Distinct c-Met activation mechanisms induce cell rounding or invasion through pathways involving integrins, RhoA and HIP1
Anja Mai, Ghaffar Muharram, Rachel Barrow-McGee, Habib Baghirov, Juha Rantala, Stéphanie Kermorgant, Johanna Ivaska
Journal of Cell Science.2014; 127(9): 1938. CrossRef
- Case Report: A rare case of MET-amplified gastric cancer with systemic metastasis: remarkable efficacy of crizotinib and the role of precision medicine
- Primary Endometrial Squamous Cell Carcinoma: A Case Report and Review of Relevant Literature on Korean Women
- Sung Jong Lee, Hyun Joo Choi
- Korean J Pathol. 2012;46(4):395-398. Published online August 23, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.4.395
- 9,734 View
- 85 Download
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF Primary endometrial squamous cell carcinoma (PESCC) is an extremely rare tumor with unclear pathogenesis. A 54-year-old postmenopausal woman presented with a 6-month history of vaginal bleeding. The patient was provisionally diagnosed with uterine submucosal leiomyoma. This was followed by total hysterectomy with a bilateral salpingo-oophorectomy under the laparoscopic guidance. Histopathologically, the tumor was PESCC which was accompanied by a lack of the tumor in the uterine cervix. The tumor showed positive immunoreactivity for p16INK4a. But there was no evidence of human papillomavirus (HPV) on
in situ hybridization and HPV DNA chip analysis. We also present a review of the relevant literature on Korean women.-
Citations
Citations to this article as recorded by- Primary squamous cell carcinoma of the uterine wall associated with adenomyosis: A rare case report and literature review
Yang Li, Lanlan Xuan, Qiucheng Wang
International Journal of Gynecology & Obstetrics.2026; 172(1): 87. CrossRef - Primary endometrial squamous cell carcinoma (PESCC): Review of the literature and case report
Kuang-Han Liu, Chia-Chin Tsai, Krystal Baysan Lin, Pei-Shen Huang
Taiwanese Journal of Obstetrics and Gynecology.2025; 64(1): 159. CrossRef - Primary squamous cell carcinoma of the endometrium: A case report
Shuhui Cui, Zhe Dong
Medicine.2025; 104(46): e45920. CrossRef - p16 Block Type Overexpression, p53 Wild Type Reactivity, and Cervical Involvement do not Always Exclude the Diagnosis of Primary Endometrial Squamous Cell Carcinoma (PESCC)
Daniela Fanni, Clara Gerosa, Michele Peiretti, Valerio Mais, Elena Massa, Stefano Angioni, Gavino Faa
International Journal of Gynecological Pathology.2024; 43(2): 200. CrossRef - Pathogenetic characteristics of endometrioid adenocarcinoma of uterus at present stage
T. I. Moiseenko, S. V. Shatalova, E. M. Nepomnyashchaya, V. A. Bandovkina, M. L. Adamyan
Medical alphabet.2024; (36): 35. CrossRef - Case report: Clinicopathological characteristic of two cases of primary endometrial squamous cell carcinoma and review of the literature
Hui-Bin Zhang, Li-Hua Lin, Qiu-Ping Lin, Yuan-Qing Lin, Dan Luo, Shu-Xia Xu
Frontiers in Oncology.2024;[Epub] CrossRef - Treatment of primary squamous cell carcinoma of the endometrium and review of previous literature: A case report
Liyun Song, Qi Wu, Suning Bai, Ren Xu, Xiaona Wang, Yanyan Yang
Medicine.2023; 102(17): e33667. CrossRef -
Prevalence of
human papilloma virus
and
Chlamydia trachomatis
in endometrial and cervical carcinoma: a comparative study in North Indian women
Heena Gautam, Sumita Mehta, Nidhi Nayar, Neha Kumar, Syed Akhtar Husain, Mausumi Bharadwaj
Systems Biology in Reproductive Medicine.2023; 69(6): 399. CrossRef - PAX8 Positivity, Abnormal p53 Expression, and p16 Negativity in a Primary Endometrial Squamous Cell Carcinoma: A Case Report and Review of the Literature
Daniela Fanni, Michele Peiretti, Valerio Mais, Elena Massa, Clara Gerosa, Francesca Ledda, Maria Luisa Fais, Gavino Faa, Stefano Angioni
International Journal of Gynecological Pathology.2022; 41(4): 431. CrossRef - Molecular Analysis of HPV-independent Primary Endometrial Squamous Cell Carcinoma Reveals TP53 and CDKN2A Comutations
Mark R. Hopkins, Doreen N. Palsgrove, Brigitte M. Ronnett, Russell Vang, Jeffrey Lin, Tricia A. Murdock
American Journal of Surgical Pathology.2022; 46(12): 1611. CrossRef - Primary squamous cell carcinoma of the endometrium—Case report with cytological characteristics in direct and indirect endometrial samples
Sanda Rajhvajn, Ana Barišić, Lada Škopljanac‐Mačina, Danijela Jurič, Vesna Mahovlić
Cytopathology.2021; 32(6): 823. CrossRef - Primary squamous cell carcinoma of the endometrium associated with human papilloma virus in a young woman: a case report
Tchin Darré, Abdoul-Samadou Aboubakari, Lantam Sonhaye, Baguilane Douaguibe, Akila Bassowa, Gado Napo-Koura
Journal of Medical Case Reports.2019;[Epub] CrossRef - Primary squamous cell carcinoma of the endometrium in a woman of perimenopausal age
Chao Zhang, Hongyan Zhang, Linqing Yang, Yunfei Wang, Xiaoyu Li, Jinfeng Guo, Jing Xu
Medicine.2018; 97(48): e13418. CrossRef - S100P is Overexpressed in Squamous Cell and Adenosquamous Carcinoma Subtypes of Endometrial Cancer and Promotes Cancer Cell Proliferation and Invasion
Hongfei Jiang, Hang Hu, Fan Lin, Yoon Pin Lim, Yunfen Hua, Xiaomei Tong, Songying Zhang
Cancer Investigation.2016; 34(10): 477. CrossRef - Überraschung in der Abradatdiagnostik
U. Kellner, A. Kellner, U. Cirkel
Der Pathologe.2015; 36(3): 317. CrossRef
- Primary squamous cell carcinoma of the uterine wall associated with adenomyosis: A rare case report and literature review
- Expression of Human Papillomavirus-Related Proteins and Its Clinical Implication in Tonsillar Squamous Cell Carcinoma
- Joon Seon Song, Min-Sik Kim, Joon Wook Park, Youn Soo Lee, Chang Suk Kang
- Korean J Pathol. 2012;46(2):177-186. Published online April 25, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.2.177
- 11,411 View
- 42 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Human papillomavirus (HPV) is known to cause of oropharyngeal squamous cell carcinoma (SqCC). HPV positive SqCCs overexpress p16 and are associated with better survival. Several markers of cell cycles and apoptosis have been reported as a prognostic value. We examined the prognostic value of HPV status, p16, cyclin D1, and Bcl-2 in patients with tonsillar SqCC.
