Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 47(1); 2013 > Article
-
Original Article
Alteration of the E-Cadherin/β-Catenin Complex Is an Independent Poor Prognostic Factor in Lung Adenocarcinoma - Hyojin Kim1, Seol Bong Yoo1,2, Pingli Sun1,3, Yan Jin1,4, Sanghoon Jheon3, Choon Taek Lee5, Jin-Haeng Chung1,4
-
Korean Journal of Pathology 2013;47(1):44-51.
DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.1.44
Published online: February 25, 2013
1Department of Pathology, Seoul National University College of Medicine, Seoul, Korea.
2Department of Pathology, Presbyterian Medical Center, Jeonju, Korea.
3Department of Thoracic Surgery, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Korea.
4Department of Pathology, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Korea.
5Department of Internal Medicine, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Korea.
- Corresponding Author: Jin-Haeng Chung, M.D., Ph.D. Department of Pathology, Seoul National University Bundang Hospital, 82 Gumi-ro 173beon-gil, Bundang-gu, Seongnam 463-707, Korea. Tel: +82-31-787-7713, Fax: +82-31-787-4012, 'chungjh@snu.ac.kr'
© 2013 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background
- Epithelial-mesenchymal transition (EMT) is an important step in the invasion and progression of cancer and in the development of chemoresistance by cancer cells.
-
Methods
- To address the clinical significance of the EMT pathway in lung adenocarcinoma and the association of the pathway with histological subtype, we examined 193 surgically resected lung adenocarcinoma samples for the expression of representative EMT-related proteins (E-cadherin, β-catenin, and vimentin) by immunohistochemistry. Histological subtypes were classified according to the 2011 International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society classification. The results for EMT-related protein expression were analyzed for correlation with clinicopathological features and with survival.
-
Results
- The loss of E-cadherin expression and aberrant β-catenin expression were significantly associated with larger tumor size, pleural invasion, lymphatic/vascular invasion, and advanced pathological stage (p<0.05). The alteration of the E-cadherin/β-catenin complex was least frequently observed in the lepidic-predominant group, but these associations were not statistically significant. In the multivariate analysis, altered E-cadherin/β-catenin complex expression was found to be an independent poor prognostic factor (p=0.017; hazard ratio, 1.926; 95% confidence interval, 1.119 to 3.314).
-
Conclusions
- The alteration of the expression of the E-cadherin/β-catenin complex was associated with aggressive tumor behavior in lung adenocarcinoma.
- Patients and specimens
- We retrospectively obtained formalin-fixed and paraffin-embedded tissues from 193 surgically resected primary lung adenocarcinomas at our university hospital from November 2004 to December 2008. None of these patients had undergone chemotherapy or radiotherapy prior to the surgery. Clinicopathological data were obtained from medical records and pathology reports. The 193 patients consisted of 90 (46.6%) men and 103 (53.4%) women with ages ranging from 33 to 84 years (mean, 62.4 years). For smoking status, patients were divided into never-smokers (<100 lifetime cigarettes) and smokers. The median follow-up period for the patients was 41.8 months, with a range of 1 to 84 months. The patient characteristics are shown in Table 1.
- Hematoxylin and eosin-stained slides were reviewed in each case to confirm the original diagnosis and subtype classification. The histological features were evaluated based on the predominant pattern, i.e., lepidic (formerly bronchioloalveolar cell carcinoma), acinar, papillary, micropapillary, and solid, according to the new IASLC/ATS/ERS adenocarcinoma classification.2 Two pathologists (H.K. and J.H.C.) independently reviewed these slides to select the most representative sections showing the predominant histological pattern. The pathological stage (p-stage) of each tumor was assigned following the guidelines from the 7th edition of the American Joint Committee on Cancer tumor-node-metastasis classification.20 This study was approved by the Institutional Review Board of Seoul National University Bundang Hospital.
- Immunohistochemistry
- The expression levels of three EMT-related proteins were analyzed by immunohistochemistry. Antibodies for the following molecules were used in this study; E-cadherin (1:200, BD Biosciences, San Jose, CA, USA), β-catenin (1:750, BD Biosciences) and vimentin (1:100, Neomarkers, Fremont, CA, USA). From the tissue microarray blocks, 4-µm-thick sections were transferred to poly-L-lysine-coated glass slides and incubated in a dry oven at 60℃ for 1 hour. These sections were then dewaxed in xylene (three changes), rehydrated in a graded series of ethanol solutions with decreasing concentrations and rinsed in Tris-buffered saline (TBS; pH 7.4). The endogenous peroxidase activity was inactivated with 5% hydrogen peroxide in methanol for 15 minutes at 37℃. The slides were then placed in citrate buffer (10% citrate buffer stock in distilled water, pH 6.0) and microwaved for 10 minutes. Non-reactive staining was blocked using 1% horse serum in TBS (pH 7.4) for 3 minutes. Primary antibodies were applied, and antibody binding was detected using the avidin-biotin-peroxidase complex (Universal Elite ABC kit PK-6200, Vectastain, Burlingame, CA, USA) for 10 minutes and diaminobenzidine tetrahydrochloride solution (Kit HK153-5K, Biogenex, San Ramon, CA, USA). Positive controls, consisting of samples with known reactivity for the antibody, and negative controls, obtained by omitting the primary antibody, were included.
