Highly prevalent BRAF V600E and low-frequency TERT promoter mutations underlie papillary thyroid carcinoma in Koreans
Article information
Abstract
Background
The presence of telomerase reverse transcriptase (TERT) promoter mutations have been associated with a poor prognosis in patients with papillary thyroid carcinomas (PTC). The frequency of TERT promoter mutations varies widely depending on the population and the nature of the study.
Methods
Data were prospectively collected in 724 consecutive patients who underwent thyroidectomy for PTC from 2018 to 2019. Molecular testing for BRAF V600E and TERT promoter mutations was performed in all cases.
Results
TERT promoter alterations in two hotspots (C228T and C250T) and C216T were found in 16 (2.2%) and 4 (0.6%) of all PTCs, respectively. The hotspot mutations were significantly associated with older age at diagnosis, larger tumor size, extrathyroidal extension, higher pathologic T category, lateral lymph node metastasis, and higher American Thyroid Association recurrence risk. The patients with C216T variant were younger and had a lower American Thyroid Association recurrence risk than those with hotspot mutations. Concurrent BRAF V600E was found in 19 of 20 cases with TERT promoter mutations. Of 518 microcarcinomas measuring ≤1.0 cm in size, hotspot mutations and C216T variants were detected in five (1.0%) and three (0.6%) cases, respectively.
Conclusions
Our study indicates a low frequency of TERT promoter mutations in Korean patients with PTC and supports previous findings that TERT promoter mutations are more common in older patients with unfavorable clinicopathologic features and BRAF V600E. TERT promoter mutations in patients with microcarcinoma are uncommon and may have a limited role in risk stratification. The C216T variant seems to have no clinicopathologic effect on PTC.
The incidence of thyroid cancer has dramatically increased over the past several decades [1,2]. The highest incidence of thyroid cancer in the world has been observed in Korea [3,4]. The increase in the incidence of thyroid cancer was responsible for the increase in papillary thyroid carcinoma (PTC), which accounts for over 95% of all thyroid cancer cases in Korea [3,5,6]. Despite the increased incidence of thyroid cancer, the thyroid cancer mortality rate has not changed significantly over the last three decades [3,5]. A multicenter cohort study reported a disease-specific 10-year survival rate of 98% in Korean patients with well-differentiated thyroid carcinoma [6].
Independent prognostic factors related to survival in patients with PTC include elements of cancer staging, such as patient age at diagnosis, tumor size, extensive extrathyroidal extension, and distant metastasis [7]. There have been many studies demonstrating the prognostic value of molecular markers for tumor recurrence and survival. Telomerase reverse transcriptase (TERT) promoter mutation is one of the most evident molecular factors related to poor prognosis of patients with PTC [8-11]. The cancer-specific TERT promoter mutations occur in two mutually exclusive hotspots in chromosome 5, g.1 295 228 C>T (C228T) and g.1 295 250 C>T (C250T) which correspond to 124 bp (c.–124C>T) and 146 bp (c.–146C>T), upstream from the translation start codon of the TERT gene promoter sequence [10-16]. The pooled prevalence of TERT promoter mutations in PTC was 11.3% (95% confidence interval, 9.3 to 13.5) in a previous meta-analysis of 13 studies [14]. However, the retrospective data may overestimate the mutation frequency because of potential patient selection bias. Patients with microcarcinoma ≤ 1.0 cm were more easily excluded from the molecular studies [8-10,15,17-19]. Furthermore, old archival paraffin blocks may have suboptimal DNA quality that results in molecular test failures and analytical errors.
The BRAF V600E mutation is the most common genetic alteration in PTC and remains controversial as an independent prognostic factor [7]. The coexistence of BRAF V600E and TERT promoter mutations, however, could more accurately indicate the highest mortality risk for patients with PTC [8,19].
The present study aimed to evaluate the real-world frequency of TERT promoter mutations in prospectively-collected consecutive cases of PTC and assess the relationship between TERT promoter mutations and clinicopathological features in Korean patients with PTC and a high frequency of BRAF V600E mutations.