Methods Tissue microarrays were constructed in 56 cases of tonsillar SqCC for which we performed an immunohistochemistry and an
in situ hybridization (ISH) of the HPV.Results Of the 56 cases, 31 (55.3%) were positive for p16 and 20 (35.7%) were positive for HPV ISH. The expressions of p16, cyclin D1, and Bcl-2 were not correlated with the clinicopathologic variables including smoking status, differentiation and pT- and pN-stages. The HPV ISH positive group showed a better overall survival than the HPV negative group (p=0.04), and the p16 positive group showed a better disease free survival (DFS) than the negative group (p=0.016). Cox regression analysis showed that only p16 positivity was an independent prognostic factor for DFS (p=0.03; hazard ratio, 10.1).
Conclusions Our results indicate that both p16 expression and HPV status are useful indicators for risk stratification in patients with tonsillar SqCC.
-
Citations
Citations to this article as recorded by- Positive Rate of Human Papillomavirus and Its Trend in Head and Neck Cancer in South Korea
Hyun Woong Jun, Yong Bae Ji, Chang Myeon Song, Jae Kyung Myung, Hae Jin Park, Kyung Tae
Frontiers in Surgery.2022;[Epub] CrossRef - Negative Prognostic Implication of TERT Promoter Mutations in Human Papillomavirus–Negative Tonsillar Squamous Cell Carcinoma Under the New 8th AJCC Staging System
Hyunchul Kim, Mi Jung Kwon, Bumjung Park, Hyo Geun Choi, Eun Sook Nam, Seong Jin Cho, Kyueng-Whan Min, Eun Soo Kim, Hee Sung Hwang, Mineui Hong, Taeryool Koo, Hyo Jung Kim
Indian Journal of Surgical Oncology.2021; 12(S1): 134. CrossRef - In situ hybridization for high risk HPV E6/E7 mRNA in oropharyngeal squamous cell carcinoma
Krish Suresh, Parth V. Shah, Sydney Coates, Borislav A. Alexiev, Sandeep Samant
American Journal of Otolaryngology.2021; 42(1): 102782. CrossRef - Prevalence of high-risk human papillomavirus and its genotype distribution in head and neck squamous cell carcinomas
Yuil Kim, Young-Hoon Joo, Min-Sik Kim, Youn Soo Lee
Journal of Pathology and Translational Medicine.2020; 54(5): 411. CrossRef - Human Papillomavirus Testing in Head and Neck Carcinomas: Guideline From the College of American Pathologists
James S. Lewis, Beth Beadle, Justin A. Bishop, Rebecca D. Chernock, Carol Colasacco, Christina Lacchetti, Joel Todd Moncur, James W. Rocco, Mary R. Schwartz, Raja R. Seethala, Nicole E. Thomas, William H. Westra, William C. Faquin
Archives of Pathology & Laboratory Medicine.2018; 142(5): 559. CrossRef - Detection of HPV infection in head and neck cancers: Promise and pitfalls in the last ten years: A meta-analysis
Carolin G�tz, Clara Bischof, Klaus-Dietrich Wolff, Andreas Kolk
Molecular and Clinical Oncology.2018;[Epub] CrossRef - Frequent hepatocyte growth factor overexpression and low frequency of c-Met gene amplification in human papillomavirus–negative tonsillar squamous cell carcinoma and their prognostic significances
Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Hyung Sik Shin, Ji Hyun Kwon, Dong Jin Lee, Jin Hwan Kim, Seong Jin Cho, Eun Sook Nam
Human Pathology.2014; 45(7): 1327. CrossRef - Human papillomavirus‐stratified analysis of the prognostic role of miR‐21 in oral cavity and oropharyngeal squamous cell carcinoma
Yoon Ho Ko, Hye Sung Won, Der Sheng Sun, Ho Jung An, Eun Kyoung Jeon, Min Sik Kim, Han Hong Lee, Jin Hyoung Kang, Chan Kwon Jung
Pathology International.2014; 64(10): 499. CrossRef - Human Papillomavirus Prevalence and Cell Cycle Related Protein Expression in Tonsillar Squamous Cell Carcinomas of Korean Patients with Clinicopathologic Analysis
Miji Lee, Sung Bae Kim, Sang-wook Lee, Jong-Lyel Roh, Seung-Ho Choi, Soon Yuhl Nam, Sang Yoon Kim, Kyung-Ja Cho
Korean Journal of Pathology.2013; 47(2): 148. CrossRef
- Positive Rate of Human Papillomavirus and Its Trend in Head and Neck Cancer in South Korea
- Detection of Survivin and COX-2 in Thyroid Carcinoma: Anaplastic Carcinoma Shows Overexpression of Nuclear Survivin and Low COX-2 Expression
- Young A Kim, Meesoo Chang, Young Joo Park, Ji Eun Kim
- Korean J Pathol. 2012;46(1):55-60. Published online February 23, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.1.55
- 10,472 View
- 67 Download
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Overexpression of survivin, a member of the inhibitors of apoptosis protein, has been reported in various carcinomas, and its interaction with cyclooxygenase 2 (COX-2) results in accelerated tumor progression. The purpose of this study is to investigate the immunohistochemical expression of survivin and COX-2 in benign and malignant thyroid tissues and to define its association with pathologic and clinical features.
Methods We examined expression of survivin and COX-2 by immunohistochemistry in 334 benign and malignant thyroid tissues and evaluated their clinical significance.
