Histologic Variations and Immunohistochemical Features of Metastatic Clear Cell Renal Cell Carcinoma
Article information
Abstract
Background
Due to advancements in treatment of metastatic and advanced renal cell carcinoma (RCC), it has become increasingly important to diagnose metastatic RCC and the specific subtype. In this study, we investigated the diverse histologic features of metastatic clear cell renal cell carcinoma (CCRCC) cases in comparison with corresponding primary lesions.
Methods
We identified 119 metastatic CCRCC cases from 81 corresponding primary lesions diagnosed between 1995 and 2010 and evaluated the diverse histologic and immunohistochemical features of these lesions.
Results
A total of 44 primary lesions (54.3%) had a non-clear cell component in addition to a typical clear cell component. Of the 119 metastatic lesions, 63 lesions (52.9%) contained a non-clear cell component, and 29 metastatic lesions were composed of a non-clear cell component only. Rhabdoid features were the most frequent non-clear cell histology among the metastatic lesions. Metastatic CCRCCs mainly showed positive CD10 and epithelial membrane antigen staining and negative cytokeratin 7 staining.
Conclusions
Metastatic CCRCC commonly showed a variety of histologic features. If there is a difficulty to diagnose metastatic CCRCC due to a variety of histologic features or small biopsy specimen, histologic review of the primary lesion and immunohistochemical analysis can help determine the correct diagnosis.
Renal cell carcinoma (RCC) patients occasionally have metastatic disease at the time of presentation (25-30%)1 and local or distant recurrences after nephrectomy in the case of localized RCC (20-40%).2 Although a large study showed that the 5-year survival rate of metastatic RCC patients is less than 10%,3 new therapeutic methods have been developed for the treatment of advanced RCC,4,5 and some can play a prominent role in the treatment of certain subtypes of RCC.6 Therefore, it has become more important to diagnose metastatic RCC and to determine the subtype of the corresponding primary lesion.
Each RCC subtype can show typical histologic features but may frequently have areas of diverse histologic variation. For example, in clear cell renal cell carcinoma (CCRCC), tumor cells typically have abundant clear cytoplasm; however, many CCRCCs contain minor populations of cells with non-clear eosinophilic cytoplasm, which is particularly common in high-grade tumors.7 Sarcomatoid differentiation occurs in 5% of tumors and is associated with a poor prognosis.7 In cases with sarcomatoid differentiation, it has been reported that the rate of metastasis at presentation or the time of nephrectomy ranges from 45% to 77%.8-12 A few reports have reported that cases of RCC could have rhabdoid tumor cells at a rate of 3.2% to 7.4%.12-16 The rhabdoid feature is characterized as sheets and clusters of variably large epithelioid cells that often have eccentric nuclei and large, paranuclear intracytoplasmic hyaline globules.17 These features were most often admixed with CCRCC and associated with poor outcome.12 When the diagnosis of RCC or determination of RCC subtypes is difficult by routine histologic examination, immunohistochemical staining may be helpful.18,19
Usually, it is easy to diagnose metastatic RCC and to determine RCC subtype by routine histologic examination of a metastatic specimen. However, diagnosis can be complicated by diverse histologic variations of RCC, as mentioned earlier. In addition, it is not uncommon to diagnose metastatic RCC lesions based only on a small biopsy specimen of a metastatic lesion without having access to the histology of the primary lesion. It can be very difficult to diagnose these samples if the small biop sy specimen consists of tumor cells showing only non-typical histologic features. Therefore, it is important to understand the histologic variations of metastatic CCRCC. Recently, Abel et al.20,21 reported two large consecutive studies regarding histologic features of metastatic RCC and pointed out that a small preoperative needle biopsy specimen from the primary or metastatic lesion may not represent characteristics of the whole tumor. However, further research on the histomorphology of metastatic RCC is still necessary. In this study, we investigated the diverse histologic features of metastatic CCRCCs in comparison with primary lesions.