MATERIALS AND METHODS
Patients
We reviewed the prospectively collected data from 724 consecutive patients who underwent thyroidectomy for PTC and molecular testing at Seoul St. Mary’s Hospital of the Catholic University of Korea from 2018 to 2019. Molecular tests for BRAF and TERT promoter mutations were performed in all patients who agreed to allow molecular analysis of their surgical specimens. In cases of multifocal PTCs, the largest tumor was defined as the primary lesion and was chosen for evaluation. The histologic variants of PTC were classified following the diagnostic criteria and terminology of the World Health Organization [7]. The tall cell variant was defined using 30% of tall cell area as a criterion. The PTCs were further classified as classic PTC with tall cell features if it harbored between 10%–30% tall cells and as classic PTC if it contained less than 10% of tall cell area and any well-formed papillae. Cancer staging was done using the 8th edition of the American Joint Committee on Cancer (AJCC) staging system [20]. Minimal extrathyroidal extension was defined as extrathyroidal invasion that was restricted to the perithyroidal soft tissues detected only on microscopic examination (including microscopic strap muscle invasion). When strap muscle invasion was found on preoperative imaging and/or at the time of surgery, the case was considered as gross extrathyroidal extension. Risk stratification of patients for tumor recurrence was done using the 2015 American Thyroid Association (ATA) guidelines [21].
Mutational analyses for TERT promoter and BRAF V600E mutations
Genomic DNA was extracted from 10 μm-thick formalin-fixed paraffin-embedded (FFPE) tissue blocks using a Maxwell 16 FFPE Tissue LEV Purification Kit (Promega, Fitchburg, WI, USA). Tumor areas were manually dissected with a scalpel under a microscope.
The TERT promoter was amplified using the nested polymerase chain reaction (PCR) method. The first-round 235-bp PCR amplicon was amplified using forward 5'-AGTGGATTCGCGGGCACAGA-3' and reverse 5'-CAGCGCTGCCTGAA ACTC-3' primers. Then, the second-round 163-bp PCR amplicon was amplified using forward 5'-GTCCTGCCCCTTCACCTT3' and reverse 5'-CAGCGCTGCCTGAAACTC-3' primers. Bidirectional Sanger sequencing was performed in both directions using the same primers that were used for the second-round PCR. BRAF V600E mutation was analyzed using the real-time PCR clamping technology of PNAClampTM BRAF kit (Panagene, Daejeon, Korea) [22]. Each test had a positive control of mutation-holding human genomic DNA and a negative control of distilled water.
Statistical analysis
Categorical variables were analyzed using the Pearson’s chi-square, Fisher exact test, or linear-by-linear association when appropriate. Continuous variables were compared using the Student’s t-test or Mann-Whitney test when appropriate. The statistical significance threshold was defined as a p-value less than 0.05. All statistical analyses were done using SPSS Statistics program, ver. 21.0 (IBM Corp., Armonk, NY, USA).