- Interpretation of the results
- For each marker, different cell sites were evaluated: membrane for E-cadherin and β-catenin and cytoplasm for vimentin. The scoring criteria used were based on a semiquantitative approach for determining the percentage of positive tumor cells (0-100%) multiplied by the staining intensity (0, negative; 1, weak; 2, moderate; 3, strong), and a total score range of 0 to 300 was generated for each sample, where 0 to 100 was classified as negative for E-cadherin and vimentin expression and 101 to 300 was classified as positive. Regarding β-catenin immunoreactivity, the membranous expression of β-catenin in the tumor was judged to be "normal" if more than 70% of the membranes of tumor cells were positively stained. If fewer than 70% of the cells were stained, the membranous expression was judged to be "reduced." The cut-off value of 70% is a standard value for the differentiation of normal and reduced levels of β-catenin expression because more than 70% of normal cells typically exhibit membranous expression of β-catenin.21 Additionally, strong positive cytoplasmic-nuclear, membranocytoplasmic and cytoplasmic expression patterns for β-catenin (≥10%) were considered altered expression.15,22
- Statistical analysis
- Pearson's chi-square test was used to evaluate the associations between EMT-related protein expression and clinicopathological variables. The Spearman ρ test was used to compare the protein expression levels to investigate the relationship between EMT-related proteins. A Kaplan-Meier analysis was performed to construct survival curves, and statistical significance was assessed using the log-rank test. A multivariate analysis was performed by Cox proportional hazards regression modeling. All statistical tests were two sided, and statistical significance was accepted for p-values <0.05. All analyses were performed using SPSS ver. 18.0 (SPSS Inc., Chicago, IL, USA).
MATERIALS AND METHODS
- Immunoreactivity of EMT-related proteins
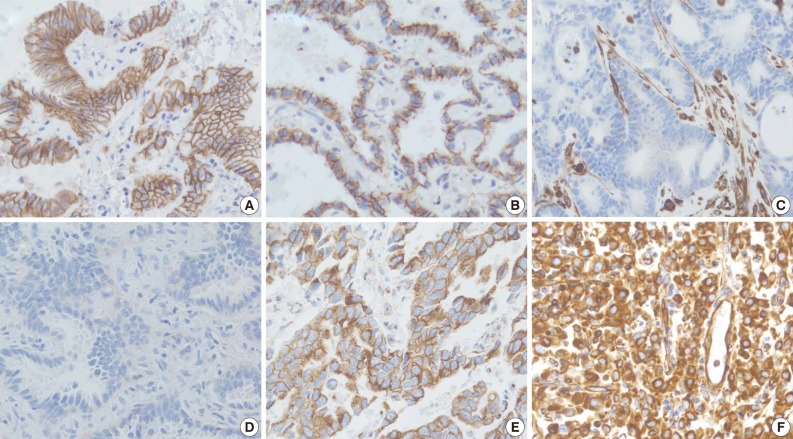
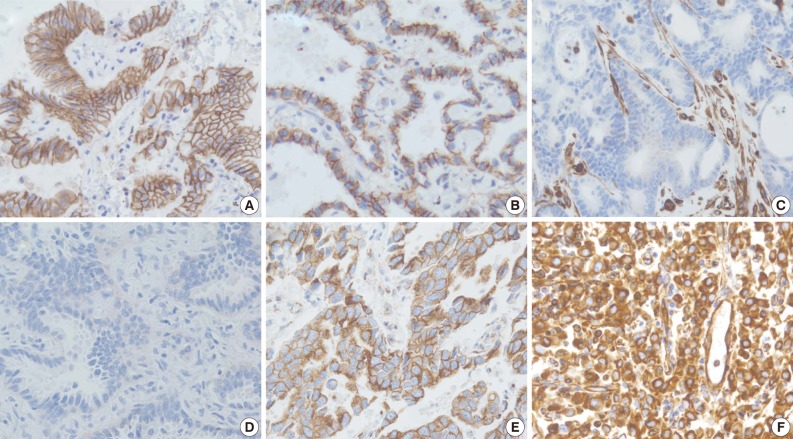
- The staining intensity and expression pattern of EMT proteins are shown in Fig. 1. The E-cadherin expression was accentuated toward the apical and basolateral regions of the cell membrane (Fig. 1A), and negative E-cadherin expression (Fig. 1D) was observed in 17.6% (34/193) of samples. β-Catenin was usually localized to the membrane (Fig. 1B), and reduced membranous expression and altered expression in the cytoplasm and/or nucleus were considered aberrant expression (Fig. 1E). Aberrant β-catenin expression was observed in 78.2% (151/193) of samples. Vimentin was usually negative in neoplastic cells (Fig. 1C), while the aberrant cytoplasmic expression of vimentin (Fig. 1F) was observed in 27.5% (53/193) of samples.
- The clinicopathological characteristics of the patients with altered expression of each protein are summarized in Table 1. Negative E-cadherin expression and aberrant β-catenin expression were significantly associated with a larger tumor size, pleural invasion, lymphatic/vascular invasion, and advanced pathological stage (p<0.05). The expression of vimentin was associated with pleural invasion (p=0.014). The Spearman ρ test revealed that negative E-cadherin expression was significantly associated with aberrant β-catenin expression in spite of a low level of correlation (correlation coefficient ρ=0.145, p=0.044). Aberrant β-catenin expression was also significantly associated with vimentin expression (correlation coefficient ρ=-0.24, p=0.001). There was no association between E-cadherin and vimentin expression (Table 2). To determine the most predictable combination for patient prognosis, we selected a combination of three markers. Among the three groups, both E-cadherin and β-catenin alterations were found in 16.1% (31/193) of patients. These alterations were also significantly associated with a larger tumor size, pleural invasion and advanced pathological stage (p=0.023, p=0.030, and p=0.020, respectively) (Table 3). The combination alterations of E-cadherin/vimentin and β-catenin/vimentin were not associated with clinicopathological factors (p>0.05, data not shown).
- EMT protein expression according to histological subtype
- The 193 adenocarcinomas consisted of 140 cases of acinar, six of papillary, 26 of lepidic, 18 of solid, two of micropapillary predominant pattern, and one of invasive mucinous adenocarcinoma according to the new IASLC/ATS/ERS classification. The correlations between the altered expression levels of the two EMT proteins and the histological subtypes are summarized in Table 4. Regarding the predominant subtype, EMT protein alteration was least frequently observed in the lepidic-predominant group, but this difference was not statistically significant (p>0.05).