Results Expression of survivin showed an increase along the spectrum of thyroid carcinoma progression; rarely positive in adenomatous goiter, moderately positive in papillary carcinoma, and strongly positive in anaplastic carcinoma (AC). Papillary microcarcinoma revealed the highest COX-2 positivity and AC demonstrated the lowest positivity among thyroid cancers. Node negative carcinomas showed higher COX-2 expression than node positive tumors. Survivin expression did not correlate with COX-2.
Conclusions Our findings suggest that survivin overexpression may be related to the pathogenesis of AC and can be a predictor of disease progression. COX-2 may be involved in the early phase of thyroid carcinoma.
-
Citations
Citations to this article as recorded by- Interplay between nuclear survivin and the PRC2 complex and its impact on H3K27me3-directed transcriptional repression
Adesh D. Vaidya, Alexander J. Fezovich, Sally P. Wheatley
Journal of Cell Science.2026;[Epub] CrossRef - Survivin as a diagnostic and therapeutic marker for thyroid cancer
Mohammad-Reza Mahmoudian-Sani, Arash Alghasi, Ali Saeedi-Boroujeni, Akram Jalali, Mohammad Jamshidi, Ali Khodadadi
Pathology - Research and Practice.2019; 215(4): 619. CrossRef - TFAP2B overexpression contributes to tumor growth and progression of thyroid cancer through the COX-2 signaling pathway
Xiaoyan Fu, Huayong Zhang, Zhipeng Chen, Zhongyuan Yang, Dingbo Shi, Tianrun Liu, Weichao Chen, Fan Yao, Xuan Su, Wuguo Deng, Miao Chen, Ankui Yang