RESULTS
Demographic and clinicopathologic characteristics
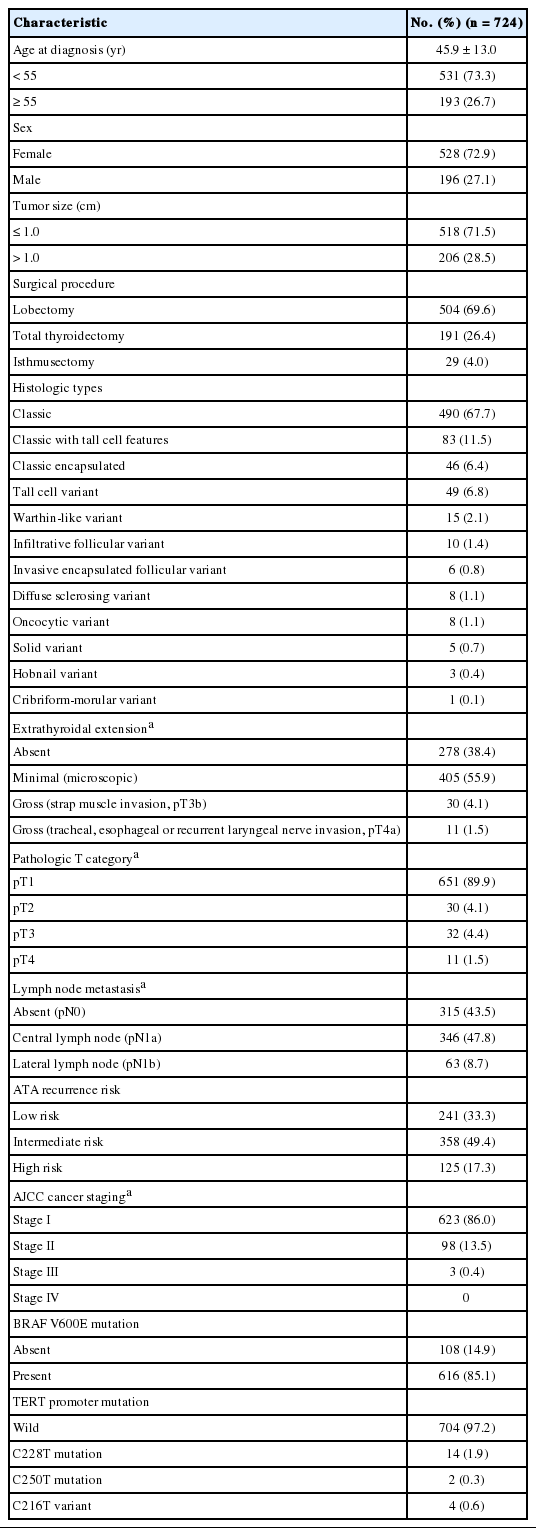
Table 1 summarizes the baseline clinicopathologic characteristics of the 724 patients with PTC. The median age of the patients at the time of diagnosis was 46 years (interquartile range [IQR], 36 to 56 years). The female to male ratio was 2.7:1. The median tumor size was 0.7 cm (IQR, 0.5 to 1.1 cm). The proportion of microcarcinomas (≤1.0 cm in size) was 71.5% (518/724). Lobectomy was done in 504 (69.6%) and total thyroidectomy in 191 patients (26.4%). The numbers of patients with minimal and gross extrathyroidal extension were 405 (55.9%) and 41 (5.7%), respectively. Cervical lymph node metastases were found in 409 patients (56.5%).
Frequency of TERT promoter and BRAF V600E mutations
Hotspot-point mutations (C228T and C250T) in the TERT promoter were found in 16 (2.2%) patients: 14 with C228T and two with C250T (Table 2, Fig. 1). Four cases had the TERT promoter variant of g.1 295 216 C>T (c.–112C>T) (hereafter C216T) (Fig. 1). The BRAF V600E mutation was found in 616 (85.1%) patients. Of 20 PTCs with TERT promoter aberrations, 19 had coexisting BRAF V600E (Table 3, Fig. 2). Fig. 2 summarizes the distribution of histologic variants of PTC and mutational profiles according to the variants. There was no correlation between TERT promoter mutations and histologic variants.