MATERIALS AND METHODS
We identified cases of metastatic CCRCC and corresponding primary lesions diagnosed at Seoul National University Hospital between 1995 and 2010. A total of 119 metastatic CCRCC cases from 81 primary CCRCCs were available. With the exception of one metastatic specimen obtained by needle biopsy, all cases were obtained by excision. We collected clinical and pathological information from electronic medical records and pathologic reports and reviewed hematoxylin and eosin-stained slides for all samples as well as all available immunohistochemical slides. The RCC subtypes were reclassified according to the 2004 World Health Organization (WHO) classification.7 Additionally, we retrospectively graded tumors as grade I to IV according to the Fuhrman nuclear grading system. This study was approved by the Institutional Review Board (IRB) of Seoul National University Hospital. Histologic and immunohistochemical differences between primary and metastatic lesions were statistically analyzed using Student's t-test, and the statistics program SPSS ver. 21.0 (IBM Co., Armonk, NY, USA) was used for statistical calculations.
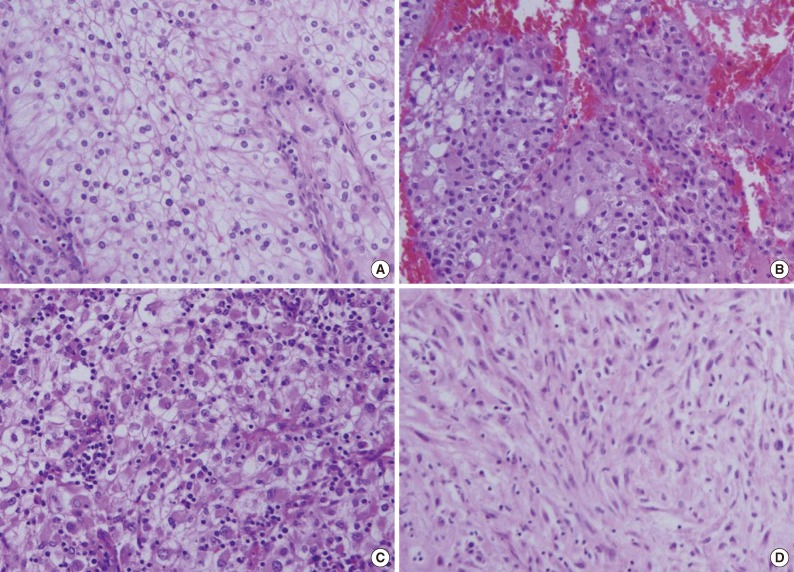
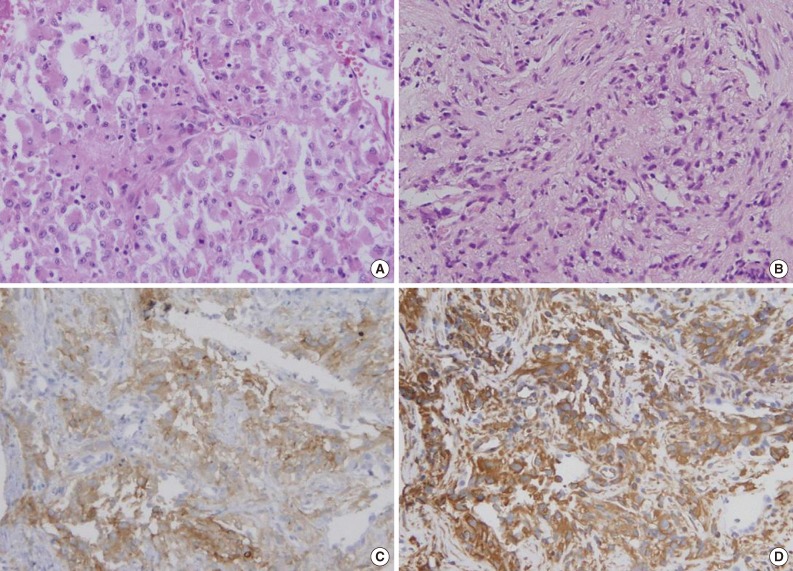
In the 81 primary CCRCC cases and 119 cases of metastatic CCRCCs, we observed several non-clear cell histologic features. Among those features, we determined relatively common fea tures such as eosinophilic cytoplasm, rhabdoid features, and sarcomatoid differentiation (Fig. 1).