Cell Death & Disease.2019;[Epub] CrossRef - Expression of nm23-H1 and COX-2 in thyroid papillary carcinoma and microcarcinoma
Marija Milkovic Perisa, Bozena Sarcevic, Koraljka Gall Troselj, Kresimir Grsic, Sanda Sitic, Sven Seiwerth
Oncology Letters.2017; 13(5): 3547. CrossRef - The Diagnostic Usefulness of HMGA2, Survivin, CEACAM6, and SFN/14-3-3 δ in Follicular Thyroid Carcinoma
Min Hye Jang, Kyeong Cheon Jung, Hye Sook Min
Journal of Pathology and Translational Medicine.2015; 49(2): 112. CrossRef - Evaluation of survivin expression and its prognostic value in papillary thyroid carcinoma
Sonja Selemetjev, Tijana Isic Dencic, Ilona Marecko, Jelena Jankovic, Ivan Paunovic, Svetlana Savin, Dubravka Cvejic
Pathology - Research and Practice.2014; 210(1): 30. CrossRef
- Interplay between nuclear survivin and the PRC2 complex and its impact on H3K27me3-directed transcriptional repression
- Fine needle aspiration cytology of so-called sclerosing hemangioma of the lung: report of two cases.
- Na Hye Myong, Chang Won Ha, Kyung Ja Cho, Ja June Jang
- J Pathol Transl Med. 1991;2(1):28-35.
- 2,049 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - So-called sclerosing hemangioma of the lung is a rare benign neoplasm which usually presents with a coin lesion detected through routine chest X-ray. We report two cases showing characteristic cytologic appearances which have been rarely reported. Both cases were young females with coin lesions in the lung. Fine needle aspiration of each case revealed unique but some different cytologic features. Case 1 showed