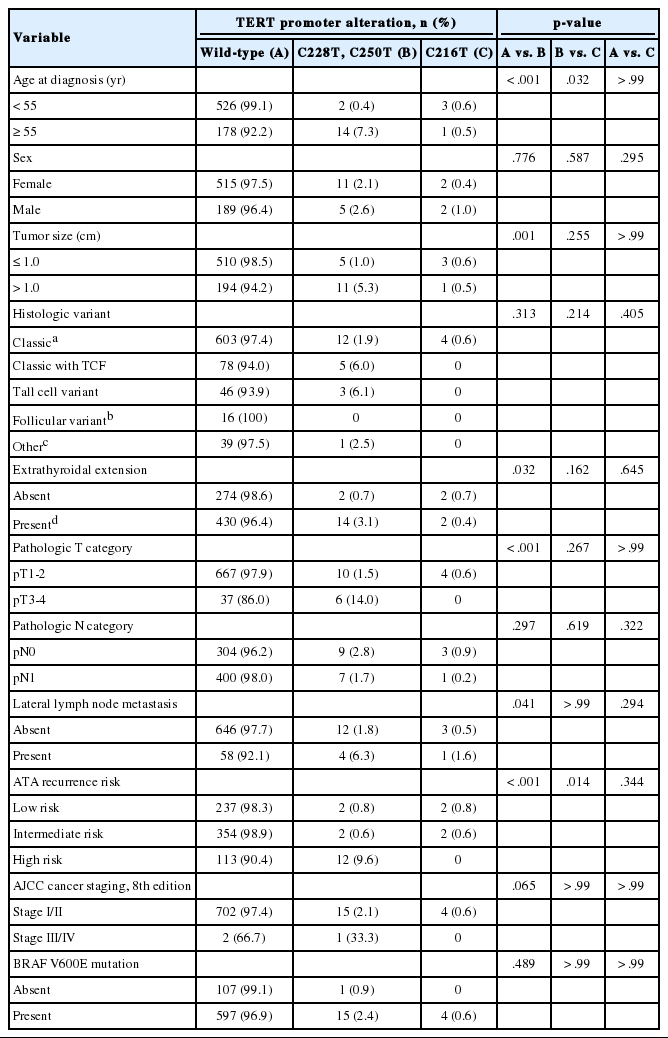
Association between TERT promoter alterations and clinicopathologic features in 724 consecutive patients with papillary thyroid carcinoma
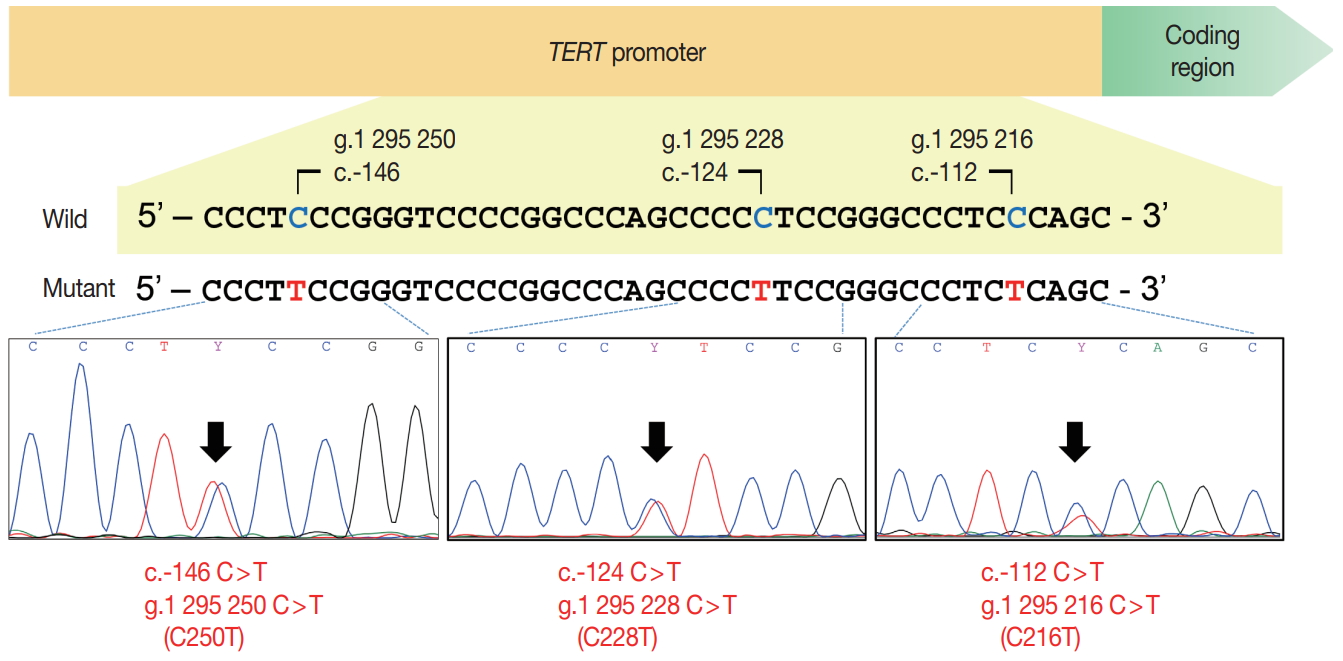
Schematic figure of the telomerase reverse transcriptase (TERT) promoter region and sequencing electropherograms of two hotspot mutations (C228T and C250T) and a C216T variant in the TERT promoter. The hotspot mutations resulted from a cytosine-to-thymine transition at genomic loci Chr5:1,295,228 (C228T) and 1,295,250 (C250T), respectively. The C216T variant is a cytosine-to-thymine transition at the 1,295,216 position of Chr5.