RESULTS
Basic clinicopathologic characteristics
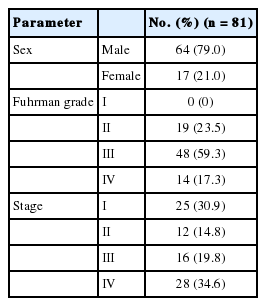
A total of 81 patients were included in this study, including 64 (79.0%) male and 17 (21.0%) female patients. The age at diagnosis ranged from 31 to 80 years, and the mean and median ages at diagnosis were 55.9 and 57 years, respectively. The distribution of the Fuhrman nuclear grading was no cases of grade I (0%), 19 cases of grade II (23.5%), 48 cases of grade III (59.3%), and 14 cases of grade IV (17.3%). According to prognostic grouping of the American Joint Committee on Cancer 7th edition, our cases had a distribution with the following pattern: 25 cases of stage I (30.9%), 12 cases of stage II (14.8%), 16 cases of stage III (19.8%), and 28 cases of stage IV (34.6%) (Table 1).
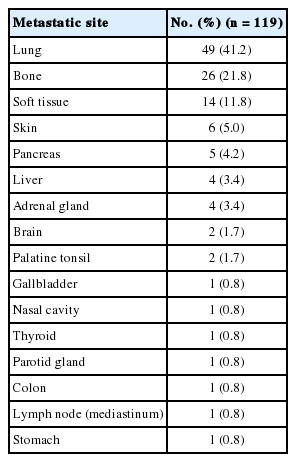
Of the 119 metastatic lesions, 49 cases (41.2%) were pulmonary metastasis and 26 (21.8%) were bone metastasis. Other frequent metastatic sites included soft tissue (14 cases, 11.8%), skin (6 cases, 5.0%), pancreas (5 cases, 4.2%), liver (4 cases, 3.4%), and adrenal gland (4 cases, 3.4%) (Table 2).
Histologic variations of primary and metastatic lesions
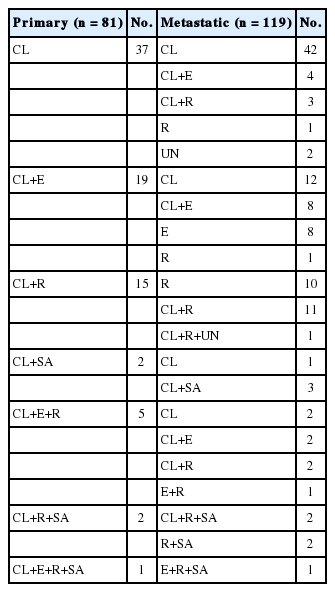
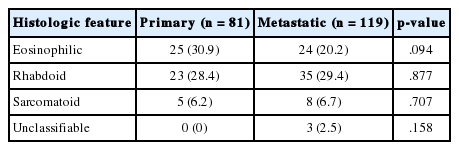
Overall histologic features of primary and metastatic lesions are described in Table 3. All 81 primary CCRCCs contained a variable proportion of typical clear cell component, and some cases had only a focal area of clear cell component. There were 37 primary lesions (45.7%) composed of only typical clear cell component, while the remaining 44 cases (54.3%) included a non-clear cell component in addition to typical clear cell area. Of the 119 metastatic lesions, 56 lesions (47.1%) were composed of only typical clear cells, and the remaining 63 lesions (52.9%) included a non-clear cell component. Among the 63 metastatic lesions with a non-clear cell component, 29 (24.4%) were composed of a non-clear cell component only without a typical clear cell area. Rhabdoid features were the most frequent non-clear cell histology in the metastatic lesions, and three metastatic lesions were exclusively composed of unclassifiable, non-characteristic histology. The frequencies of each histologic feature between primary and metastatic lesions were not statistically different (Table 4).