- Survival analysis
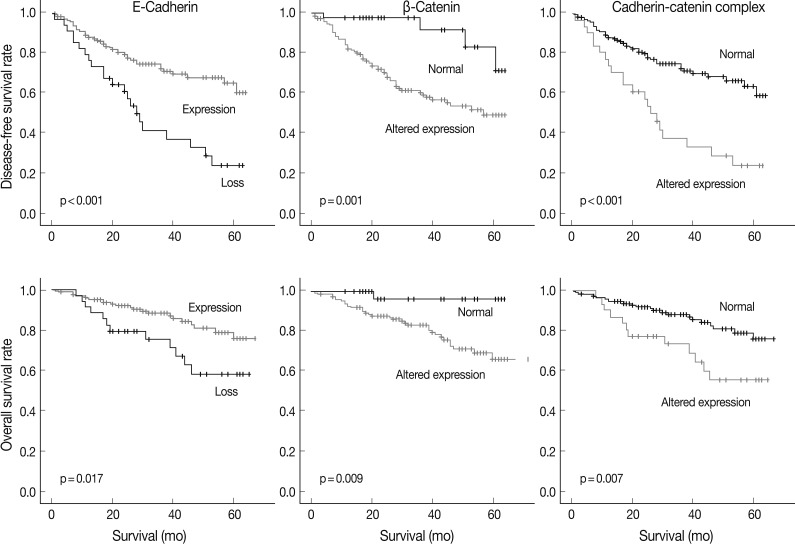
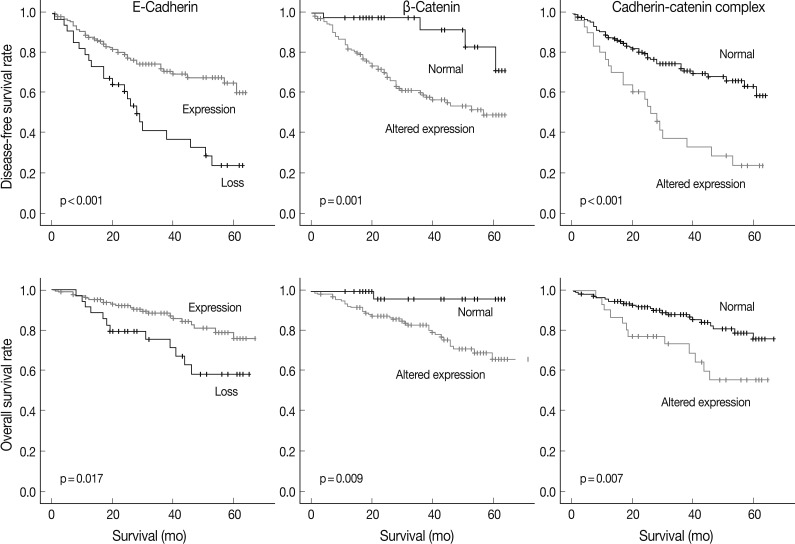
- At the time of analysis, the number of tumor recurrences was 65 (33.7%), and the number of cancer-specific deaths was 35 (18.1%). The results of the Kaplan-Meier univariate analysis showed that negative E-cadherin expression and aberrant β-catenin expression were significantly associated with a lower disease-free survival (DFS) rate (p<0.001 and p=0.001) and overall survival (OS) rate (p=0.017 and p=0.009) (Fig. 2). Altered expression of both proteins together was also significantly associated with a lower DFS (p<0.001) and OS (p=0.007) (Fig. 2). Vimentin expression was not related to DFS or OS (p>0.05, data not shown).
- A multivariate Cox proportional hazards regression analysis indicated that the altered expression of the cadherin/catenin complex was an independent poor prognostic indicator (p=0.017; hazard ratio [HR], 1.926; 95% confidence interval, 1.119 to 3.314), although the pathological stage was the strongest predictive factor (p≤0.005) (Table 5).
RESULTS
- In this study, we demonstrated that the altered expression of the E-cadherin/β-catenin complex was an independent poor prognostic factor in lung adenocarcinoma. Our results are in agreement with those of previous studies that demonstrated that the altered expression of various EMT-related molecules was associated with tumor progression and poor survival in various malignancies.21,23-25 Kase et al.21 demonstrated a significant unfavorable prognosis in NSCLC when both E-cadherin and β-catenin were reduced. However, the impact of vimentin expression was inconsistent.18 The loss of epithelial protein expression in tumor cells reflects the ability of epithelial cells to overcome their physical constraints and detach from adherent junctions. E-Cadherin is not only one of the typical adhesion molecules, but is also a master programmer of EMT.26,27 The E-cadherin gene is somatically inactivated in many diffuse-type cancers, including lobular carcinoma of the breast28 and diffuse gastric carcinoma.29 Moreover, the downregulation of E-cadherin is observed in solid, non-diffuse-type cancers at the tumor-stroma boundary where singly invading, EMT-derived tumor cells are observed in histological sections. β-Catenin is a pivotal component of the canonical Wnt signaling pathway and E-cadherin-associated homotypic cell adhesion.30 Regarding this pivotal role of β-catenin, we also analyzed Wnt1/β-catenin expression (data not shown). In a previous study, the authors demonstrated that aberrant Wnt1/β-catenin expression was an independent poor prognostic marker of NSCLC.15 More specifically, Wnt1 overexpression and aberrant expression of β-catenin were correlated with each other and significantly associated with poor prognosis in patients with squamous cell carcinoma but was not in the patients with adenocarcinoma. In adenocarcinoma histology, loss of E-cadherin not Wnt1 overexpression was correlated with aberrant β-catenin expression, and altered expression of the E-cadherin/β-catenin served as a poor prognostic factor. From these results, we suggest that β-catenin may play a dual role in cells as a major structural component of cell-cell adherent junctions in the adenocarcinoma and as a pivotal signaling molecule in the Wnt pathway in squamous cell carcinoma.