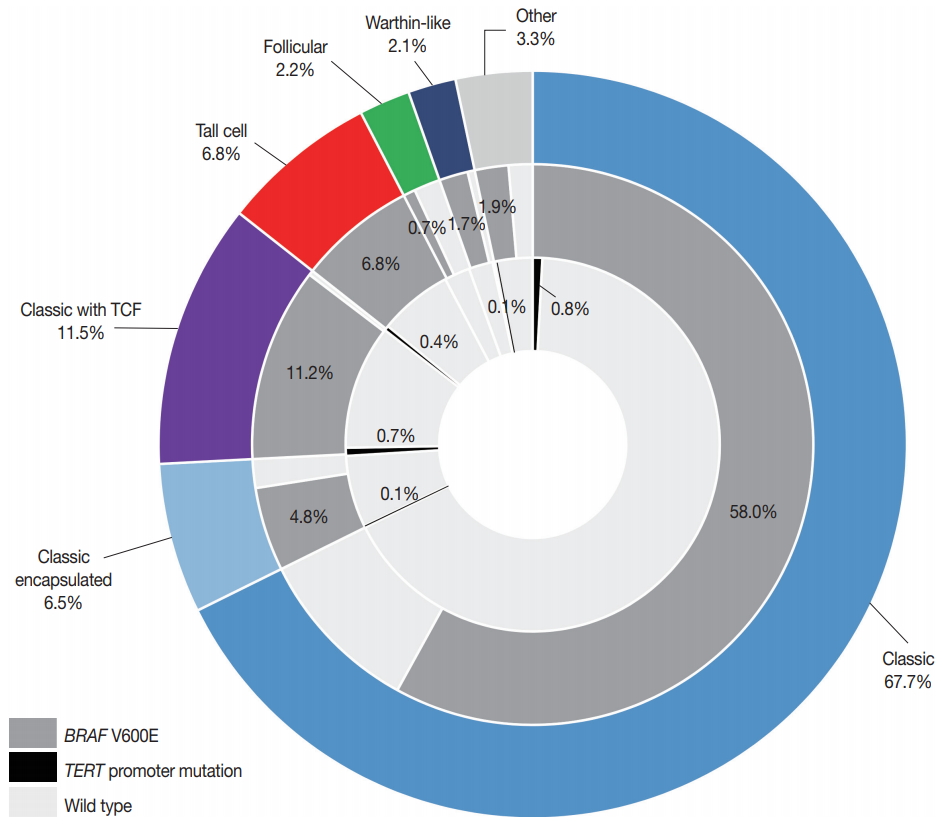
A pie chart depicting a portion of BRAF V600E and telomerase reverse transcriptase (TERT) promoter mutations (C228T and C250T) in relation to histologic variants of papillary thyroid carcinoma (n=724). The middle and inner circles show the frequency of BRAF V600E and TERT promoter mutations, respectively. The other variants included eight diffuse sclerosing, eight oncocytic, five solid, three hobnail, and one cribriform-morular variant. TCF, tall cell features.