bland-looking polygonal epithelial cells resembling bronchioloalveolar cells having predominantly papillary configurations with loosely arranged solid sheets or isolated cells. Cytoplasms were plump, cyanophilic, and finely granular, with eccentric nuclei. The nuclei were usually monotonous, round-to-ovoid, and vesicular with a small but conspicuous nucleolus. In comparison to case 1, case 2 revealed largely loose pavement-like solid sheets or clusters rather than papillary patterns in the hemorrhagic background. The size of tumor cells were a little smaller than that of case 1. Bronchiotoalveolar carcinoma and papillary adenocarcinoma of metastatic origin were considered to be one of the important differential diagnoses with these cytologic features. Histologically, both cases exhibited findings compatible with so-called sclerosing hemangioma of the lung.

 E-submission
E-submission

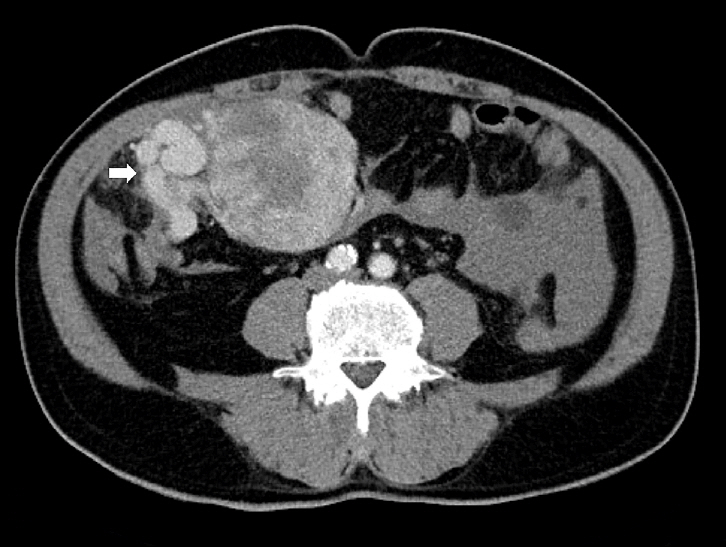
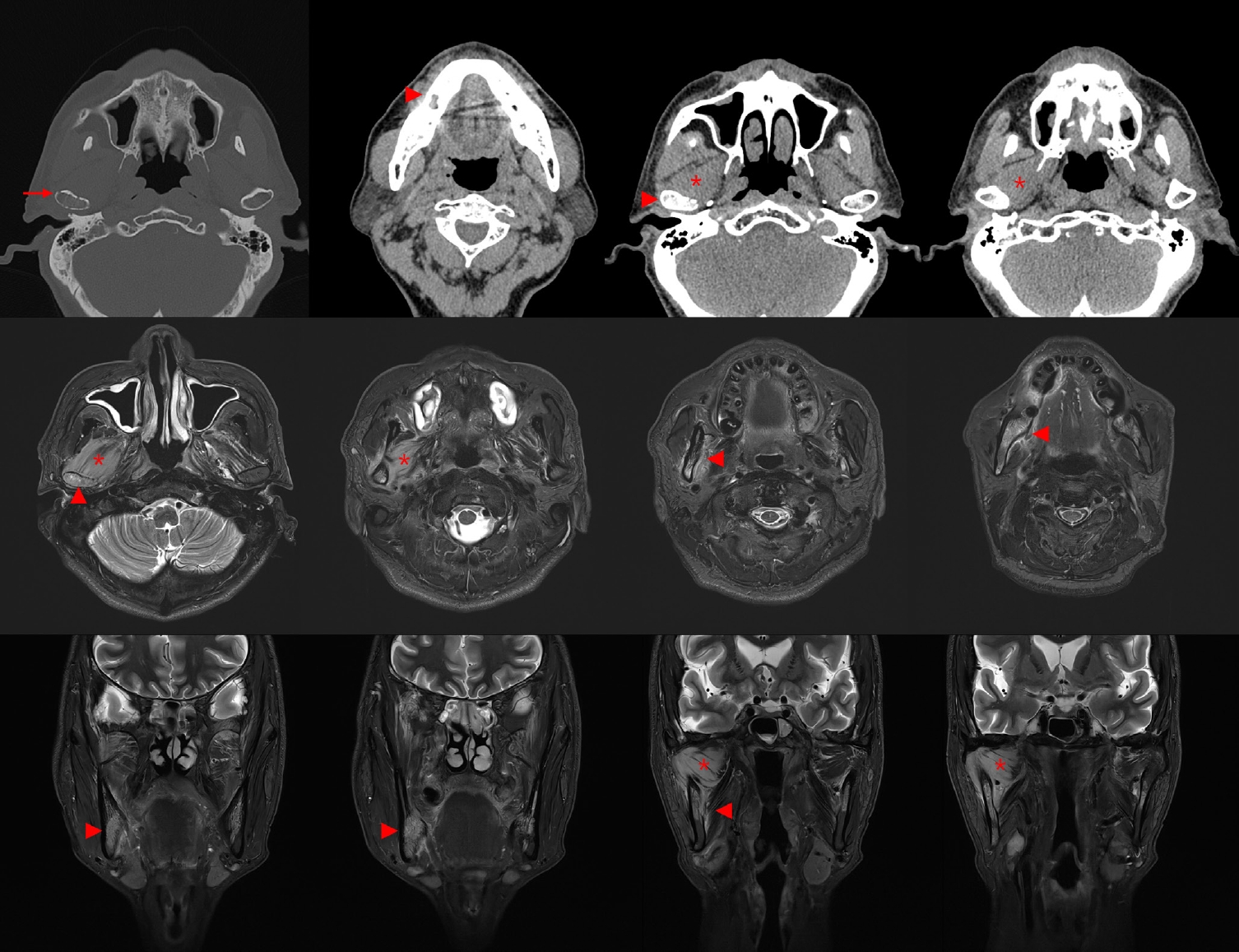
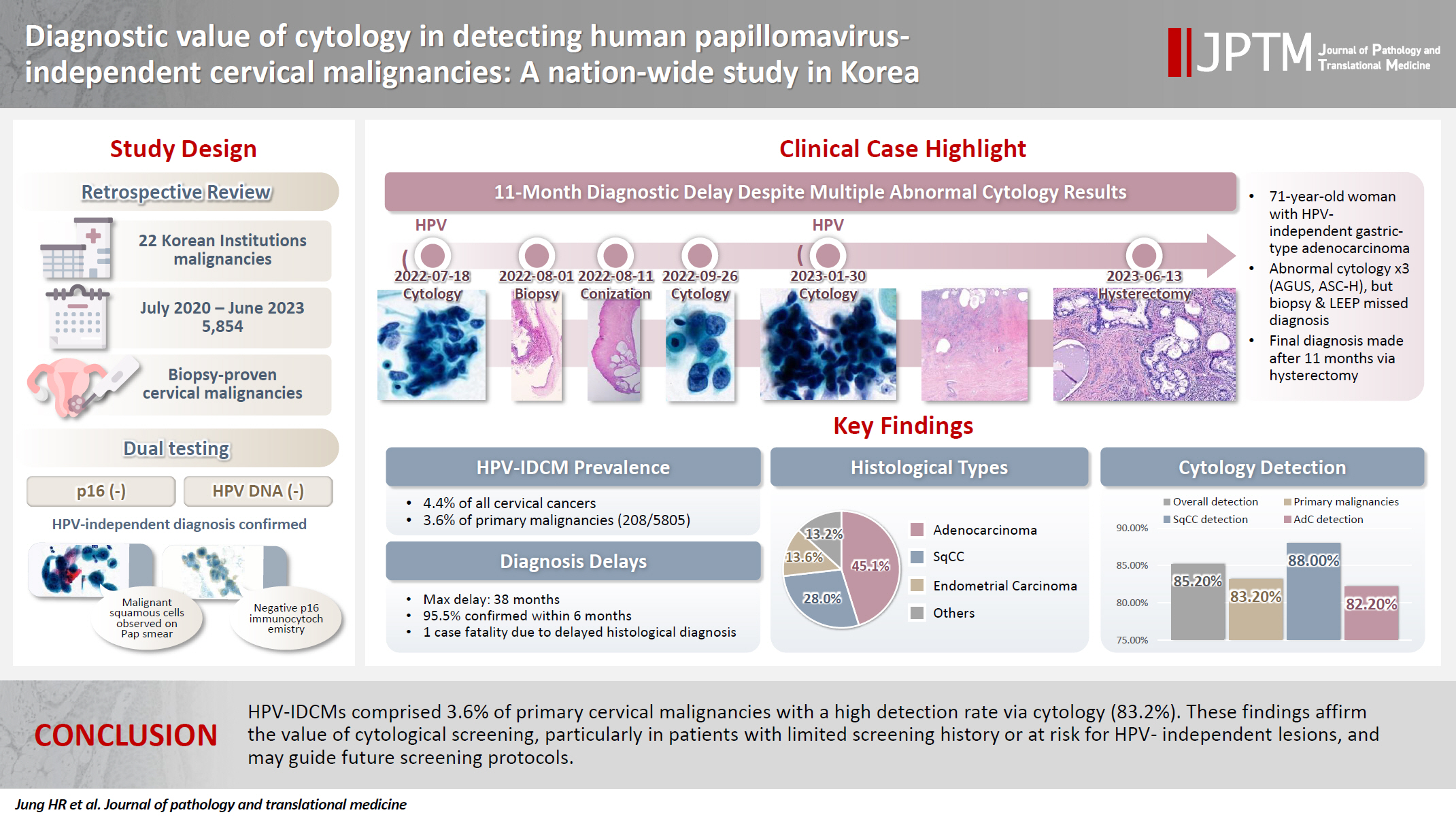
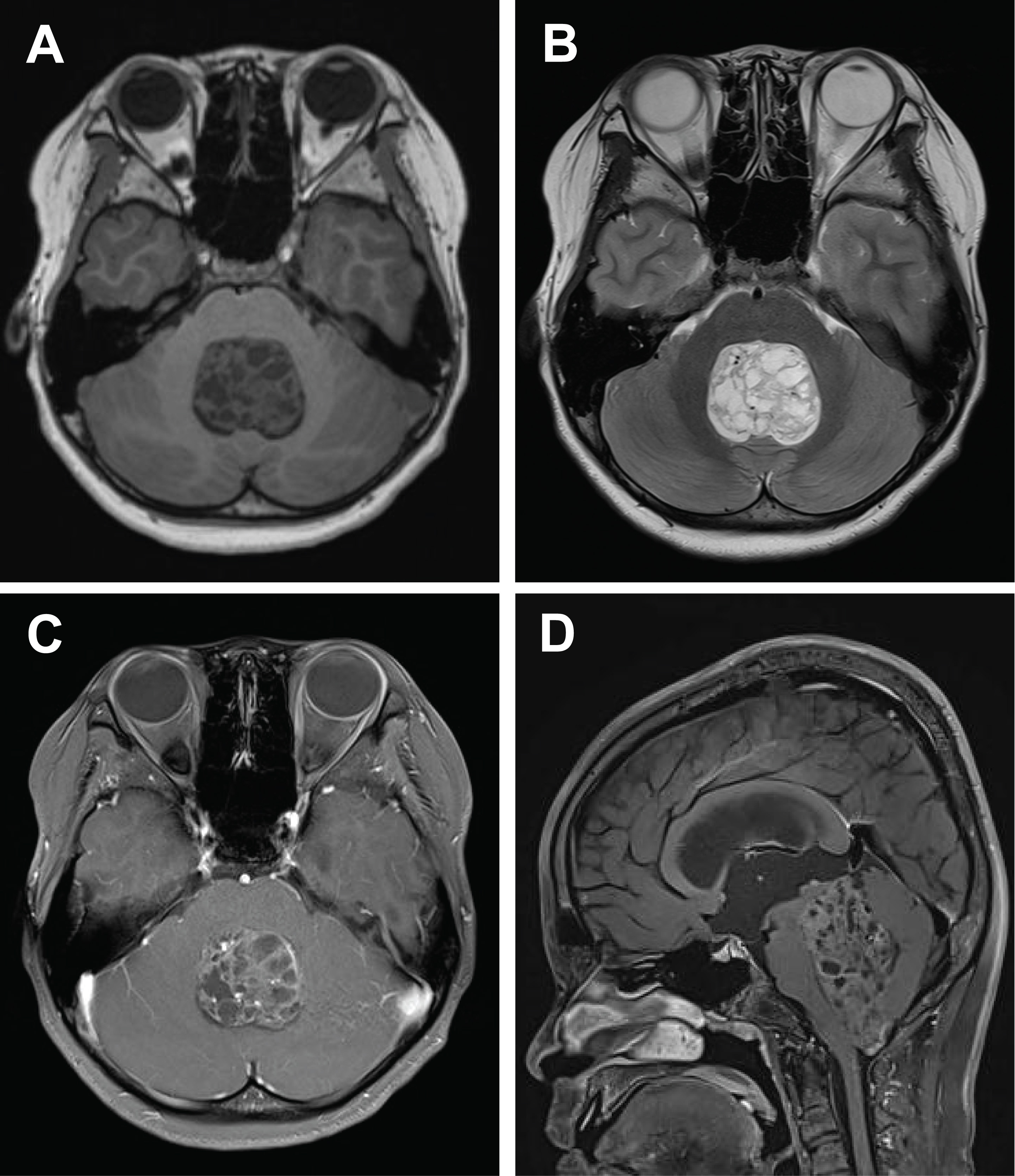
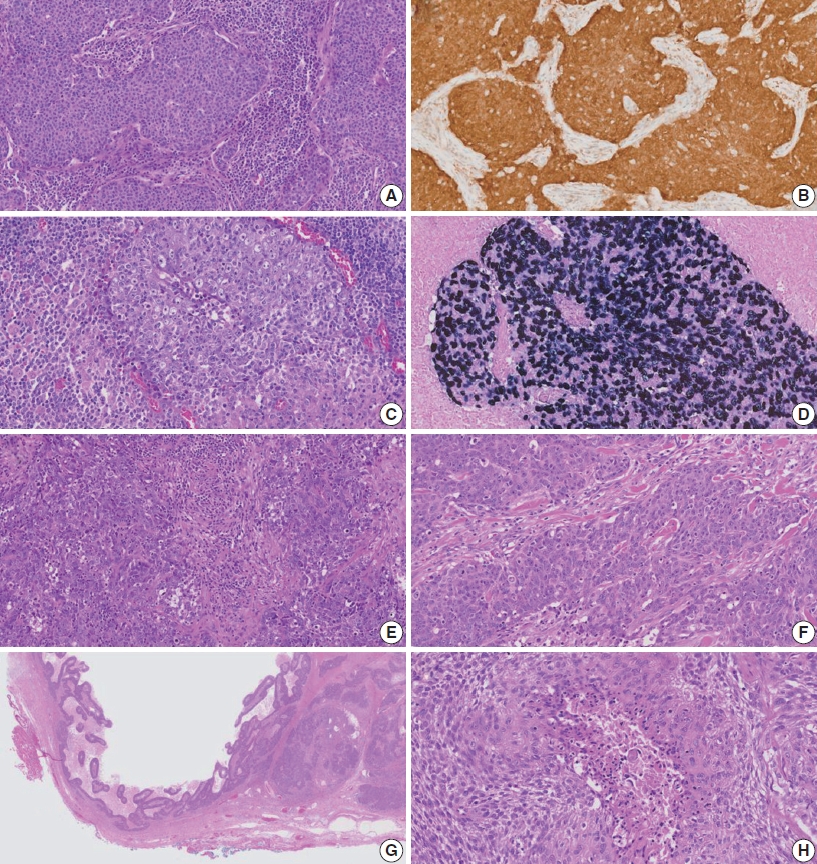

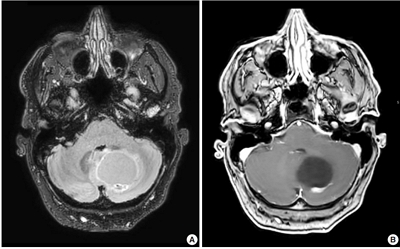
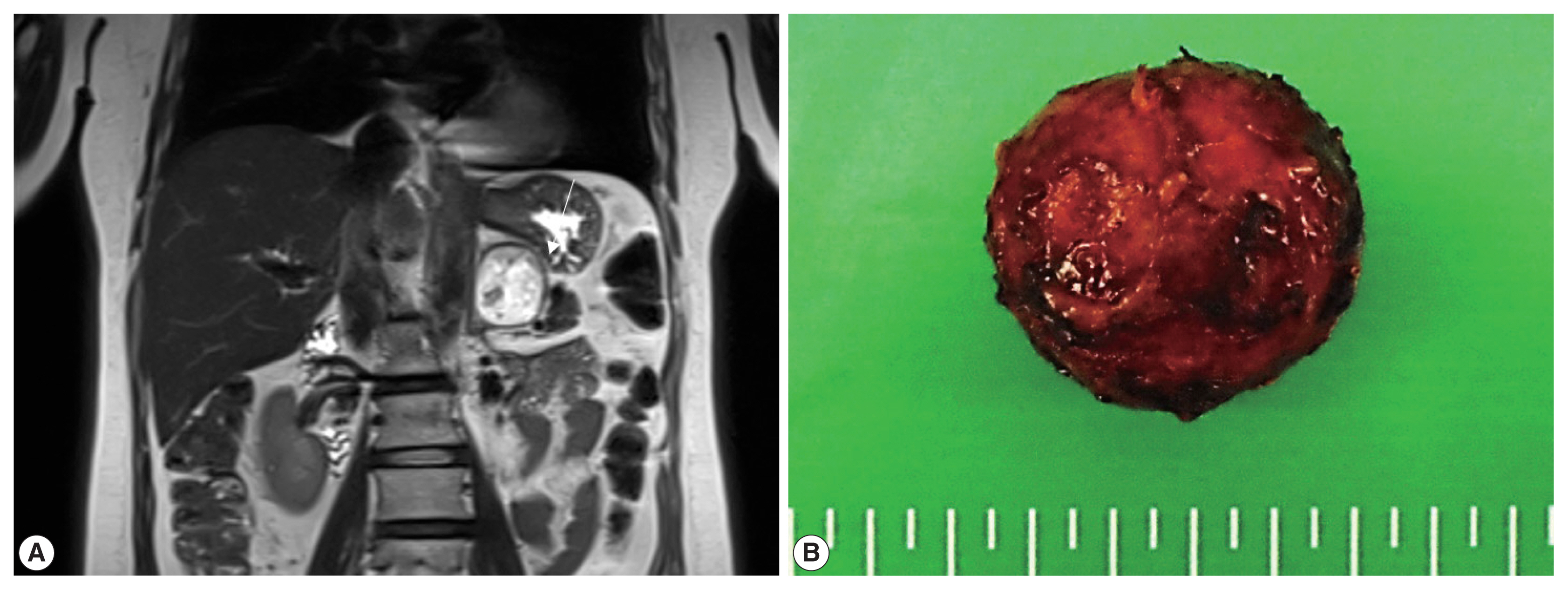
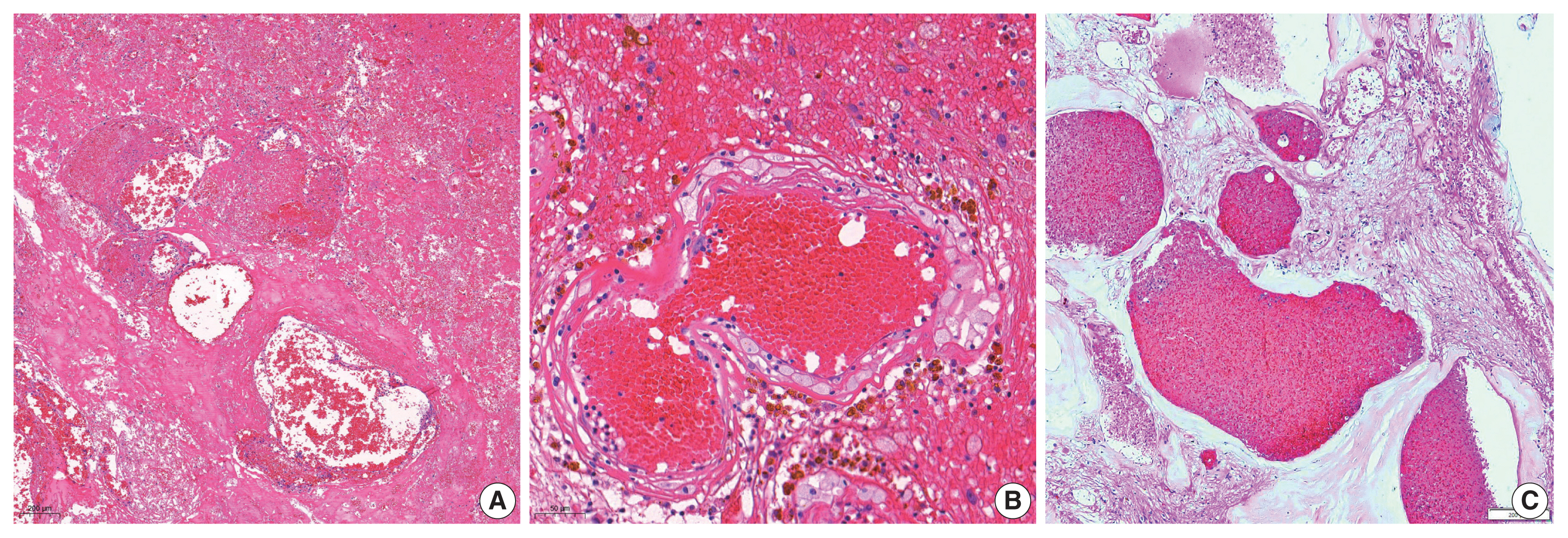
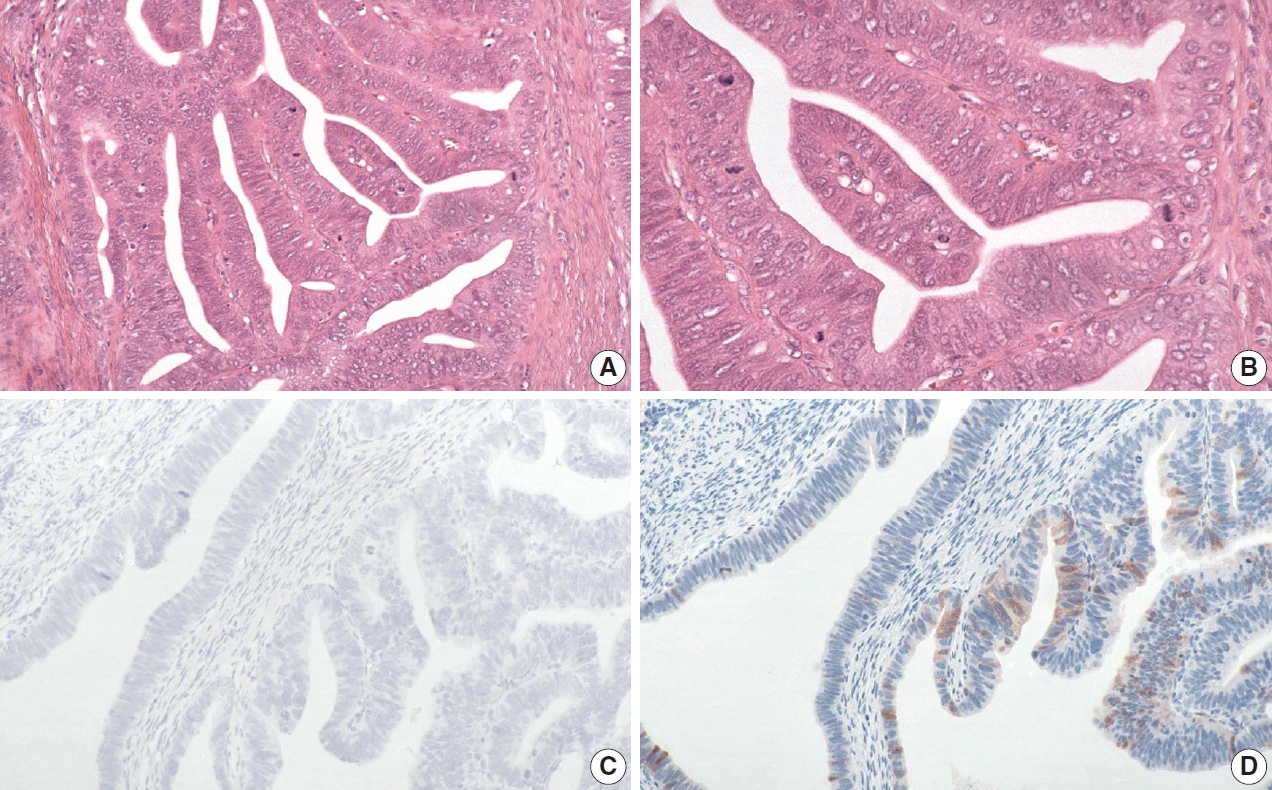
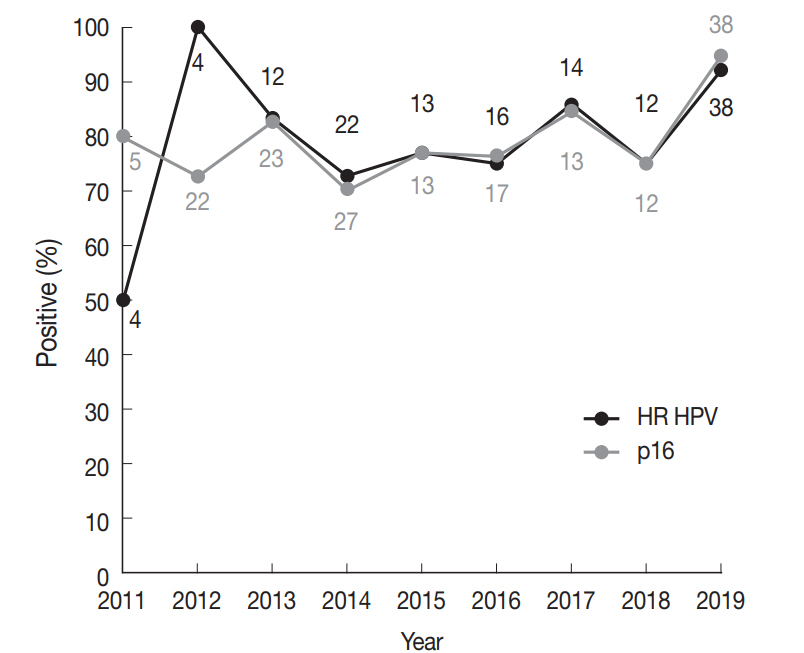
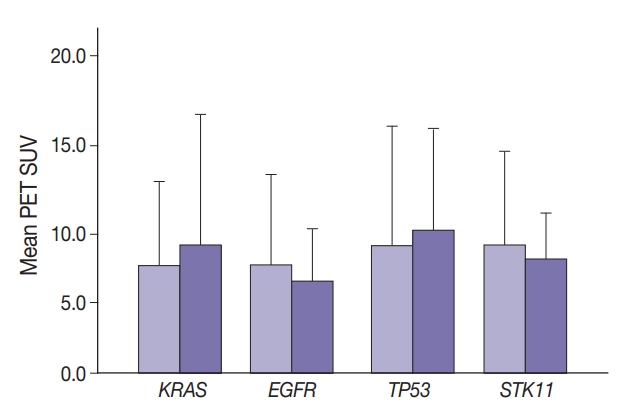
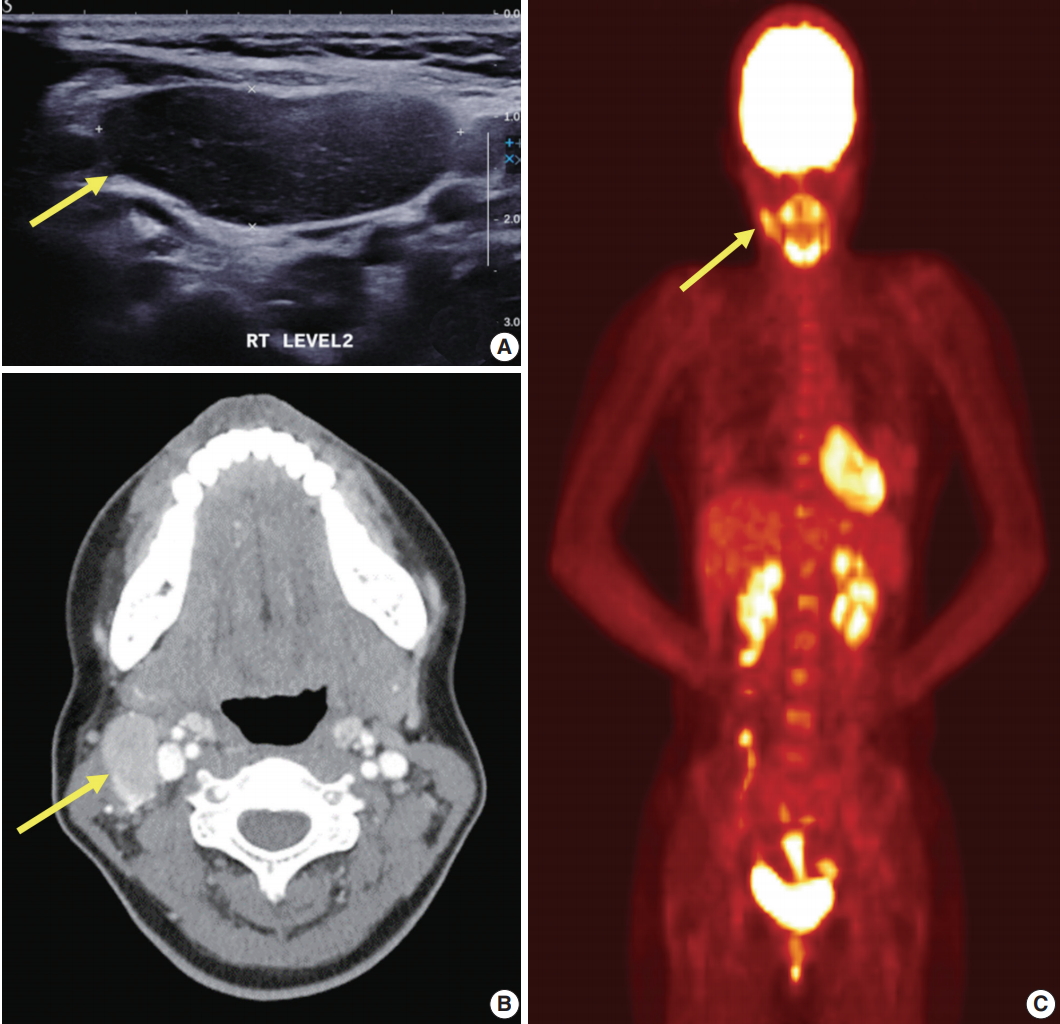
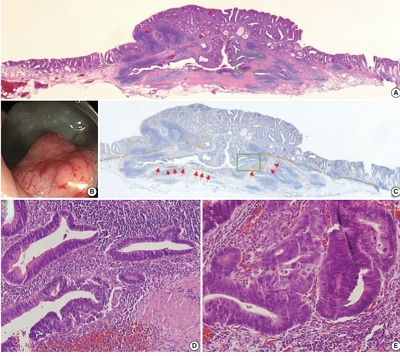

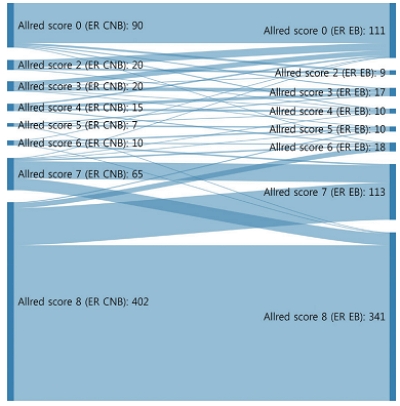
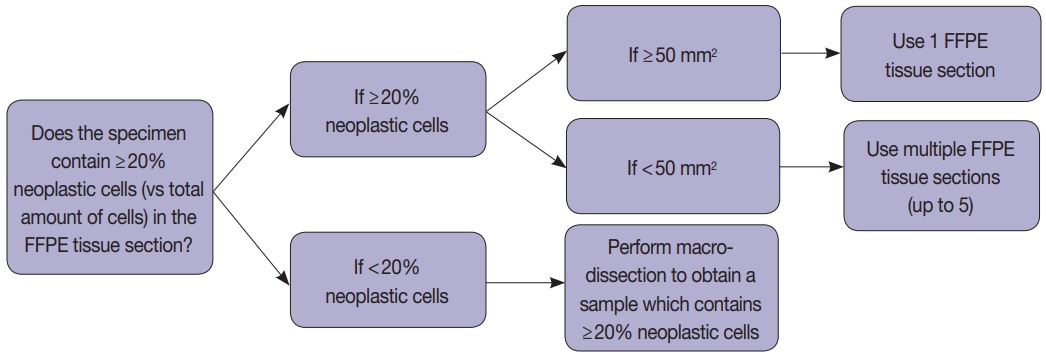
 First
First Prev
Prev