- In our study, altered E-cadherin/β-catenin complex expression was significantly associated with various pathological parameters including the invasiveness of tumor cells, DFS and OS. Moreover, altered E-cadherin/β-catenin complex expression was an independent prognostic factor, although neither the loss of E-cadherin nor altered β-catenin expression was a significant prognostic factor according to the multivariate analysis. These results suggest that alteration of cadherin-catenin complex expression is important in tumor invasion and affects the survival of patients with lung adenocarcinoma. In addition, the expression patterns for the cadherin-catenin complex may more accurately predict patient outcome than expression of a single marker.
- Aberrant cytoplasmic expression of vimentin was observed in 27.5% of lung adenocarcinoma in our study. Vimentin expression showed an association with aberrant β-catenin expression; however, there was no implication of aberrant β-catenin/vimentin complex on patient clinicopathologic factors or survival. Similar to our findings, Soltermann et al.18 reported inconsistent associations between vimentin expression and clinicopathologic factors in NSCLC. Therefore, the role of vimentin expression needs further investigation.
- We investigated the expression of EMT-related proteins according to histological subtype based on the new adenocarcinoma classification of the IASLC/ATS/ERS. EMT protein alteration was least frequent in the lepidic-predominant group, but this association was not statistically significant. These findings support the hypothesis that the lepidic subtype, known as neoplastic cell replacement with retained normal alveolar architecture, shows less aggressive behavior and is associated with a better prognosis compared to other histological subtypes of pulmonary adenocarcinoma.6,7
- In summary, altered E-cadherin/β-catenin complex expression was found to be an independent poor prognostic factor (p=0.017; HR, 1.926; 95% confidence interval, 1.119 to 3.314) for surgically resected lung adenocarcinoma patients. Our current results suggest that the alteration of the expression of the E-cadherin/β-catenin complex is associated with aggressive tumor behavior and non-lepidic histology in lung adenocarcinoma.
DISCUSSION
Acknowledgments
Acknowledgments
- 1. Jemal A, Siegel R, Xu J, Ward E. Cancer statistics, 2010. CA Cancer J Clin 2010; 60: 277–300. PMID: 20610543. ArticlePubMed
- 2. Travis WD, Brambilla E, Noguchi M, et al. International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society: international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol 2011; 6: 244–285. PMID: 21252716. ArticlePubMedPMC
- 3. Yoshizawa A, Motoi N, Riely GJ, et al. Impact of proposed IASLC/ATS/ERS classification of lung adenocarcinoma: prognostic subgroups and implications for further revision of staging based on analysis of 514 stage I cases. Mod Pathol 2011; 24: 653–664. PMID: 21252858. ArticlePubMed
- 4. Russell PA, Wainer Z, Wright GM, Daniels M, Conron M, Williams RA. Does lung adenocarcinoma subtype predict patient survival?: A clinicopathologic study based on the new International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society international multidisciplinary lung adenocarcinoma classification. J Thorac Oncol 2011; 6: 1496–1504. PMID: 21642859. ArticlePubMed
- 5. Travis WD, Brambilla E, Noguchi M, et al. International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society: international multidisciplinary classification of lung adenocarcinoma: executive summary. Proc Am Thorac Soc 2011; 8: 381–385. PMID: 21926387. ArticlePubMed
- 6. Sakurai H, Maeshima A, Watanabe S, et al. Grade of stromal invasion in small adenocarcinoma of the lung: histopathological minimal invasion and prognosis. Am J Surg Pathol 2004; 28: 198–206. PMID: 15043309. ArticlePubMed
- 7. Yim J, Zhu LC, Chiriboga L, Watson HN, Goldberg JD, Moreira AL. Histologic features are important prognostic indicators in early stages lung adenocarcinomas. Mod Pathol 2007; 20: 233–241. PMID: 17192789. ArticlePubMed
- 8. Ohtaki Y, Yoshida J, Ishii G, et al. Prognostic significance of a solid component in pulmonary adenocarcinoma. Ann Thorac Surg 2011; 91: 1051–1057. PMID: 21440121. ArticlePubMed
- 9. Takuwa T, Ishii G, Nagai K, et al. Characteristic immunophenotype of solid subtype component in lung adenocarcinoma. Ann Surg Oncol 2012; 19: 3943–3952. PMID: 22669454. ArticlePubMed