Proportions of non-clear cell histologic component in primary and metastatic clear cell renal cell carcinomas
Non-clear cell components observed in metastatic lesions were also present in the primary lesions. In 51 of 63 (81.0%) metastatic lesions with a non-clear cell component, the corresponding primary lesion showed the same histologic features. However, the remaining 12 metastatic tumors (19.0%) had a non-clear cell component not found in the corresponding primary tumor.
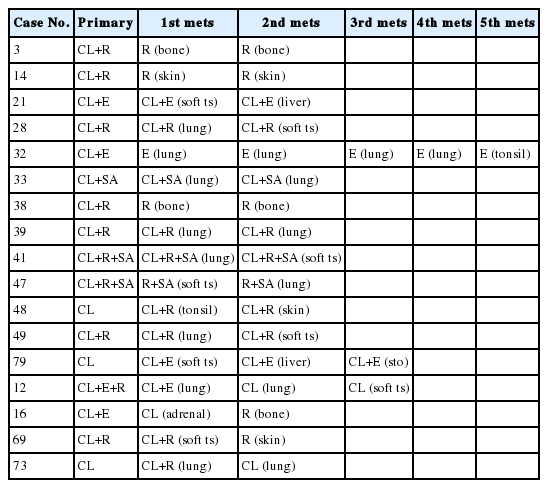
Of the 63 metastatic lesions with a non-clear cell component, 17 cases had multiple metastatic lesions. The histologic variations of multiple metastatic lesions are described in Table 5. Among 17 multiple metastasis cases, four cases (case nos. 12, 16, 69, and 73) revealed different histology in each metastatic lesion (Table 5).
Immunohistochemical results
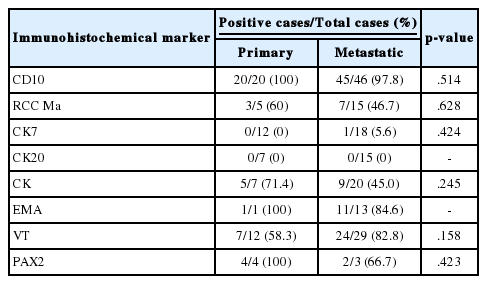
Immunohistochemical staining was performed in 21 primary lesions and 51 metastatic lesions. We reviewed all immunohistochemical staining and classified results as positive or negative. The results are shown in Table 6. Staining for CD10 and epithelial membrane antigen (EMA) was positive in most primary and metastatic CCRCCs. Renal cell carcinoma marker (RCC Ma), pan-cytokeratin (CK), vimentin (VT), and PAX2 showed positive staining in approximately 50% of the primary and metastatic CCRCCs. Cytokeratin 7 (CK7) showed positive staining in only one case of metastatic CCRCC, and cytokeratin 20 (CK20) showed negative staining in all stained tumors. Immunohistochemical results between primary and metastatic lesions were not statistically different (Table 6).
Diagnosis of the three metastatic lesions exclusively composed of non-characteristic, unclassifiable histology was difficult, but immunohistochemical staining aided in making the correct diagnosis (Fig. 2).
DISCUSSION
In this study, we found that metastatic CCRCCs frequently showed non-typical histologic features such as eosinophilic cytoplasm, rhabdoid features, and sarcomatoid differentiation, which were features also found in corresponding primary lesions. These non-typical histologic variations occasionally made the diagnosis of metastatic RCC difficult, and in these cases, histologic review of the primary lesion is important for the diagnosis of metastatic RCC.