Clinicopathologic features of patients with TERT promoter mutation
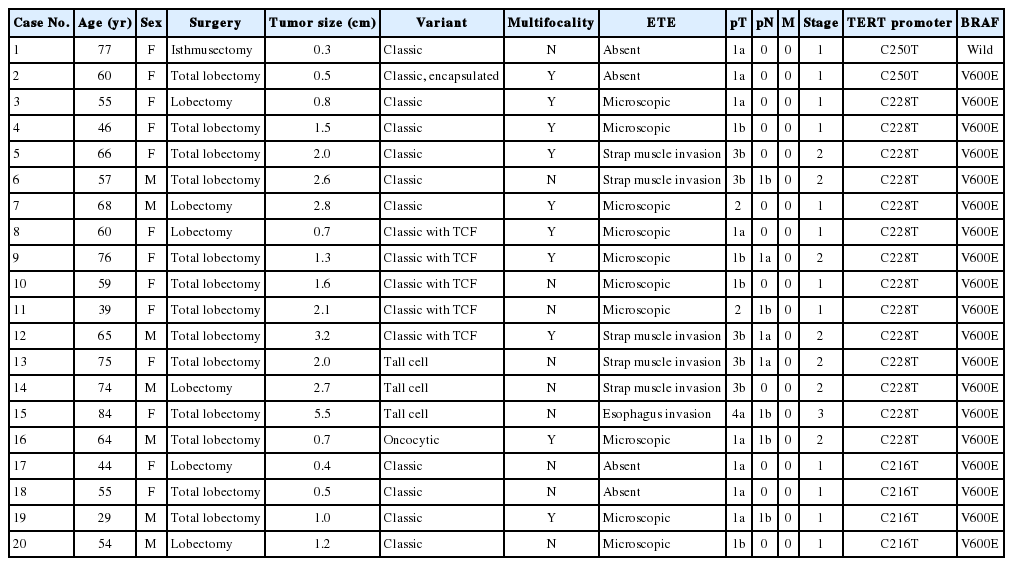
Hotspot mutations in the TERT promoter were significantly associated with age ≥55 years (p<.001), tumor size >1.0 cm (p=.001), extrathyroidal extension (p=.032), lateral lymph node metastasis (p=.041), and higher ATA recurrence risk (p<.001) (Table 2). Compared with patients with hotspot mutations, those with C216T variant were younger (p=.032) and had a lower rate of high ATA recurrence risk (p=.014). There were no significant differences in the clinicopathologic features between the patients with wild-type TERT promoter mutations and those with C216T variant of the TERT promoter (Table 2). Table 3 shows the detailed clinicopathologic features of the patients with a TERT promoter mutation.
DISCUSSION
The strength of this study stems from the prospectively collected data encompassing all consecutive patients treated for PTC with thyroid surgery. In our study, almost three-quarters of patients with PTC underwent thyroid surgery before the age of 55 years (73.3%) and had microcarcinomas (71.5%). Gross extrathyroidal extension was found in only 41 patients (5.7%). No case developed synchronous distant metastasis. Therefore, it stands to reason that the vast majority (86.0%) of patients with PTC were assigned to stage I by the 8th edition of the AJCC staging system. Although BRAF V600E mutations were highly prevalent in our study cohort, the frequency of hotspot mutations in the TERT promoter was 2.2%, which is far lower than that reported in previous studies for PTC (pooled mean prevalence of 11.3%) [14,23]. These results indicate that most PTC tumors in the current study should have indolent behavior.