- 10. Christiansen JJ, Rajasekaran AK. Reassessing epithelial to mesenchymal transition as a prerequisite for carcinoma invasion and metastasis. Cancer Res 2006; 66: 8319–8326. PMID: 16951136. ArticlePubMed
- 11. Burdsal CA, Damsky CH, Pedersen RA. The role of E-cadherin and integrins in mesoderm differentiation and migration at the mammalian primitive streak. Development 1993; 118: 829–844. PMID: 7521282. ArticlePubMedPDF
- 12. Nieto MA. The early steps of neural crest development. Mech Dev 2001; 105: 27–35. PMID: 11429279. ArticlePubMed
- 13. Iwatsuki M, Mimori K, Yokobori T, et al. Epithelial-mesenchymal transition in cancer development and its clinical significance. Cancer Sci 2010; 101: 293–299. PMID: 19961486. ArticlePubMed
- 14. Thiery JP, Acloque H, Huang RY, Nieto MA. Epithelial-mesenchymal transitions in development and disease. Cell 2009; 139: 871–890. PMID: 19945376. ArticlePubMed
- 15. Xu X, Sun PL, Li JZ, Jheon S, Lee CT, Chung JH. Aberrant Wnt1/beta-catenin expression is an independent poor prognostic marker of non-small cell lung cancer after surgery. J Thorac Oncol 2011; 6: 716–724. PMID: 21336184. ArticlePubMed
- 16. Yauch RL, Januario T, Eberhard DA, et al. Epithelial versus mesenchymal phenotype determines in vitro sensitivity and predicts clinical activity of erlotinib in lung cancer patients. Clin Cancer Res 2005; 11(24 Pt 1):8686–8698. PMID: 16361555. ArticlePubMed
- 17. Prudkin L, Liu DD, Ozburn NC, et al. Epithelial-to-mesenchymal transition in the development and progression of adenocarcinoma and squamous cell carcinoma of the lung. Mod Pathol 2009; 22: 668–678. PMID: 19270647. ArticlePubMedPMC
- 18. Soltermann A, Tischler V, Arbogast S, et al. Prognostic significance of epithelial-mesenchymal and mesenchymal-epithelial transition protein expression in non-small cell lung cancer. Clin Cancer Res 2008; 14: 7430–7437. PMID: 19010860. ArticlePubMed
- 19. Chung JH, Rho JK, Xu X, et al. Clinical and molecular evidences of epithelial to mesenchymal transition in acquired resistance to EGFR-TKIs. Lung Cancer 2011; 73: 176–182. PMID: 21168239. ArticlePubMed
- 20. Rusch VW, Asamura H, Watanabe H, et al. The IASLC lung cancer staging project: a proposal for a new international lymph node map in the forthcoming seventh edition of the TNM classification for lung cancer. J Thorac Oncol 2009; 4: 568–577. PMID: 19357537. ArticlePubMed
- 21. Kase S, Sugio K, Yamazaki K, Okamoto T, Yano T, Sugimachi K. Expression of E-cadherin and beta-catenin in human non-small cell lung cancer and the clinical significance. Clin Cancer Res 2000; 6: 4789–4796. PMID: 11156236. ArticlePubMed
- 22. Xu HT, Wang L, Lin D, et al. Abnormal beta-catenin and reduced axin expression are associated with poor differentiation and progression in non-small cell lung cancer. Am J Clin Pathol 2006; 125: 534–541. PMID: 16627264. ArticlePubMed
- 23. Li L, Zhang Z, Li B, Gao F, Li L, Jonas JB. E-cadherin and beta-catenin expression in sebaceous eyelid adenocarcinomas. Graefes Arch Clin Exp Ophthalmol 2011; 249: 1867–1873. PMID: 21739269. ArticlePubMed
- 24. Matsuoka T, Mitomi H, Fukui N, et al. Cluster analysis of claudin-1 and -4, E-cadherin, and beta-catenin expression in colorectal cancers. J Surg Oncol 2011; 103: 674–686. PMID: 21360533. ArticlePubMed
- 25. Galera-Ruiz H, Ríos MJ, González-Cámpora R, et al. The cadherin-catenin complex in nasopharyngeal carcinoma. Eur Arch Otorhinolaryngol 2011; 268: 1335–1341. PMID: 21240516. ArticlePubMedPMC
- 26. Cavallaro U, Christofori G. Cell adhesion and signalling by cadherins and Ig-CAMs in cancer. Nat Rev Cancer 2004; 4: 118–132. PMID: 14964308. ArticlePubMed
- 27. Guarino M, Rubino B, Ballabio G. The role of epithelial-mesenchymal transition in cancer pathology. Pathology 2007; 39: 305–318. PMID: 17558857. ArticlePubMed
- 28. Willipinski-Stapelfeldt B, Riethdorf S, Assmann V, et al. Changes in cytoskeletal protein composition indicative of an epithelial-mesenchymal transition in human micrometastatic and primary breast carcinoma cells. Clin Cancer Res 2005; 11: 8006–8014. PMID: 16299229. ArticlePubMed
- 29. Kim MA, Lee HS, Lee HE, Kim JH, Yang HK, Kim WH. Prognostic importance of epithelial-mesenchymal transition-related protein expression in gastric carcinoma. Histopathology 2009; 54: 442–451. PMID: 19309396. ArticlePubMed
- 30. Ben-Ze'ev A, Shtutman M, Zhurinsky J. The integration of cell adhesion with gene expression: the role of beta-catenin. Exp Cell Res 2000; 261: 75–82. PMID: 11082277. ArticlePubMed
References
| Characteristics | No. of examined |
E-Cadherin |
p-value |
β-Catenin |
p-value |
Vimentin |
p-value | |||
|---|---|---|---|---|---|---|---|---|---|---|