Abel et al.20,21 claimed that preoperative biopsy specimens were limited in their ability to identify histologic subtype (especially non-clear cell type), Fuhrman nuclear grade, or sarcomatoid differentiation. They analyzed needle biopsy specimens from primary or metastatic lesions from patients with metastatic RCC compared with cytoreductive nephrectomy specimens.20 When surgical resection is not available, they recommend obtaining multiple samples from primary sites to obtain more precise information about the tumor.20 The studies involved all subtypes of RCC samples, but this study only included CCRCC samples. We also experienced the limitation of small biopsy specimens showing only non-typical histologic features. However, because we analyzed mainly resected specimens, the difficulties of diagnosing metastatic CCRCC were thought to be due to non-typical histologic features, which tended to appear frequently in metastatic CCRCCs, rather than small specimen size. As mentioned earlier, 29 of 119 (24.4%) metastatic CCRCC cases showed non-clear cell morphology only, while all 81 primary CCRCC cases contained a typical clear cell area.
The rhabdoid cells in RCCs have a high nuclear grade and are associated with a high nuclear grade of a non-rhabdoid RCC component. Additionally, the presence of rhabdoid features in RCC is related to advanced pathologic stage. These associations suggest that identification of the rhabdoid feature in RCC likely portends a poor outcome.12 One study suggests that RCC with rhabdoid features is a highly aggressive neoplasm with a malignant behavior that may be due to the high activity of cell proliferation of the rhabdoid area.13 Another study suggests that rhabdoid areas show higher immunohistochemical p53 positivity than non-rhabdoid areas in the same tumors.15 Molecular genetic studies in a few cases have shown concordant loss of chromosome 3p and a VHL gene mutation in rhabdoid and clear cells from the same case, suggesting divergent differentiation from the same clone.22 Rhabdoid RCC is associated with sarcomatoid RCC in a significant number (22%) of cases.22 In this study, rhabdoid features were observed in approximately 30% of metastatic CCRCCs, and this frequency is quite higher than in primary lesions of RCC.12-16 This finding also suggests that rhabdoid features are associated with a poor prognosis.
Several studies have suggested that most primary and metastatic CCRCCs are positive for CD10.23-27 These studies have shown that the immunohistochemical results of RCC Ma, CK, EMA, and VT staining were variable but have relatively high positivity in primary and metastatic CCRCCs.23-28 Additionally, these studies reported low positivity of CK7 and negativity of CK20 in primary CCRCCs.23 Although we investigated 21 primary lesions and 51 metastatic lesions with immunohistochemical staining, our findings were similar to those of the previous study. The positivity of CD10 and EMA and negativity of CK7 suggested metastatic CCRCC, which suggests that CD10, EMA, and CK7 may be useful makers for diagnosis of metastatic CCRCC. Also, recent studies have proposed the utility of PAX-2 or PAX-8 for the diagnosis of metastatic RCC.19,27,29,30
In general, it is not difficult to diagnose metastatic RCC and to determine the subtype of the primary lesion from a metastatic specimen. However, it can be difficult in some cases, especially when small needle biopsy specimens are utilized. During the pathologic diagnosis of a lesion thought to be metastatic RCC, histologic variations of metastatic CCRCC such as eosinophilic cytoplasm, rhabdoid features, or sarcomatoid differentiation must be considered. It is also important to review the histology of the primary lesion, if possible. If metastatic RCC cannot be diagnosed by routine hematoxylin and eosin slides only, immunohistochemical staining may be helpful.
In conclusion, metastatic CCRCC commonly showed a variety of histologic features, including eosinophilic cytoplasm, rhabdoid features, or sarcomatoid differentiation. If there is a difficulty to diagnose metastatic CCRCC because of a variety of histologic features or small biopsy specimens, histologic review of the primary lesion and immunohistochemical analysis can help determine the correct diagnosis.
Acknowledgments
This work was supported by grant 04-2011-021 from the Seoul National University Hospital Research Fund.
Notes
No potential conflict of interest relevant to this article was reported.