In our study, additional benefits were gained by including microcarcinomas in the molecular analysis. Hotspot mutations of the TERT promoter were found in five of 518 papillary microcarcinomas (1.0%). Minimal extrathyroidal extension, found in three of the five patients with hotspot mutations, did not affect the pathologic T category. Patient age ranged from 39 to 84 years. Although the frequency of TERT promoter mutations is lower than that of previous studies, these findings are in line with a previous Italian study showing no correlation with unfavorable outcomes [24]. The Italian study showed that TERT promoter mutations were found in 4.7% of papillary microcarcinomas and were not associated with poor clinical features [24]. As active surveillance is one of the treatment options for low-risk papillary microcarcinomas, the identification of TERT promoter mutations may facilitate decision-making on appropriate candidates for active surveillance [21,25]. One Japanese study reported that no TERT promoter mutations were found in 25 patients selected from 1,252 patients with low-risk papillary microcarcinoma who were managed with active surveillance [25]. These results, however, need to be validated in further larger studies.
Since most studies reported only pathogenic hotspot mutations, little is known about the prevalence and functional role of the TERT promoter C216T variant in human cancers. The C216T variant was found in four cases of our study cohort and has been previously reported in two lung adenocarcinomas [26] and one esophageal squamous cell carcinoma [27]. In our study, all four patients with the C216T were younger (range, 29 to 55 years) than those with hotspot mutations and had no unfavorable clinicopathologic features. Therefore, we suggest that the TERT promoter C216T variant may be a non-pathogenic DNA polymorphism in PTC.
Many studies have shown synergistic effects of concurrent BRAF V600E and TERT promoter mutations on the poor prognosis and mortality risk of patients with PTC [8,11,17-19,23]. The C228T and C250T mutations of the TERT promoter generate an 11-bp binding motif (5'-CCCCTTCCGGG-3') for E-twentysix (ETS) transcription factors [13]. Mitogen-activated protein kinase pathway activation by the BRAF V600E mutation upregulates ETS transcription factors, which results in increased TERT mRNA expression by the binding of the mutated TERT promoter to ETS [28]. In our study, all 14 patients with the TERT promoter C228T mutation had a concurrent BRAF V600E mutation. In Korean patients with PTC and a high prevalence of the BRAF V600E, further studies are needed to validate the prognostic utility of risk stratification of patients with PTC by combining BRAF V600E and TERT promoter mutations.
In summary, this study demonstrated that the TERT promoter mutation frequency was 2.2% in prospectively collected patients, and the presently reported frequency is lower than that reported in previous studies. TERT promoter mutations were more common in older patients with unfavorable clinicopathologic features and a BRAF V600E mutation. Although they were observed less frequently than in those with larger tumors, TERT promoter mutations also occurred in patients with microcarcinoma and low-risk clinicopathologic features. The C216T variant was found in 0.6% of all PTCs and may be a non-pathogenic DNA polymorphism.
Notes
Ethics Statement
This study was approved by the Institutional Review Board of Seoul St. Mary’s Hospital, the Catholic University of Korea (KC16SISI0709). Informed consent was obtained from each patient.
Author contributions
Conceptualization: CKJ. Data curation: SYK, TK, KK, JSB, JSK, CKJ. Formal analysis: SYK, TK, CKJ. Funding acquisition: CKJ. Investigation: SYK, TK, CKJ. Methodology: SYK, TK, CKJ. Project administration: SYK, CKJ. Resources: SYK, KK, JSB, JSK, CKJ. Software: SYK, CKJ. Supervision: CKJ. Validation: KK, JSB, JSK, CKJ. Visualization: SYK, KK, JSB, JSK, CKJ. Writing—original draft: SYK, CKJ. Writing—review & editing: SYK, TK, KK, JSB, JSK, CKJ. Approval of final manuscript: all authors.
Conflicts of Interest
C.K.J. is the editor-in-chief of the Journal of Pathology and Translational Medicine and was not involved in the editorial evaluation or decision to publish this article. All remaining authors declare that they have no potential conflicts of interest.
Funding
This study was supported by a grant (2017R1D1A1B03029597) from the Basic Science Research Program through the National Research Foundation of Korea.