| Negative | Expression | Aberrant expression | Normal | Expression | Normal | |||||
| Total | 193 (100) | |||||||||
| Sex | ||||||||||
| Male | 90 (46.6) | 20 (22.2) | 70 (77.8) | 0.084 | 71 (78.9) | 19 (21.1) | 0.489 | 27 (30.0) | 63 (70.0) | 0.282 |
| Female | 103 (53.3) | 14 (13.6) | 89 (86.4) | 80 (77.7) | 23 (22.3) | 26 (25.2) | 77 (74.8) | |||
| Age (yr) | ||||||||||
| ≤ 65 | 79 (40.9) | 12 (15.2) | 67 (84.8) | 0.295 | 60 (75.9) | 19 (24.1) | 0.32 | 23 (29.1) | 56 (70.9) | 0.394 |
| > 65 | 114 (59.1) | 22 (19.3) | 92 (80.7) | 91 (79.8) | 23 (20.2) | 30 (26.3) | 84 (73.7) | |||
| Smoking history | ||||||||||
| No | 115 (59.6) | 15 (13.0) | 100 (87.0) | 0.034* | 92 (80.0) | 23 (20.0) | 0.292 | 33 (28.7) | 82 (71.3) | 0.383 |
| Yes | 78 (40.4) | 19 (24.4) | 59 (75.9) | 59 (75.6) | 19 (24.4) | 20 (25.6) | 58 (74.4) | |||
| Tumor size (cm) | ||||||||||
| ≤ 3 | 127 (65.8) | 17 (13.4) | 110 (86.6) | 0.028* | 92 (72.4) | 35 (27.6) | 0.004* | 32 (25.2) | 95 (74.8) | 0.209 |
| > 3 | 66 (34.2) | 17 (25.8) | 49 (74.2) | 59 (89.4) | 7 (10.6) | 21 (31.8) | 45 (68.2) | |||
| Pleural invasion | ||||||||||
| Absent | 132 (67.9) | 17 (13.0) | 114 (87.0) | 0.013* | 93 (71.0) | 38 (29.0) | <0.001* | 29 (22.1) | 102 (77.9) | 0.014* |
| Present | 62 P2.1) | 17 (27.4) | 45 (72.6) | 58 (93.5) | 4 (6.5) | 24 (38.7) | 38 (61.3) | |||
| Lymphatic invasion | ||||||||||
| Absent | 124 (64.2) | 18 (14.5) | 106 (85.5) | 0.095 | 88 (71.0) | 36 (29.0) | 0.001* | 31 (25.0) | 93 (75.0) | 0.195 |
| Present | 69 (35.8) | 16 (23.2) | 53 (76.8) | 63 (91.3) | 6 (8.7) | 22 (31.9) | 47 (68.1) | |||
| Vascular invasion | ||||||||||
| Absent | 174 (90.2) | 27 (15.5) | 147 (84.5) | 0.029* | 133 (76.4) | 41 (23.6) | 0.051 | 48 (27.6) | 126 (72.4) | 0.573 |
| Present | 19 (9.8) | 7 (36.8) | 12 (63.2) | 18 (94.7) | 1 (5.3) | 5 (26.3) | 14 (73.7) | |||
| Stage | ||||||||||
| I | 126 (65.3) | 17 (13.5) | 109 (86.5) | 0.023* | 88 (69.8) | 38 (30.2) | <0.001* | 33 (26.2) | 93 (73.8) | 0.921 |
| II | 23 (11.9) | 4 (17.4) | 19 (82.6) | 20 (87.0) | 3 (13.0) | 9 P9.1) | 14 (60.9) | |||
| III | 44 (22.8) | 13 (29.5) | 31 (70.55) | 43 (97.7) | 1 (2.3) | 11 (25.0) | 33 (75.0) | |||
|
Correlation coefficients ρ (n = 193) |
|||
|---|---|---|---|
| E-Cadherin | β-Catenin | Vimentin | |
| E-Cadherin | 1 | 0.145* | -0.051 |
| β-Catenin | 1 | -0.24* | |
| Vimentin | 1 | ||
| Characteristics | No. of examined |
Altered caherin-catenin complex |
||
|---|---|---|---|---|
| Alteration | Normal | p-value | ||
| Total | 193 (100) | |||
| Sex | ||||
| Male | 90 (46.6) | 18 (20.0) | 72 (80.05) | 0.116 |
| Female | 103 (53.3) | 13 (12.6) | 90 (87.4) | |
| Age (yr) | ||||
| ≤ 65 | 79 (40.9) | 11 (13.9) | 68 (86.1) | 0.32 |
| > 65 | 114 (59.1) | 20 (17.5) | 94 (82.5) | |
| Smoking history | ||||
| No | 115 (59.6) | 13 (11.3) | 102 (88.7) | 0.024* |
| Yes | 78 (40.4) | 18 (23.1) | 60 (76.9) | |
| Tumor size (cm) | ||||
| ≤ 3 | 127 (65.8) | 15 (11.8) | 112 (88.2) | 0.023* |
| > 3 | 66 (34.2) | 16 (24.2) | 50 (75.8) | |
| Pleural invasion | ||||
| Absent | 132 (67.9) | 16 (12.2) | 115 (87.8) | 0.030* |
| Present | 62 (32.1) | 15 (24.2) | 47 (75.8) | |
| Lymphatic invasion | ||||
| Absent | 124 (64.2) | 16 (12.9) | 108 (87.1) | 0.083 |
| Present | 69 (35.8) | 15 (21.7) | 54 (78.3) | |
| Vascular invasion | ||||
| Absent | 174 (90.2) | 25 (14.4) | 149 (85.6) | 0.061 |
| Present | 19 (9.8) | 6 (31.6) | 13 (68.4) | |
| Stage | ||||
| I | 126 (65.3) | 15 (11.9) | 111 (88.1) | |
| II | 23 (11.9) | 4 (17.4) | 19 (82.6) | 0.020* |
| III | 44 (22.8) | 12 (27.3) | 32 (72.7) | |
| Prognostic factors | Hazard ratio (95% CI) | p-value |
|---|---|---|
| Cadherin-catenin complex | 1.926 (1.119-3.314) | 0.018* |
| Alteration vs normal | ||
| Pleural invasion | ||
| Present vs absent | 1.071 (0.942-1.513) | 0.458 |
| Pathologic stage | ||
| II vs I | 2.928 (1.387-6.183) | 0.005* |
| III vs I | 6.034 (3.292-11.060) | < 0.001* |
Figure & Data
References
Citations

- Prognostic significance of stem cell-related marker expression and its correlation with histologic subtypes in lung adenocarcinoma
Eunhyang Park, Soo Young Park, Ping-Li Sun, Yan Jin, Ji Eun Kim, Sanghoon Jheon, Kwhanmien Kim, Choon Taek Lee, Hyojin Kim, Jin-Haeng Chung
Oncotarget.2106; 7(27): 42502. CrossRef - Epigenetic Alterations of DNA Methylation and miRNA Contribution to Lung Adenocarcinoma
Wenhan Cai, Miao Jing, Jiaxin Wen, Hua Guo, Zhiqiang Xue
Frontiers in Genetics.2022;[Epub] CrossRef - Clinicopathological significance and prognostic value of E-cadherin expression in non-small cell lung cancer
Dong Chao, Gawei Hu, Qingxin Li
Medicine.2021; 100(7): e24748. CrossRef - Aberrant Expression of β-Catenin Correlates with Infiltrating Immune Cells and Prognosis in NSCLC
Hongmei Zheng, Yue Ning, Yang Yang, Yuting Zhan, Haihua Wang, Qiuyuan Wen, Jinwu Peng, Songqing Fan
Pathology and Oncology Research.2021;[Epub] CrossRef - Prognostic Significance of Wnt1, Wnt2, E-Cadherin, and β-catenin Expression in Operable Non-small Cell Lung Cancer
Anna Wrona, Aleksandra Sejda, Rafał Dziadziuszko, Jacek Jassem
Journal of Histochemistry & Cytochemistry.2021; 69(11): 711. CrossRef - Analysis of genes associated with prognosis of lung adenocarcinoma based on GEO and TCGA databases
Ye Yu, Xuemei Tian
Medicine.2020; 99(19): e20183. CrossRef - The roles of TG-interacting factor in cadmium exposure-promoted invasion and migration of lung cancer cells
Yadong Wang, Li Shi, Jiangmin Li, Haiyu Wang, Haiyan Yang
Toxicology in Vitro.2019; 61: 104630. CrossRef - Pizotifen inhibits the proliferation and invasion of gastric cancer cells
Ying Jiang, Wei Wang, Xi Wu, Jihua Shi
Experimental and Therapeutic Medicine.2019;[Epub] CrossRef - SNAI2 and TWIST1 in lymph node progression in early stages of NSCLC patients
Camille Emprou, Pauline Le Van Quyen, Jérémie Jégu, Nathalie Prim, Noëlle Weingertner, Eric Guérin, Erwan Pencreach, Michèle Legrain, Anne‐Claire Voegeli, Charlotte Leduc, Bertrand Mennecier, Pierre‐Emmanuel Falcoz, Anne Olland, Nicolas Santelmo, Elisabet
Cancer Medicine.2018; 7(7): 3278. CrossRef - E-Cadherin Loss Accelerates Tumor Progression and Metastasis in a Mouse Model of Lung Adenocarcinoma
Kerstin W. Sinkevicius, Kelly J. Bellaria, Juliana Barrios, Patrizia Pessina, Manav Gupta, Christine Fillmore Brainson, Roderick T. Bronson, Carla F. Kim
American Journal of Respiratory Cell and Molecular Biology.2018; 59(2): 237. CrossRef - Downregulation of peroxiredoxin II suppresses the proliferation and metastasis of gastric cancer cells
Linjun Niu, Ang Liu, Wei Xu, Liang Yang, Wugang Zhu, Yuming Gu
Oncology Letters.2018;[Epub] CrossRef - Implications of NOVA1 suppression within the microenvironment of gastric cancer: association with immune cell dysregulation
Eun Kyung Kim, Sun Och Yoon, Woon Yong Jung, Hyunjoo Lee, Youngran Kang, You-Jin Jang, Soon Won Hong, Seung Ho Choi, Woo Ick Yang
Gastric Cancer.2017; 20(3): 438. CrossRef - High FDG uptake on PET is associated with negative cell-to-cell adhesion molecule E-cadherin expression in lung adenocarcinoma
Kotaro Higashi, Yoshimichi Ueda, Miyako Shimasaki, Yasuhito Ishigaki, Yuka Nakamura, Manabu Oguchi, Tsutomu Takegami, Naoto Watanabe
Annals of Nuclear Medicine.2017; 31(8): 590. CrossRef - MicroRNA expression profiles and clinicopathological implications in lung adenocarcinoma according to EGFR, KRAS, and ALK status
Hyojin Kim, Jeong Mi Yang, Yan Jin, Sanghoon Jheon, Kwhanmien Kim, Choon Taek Lee, Jin-Haeng Chung, Jin Ho Paik
Oncotarget.2017; 8(5): 8484. CrossRef - A meta-analysis of abnormal β-catenin immunohistochemical expression as a prognostic factor in lung cancer: location is more important
Y. Yang, J. Shen, Jiaxi He, Jianxing He, G. Jiang
Clinical and Translational Oncology.2016; 18(7): 685. CrossRef - Aquaporin 1 Is an Independent Marker of Poor Prognosis in Lung Adenocarcinoma
Sumi Yun, Ping-Li Sun, Yan Jin, Hyojin Kim, Eunhyang Park, Soo Young Park, Kyuho Lee, Kyoungyul Lee, Jin-Haeng Chung
Journal of Pathology and Translational Medicine.2016; 50(4): 251. CrossRef - Prognostic Values of Vimentin Expression and Its Clinicopathological Significance in Non-Small Cell Lung Cancer: A Meta-Analysis of Observational Studies with 4118 Cases
Zhihua Ye, Xin Zhang, Yihuan Luo, Shikang Li, Lanshan Huang, Zuyun Li, Ping Li, Gang Chen, Aamir Ahmad
PLOS ONE.2016; 11(9): e0163162. CrossRef - Myoferlin expression in non-small cell lung cancer: Prognostic role and correlation with VEGFR-2 expression
DAE HYUN SONG, GYUNG HYUCK KO, JEONG HEE LEE, JONG SIL LEE, GYEONG-WON LEE, HYEON CHEOL KIM, JUNG WOOK YANG, ROK WON HEO, GU SEOB ROH, SUN-YOUNG HAN, DONG CHUL KIM
Oncology Letters.2016; 11(2): 998. CrossRef - Short hairpin RNA silencing of TGF-βRII and FZD-7 synergistically suppresses proliferation and metastasis of hepatocellular carcinoma cells
CONG CHEN, YUYANG XUE, DEJUN ZHANG, WEI XU, HAO XU, HONG YAO, DONGSHENG PEI, YUMING GU
Oncology Letters.2016; 11(3): 2039. CrossRef - NOVA1 inhibition by miR-146b-5p in the remnant tissue microenvironment defines occult residual disease after gastric cancer removal
Sun Och Yoon, Eun Kyung Kim, Mira Lee, Woon Yong Jung, Hyunjoo Lee, Youngran Kang, You-Jin Jang, Soon Won Hong, Seung Ho Choi, Woo Ick Yang
Oncotarget.2016; 7(3): 2475. CrossRef - Immunohistochemical demonstration of alteration of β-catenin during tumor metastasis by different mechanisms according to histology in lung cancer
XIANHUA XU, JI EUN KIM, PING-LI SUN, SEOL BONG YOO, HYOJIN KIM, YAN JIN, JIN-HAENG CHUNG
Experimental and Therapeutic Medicine.2015; 9(2): 311. CrossRef - FRK Inhibits Migration and Invasion of Human Glioma Cells by Promoting N-cadherin/β-catenin Complex Formation
Qiong Shi, Xu Song, Jun Wang, Jia Gu, Weijian Zhang, Jinxia Hu, Xiuping Zhou, Rutong Yu
Journal of Molecular Neuroscience.2015; 55(1): 32. CrossRef - Dissociation of E-cadherin/β-catenin complex by MG132 and bortezomib enhances CDDP induced cell death in oral cancer SCC-25 cells
Lanhai Lü, Xiqiang Liu, Cheng Wang, Fengchun Hu, Jianning Wang, Hongzhang Huang
Toxicology in Vitro.2015; 29(8): 1965. CrossRef - Epigallocatechin-3-gallate inhibits nicotine-induced migration and invasion by the suppression of angiogenesis and epithelial-mesenchymal transition in non-small cell lung cancer cells
JINGLI SHI, FEI LIU, WENZHANG ZHANG, XIN LIU, BIHUA LIN, XUDONG TANG
Oncology Reports.2015; 33(6): 2972. CrossRef - Clinicopathologic and prognostic significance of c-MYC copy number gain in lung adenocarcinomas
A N Seo, J M Yang, H Kim, S Jheon, K Kim, C T Lee, Y Jin, S Yun, J-H Chung, J H Paik
British Journal of Cancer.2014; 110(11): 2688. CrossRef - The Clinicopathological Significance of Epithelial Mesenchymal Transition Associated Protein Expression in Head and Neck Squamous Cell Carcinoma
Kyu Ho Kim, Lucia Kim, Suk Jin Choi, Jee Young Han, Joon Mee Kim, Young Chae Chu, Young-Mo Kim, In Suh Park, Joo Han Lim
Korean Journal of Pathology.2014; 48(4): 263. CrossRef - Adenoid dysplasia of the oral mucosa
Belinda Bunn, Keith Hunter, Syed Ali Khurram, W.F.P. van Heerden
Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.2014; 118(5): 586. CrossRef - FGFR1 amplification is associated with poor prognosis and smoking in non-small-cell lung cancer
An Na Seo, Yan Jin, Hee Jin Lee, Ping-Li Sun, Hyojin Kim, Sanghoon Jheon, Kwhanmien Kim, Choon-Taek Lee, Jin-Haeng Chung
Virchows Archiv.2014; 465(5): 547. CrossRef - FNC, a Novel Nucleoside Analogue, Blocks Invasion of Aggressive Non-Hodgkin Lymphoma Cell Lines Via Inhibition of the Wnt/β-Catenin Signaling Pathway
Yan Zhang, Chen-Ping Wang, Xi-Xi Ding, Ning Wang, Fang Ma, Jin-Hua Jiang, Qing-Duan Wang, Jun-Biao Chang
Asian Pacific Journal of Cancer Prevention.2014; 15(16): 6829. CrossRef - β-Catenin overexpression is associated with gefitinib resistance in non-small cell lung cancer cells
Xia Fang, Pan Gu, Caicun Zhou, Aibin Liang, Shenxiang Ren, Fang Liu, Yu Zeng, Yunjin Wu, Yinmin Zhao, Binbin Huang, Zongmei Zhang, Xianghua Yi
Pulmonary Pharmacology & Therapeutics.2014; 28(1): 41. CrossRef - Tumor‐size‐based morphological features of metastatic lymph node tumors from primary lung adenocarcinoma
Eiji Yamada, Genichiro Ishii, Nao Aramaki, Keiju Aokage, Tomoyuki Hishida, Junji Yoshida, Motohiro Kojima, Kanji Nagai, Atsushi Ochiai
Pathology International.2014; 64(12): 591. CrossRef - Prognostic and Clinicopathological Significance of Downregulated E-Cadherin Expression in Patients with Non-Small Cell Lung Cancer (NSCLC): A Meta-Analysis
Yan-Long Yang, Ming-Wu Chen, Lei Xian, Alfons Navarro
PLoS ONE.2014; 9(6): e99763. CrossRef - Hepatic Stellate Cells Secreted Hepatocyte Growth Factor Contributes to the Chemoresistance of Hepatocellular Carcinoma
Guofeng Yu, Yingying Jing, Xingrui Kou, Fei Ye, Lu Gao, Qingmin Fan, Yang Yang, Qiudong Zhao, Rong Li, Mengchao Wu, Lixin Wei, Xin-Yuan Guan
PLoS ONE.2013; 8(9): e73312. CrossRef - A Comprehensive Comparative Analysis of the Histomorphological Features of ALK-Rearranged Lung Adenocarcinoma Based on Driver Oncogene Mutations: Frequent Expression of Epithelial-Mesenchymal Transition Markers than Other Genotype
Hyojin Kim, Se Jin Jang, Doo Hyun Chung, Seol Bong Yoo, Pingli Sun, Yan Jin, Kyung Han Nam, Jin-Ho Paik, Jin-Haeng Chung, Alfredo Fusco
PLoS ONE.2013; 8(10): e76999. CrossRef - Non-small cell lung cancer cells survived ionizing radiation treatment display cancer stem cell and epithelial-mesenchymal transition phenotypes
Roberto Gomez-Casal, Chitralekha Bhattacharya, Nandita Ganesh, Lisa Bailey, Per Basse, Michael Gibson, Michael Epperly, Vera Levina
Molecular Cancer.2013;[Epub] CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure

 E-submission
E-submission